Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Epidemiologia e Serviços de Saúde
versão impressa ISSN 1679-4974versão On-line ISSN 2337-9622
Epidemiol. Serv. Saúde v.26 n.3 Brasília jul./set. 2017
http://dx.doi.org/10.5123/s1679-49742017000300015
ORIGINAL ARTICLE
Procedures of measurement of the body mass in children by community health agents in Macaé, Rio de Janeiro, Brazil, 2010-2011*
1Universidade Federal do Rio de Janeiro, Curso de Nutrição, Macaé-RJ, Brasil
2Fundação Oswaldo Cruz, Departamento de Epidemiologia e Métodos Quantitativos em Saúde, Rio de Janeiro-RJ, Brasil
3Fundação Oswaldo Cruz, Instituto de Comunicação e Informação Científica e Tecnológica em Saúde, Rio de Janeiro-RJ, Brasil
4Universidade do Estado do Rio de Janeiro, Departamento de Epidemiologia, Rio de Janeiro-RJ, Brasil
OBJECTIVE:
to describe the measurement process of the body mass in children under seven years old, assisted by community health agents in primary health care units of the Family Health Strategy, in Macaé-RJ, Brazil.
METHODS:
a descriptive study with community health agents who measured the body mass of children, from August 2010 to August 2011.
RESULTS:
¾ (n=65) of the community health agents from Macaé Primary Health Care were observed in 196 measurements; in 66.8% of measurements, the professionals used domestic scales (p<0.001); 65.3% of the scales were put on uneven floor; the procedure ‘undress the child’ was followed in 18.4% of cases; of those, 72.2% were performed properly (p<0.001).
CONCLUSION:
failures in the technical procedures of measurement were detected, pointing to the need to expand the reflection and discussion on the impact of the measurements, which help determine the nutritional diagnose of children.
Keywords: Anthropometry; Child; Primary Health Care; Epidemiology, Descriptive
Introduction
Food and health surveillance (FHS) has been recommended by international organizations since the 1970s. In Brazil, however, it was implemented only after the consolidation of the Brazilian National Health System (SUS), in 1990.1 In the XXI century, even after more than 25 years since several political and technical devices have been implemented, such as the National Policies of Food and Nutrition2 and Primary Health Care,3 and the recommendations of Protocols of the Food and Health Surveillance System (Sisvan)4 have contributed to the improvement of this subject, the indicators of population coverage are yet low and there are huge fragilities in the technical procedures used.1,4
The technological innovations that have happened since the 2000s allowed Sisvan to become computerized (Sisvan Web) and to receive, continuously, food and health data from all Brazilian municipalities, making the public access to the information easier - by health managers, health professionals, and the general population.5,6 Sisvan Web provides the updated knowledge on the nutritional profile available, which is necessary to subsidize decision making and assess the effectiveness of the measurements implemented. Nevertheless, for the nutritional profile to reflect the reality both in individual and collective levels the collected data must be reliable; the anthropometric measures are among these data.8,9
Given the intense growth during childhood, the monitoring of body mass is essential to detect nutritional disorders.10 Sisvan protocols recommend that children go through anthropometric evaluation which includes, mainly, body mass measurements (in kilograms) and length/height (in centimeters). Once combined with age and sex, these measurements allow the evaluation of the nutritional status, through the construction of the main nutritional indicators in childhood: weight-for-age age; height-for-age; weight-for-height; and body mass index (BMI) for age.1,4 Also, in order to have reliable values of anthropometric measurements, they must be produced by properly qualified professionals in terms of measurement techniques.9,11,12
The literature points out that one of the measurements commonly affected by mistakes made during the evaluation performed by health professionals is the body mass.8,9,13 The inadequate measurement of body mass biases the values obtained, compromising the nutritional diagnosis of both individual and collective and, consequently, the formulation and reorientation of actions and strategies destined to assist the real health and food needs of the population.14
The studies that analyze how the health professionals - including the health community agents (HCA) - perform the measurements of body mass in the Primary Health Care are yet limited. However, there are doubts about the validity of data produced by professionals who are not qualified to collect these measurements.13-15
The present study aimed to describe the procedures of body mass measurement in children under seven years old, assisted by the HCA in primary health care units (PHU) of the Family Health Strategy (FHS) in the municipality of Macaé in Rio de Janeiro, Brazil.
Methods
This is an observational study with descriptive design, conducted from August 2010 to August 2011, in the municipality of Macaé, located in the North region of Rio de Janeiro, with a population estimate, in the year of 2010, of 206,728 inhabitants.16
During the period studied, a total of 85 HCA worked at the PHU (n=25) of the municipality, located both in urban and rural areas. The PHU with poor access were excluded from the study (mainly those located at Serrana Region), as well as those with records of urban violence, for putting in risk the lives and safety of the observers. Thus, 13 PHUs were selected, and all the HCA (n=65) working there were eligible for the study, which corresponded to approximately ¾ of the total HCA working at the PHU of Macaé. All the HCA who performed, in their routines of work, the assessment of body mass in children younger than seven years old, in compliance with Sisvan, and who accepted to participate in the study were included. The measurement was conducted under the supervision of the observers, as the date was scheduled with each unit manager.
The group of the population assisted by the HCA during the measurement of body mass is large and includes all age groups; however, only children under seven years old were selected, due to the biological and social vulnerability4 and intense weight and height development10 to which infants and preschool children usually go through. The measurements of length/height were not included in the HCA duties at the time of the study, reason why they have not been observed.
To collect the data, observers previously trained according to the standards of anthropometric evaluation visited the PHU in two shifts per week, observing one HCA in each shift. Each observer dedicated a maximum of 8 hours per week to field work, to maintain the quality of observation. All steps of measurement of body mass done by the HCA in children younger than seven years old were verified using a standardized instrument (checklist).
The checklist was adapted from Capelli15 and includes the following variables:
a) types of equipment available at the PHU
- mechanical pediatric weighing scale;
- electronic pediatric weighing scale;
- mechanical platform weighing scale;
- domestic electronic weighing scale;
- domestic mechanical weighing scale;
b) adequacy of physical space
- weighing scale positioned near the door (if yes, open or closed door);
- near the window (if yes, open or closed window);
- leaning against the wall (yes or no);
c) weighing scale support (even or uneven); and
d) assessment techniques to measure body mass in children younger than seven years old.
In the routine of body mass measurement done by the HCA, each observer checked the execution of technical procedures and its adequacy or not to the recommendations described in the literature1,4,10 (Figure 1).

Figure 1 - Technical procedures of total body mass measure, according to adequate and inadequate procedures, verified by observers and performed by health community agents of primary health care units from the Family Health Strategy (n=13), in the municipality of Macaé-RJ, August/2010-August/2011
The technical procedures of measurement were displayed in a chart in the checklist; each of its variables was followed by the terms 'performed' and 'properly', with the option to mark 'yes' or 'no' in each item. Only for the variables 'read the value of body mass on the monitor of electronic weighing scale or on the markers of the mechanical weighing scale' and 'wrote down the value of body mass in the file', there was no need to use 'properly' (Figure 1); the observer stayed far from the HCA in order not to disturb the work. At the end of the weighing, the observer verified the level of the floor or the table where the weighing scales was placed, using an aluminum level.
First, a descriptive analysis of the variables was done using the absolute and relative frequencies. Then, Pearson's chi-squared test or Fisher exact test (used with small samples) were performed, since all the variables analyzed were categorical. The statistical significance level adopted was of 1% to all analyses. The computer statistic program SPSS, version 20.0® was used.
In accordance with the Resolution of the National Health Council (CNS), No. 466, dated December, 12th, 2012,17 the participation of the HCA was possible upon explanations about the study and after they signed the Free Informed Term of Consent. The study project was approved by the Research Ethic Committee of the Medical School from Campos dos Goytacazes-RJ: Protocol No. 31856414.0.0000.5244
Results
The 13 PHU selected were visited and all 65 HCA who worked there accepted to participate in the study, and were monitored by the observers at the moment of measurement of body mass of 196 children aged less than seven years old. Table 1 presents the distribution of the HCA and the anthropometric evaluations conducted by them in the PHU.
Table 1 - Distribution of health community agents and children aged less than seven years old (n=196) evaluated at primary health care units from Family Health Strategy (n=13) in the municipality of Macaé-RJ, August/2010 - August/2011
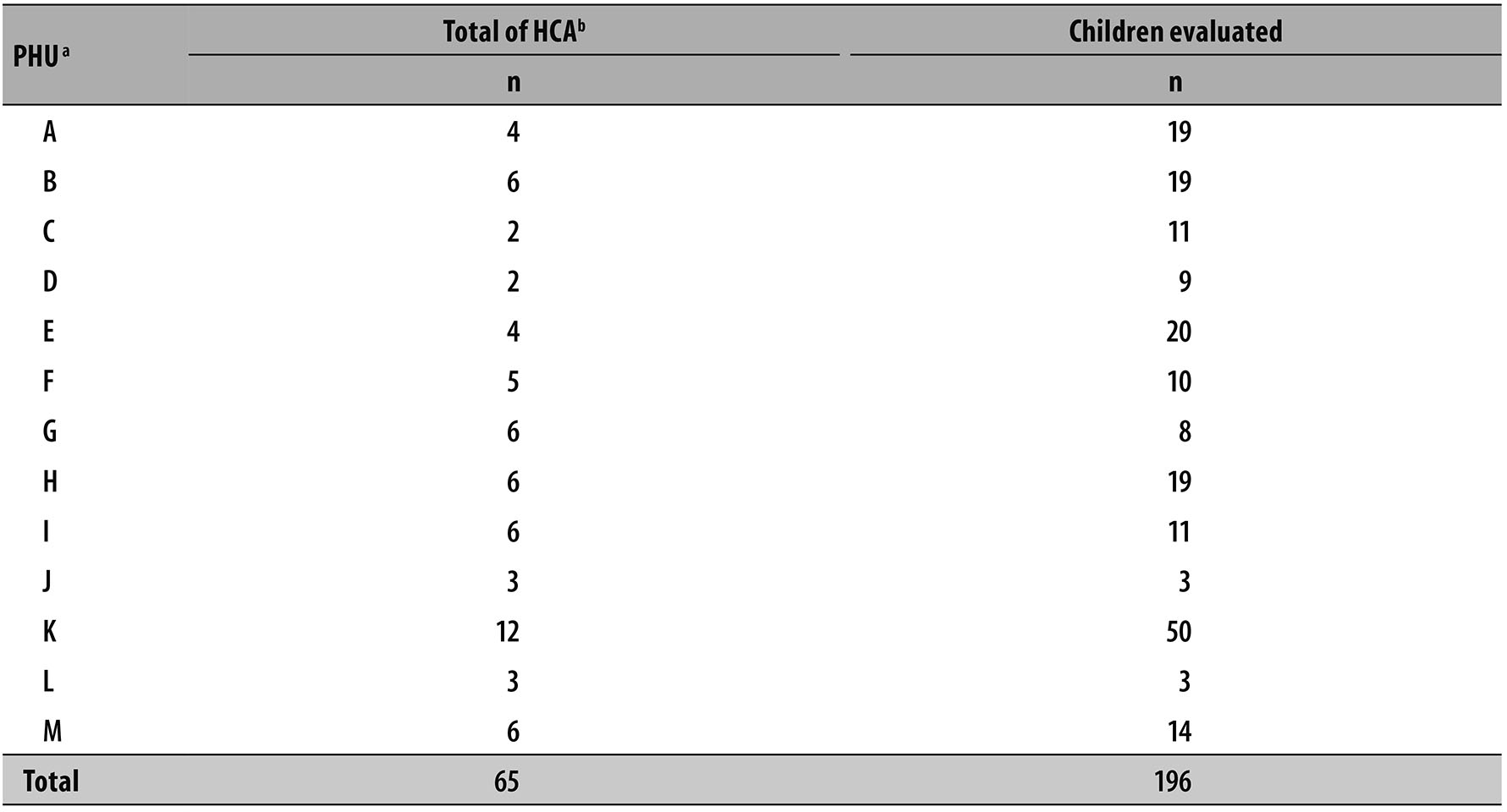
a) PHU: primary health care unit
b) HCA: health community agent
Regarding the kind of weighing scale used by the HCA, 57.4% of the measurement was performed on domestic electronic weighing scales, 23.5% on pediatric mechanical weighing scales, 9.4% on domestic mechanical weighing scales, 9.2% on mechanical platform weighing scales and 0.5% on pediatric electronic weighing scales. The differences observed revealed to be statistic relevant (p<0.001), demonstrating higher use of domestic electronic weighing scales by the HCA, in comparison to the other types of scales.
With regard to where scales were placed, 48.2% were near the door; in those cases, 87.8% of measurements were done with the door opened (p<0.001). There were only 6.5% of scales near the window at the moment of measurement and, in those cases, the procedures were performed with the window closed (p=0.011). Furthermore, 18% of measurements were done with the mechanical platform weighing scale leaning against the wall (p<0.001). About two-thirds of the measurements (65.3%, p<0.001) were performed with equipment the placed on uneven floor (n=190).
Table 2 presents the frequency and adequacy of all the listed technical procedures used for anthropometric measurement. The domestic weighing scales were previously reset in 96.2% of the times. The procedure to align the pointer of the mechanical scales (pediatric and platform/adult), was done in 51.6% of the times, and properly in 87.9% of cases (p<0.001).
Table 2 - Frequency of technical procedures of measurement of body mass, and their adequacy, in children aged less than seven years old, performed by health community agents at primary health care units of the Family Health Strategy in the municipality of Macaé-RJ, August/2010-August/2011
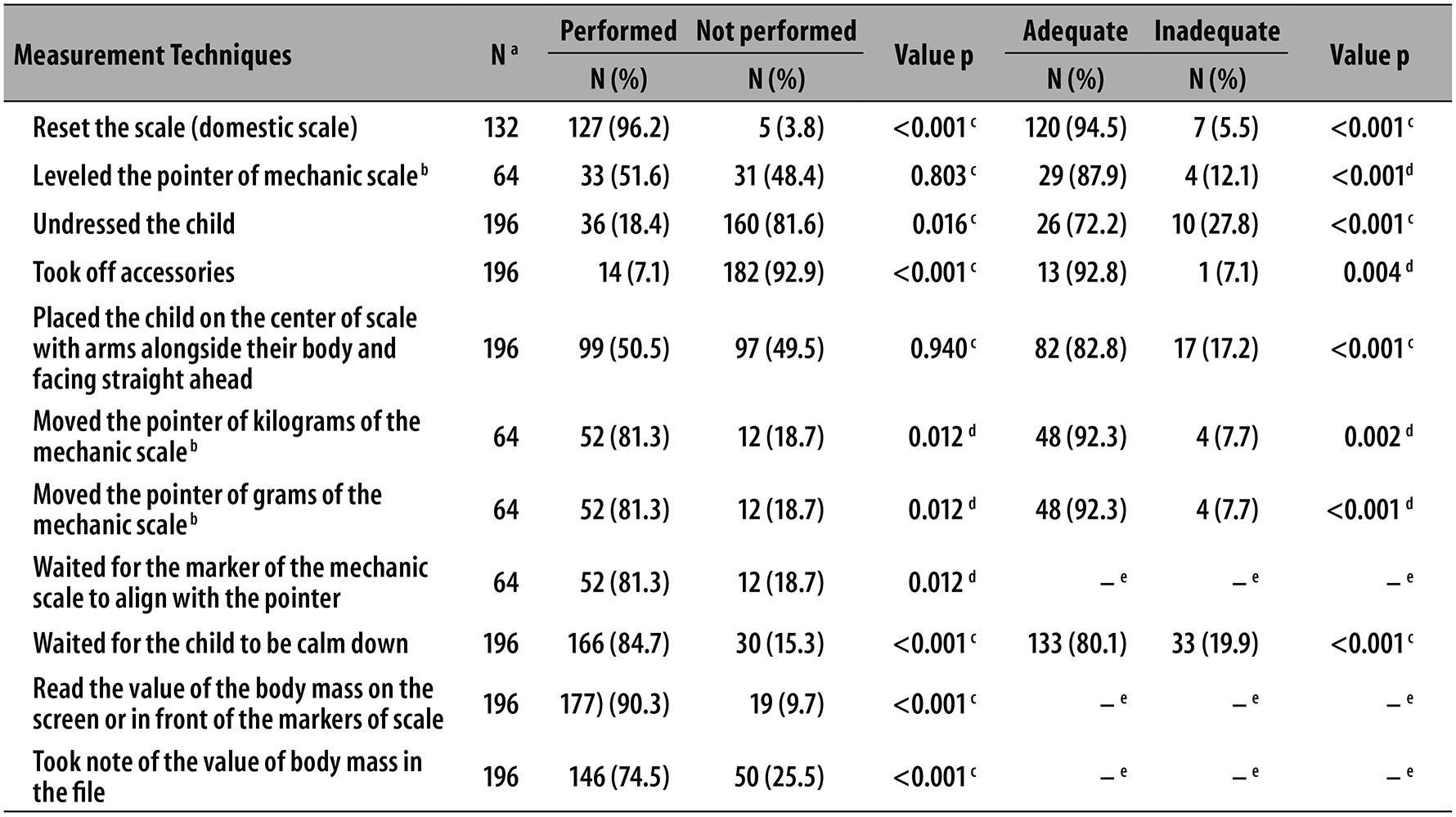
a) Number of children measured - the reduced number of measurements is observed due to the kind of equipment and/or age group of the child measured on the equipment; up to two years old, the scale used is the pediatric one and, for over two years old, the scale used is the adult platform.
b) Pediatric scale or adult platform
c) Pearson's chi-square test
d) Fisher's exact test
e) Does not apply (it was not possible to measure).
The procedure of undressing the child occurred in 18.4% of the measurements, of which, 72.2% were done properly (p<0.001). In 7.1% of the measurements, accessories such as bracelets and hair clips were taken off; in 92.8% of those cases, the procedure was performed properly (Table 2).
The procedure to put the child in the center of the scale with their arms extended alongside their bodies and looking straight ahead was performed in 50.5% of measurements, of which 82.8% were done properly (p<0.001) (Table 2).
Regarding the mechanical weighing scales - pediatric and platform/adult -, where the pointer of kilograms and grams needed to be moved, the HCA paid attention to this detail in 81.3% of the procedures, among which 92.3% were done properly (p=0.002 to pediatric scales and p<0.001 to platform/adult). The same proportion (81.3%) was observed to waiting the marker of the mechanical scales align with the pointer, and 84.7% of the HCA waited for the child to stand still before making the measurements (p<0.001) (Table 2).
The HCA read the values of body mass on the displays or markers of the scales in 90.3% of the times (p<0.001). A quarter of the values of body mass (25.5%, p<0.001) were not properly written down on the child’s health care file (Table 2).
Discussion
In general, this study showed a high proportion of inadequacy in the process of measurement of body mass by the HCA, regarding the analysis of the technical procedures to obtain body mass, the type of scale and where the weighing equipment was placed, when compared to the recommended standards and measurement techniques available in the national and international literatures.10,12,18-20
When we analyzed the type of scale used to measure the children’s body mass, we noticed that more than three-quarters of the scales (mechanical and electronic) were of domestic use and with no quality seal from the National Institute of Metrology, Quality and Technology (Inmetro), which can affect the validity of the measurement. In a study to validate the body mass measurements, destined to assess the nutritional status of adults, the researchers argued that the low validity of body mass index found, provided through referred information could be a result of the use of domestic scales.21
The characteristics of anthropometric equipment have great impact on the quality of measurements. Hence, the use of inadequate equipment or of inferior quality, regardless of the stage of life, might affect the results obtained, resulting in errors of individual and collective nutritional diagnosis.22
The type of scale recommended to obtain children’s body mass should have precision or scale division of 10g. The variation in grams of body mass of an infant and of a child occur constantly, thus, causing small changes in the total body mass value and changing the final result of the nutritional diagnosis.19,23 However, the domestic scales used by the HCA had the precision of 100g, which can lead to a final value of body mass not consistent with reality and, consequently, a wrong nutritional status classification, such as, a child presenting underweight and being diagnosed with adequate weight.6
It is also necessary to use equipment with a quality seal by Inmetro. The producers of this type of equipment must have their products assessed for their accordance to the standards, to ensure their quality.24 It is also important to conduct the metrology inspection of the scale used in health services periodically, to know if the equipment reaches the requirements of maximum errors. The verification expires every one year;25 however, the cost of equipment calibration by Inmetro is high. In this study, we observed that all the scales used were with the Inmetro seal expired, and needed new calibration and inspection. Depending on the quality of measurement made by the equipment,26,27 the manager of the PHU must observe the best period for inspection, possibly biannual or annual.
With regard to the position of the scale, the observers noticed that almost two-thirds of the measurements were done with scales positioned on uneven ground/floor.
The weighing equipment, both the pediatric and platform scales for adults, must be placed on horizontal surface, that is, without slopes, lumps or inclination, avoiding mistakes in the values of the collected measures. The position of scales - on the unleveled ground - by the HCA identified in the present study, constitutes one of the factors capable of contributing with the acquisition of a non-reliable body mass measure.
It was also observed that 18.8% of the scales were placed leaning against the wall, 48.2% were near the door and 6.5% of them were placed near the windows. Likewise, most of the times, the weighing procedures were conducted with the door (87.8%) or the window (90.05) opened. In case the equipment is near the door or window, it may interfere on the leveling of the scale's pointer, on the tare weight of electronic devices, among other effects, given the possible airstream and constant movement of individuals near the equipment, not being indicated, therefore, to be placed near pathways or slots.8,16
In Alagoas, a study conducted from March to July 2006, which aimed to evaluate the reliability of anthropometric data of children obtained from the State Primary Healthcare Network,13 found that 35.9% of the mechanic weighing platform scales and 26.5% of pediatric mechanic scales were positioned inadequately. The inadequacy found in Macaé is high when compared with the study in Alagoas.13
With regard to measuring techniques, it was observed that the procedure to level the pointer of the scale - recommended to be done or verified whenever there is a new weighing - was not performed in 48.4% of the cases. Other procedures that called attention for the lower percentage were (i) undress the child, (ii) take off accessories and (iii) put the child in the center of the scale with arms extended alongside their body and looking straight ahead; they were performed, respectively, 18.4%, 7.1% and 50.5% of times. These findings might interfere negatively with the final result of body mass measurement and, consequently, with the nutritional diagnosis from the indicators, especially in children younger than two years old.
A study that aimed to evaluate the quality of values of body mass measure in Municipal Health Care Units in Rio de Janeiro in 1996,28 among children under five years old, detected that the procedure to level the pointer was done in 21.9% of the times.28 In the municipality of Macaé, we observed a higher proportion for this procedure (51.6%), closer to the reality observed in a study conducted in Alagoas,13 where about 50% of measurements had this procedure.
That study also detected that 75.7% of the healthcare professionals (most of them, nursing assistants) undressed the child before the measurement;28 the same study highlighted that when this procedure was not done, the professionals, most of the times, informed that it was not necessary to undress the child.28
The present study detected a bigger concern of the HCA to perform the procedure of undressing the younger children. This was statistically confirmed, through t-Student test: the children undressed properly, before the weighing, presented an average age of 24.6 months old (Standard Error = 5.3), whilst for those who were submitted to this procedure, or to whom it was not performed properly, they were on average 44.7 months old (Standard Error = 1.8).
The results of the research conducted in the municipality of Alagoas13 pointed to a high proportion of false-negatives to malnutrition in the index of weight-for-age (38.5%), which shows a notorious underestimation of the prevalence of malnutrition. The immediate consequence of this finding is the lack of proper attention to children who suffer from malnutrition and are wrongly diagnosed. Such fact happened, mainly, due to the wrong procedure of undressing the child before weighing.
It is possible that even small "quantities" of additional mass to a child's body, at the moment of measurement of body mass, might cause changes in the value of their weight (in kg) and, consequently, in the final nutritional diagnosis. It is possible that in Macaé, the mistake on classifying the nutritional status might affect some of the evaluated children.
With regard to the procedure ‘put the child in the center of the scale to weigh’, the study conducted in Rio de Janeiro28 showed that in 99.0% of measurements this procedure was carried out, whilst the present study obtained a smaller percentage, reaching less than half. Nonetheless, there is also the fact that 25.4% of the HCA have not written down on the health care file the value of body mass immediately after reading it on the equipment.
In general, during the anthropometric measurement procedure, it is essential to pay close attention both to the production procedure and to the information record,26 as both have potential to interfere with the nutritional diagnosis results. The most common mistakes were related to the lack of attention to the performance of technical procedures of measurement or information record, inadequate use of instruments (such as tables and charts), bad maintenance of equipment or lack of supervision of qualified professionals, not to mention the periodic staff refresher courses.9,29
Refresher courses for professionals in charge of anthropometric measurements in health services is necessary and must be done continuously.9 These professionals must be precise, that is, capable of obtaining equal or close enough values in different measures done in one person; and accurate, that is, able to obtain values equal to the real value. Professionals with low precision or accuracy on these measurements can lead to errors on the "estimates of nutritional disorders", resulting in harm to individuals and to the collectivity, such as, for instance, deprive ill patients from receiving specialized treatment.9 The health professional properly qualified will be sensible and conscious about the importance of the information to be collected;9 and will provide reliable data during their routine, updating the health information systems, which are widely used by managers on the development of nutritional indicators that can truly describe the nutritional profile of the population.2,30
A possible limitation of the present study is the potential information bias. To obtain the data, the observers followed the activity routine of the HCA, which might make health professionals change their behavior during the activity; for example, being more attentive to procedures due to the presence of an observer and evaluator of their work. A difficulty found by the teams of Family Health Strategy, within the period of study, was the intense staff turnovers, and all the information obtained reflect this reality of the health community agent. Another limitation was logistic, given the impossibility to include the rural area in the study, neither the units located in violent urban areas, not being possible to understand the reality of body mass measurements by the HCA in those localities.
Nonetheless, a favorable aspect of the study was the previous knowledge that, during the research period, the training of professionals - performed in a single day - was done before the activity started, incorporating to their work routine all the attributions of measurement of children body mass. The training course on measurement techniques was not detailed: the professionals learned about the basic procedures and equipment. In the municipality of Macaé, the professionals were going through another annual training course, called "refresher", and the subject were the measurement techniques and form filling. In the period of study, the professionals had not yet participated in the "refresher" and the equipment had not been assessed by Inmetro since their acquisition.
The need for acquisition and maintenance of equipment, and the promotion of continuous training of HCA, at least twice a year, in the field of anthropometrics are evident.
By observing inadequacies on the process of body mass measurement by health community agents, the present study brings up the discussion about the importance of accuracy of nutritional diagnosis of individuals and the society, and reinforces the need for a reflection about the impact of this measure on children assisted at primary health care units of the studied municipality, as well as in other municipalities of the country. This kind of research is justified, considering that the information produced by health professionals is used to subsidize the planning and development of public policies on food and nutrition, aiming to provide a better health and nutritional epidemiological panorama of the population assisted.2,9,30
Acknowledgments
To the health manager Michel Haddad, from the Municipal Department of Health of Macaé. To the health manager, nutritionist Carine Lime, and to the nutritionist Carolina da Costa Pires, from the Coordination of Technical Area of Food and Nutrition of the municipality of Macaé, for authorizing the research and disclosure of its results.
REFERENCES
1. Ministério da Saúde (BR). Vigilância alimentar e nutricional - Sisvan: orientações básicas para a coleta, processamento, análise de dados e informação em serviços de saúde. Brasília: Ministério da Saúde; 2004. (Série A. Normas e Manuais Técnicos). [ Links ]
2. Ministério da Saúde (BR). Secretaria de Atenção à Saúde. Departamento de Atenção Básica. Política Nacional de Alimentação e Nutrição. Brasília: Ministério da Saúde; 2013. [ Links ]
3. Ministério da Saúde (BR). Secretaria de Atenção à Saúde. Departamento de Atenção Básica. Política Nacional de Atenção Básica. Brasília: Ministério da Saúde; 2012. (Série E. Legislação em Saúde). [ Links ]
4. Ministério da Saúde (BR). Secretaria de Atenção à Saúde. Departamento de Atenção Básica. Protocolos do Sistema de Vigilância Alimentar e Nutricional - SISVAN na assistência à saúde. Brasília: Ministério da Saúde; 2008. (Série B. Textos Básicos de Saúde). [ Links ]
5. Rocha CMM, Capelli JCS, Almeida MFL. Sisvan Web. In: Capelli JCS, Ribeiro BG, Rocha CMM, Almeida MFL, organizadores. Avaliaçao nutricional de crianças e adolescentes: antropometria e reflexões sobre o diagnóstico em saúde a partir da prática do profissinal na atenção básica. Macaé, RJ: FUNEMAC; 2015. p. 41-4. [ Links ]
6. Ministério da Saúde (BR). Secretaria de Atenção à Saúde. Departamento de Atenção Básica. Marco de referência da vigilância alimentar e nutricional na atenção básica. Brasília: Ministério da Saúde; 2015. [ Links ]
7. Lima CRA, Schramm JMA, Coeli CM, Silva MEM. Revisão das dimensões de qualidade dos dados e métodos aplicados na avaliação dos sistemas de informação em saúde. Cad Saude Publica. 2009 out;25(10):2095-109. [ Links ]
8. Campos EJE, Ribeiro BG, Capelli JCS. Medidas Antropométricas: medidas e procedimentos. In: Capelli JCS, Ribeiro BG, Rocha CMM, Almeida MFL, organizadores. Avaliaçao nutricional de crianças e adolescentes: antropometria e reflexões sobre o diagnóstico em saúde a partir da prática do profissinal na atenção básica. Macaé, RJ: Funemac; 2015. p. 33-40. [ Links ]
9. Bagni UV, Barros DC. Capacitação em antropometria como base para o fortalecimento do Sistema de Vigilância Alimentar e Nutricional no Brasil. Rev Nutr. 2012 mai-jun;25(3):393-402. [ Links ]
10. Barros DC. SISVAN: instrumento para o combate aos distúrbios nutricionais na atenção à saúde: a antropometria. 2 ed. Rio de Janeiro: Fundação Oswaldo Cruz; 2010. [ Links ]
11. Barros DC, Felipe GC, Silva JP. Antropometria. In: Barros DC, Silva DO, Gugelmin SA, organizadores. Vigilância alimentar e nutricional para a saúde indígena. Rio de Janeiro: Fundação Oswaldo Cruz; 2008. p. 33-74. [ Links ]
12. World Health Organization. Physical Status: the use and interpretation of anthropometry. Geneva: World Health Organization; 1995. (Techinical Report Series, 854). [ Links ]
13. Lima MAA, Oliveira MAA, Ferreira HS. Confiabilidade dos dados antropométricos obtidos em crianças atendidas na Rede Básica de Saúde de Alagoas. Rev Bras Epidemiol. 2010 mar;13(1):69-82. [ Links ]
14. Bagni UV, Fialho-Júnior CC, Barros DC. Influência do erro técnico de medição em antropometria sobre o diagnóstico nutricional. Nutrire Rev Soc Bras Aliment Nutr. 2009 dez;34(3):187-200. [ Links ]
15. Capelli JCS. Qualidade do valor da medida de massa corporal nos Centros Municipais de Saúde do Município do Rio de Janeiro, 1996. [dissertação]. 1996. Recife: Instituto Materno Infantil de Pernanbuco;1998. [ Links ]
16. Instituto Brasileiro de Geografia e Estatística. Macaé. Rio de Janeiro. Cidades [Internet]. Rio de Janeiro: Instituto Brasileiro de Geografia e Estatística; 2016 [citado 2016 mai 22]. Disponível em: Disponível em: http://cidades.ibge.gov.br/xtras/perfil.php?codmun=330240 . [ Links ]
17. Brasil. Resolução nº 466, de 12 de dezembro de 2012. Diário Oficial da República Federativa do Brasil, Brasília (DF), 2013 jun 13;Seção 1:59. [ Links ]
18. Ministério da Saúde (BR). Secretaria de Atenção à Saúde. Departamento de Atenção Básica. Orientações para a coleta e análise de dados antropométricos em serviços de saúde: Norma Técnica do Sistema de Vigilância Alimentar e Nutricional - SISVAN. Brasília: Ministério da Saúde; 2011. (Série G. Estatística e Informação em Saúde). [ Links ]
19. Gibson RS. Anthropometric reference data. In: Gibson RS, organizador. Principles of nutritional assessment. New York: Oxford University Press; 1990. Pt.12. p.209-46. [ Links ]
20. Lohman TG, Roche AF, Martorell R. Anthropometric standardization reference manual. Illinois: Human Kinetics; 1988. [ Links ]
21. Silveira EA, Araújo CL, Gigante DP, Barros AJD, Lima MS. Validação do peso e altura referidos para o diagnóstico do estado nutricional em uma população de adultos no Sul do Brasil. Cad Saude Publica. 2005 jan-fev;21(1):235-45. [ Links ]
22. Bagni UV, Barros DC. Especificações de equipamentos antropométricos para estabelecimentos de saúde: para estabelecimentos de saúde. Rio de Janeiro: Ministério da Saúde; Fundação Oswaldo Cruz; 2011. [ Links ]
23. Ministério da Saúde (BR). Secretaria de Atenção à Saúde. Departamento de Atenção Básica. Coordenação-Geral de Alimentação e Nutrição. Manual orientador para aquisição de equipamentos antropométricos: portaria nº 2.975, de 14 de dezembro de 2011. Brasília: Ministério da Saúde; 2012. [ Links ]
24. Instituto Nacional de Metrologia, Qualidade e Tecnologia. Avaliação da conformidade [Internet]. Brasília: Instituto Nacional de Metrologia, Qualidade e Tecnologia; 2012 [citado 2015 jun 15]. Disponível em: Disponível em: http://www.inmetro.gov.br/qualidade/definicaoAvalConformidade.asp . [ Links ]
25. Instituto Nacional de Metrologia, Qualidade e Tecnologia. Serviços prestados pela Metrologia Legal [Internet]. Brasília: Instituto Nacional de Metrologia, Qualidade e Tecnologia ; 2012 [citado 2015 jun 15]. Disponível em: Disponível em: http://www.inmetro.gov.br/metlegal/servicoApreciacao.asp [ Links ]
26. Barros DC, Silva DO, Bagni UV, Veggi A. O diagnóstico nutricional na atenção básica. In: Barros DC, Silva DO, Santos MMAS, Baião MR, organizadores. Alimentação e nutrição: fundamentos para a prática em saúde coletiva. Rio de Janeiro: Editora Fiocruz; 2013. p.127-222. [ Links ]
27. Instituto Nacional de Metrologia, Qualidade e Tecnologia. Vocabulário Internacional de Termos Fundamentais e Gerais de Metrologia. Duque de Caxias: Instituto Nacional de Metrologia, Qualidade e Tecnologia; 1995. [ Links ]
28. Capelli JCS, Anjos LA, Castro IRR. Qualidade do valor da medida de massa corporal nos Centros Municipais de Saúde do Município do Rio de Janeiro, 1996. Cad Saude Publica. 2002 jan-fev;18(1):63-70. [ Links ]
29. Silva DO, Engstrom EM, Zaborowski EL. Sisvan: instrumento para o combate aos distúrbios nutricionais de saúde: o diagnóstico coletivo. Rio de Janeiro: Fundação Oswaldo Cruz; 2002. [ Links ]
30. Correia LOS, Padilha BM, Vasconcelos SML. Métodos para avaliar a completitude dos dados dos sistemas de informação em saúde do Brasil: uma revisão sistemática. Cien Saude Colet. 2014 nov;19(11):4467-78. [ Links ]
Received: July 11, 2016; Accepted: February 02, 2017











 texto em
texto em 
 Curriculum ScienTI
Curriculum ScienTI

