Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Epidemiologia e Serviços de Saúde
versão impressa ISSN 1679-4974versão On-line ISSN 2337-9622
Epidemiol. Serv. Saúde v.26 n.1 Brasília jan./mar. 2017
http://dx.doi.org/10.5123/s1679-49742017000100017
RESEARCH NOTE
Profile of human anti-rabies treatment in the ‘agreste’ region of Pernambuco State, Brazil, 2010-2012*
1Universidade Federal Rural de Pernambuco, Departamento de Medicina Veterinária, Recife-PE, Brasil
2Universidade de Pernambuco, Campus Caruaru, Caruaru-PE, Brasil
3Universidade Federal Rural de Pernambuco, Departamento de Medicina Veterinária, Recife-PE, Brasil
Objective:
to describe the characteristics of reported human anti-rabies treatment in municipalities of the ‘agreste’ region of Pernambuco State, Brazil, 2010-2012.
Methods:
this was a descriptive study using data from human anti-rabies medical records filed on the Information System for Notifiable Diseases (Sinan).
Results:
10,138 reported records of anti-rabies treatment were included; canines were the most involved species (68.1%), in good health condition (79.9%). Biting was the most common contact (83.8%), causing multiple injuries (58.3%), to hands/feet (39.4%), and deep wounds in 56.8% of cases; combined vaccine + serum administration frequency was found to be low (10.5%), even though 47.9% of injuries were considered severe and therefore required this prophylactic procedure.
Conclusion:
possible inadequate prophylaxis procedures were found, showing the need for health worker training aimed at ensuring correct human anti-rabies prophylaxis and the proper filling in of medical record files.
Key words: Rabies/prevention & control; Health Services; Disease Prevention; Epidemiology, Descriptive
Introduction
Climate change induced by human activities can have an influence on the occurrence and resurgence of infectious diseases, such as leishmaniasis, dengue fever, hantavirus infection and rabies.1-3 Scientific progress, such as vaccine development, can also modify the epidemiology of infectious diseases. This is the case of human rabies, for instance. The availability of an effective vaccine and the implementation of new strategies by health administrators enabled the refinement of urban rabies control, aiming its eradication. On the other hand, the pressure of human activities over the environment and the contact, increasingly close, between humans and wild animals influence the epidemiology of rabies in areas where the disease is endemic.4-7
Researches on the epidemiologic situation of rabies in the Americas revealed that its incidence has suffered great reduction, especially since 1990.4,6 The incidence of cases of rabies on humans reduced from 216 (1993) to 39 (2002). The reduction was also observed in cases of rabies on dogs. In 1993, there were 6,716 cases notified and in 2002, 1,311.3 An analysis of tendency to rabies cases in the period of 1982 to 2003 showed a decrease in human cases from 355 to 35.6 We can attribute the success of rabies control to the vaccination campaigns for dogs and cats and to the prophylaxis, with application of the post-exposure anti-rabies vaccination for humans.6 In Brazil, like in the Americas, we can also observe the tendency towards reduction of rabies cases.8
Since the nineties from the 20th century, anti-rabies vaccination campaigns for dogs and cats were conducted periodically in most countries where human rabies is considered endemic.4 Moreover, each year, approximately one million people exposed to potential transmitters of the rabies virus sought assistance and 30% received prophylactic treatment.4 Thus, the number of human rabies cases transmitted by dogs in Brazil has suffered a considerable decrease. In contrast, cases of rabies transmitted by wild animals has showed a relative increase over the past few years.4,9,10
In Pernambuco state, there were no cases of human rabies since 2006, despite the constant reports of cases of rabies in animals.8,11 Cases of animal attack on humans, however, are frequently reported in the state, which indicates risk of occurrence of human rabies.
The present study aims to describe the characteristics in reports of human anti-rabies treatment and prophylactic measures adopted in municipalities of the Pernambuco ‘agreste’ mesoregion, from 2010 to 2012.
Methods
We carried out a time series epidemiologic descriptive study about the assistance and conduct of post-exposure prophylactic anti-rabies treatment on humans in 32 municipalities of the ‘agreste’ mesoregion of Pernambuco state (Figure 1), Northeast, Brazil, in the period from 2010 to 2012, with data obtained from the Information System for Notifiable Diseases (Sinan).
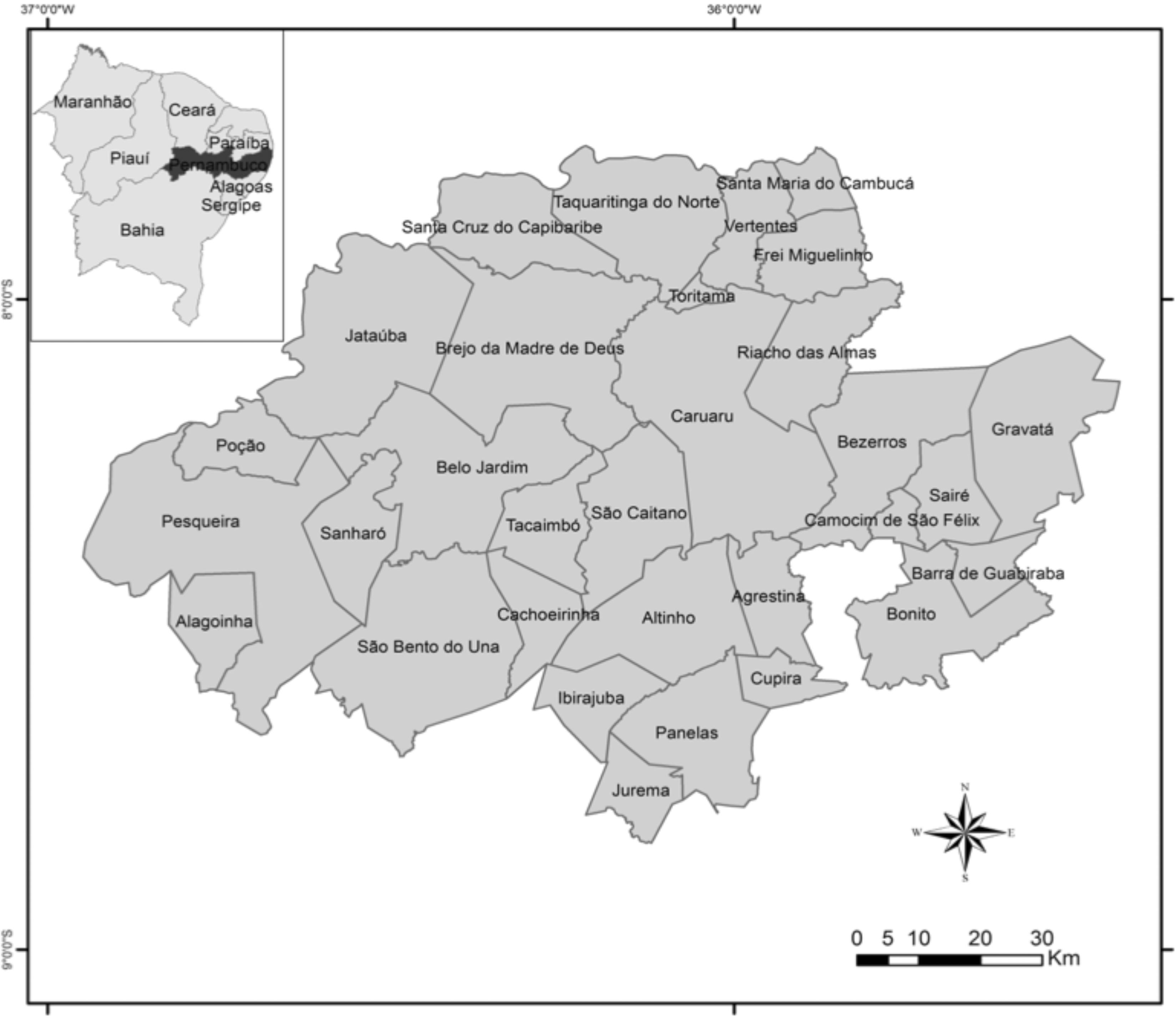
Figure 1 - Map of the municipalities that assemble the IV Regional Management of Health, of the ‘agreste’ mesoregion of Pernambuco state
It was calculated the relative and absolute frequency of the following variables:
a) Attack
- month of report;
- anatomical position;
- depth of the injury (deep, superficial or lacerating);
- appearance of the injury (single, multiple or no injury);
- and type of the attack (scratching, licking, biting and others).
b) Attacked individual
- gender; and
- age.
c) Species of the attacker
- species (canine, feline, chiroptera, primates, foxes, domestic herbivores and others) and
- initial physical condition (healthy, suspicious, rabid and dead/missing).
d) Treatment
- performed conduct (pre-exposure, dismissed of treatment, animal observation, observation and vaccine, vaccine, serum and vaccine, and plan of re-exposure);
- interruption of treatment; and
- reason for interruption of treatment (recommendation of health unit, abandonment of therapy or health unit transference).
Data were analysed with the softwares Microsoft Excel 2010 and TabWin version 3.2.
The research was conducted according to the ethical principles of the resolution of the National Health Council (CNS) No. 466, of December 12th, 2012. The authors did not have access to data that allowed the identification of the individuals. Secondary data were obtained with authorization and knowledge from the IV Regional Management of Health of Pernambuco state.
Results
In the period from 2010 to 2012, 10,138 patients undergone prophylactic anti-rabies treatment after a potential exposure to the virus. The period with the most occurrences of assistances was the third quarter (months of July, August, and September), with 26% of reported cases (Table 1).
Table 1 - Main Characteristics of anti-rabies assistances performed in municipalities of the ‘agreste’ mesoregion of Pernambuco state, 2010-2012
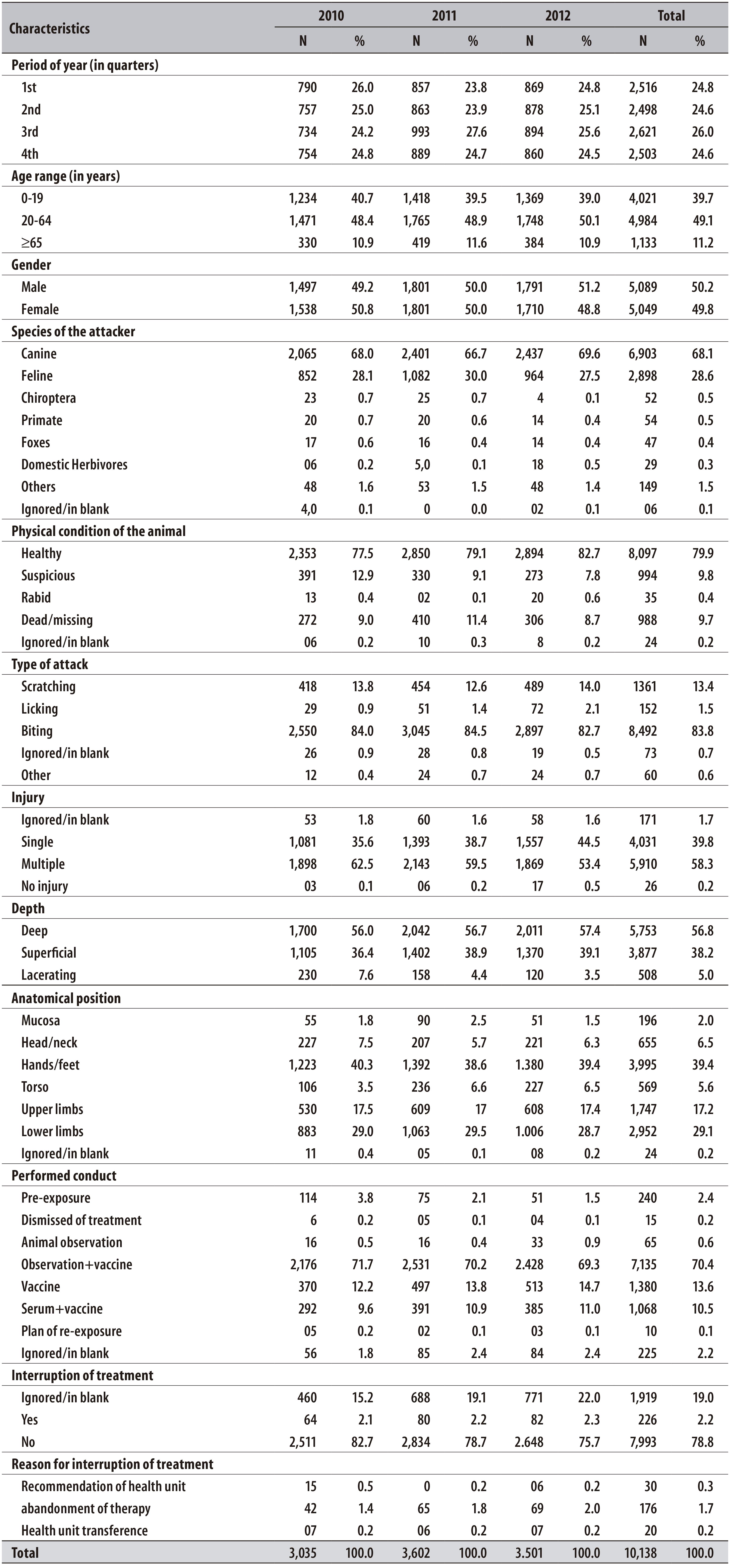
Distribution among genders was greatly homogeneous, with 50.2% of individuals from the male gender. The most affected age group was from 20 up to 64 years old, with 49.1% of cases (Table 1).
Dogs were responsible for 68.1% of the attacks, followed by felines (28.6%). Other species (chiroptera, foxes, primates, and others) totaled 3.2% of the reports. Among dogs and cats, approximately 80.0% were classified as healthy (Table 1).
The most frequent type of contact was biting (83.8%). We verified that 58.3% of the injuries were multiple and 39.8% were single. Deep injuries (56.8%) were more frequently reported, followed by superficial injuries (38.2%) and lacerating injuries (5.0%). Regarding the anatomical position, we observed that hands and feet were most affected (39.4%), followed by lower limbs (29.1%) (Table 1).
With respect to the prophylactic conducts, the majority of recommendations were associated to observation and vaccine (70.4%), followed by vaccination (13.6%), and use of serum combined with vaccine (10.5%). Only 0.2% of the analyzed cases were dismissed of treatment. Regarding the reports forms, 58.33% (7/12) had unfilled variables (left in blank) or with ‘ignored’ register of the data. We also verified that 2.2% of the patients interrupted the treatment, and the reason for the interruption was not stated on the report form (Table 1).
Discussion
The research pointed out that the majority of anti-rabies prophylactic assistances occurred in July, August and September, corresponding with the holidays period, with a higher human mobility, like travelling and other activities taking place outside residences, which make individuals more exposed to animal contact and attacks.12,13
In the present study, we observed homogeneity in distribution of cases according to gender, while other similar studies had found predominance of assistance to individuals of the male gender.7,14,15 Regarding the age range, adults between 20 and 64 years old were the most affected, data which is similar to other studies.16,17 It is possible that adults are more prone to such attacks because of their daily work activities (the case of professionals with occupational hazards), their care for domestic animals and mobility through public roads.16,17
The majority of attacks were provoked by canine and feline species. Historically, cats and dogs were indicated as the main transmitters of human rabies. However, since the nineties, the occurrence of human rabies transmitted by wild animals has increased in Latin America, and in several regions of Brazil, where the transmission of the rabies virus to humans by hematophagous bats has also increased and, in certain cases, has surpassed the transmission by canine species. For these reasons, even if attacks by wild animals were reported less frequently, we must observe its importance in transmission of rabies.4,6,9,18-22
In this research, we observed the predominance of biting, multiple and deep injuries. Probably, the population’s awareness of the high risk of infection of the rabies virus through biting results in more searches for assistance after the occurrence of this type of possible exposure.14,23-25 The most affected body parts of victims were hands and/or feet, because, we presume, these are regions related to defense positions of the victim or to the impulsive act of trying to hold/contain the animal at the time of the attack.14
We highlight that in only 10.5% of the assistances the serum and vaccine combination was recommended, although 47.9% of the reported cases were accidents considered serious (located on the head, hands/feet and mucosa; deep and multiple injuries; attacks by wild animals or dead/missing animals), which should be treated with the serum and vaccine combination. This finding, along with the inadequate filling of the report forms, suggests that part of the conducts performed in healthcare units are inappropriate for the types of attack, as it has been verified in other locations in Pernambuco state.7,26
We identified gaps in the filling of the report forms. For example, some reports had some variables left in blank or registered as data ‘ignored’, like ‘Animal condition for purposes of conduct and treatment’, ‘Injury’ and ‘Recommended treatment’, a situation that hampers the process to evaluate the epidemiologic characteristics and the establishment of the correct conduct by the healthcare team.
In the region of the analyzed municipalities, we observed a slight percentage of interruption of the anti-rabies prophylactic treatment, probably due to the success of the decentralization of the assistance as a way to ease accessibility. Furthermore, it is not necessary to schedule the medical appointment. 16,27-29
Health authorities should continue to concentrate their efforts in control measurements and eradication of rabies. We recommend the introduction of permanent training programs of healthcare teams for the correct filling of the human anti-rabies assistance report forms and educational health orientation. In addition to this, we recommend the integration of doctors to veterinary physicians, aiming to enable a careful analysis of the attack, animal condition and epidemiologic risk of the disease, so then the decision for the prophylactic measure will be adequately performed by the institution.
REFERENCES
1. McMichael AJ, Woodruff RE, Hales S. Climate change and human health: present and future risks. Lancet. 2006 Mar;367(9513):859-69. [ Links ]
2. Patz JA, Graczyk TK, Geller N, Vittor AY. Effects of environmental change on emerging parasitic diseases. Int J Parasitol. 2000 Nov;30(12-13):1395-405. [ Links ]
3. Morse SS, editor. Emerging viruses. Oxford:Oxford University Press;1993. [ Links ]
4. Belotto A, Leanes LF, Schneider MC, Tamayo H, Correa E. Overview of rabies in the Americas. Virus Res. 2005 Jul;111(1):5-12. [ Links ]
5. Rupprecht CE, Smith JS, Fekadu M, Childs JE. The ascension of wildlife rabies: a cause for public health concern or intervention? Emerg Infect Dis. 1995 Oct-Dez;1(4):107-14. [ Links ]
6. Schneider MC, Belotto A, Adé MP, Leanes LF, Correa E, Tamayo H, et al. Epidemiologic situation of human rabies in Latin America in 2004. Epidemiol Bull. 2005 Mar;26(1):2-4. [ Links ]
7. Silva GM, Brandespim DF, Rocha MDG, Leite RMB, Oliveira JMB. Notificações de atendimento antirrábico humano na população do município de Garanhuns, Estado de Pernambuco, Brasil, no período de 2007 a 2010. Epidemiol Serv Saude. 2013 jan-mar;22(1):95-102. [ Links ]
8. Wada MY, Rocha SM, Maia-Elkhoury, ANS. Situação da Raiva no Brasil, 2000 a 2009. Epidemiol Serv Saude. 2011 out-dez;20(4):509-18. [ Links ]
9. Favoretto SR, Mattos CC, Morais NB, Carrieri ML, Rolim BN, Silva LM, et al. Rabies virus maintained by dogs in humans and terrestrial wildlife, Ceará State, Brazil. Emerg Infect Dis. 2006 Dec;12(12):1978-81. [ Links ]
10. Rosa EST, Kotait I, Barbosa TFS, Carrieri ML, Brandão PE, Pinheiro AS, et al. Bat-transmitted human rabies outbreaks, Brazilian Amazon. Emerg Infect Dis. 2006 Aug;12(8):1197-202. [ Links ]
11. Ministério da Saúde (BR). Secretaria de Vigilância em Saúde. Sistema Nacional de Vigilância em Saúde: relatório de situação: Pernambuco. Brasília: Ministério da Saúde; 2006. [ Links ]
12. Frangakis CE, Petridou E. Modelling risk factors for injuries from dog bites in Greece: a case only design and analysis. Accid Anal Prev. 2003 May;35(3):435-8. [ Links ]
13. Silveira MMM. Características do tratamento anti-rábico humano em Belo Horizonte, de 1990-2000 [dissertação]. Belo Horizonte: Universidade Federal de Minas Gerais; 2001. [ Links ]
14. Mundim APM. Exposição à raiva humana no Município de Cuiabá-MT: epidemiologia e avaliação das medidas preventivas [dissertação]. Cuiabá: Universidade Federal de Mato Grosso; 2005. [ Links ]
15. Filgueira AC, Cardoso MD, Ferreira LOC. Profilaxia antirrábica humana: uma análise exploratória dos atendimentos ocorridos em Salgueiro - PE, no ano de 2007. Epidemiol Serv Saude. 2011 abr-jun;20(2):233-44. [ Links ]
16. Veloso RD, Aerts DRGC, Fetzer LO, Anjos CB, Sangiovanni JC. Motivos de abandono do tratamento antirrábico humano pós-exposição em Porto Alegre (RS, Brasil). Cienc Saude Coletiva .2011 fev;16(2):537-46. [ Links ]
17. Blanton JD, Bowden NY, Eidson M, Wyatt JD, Hanlon CA. Rabies postexposure prophylaxis, New York, 1995-2000. Emerg Infect Dis. 2005 Dec;11(12):1921-7. [ Links ]
18. Mayen F. Haematophagous bats in Brazil, their role in rabies transmission, impact on public health, livestock industry and alternatives to an indiscriminate reduction of bat population. J Vet Med B Infect Dis Vet Public Health. 2003 Dec;50(10):469-72. [ Links ]
19. Queiroz LH, Carvalho C, Buso DS, Ferrari CIL, Pedro WA. Perfil epidemiológico da raiva na região Noroeste do Estado de São Paulo no período de 1993 a 2007. Rev Soc Bras Med Trop. 2009 jan-fev;42(1):9-14. [ Links ]
20. Albas A, Souza EAN, Picolo MR, Favoretto SR, Gama AR, Sodré MM. Os morcegos e a raiva na região oeste do Estado de São Paulo. Rev Soc Bras Med Trop. 2011 mar-abr;44(2):201-5. [ Links ]
21. Sodré MM, Gama AR, Almeida MF. Lista atualizada das espécies de morcegos positivas para raiva no Brasil. Rev Inst Med Trop S Paulo. 2010 mar-abr;52(2):75-81. [ Links ]
22. Ministério da Saúde (BR). Secretaria de Vigilância em Saúde. Departamento de Vigilância Epidemiológica. Manual de vigilância epidemiológica de eventos adversos pós-vacinação. Brasília: Ministério da Saúde; 2008. p.106-13. [ Links ]
23. Garcia RCM, Vasconcelos AS, Sakamoto SM, Lopes AC. Análise de tratamento anti-rábico humano pós exposição em região da Grande São Paulo, Brasil. Rev Saude Publica. 1999 jun;33(3):295-301. [ Links ]
24. Dantas-Torres F, Oliveira-Filho EF. Human exposure to potential rabies virus transmitters in Olinda, State of Pernambuco, between 2002 and 2006. Rev Soc Bras Med Trop. 2007 nov-dez;40(6):617-21. [ Links ]
25. Rigo L, Honer MR. Análise da profilaxia da raiva humana em Campo Grande, Mato Grosso do Sul, Brasil, em 2002. Cad Saude Publica. 2005 nov-dez;21(6):1939-45. [ Links ]
26. Ministério da Saúde (BR). Secretaria de Vigilância em Saúde. Departamento de Vigilância Epidemiológica. Normas técnicas de profilaxia da raiva humana. Brasília: Ministério da Saúde; 2011. (Série A: Normas e Manuais Técnicos) [ Links ]
27. Gomide Júnior MH. Profilaxia da raiva humana em Luís Antônio, SP, Brasil: características das ocorrências a atenção médica prestada aos pacientes [dissertação]. Ribeirão Preto: Universidade de São Paulo; 2013. [ Links ]
28. Alvarez E, Ruiz A. La situación de la rabia en América Latina de 1990 a 1994. Bol Oficina Sanit Panam. 1995 nov;119(5):451-6. [ Links ]
29. Brasil. Lei nº 8080, de 19 de setembro de 1990. Dispõe sobre as condições para a promoção, proteção e recuperação da saúde, a organização e o funcionamento dos serviços correspondentes, e dá outras providências. Diário Oficial da República Federativa do Brasil, Brasília (DF), 1990 set 20;Seção 1:18055. [ Links ]
Received: May 29, 2016; Accepted: July 12, 2016











 texto em
texto em 


