Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Epidemiologia e Serviços de Saúde
versão impressa ISSN 1679-4974versão On-line ISSN 2337-9622
Epidemiol. Serv. Saúde v.26 n.2 Brasília abr./jun. 2017
http://dx.doi.org/10.5123/s1679-49742017000200015
Original article
Prevalence of Kaposi's sarcoma in patients with AIDS and associated factors, São Paulo-SP, Brazil, 2003-2010*
1Secretaria de Estado da Saúde de São Paulo, Programa Estadual de DST/Aids, São Paulo-SP, Brasil
2Secretaria de Estado da Saúde de São Paulo, Instituto de Infectologia Emílio Ribas, São Paulo-SP, Brasil
3Johns Hopkins University School of Medicine, Johns Hopkins Bloomberg School of Public Health, Baltimore-MD, United States of America
OBJECTIVE:
to estimate the prevalence of Kaposi’s sarcoma (KS) in patients with AIDS and identify the associated factors to the occurrence of this neoplasm.
METHODS:
this is a cross-sectional study with notification data from two AIDS reference centers in São Paulo-SP, Brazil, from January, 2003 to March, 2010; probabilistic linkage and multiple logistic regression methods were applied.
RESULTS:
among 3,557 AIDS cases, 213 (6%) presented KS; 95.3% of them occurred in males; male sex (OR=3.1; 95%CI=1.4;6.6), age at the AIDS diagnosis >28 years old (OR=1.6; 95%CI=1.0;2.6), MSM (OR=3.2; 95%CI=2.0;4.9), prior use of HAART (OR=0.4; 95%CI=0.3;0.5), AIDS diagnosis between 2007-2010 (OR=0.3; 95%CI=0.2;0.4), and CD4+ T-cell counting under 200cells/mm3 (OR=16.0; 95%CI=6.0;42.7) and 200-500cells/mm³ (OR=2,5; 95%CI=1.1;6.4) were associated to the occurrence of KS.
CONCLUSION:
KS has a high prevalence in São Paulo-SP; strategies for early HIV diagnosis may reduce this prevalence.
Keywords: Acquired Immunodeficiency Syndrome; Kaposi's Sarcoma; Highly Active Antiretroviral Therapy; Epidemiology, Descriptive
Introduction
Kaposi's sarcoma (KS) is a mesenchymal tumor, caused by herpes virus type 8 (HHV-8), and a characteristic neoplasm of acquired immunodeficiency syndrome (AIDS). After the emergence of AIDS in 1980, a more aggressive form of the disease, more common among homosexual or bisexual men and associated with the human immunodeficiency virus (HIV), was documented. It was soon recognized as an epidemic form of KS,1 which had a big impact on the Public Health due to its high magnitude and mortality. KS was the first opportunistic infection recognized in association with HIV and is still the most common neoplasm related to AIDS.1,2
The introduction of highly active antiretroviral therapy (HAART) helped to strengthen the immune system of people infected with HIV and lowered the risk of these people to develop KS. Nevertheless, KS is still considered the most prevalent tumor among this population.3,4
Although HAART does not interfere directly with the replication of HHV-8, cases of regression of KS-AIDS lesion have been observed frequently after the use of HAART in combination with chemotherapy or radiotherapy,5 though the mechanism by which HAART leads to the regression of KS remains controversial.2,3 The incidence of KS has substantially declined due to HAART,4 in the same way that KS-AIDS became less aggressive when compared to KS among individuals with no antiretroviral treatment.6,7
In Brazil, from 1996 to 2010 - already in the post-HAART era -, the incidence of KS was still 2.5 times higher than in the United States of America (USA), and it remains as the most common neoplasm in HIV carriers.8
The aim of this study was to estimate the prevalence of Kaposi's sarcoma in patients with AIDS and identify the factors associated with the occurrence of this neoplasm.
Methods
This is a cross-sectional study based on data of patients with AIDS under follow-up at two AIDS reference centers, from January 2003 to March 2010.
Both centers offer specialized care in AIDS in the municipality of São Paulo-SP, each with approximately 5,000 patients followed-up for HIV/AIDS. São Paulo-SP is the largest municipality in Brazil, and had 11.3 million inhabitants, according to 2010 census.9 It is the capital of São Paulo State and the main financial, corporate and commercial center in South America. From 1980 to 2014, 86,112 AIDS cases were reported in the municipality, representing a detection rate of 18.6 per 100,000 inhabitants/year at the end of the period, with 41,704 individuals living with HIV,10 to whom the municipality offers free treatment since 2014, regardless of the CD4+ T-cell count in the laboratory result of the patient.
The study population consisted of patients aged 13 years old or over with AIDS, registered on the Information System for Notifiable Diseases (Sinan), and being followed-up in those centers, in the period of the study.
We defined AIDS cases as 'every individual infected with HIV who had at least one disease indicative of AIDS, and/or CD4+ T-cell count below 350 cells/mm3, regardless of the presence of other causes of immunodeficiency'.
During the study period, the Brazilian Ministry of Health proposed several changes for AIDS cases definition: 1) Centers for Disease Control and Prevention (CDC)/USA criterion; 2) Rio de Janeiro-Caracas criterion; 3) death exceptional criterion; and 4) adapted CDC criterion. In this study, each of these changes was followed, according to their period of validity. Exposure categories for HIV transmission and treatment regimens were classified according to the criteria of the Brazilian Ministry of Health.
Although a presumptive diagnosis of KS is often based on medical history and appearance of skin lesions,11 only cases confirmed by biopsy were considered.
The data sources used in the research were: (i) São Paulo Integrated AIDS Database (BIPAIDS), created from the linkage between the deaths database of the State System for Data Analysis (SEADE) and the database of the Information System for Notifiable Diseases (Sinan-AIDS) of São Paulo State Program for STD/AIDS; (ii) Laboratory Tests Control System (SISCEL); and (iii) Drug Logistics Control System (SICLOM), of the Ministry of Health.
RecLinkII software, version 3.1, performed the linkage between the databases. The databases were linked through the probabilistic method. Routines were used for standardization of common fields that would be used to relate and identify duplicate records between the bases. True pairs were classified through the blocking of variables consisting of first and last name, sex, date of birth and mother's name, in order to optimize the comparison between records. The application of algorithms to an approximate comparison of strings aimed to identify possible phonetic and typographical errors. The calculation of scores that summarize the overall level of agreement between records of the same pair was established; we also set thresholds for the classification of pairs of records into true pairs, non-pairs and doubtful pairs. A manual review of doubtful pairs was made aiming to classify them as true pairs or non-pairs and to check for duplicate records in files. These data were individually checked to confirm the coinfection.
In order to complete the ignored information, additional data were collected from patients' medical records.
The independent variables of the study were:
a) Sociodemographic characteristics
- Sex (male; female);
- Age (in years: 13 to 19; 20 to 29; 30 to 39; 40 to 49; 50 to 59; 60 to 69; 70 to 79);
- Education level (in years of schooling: ≤8; 9 to 12; ≥13; none);
- Ethnicity/skin color (white, black, brown, Asian, indigenous);
b) Behavioral characteristics
- Exposure category (heterosexual, men who have sex with men - MSM -, injectable drug users; other);
c) Clinical and laboratory characteristics
- KS (yes; no);
- Use of HAART prior to the diagnosis of KS (yes; no);
- CD4+ T-cell count (<200cells/mm³; 200 to 500cells/mm³; > 500cells/mm³); and
- period of AIDS diagnosis (2003 to 2006; 2007 to 2010)
The CD4+ T-cell count at the time of diagnosis of AIDS was considered for the analysis.
KS was the event chosen as the dependent variable. Sociodemographic, behavioral, clinical and laboratory characteristics were regarded as independent variables of interest. The associated factors were analyzed in blocks through the multiple logistic regression model, and all variables with a significance level of p<0.15 were considered eligible to be included in the model. The test based on the likelihood ratio was used every time a new variable was included, and, if the significance of the new model was higher than 0.05, the variable was excluded.
Epi Info TM software, version 3.4.3, was used to complement data entry, and STATA, version 10.0 was used for modeling.
The study was approved by the Ethics Research Committees of the Reference and Training Center in STD/AIDS (RTC-DST/AIDS) - Protocol No. 555.248, dated March 11th, 2014 - and of the Institute of Infectious Diseases Emilio Ribas (IDERI) - Protocol No. 618.177, dated April 9th, 2014.
Results
The study population consisted of 3,557 AIDS cases, of which 213 (6.0%) had KS.
The epidemiological, demographic, and clinical and laboratory characteristics of patients with AIDS and Kaposi's sarcoma are presented in Table 1.
Table 1 - Sociodemographic, behavioral and clinical laboratory characteristics of patients with AIDS treated at the Reference and Training Center for STD/AIDS and at the Institute of Infectious Diseases Emilio Ribas, São Paulo-SP, 2003-2010
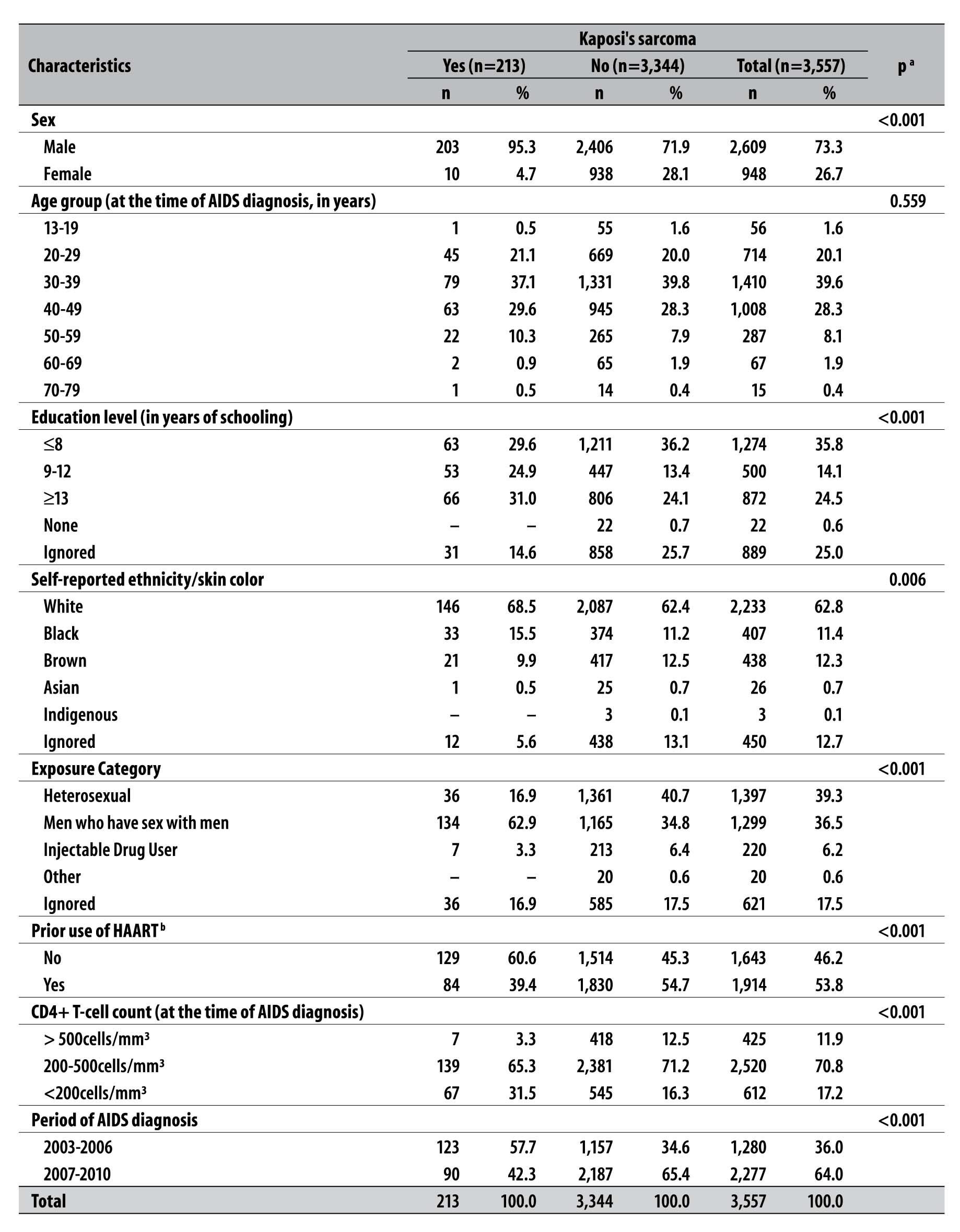
a) Fisher's exact test
b) HAART: Highly active antiretroviral therapy
There was a predominance of males in the total number of AIDS cases (73.3%) and in almost all cases of KS (95.3%). The diagnosis of AIDS was predominant at the age of 30 to 39 years old (39.6%), the same age group that presented the highest proportion of KS cases (37.1%).
Cases of AIDS - 38.6% (1,372/3,557) - and of KS - 55.9% (119/213) - occurred more often in individuals with nine or more years of schooling. About two-thirds of them (62.8%) reported being white; and this proportion rose to 68.5% among the cases of KS.
The largest proportion of patients with AIDS was of heterosexual individuals (39.3%); however, among the cases of KS, the highest proportion was represented by MSM (62.9%).
More than half of patients with AIDS reported prior use of HAART (53.8%), whereas only 39.4% of individuals with KS were undergoing this therapy.
Most patients with AIDS (70.8%) had a CD4+ T-cell count between 200 and 500cells/mm³; in the cases of KS, the proportion of CD4+ T-cells at this range was of 65.3%.
Comparing the periods of 2003-2006 and 2007-2010, there was a higher number of diagnosis of AIDS in the second period (2,277 versus 1,280), although the highest number of cases of KS were diagnosed in the first period (123 versus 90).
In the crude analysis, presented in Table 2, the following variables were associated with the progression to KS: male sex (OR=7.9; 95%CI=4.2; 15.0); age under 28 years old at the time of AIDS diagnosis (OR=1.3; 95%CI= 0.9; 2.0); up to 8 years of schooling (OR=1.6; 95%CI=1.1; 2.2) and 9 to 12 years of schooling (OR=2.3; 95%CI=1.5; 3.3) ; MSM (OR=4.3; 95%CI=3.0; 6.3); prior use of HAART (OR=0.5; 95%CI=0.4; 0.7); CD4+ T-cell count at the time of diagnosis of AIDS between 200 and 500cells/mm³ (OR=3.5; 95%CI=1.6; 7.5) and below 200cells/mm³ (OR = 7.3; 95%CI=3.3; 16.1); and period of AIDS diagnosis from 2007 to 2010 (OR = 0.4; 95%CI=0.3; 0.5).
Table 2 - Crude and adjusted analysis of factors associated with Kaposi's sarcoma in patients with AIDS treated at the Reference and Training Center for STD/AIDS and the Institute of Infectious Diseases Emilio Ribas, São Paulo-SP, 2003-2010
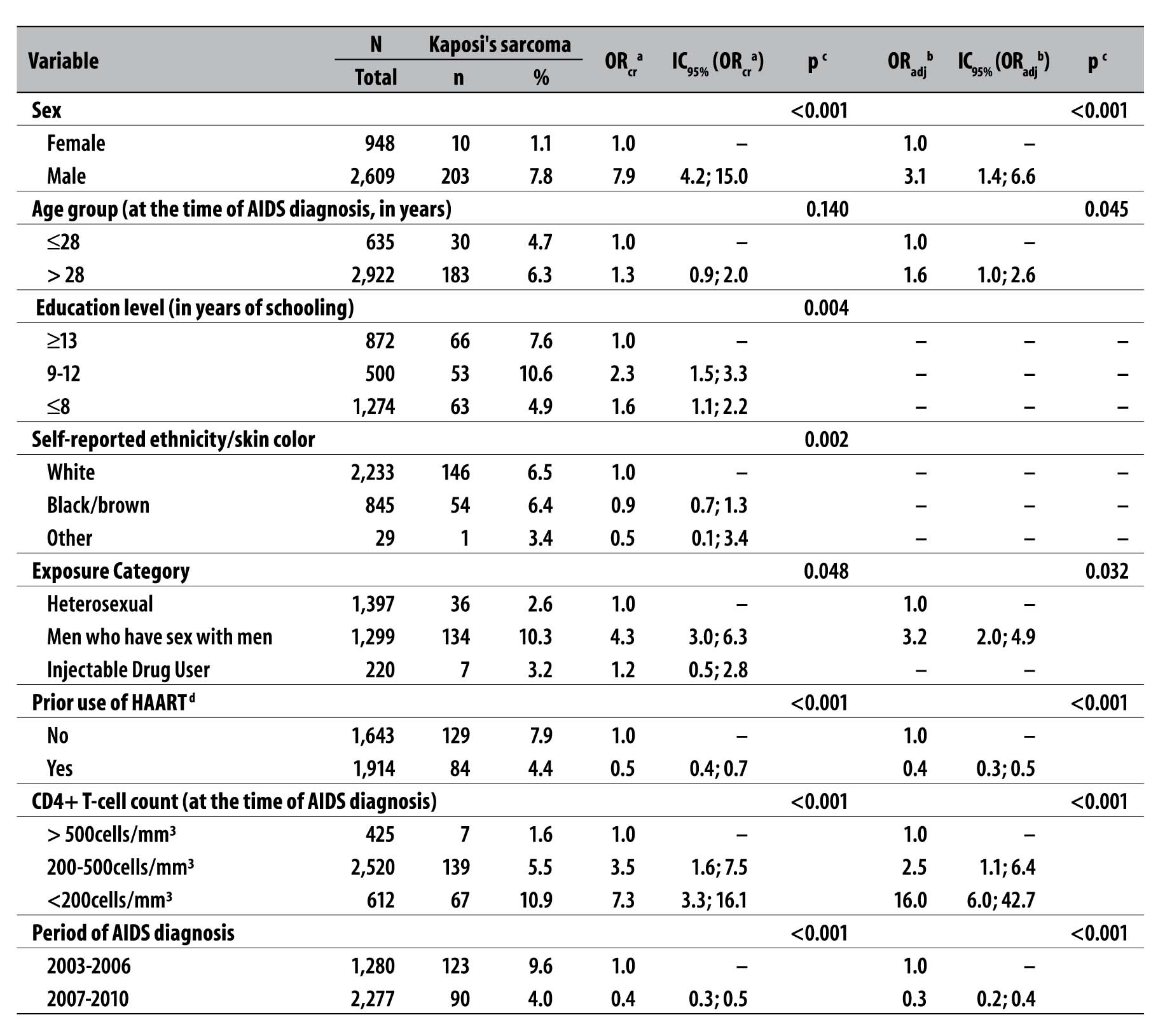
a) ORcr: crude odds ratio
b) ORadj: adjusted odds ratio
c) Wald test
d) HAART: Highly active antiretroviral therapy
Table 2 also shows the multiple logistic regression model, which identified the following associated factors: male sex (OR=3.1; 95%CI=1.4; 6.6); age under 28 years old at the time of AIDS diagnosis (OR=1.6; 95%CI=1.0;2.6); MSM (OR=3.2; 95%CI=2.0; 4.9); prior use of HAART (OR=0.4; 95%CI=0.3; 0.5); CD4+ T-cell count at the time of AIDS diagnosis between 200 and 500cells/mm³ (OR=2.5; 95%CI=1.1; 6.4) and below 200 cells/mm³ (OR=16.0; 95%CI=6.0;42.7); and period of AIDS diagnosis from 2007 to 2010 (OR=0.3; 95%CI=0.2;0.4).
Discussion
The findings of this study indicate that, despite the therapeutic arsenal available in Brazil and the free access to treatment for people with HIV, KS is still highly prevalent (about 1 in 20 cases) among individuals with AIDS in São Paulo-SP, showing a strong association with sex, age, MSM, prior use of HAART, period of AIDS diagnosis and low CD4+ T-cell count. Early diagnosis of HIV infection and use of HAART were identified as the main protective factors against KS.
The prevalence found was much higher than the one shown by the data of national registers, among which 3,103 cases of KS/AIDS were reported in the same period,11 corresponding to 1.5% of all reported AIDS cases.12 Other studies conducted in Brazil have estimated prevalences of 9.1% and 17.1% of KS in people with AIDS in the municipality of Rio de Janeiro-RJ (2009) and in São Paulo State (2010), respectively.13,14
Prevalence of KS in individuals with AIDS has been observed in other countries, ranging from 7 to 32% in Africa (2005 to 2011),15,16 22.6% in Cuba (1998-2002)17 and 1.0% in Spain (1997-2008).18
Although it was described in 1872, in its classic form, KS achieved global clinical importance as an opportunistic disease since the first reports of the AIDS epidemic. Nowadays, despite advances in the diagnosis and HAART, KS remains the most common neoplasm in HIV-infected individuals,1,2 and is an AIDS-defining illness. Up to 2008, in the United States, and 2009, in Australia, KS was the second most common neoplasm associated with AIDS, even after the HAART era, which began in 1996.19,20
In Brazil, KS is predominant among men (95.3%). As observed in other studies, men who have sex with men were identified as the predominant group, being approximately three times more likely to contract the disease when compared to heterosexuals, which corroborates data from a study that showed an association of KS with homosexual and bisexual males.21
KS risk found in this study was three times higher for men, which is similar to a South African study22 conducted from 2004 to 2010. Despite the higher risk for men, women with AIDS should not be neglected in relation to Kaposi's sarcoma: a study conducted in Italy23 showed that KS is more aggressive and involves greater risk of death in women than in men, with higher proportion of visceral diseases, particularly in pulmonary involvement. This disease, when spread out among women, is usually mistaken with lung infection. Perhaps this mistake occurs due to the low suspicion of KS in women with AIDS.24
In the present study, KS was associated with age over 28 years, a finding consistent with other researches that correlated this variable with the outcome.19 In the pre-HAART era, KS was not consistently related to age or ethnicity/ skin color, but in the USA, Beral et al identified, in the 1981-1989 period, that the proportion of KS increased in the age group of 35 to 40 years.1
KS was predominant in white individuals, although this variable did not reveal statistical association. In the USA, from 1995 to 2008, with regard to adolescents and young adults with AIDS, the incidence was higher in black people and Hispanics, when compared to white individuals.25
In this study, the prior use of HAART proved to be a protective factor against the development of KS, in agreement with other studies, according to which the use of HAART leads to a significant reduction in the incidence of Kaposi's sarcoma,21,26 in addition to extending the survival of patients with KS, with an 80% reduction in the risk of death.27
Two periods of AIDS diagnosis were compared (2003-2006 and 2007-2010), and we observed a reduction in the number of KS cases in the most recent period, despite the increase in the number of AIDS cases in the same period, probably due to the increased adherence to antiretroviral drugs.
KS still prevails as the most frequent neoplasm in patients with AIDS living in São Paulo,14 although it showed a lower prevalence in the reported cases in the state,27 from 4.6% from 1990 to 1995 to 1.6% from 2001 to 2005 - a possible effect of HAART, in line with decreases observed in the USA and Europe.28,29
A strong association between KS and CD4+ T-cell count was identified in this study, with a risk 16 times higher when the count was below 200cells/mm3. Frequently, the development of KS in people living with HIV is correlated with low levels of CD4+ T-cell, confirming the results of a study conducted in Brazil8 and also the findings from researches conducted in other countries, such as South Africa22 and Malawi,15 in which CD4+ T-cell count below 150cells/mm3 was associated with higher mortality; in the USA, low levels of CD4+ T-cell was found to be associated with a risk of death 4 times higher;26 in France30 the risk of KS doubled when related to CD4+ T-cell count between 350 and 499cells/mm3; and in Italy,21 the highest risk of contracting KS was associated with a CD4+ T-cell count below 200cells/mm3.
Different findings were reported by Lima et al27 in Brazil and by Nguyen et al5 in the United States, in which there was no association between KS and low CD4+ T-cell counts; however, 83% of that sample had CD4+ T-cell count below 200 cells/mm³.
A limitation found in this study was the difficulty to identify the time sequence of the exposure of interest in relation to the effect (Kaposi's sarcoma). The lack of an evaluation of individual adherence to antiretroviral drugs was another limitation. Likewise, the staging of KS was not known, which hampered the verification of differences between cases exclusively cutaneous and those with visceral involvement.
Albeit these limitations, this study allowed us to determine the prevalence and factors associated with KS among patients with AIDS treated at two specialized centers in Brazil's largest city. The potential for transmission of HIV and HHV-8 through unprotected sex reinforces the need for health education actions, to promote safe sex practices. In Brazil, where free condoms are available, the main question to address is the reduction of barriers against the access to these means for prevention of HIV and Herpes virus infections. Moreover, universal access to antiretroviral therapy by the Brazilian National Health System (SUS) and the early diagnosis and treatment enable the immunity system compatible with life in those people who have HIV infection, remaining the challenge of treatment adherence to prevent Kaposi's sarcoma.
REFERENCES
1. Beral V, Peterman TA, Berkelman RL, Jaffe HW. Kaposi’s sarcoma among persons with AIDS: a sexually transmitted infection? Lancet. 1990 Jan;335(8682):123-8. [ Links ]
2. Feller J, Lemmer J. Insights into pathogenic events of HIV-associated Kaposi’s sarcoma and immune reconstitution syndrome related Kaposi’s sarcoma. Infect Agent Cancer. 2008 Jan;3:1. [ Links ]
3. Monini P, Sgadari C, Toschi E, Barillari G, Ensoli B. Antitumour effects of antiretroviral therapy. Nat Rev Cancer. 2004 Nov;4(11):861-75. [ Links ]
4. Robey RC, Bower M. Facing up to the ongoing challenge of Kaposi's sarcoma. Curr Opin Infect Dis. 2015 Feb;28(1):31-40. [ Links ]
5. Nguyen HQ, Magaret AS, Kitahata MM, Van Rompaey SE, Wald A, Casper C. Persistent Kaposi’s sarcoma in the era of highly active antiretroviral therapy: characterizing the predictors of clinical response. AIDS. 2008 May;22(8):937-45. [ Links ]
6. Nasti G, Martellotta F, Beretta M, Mena M, Fasan M, Di Perri G, et al. Impact of highly active antiretroviral therapy on the presenting features and outcome of patients with acquired immunodeficiency syndrome-related Kaposi’s sarcoma. Cancer. 2003 Dec;98(11):2440-6. [ Links ]
7. Gallafent JH, Buskin SE, De Turk PB, Aboulafia DM. Profile of patients with Kaposi’s sarcoma in the era of highly active antiretroviral therapy. J Clin Oncol. 2005 Feb;23(6):1253-60. [ Links ]
8. Castilho JL, Luz PM, Shepherd BE, Turner M, Ribeiro SR, Bebawy SS, et al. HIV and cancer: a comparative retrospective study of Brazilian and U.S. clinical cohorts. Infect Agent Cancer. 2015 Feb;10:4. [ Links ]
9. Instituto Brasileiro de Geografia e Estatística. Cidades: São Paulo. Brasília: Instituto Brasileiro de Geografia e Estatística; 2016 [citado 2016 set 1] Disponível em: Disponível em: http://www.cidades.ibge.gov.br/xtras/perfil.php?lang=&codmun=355030&search=sao-paulo|sao-paulo . [ Links ]
10. Secretaria Municipal de Saúde (São Paulo). Aids em adultos (com 13 anos ou mais de idade). Bol Epidemiol AIDS, HIV e DST Municipio São Paulo. 2014 jun;18(17): 18-49. [ Links ]
11. Arruda E, Jacome AA, Toscano AL, Silvestrini AA, Rego AS, Wiermann EG, et al. Consensus of the Brazilian Society of Infectious Diseases and Brazilian Society of Clinical Oncology on the management and treatment of Kaposi’s sarcoma. Braz J Infect Dis. 2014 May-Jun;18(3):315-26. [ Links ]
12. Ministério da Saúde (BR). Secretaria de Vigilância em Saúde. Departamento de DST, Aids e Hepatites virais. Aids e DST.Bol Epidemiol AIDS DST. Brasília: Ministério da Saúde; 2011. [ Links ]
13. Corriça TMC, Caldas MLR. Sarcoma de Kaposi em pacientes com Aids: estudo de 20 anos de necropsias em hospital universitário. DST J Bras Doenças Sex Transm. 2009;21(1):9-11. [ Links ]
14. Toscano ALCC, Jamal LF, Tayra A, Polon MC, Gonçalves A. Immunosuppression level at the time of diagnosis of AIDS-defining malignancies in São Paulo State, Brazil. XVIII International AIDS Conference; 2010; Viena. Viena: [World Health Organization; 2010. [ Links ]
15. Chu K, Misinde D, Massaquoi M, Pasulani O, Mwagomba B, Ford N, et al. Risk factors for mortality in AIDS-associated Kaposi sarcoma in a primary care antiretroviral treatment program in Malawi. Int Health. 2010 Jun;2(2):99-102. [ Links ]
16. Ukonu BA, Eze EU, Onunu AN. Comparison of prevalence of Kaposi's sarcoma in HHV8+ e HHV8- HIV infected patients in South-South Nigeria. Glob J Health Sci. 2011 Apr;3(1):231-6. [ Links ]
17. Kouri V, Eng SM, Rodríguez ME, Resik S, Orraca O, Moore PS, et al. Seroprevalence of Kaposi's sarcoma-associated herpesvirus in various populations in Cuba. Rev Panam Salud Publica. 2004 May;15(5):320-5. [ Links ]
18. Suarez-Garcia I, Jarrín I, Iribarren JA, Lopez-Cortez LF, Lacruz-Rodrigo J, Masiá M, et al. Incidence and risk factors of AIDS-defining cancers on a cohort of HIV-positive adults: importance of the definiton of incedent cases. Enferm Infecc Microbiol Clin. 2013 May;31(5):304-12. [ Links ]
19. Engels EA, Biggar RJ, Hall HI, Cross H, Crutchfield A, Finch JL, et al. Cancer risk in people infected with human immunodeficiency virus in the United States. Int J Cancer. 2008 Jul;123(1):187-94. [ Links ]
20. van Leeuwen MT, Vajdic CM, Middleton MG, McDonald AM, Law M, Kaldor JM, et al. Continuing declines in some but not all HIV-associated cancers in Australia after widespread use of antiretroviral therapy. AIDS. 2009 Oct;23(16):2183-90. [ Links ]
21. Prosperi MCF, Cozzi-Lepri A, Castagna A, Mussini C, Murri R, Giacometti A, et al. Incidence of malignancies in HIV-infected patients and prognostic role of current CD4 cell count: evidence from a large Italian cohort study. Clin Infect Dis. 2010 May;50(9):1316-21. [ Links ]
22. Rohner E, Valeri F, Maskew M, Prozesky H, Rable H, Garone D, et al. Incidence rate of Kaposi sarcoma in HIV-infected patients on antiretroviral therapy in Soutern Africa: a prospective multi-cohort study. J Acquir Immune Defic Syndr. 2014 Dec;67(5):547-54. [ Links ]
23. Nasti G, Serraino D, Ridolfo A, Antinori A, Rizzardini G, Zeroli C, et al. AIDS-associated Kaposi´s sarcoma is more aggressive in women: a study of 54 patients. J Acquir Immune Defic Syndr Hum Retrovirol. 1999 Apr;20(4):337-41. [ Links ]
24. Hamarati LB, Wong J. Intrathoracic Kaposi´s sarcoma in women with AIDS. Chets. 2000 Feb;117(2):410-4. [ Links ]
25. Hsieh MC, Wu XC, Andrews PA, Chen VW. Racial and ethnic disparities in the incidence and trends of soft tissue sarcoma among adolescents and young adults in the United States, 1995-2008. J Adolesc Young Adult Oncol. 2013 Sep;2(3):89-94. [ Links ]
26. Long JL, Engels EA, Moore RD, Gebo KA. Incidence and outcomes of malignancy in the HAART era in an urban cohort of HIV-infected individuals. AIDS. 2008 Feb;22(4):489-96. [ Links ]
27. Lima DB, Barbosa A, Cunha EF, Cunha RG, Almeida JP, Gomes VR. Kaposi sarcoma and AIDS: survival study. International Journal of Infectious Diseases. 2010; 14(Suppl 1):e401. [ Links ]
28. Jacobson LP, Yamashita TE, Detels R, Margolick JB, Chmiel JS, Kingsley LA, et al. Impact of potent antiretroviral therapy on the incidence of Kaposi’s sarcoma and non-Hodgkin’s lymphomas among HIV-1-infected individuals. Multicenter AIDS Cohort Study. J Acquir Immune Defic Syndr. 1999 Aug;21 Suppl 1:S34-41. [ Links ]
29. Mocroft A, Kirk O, Clumeck N, Gargalianos-Kakolyris P, Trocha H, Chentsova N, et al. The changing pattern of Kaposi sarcoma in patients with HIV, 1994-2003: the EuroSIDA Study. Cancer. 2004 Jun;100(12):2644-54. [ Links ]
30. Guiguet M, Boué F, Cadranel J, Lang JM, Rosenthal E, Costagliola D, et al. Effect of immunodeficiency, HIV viral load, and antiretroviral therapy on the risk of individual malignancies (FHDH-ANRS CO4): a prospective cohort study. Lancet Oncol. 2009 Dec;10(12):1152-59. [ Links ]
3Toscano ALCC and Tancredi MV contributed to the conception and design of the study, analysis and interpretation of data, discussion of results and drafting of the article. Pinto VM, Pimentel SR, Silva TSB, Ito SMA, Golub J and Silva MH contributed to the study design, analysis and interpretation of data, discussion of results and critical proofreading of the article. All authors have approved the final version of the manuscript and declared to be responsible for all aspects of the study, ensuring its accuracy and integrity.
Received: October 27, 2015; Accepted: July 24, 2016











 texto em
texto em 


