Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Epidemiologia e Serviços de Saúde
versão impressa ISSN 1679-4974versão On-line ISSN 2237-9622
Epidemiol. Serv. Saúde vol.28 no.1 Brasília mar. 2019 Epub 24-Jan-2019
http://dx.doi.org/10.5123/s1679-49742019000100001
ORIGINAL ARTICLE
Hospitalization for ambulatory care-sensitive conditions in the state of Rondônia, Brazil: a descriptive study of the period 2012-2016
1Faculdade de Ciências Biomédicas de Cacoal, Cacoal, RO, Brasil
Objective:
to describe the frequency and reasons for hospitalizations for ambulatory care-sensitive conditions (HACSC) in Rondônia, Brazil, between 2012 and 2016, and to analyze their relationship with the evolution of the coverage of the family health strategy (FHS) in the same period.
Methods:
this was a descriptive study of secondary data from the Brazilian National Health System’s Hospital Information System.
Results:
during the period of the study 133,958 HACSC were authorized, corresponding to a rate of 75 hospitalizations/1,000 inhab.; there was a parallel annual increase in FHS coverage and a slightly decreasing trend of authorized HACSC, although this was not statistically significant; in 2012, HACSC frequency was 20.7% in relation to all hospitalizations that occurred in the state, while in 2016 this indicator declined to 16.7%.
Conclusion:
HACSC frequency in Rondônia was high between 2012 and 2016; although there was an increase in FHS coverage in the same period, this increase was not accompanied by a significant change in the frequency of HACSC registered in the state.
Keywords: Primary Health Care; Family Health Strategy; Epidemiology, Descriptive
Introduction
The primary level of health care (PHC) has the capacity to respond to 75 to 85% of the health needs of a community. This level of care is expected to be the entry point to the health service to meet all new health needs and problems of the population. It is also expected to provide care to people over the course of time, to care for the majority of health conditions - except very uncommon or rare conditions - and to coordinate or integrate care provided at other points in the health care network.1
Evaluating PHC quality is fundamental for the management of its organization and practice, in the quest for excellent performance at this level of care. To this end indicators are used, these being succinct measures of relevant information not only about certain attributes and dimensions of the health situation, but also about the performance of the health system.2-4
Ambulatory Care Sensitive Conditions (ACSC) are health conditions for which effective PHC actions can reduce the risk of hospitalization.3 Activities focused on early diagnosis and proper treatment of acute diseases, control and monitoring of chronic conditions, will have a direct impact on reducing the incidence of common diseases and, consequently, ACSC as well.4
With effect from the 1980s, hospitalizations for ambulatory care-sensitive conditions (HACSC) began to be considered as an indicator that enables evaluation of the first level of health care. Reduction in hospitalizations due to ACSC is a reflection of effective care and case management in PHC.3
In 2008, the Brazilian Ministry of Health established the first Brazilian list of ACSC by means of Ordinance SAS/MS No. 221, dated 17 April 2008. This list includes 120 three-digit categories and 15 four-digit subcategories taken from the International Statistical Classification of Diseases and Related Health Problems 10th Revision (ICD-10), grouped together in accordance with the possibility of interventions and disease magnitude, thus resulting in 19 diagnostic groups. The Brazilian ASCS list was drawn up based on consensus between researchers and health service managers, including the establishment of the use of the HACSC indicator for evaluating and monitoring the health care system through a single instrument.5 Despite its limitations, usually attributed to regional differences in installed health service capacity, prudent use of the HACSC indicator can help to increase PHC effectiveness, by identifying priority areas for intervention and making evident health problems that need better follow-up and coordination between levels of care.6,7
While reductions in HACSC proportions or rates suggest possible improvements in PHC, when these rates are high this is not always indicative of deficiencies in primary care, but rather a warning signal that in-depth investigation is needed in the places where they occur.8 Patients’ characteristics, variability in the criteria used to indicate the need for hospitalization and the admission policies of tertiary care centers are some of the variables capable of contributing to increases or decreases in the HACSC indicator.9
Information about HACSC may inform objective analysis of the health situation in a given locality or region, with a view to evidence-based decision-making and the proposition of health actions more aligned with the needs of the population. Considering national and state-level public health policies, especially the need for PHC organization and evaluation in emerging areas of Brazil, the study of HACSC frequency and characterization in Rondônia proposed here is justified. It is expected that this knowledge can contribute to the construction of a quality Brazilian National Health System (SUS) in that state. The objective of this study was therefore to describe the profile of HACSC in Rondônia, between 2012 and 2016, as a preliminary proposal to provide information on the quality of state-level PHC there.
Methods
An ecological study was conducted taking the unit of analysis to be hospitalizations throughout the state of Rondônia in the period between 2012 and 2016, recorded on the Brazilian National Health System Hospital Information System (SIH/SUS). Rondônia is located in the Northern Brazilian region, occupies an area of 237,576 km² and comprises 52 municipalities inhabited by 1,787,279 people.10 All the hospitalizations that occurred in the state between 2012 and 2016 were eligible for this study, while analysis was performed on those cases admitted to hospital because their primary diagnosis was that of a condition found on the list of ACSCs.5 In parallel, an analysis was made of the situation of the Family Health Strategy (FHS) coverage in all the state’s municipalities, using data provided by the Brazilian Ministry of Health’s Department of Primary Health Care which were representative of an estimated proportion of FHS team population coverage in a defined territory.6 The health conditions considered for HACSC were based on the Brazilian list of ACSC as defined by Ordinance SAS/MS Nº 221/2008.5 Data related to population of the state of Rondônia in 2016 were obtained from the Brazilian Institute of Geography and Statistics (IBGE) website.10
In order to initially identify HACSC, a SIH/SIS spreadsheet was generated based on the selection of the causes of hospital admissions according to their respective ICD-10 code. We used Tabwin version 3.5, developed by the Brazilian National Health System Information Technology Department (DATASUS) to convert the database formats;11 we then tabulated and analyzed the data using EpiData version 2.2.3.
In addition to causes of hospitalization and FHS coverage, we also analyzed other relevant information found on the Hospital Admission Authorization forms (IHA-SUS) in order to obtain the demographic characterization of the patients: sex, age, ethnicity/skin color and municipality of residence. The specific characteristics of HACSC analyzed were the year when hospitalization occurred, medical specialty under which the patient was hospitalized, nature of hospitalization (whether elective or emergency), length of inpatient stay, need for intensive treatment and evolution to death.
Initially, we described HACSC frequency in relation to all hospitalizations that occurred during the period and the evolution of FHS coverage for Rondônia state and all its municipalities. We also calculated the proportion of HACSC in relation to all hospitalizations that occurred during the period, for the state of Rondônia and its municipalities, as well as the HACSC rate (per 1,000 inhab.). The hospitalization rate was calculated by dividing the number of HACSC by the population estimated by IBGE for 2016. Subsequently, the demographic and clinical characteristics of the patients were summarized. We carried out ecological analysis with the aim of assessing the relationship between HACSC frequency from 2012-2016 and the evolution of FHS coverage in the same period. To this end, Spearman's correlation coefficient was determined based on an alpha error of 0.05.
The study project was not submitted to the appraisal of a Research Ethics Committee because it was based on secondary public domain data, in accordance with National Health Council Resolution CNS/MS No. 510, dated 7 April 2016. Notwithstanding, the rules in force relating to ethics in research with human beings in Brazil were complied with. The data were analyzed specifically for this research in a global manner, without any individual identification of persons registered on the hospital admissions information system.
Results
Between January 2012 and December 2016, 133,958 hospitalizations for ambulatory care-sensitive conditions in SUS public health services and outsourced services were notified in the state of Rondônia. HACSC accounted for 24.8% of all SUS hospitalizations recorded in the state in the period analyzed. Of the hospitalizations analyzed, 62,994 (47.0%) were male and 70,964 (53.0%) were female. Elderly patients (39.6%) and adults between 20 and 49 years old (26.4%) comprised the majority of these hospitalizations. Patients’ mean age was 38.4 (standard deviation [SD]=38.3) years. Although information on ethnicity/color had been omitted for a large proportion (58.4%) of patients, brown skin color was the most frequently (31.6%) recorded for the remaining HACSC (Table 1).
Table 1 - Frequency, Family Health Strategy coverage and demographic characteristics of patients hospitalized for ambulatory care sensitive conditions, Rondônia, 2012-2016
| Characteristics | N | % |
|---|---|---|
| Yeara | ||
| 2012 | 27,695 | 20.7 |
| 2013 | 28,359 | 21.2 |
| 2014 | 29,860 | 22.3 |
| 2015 | 25,687 | 19.2 |
| 2016 | 22,357 | 16.7 |
| Total period | 133,958 | 24.8 |
| FHS Coverageb | - | |
| 2012 | - | 60.4 |
| 2013 | - | 63.1 |
| 2014 | - | 68.7 |
| 2015 | - | 70.9 |
| 2016 | - | 71.3 |
| Total for the state | - | 66.9 |
| Sex | ||
| Male | 62,994 | 47.0 |
| Female | 70,964 | 53.0 |
| Age (in years) | ||
| Mean (SDc) | 38.4 (38.3) | |
| Median (Q1;Q3) | 36.0 (10.0;64.0) | |
| Age group (in years) | ||
| 0-4 | 19,788 | 14.8 |
| 5-9 | 12,469 | 9.3 |
| 10-19 | 13,343 | 10.0 |
| 20-49 | 35,354 | 26.4 |
| 50-100 | 53,004 | 39.6 |
| Ethnicity/skin color | ||
| White | 8,902 | 6.6 |
| Black | 1,186 | 0.9 |
| Brown | 42,376 | 31.6 |
| Asian | 983 | 0.7 |
| Indigenous | 2,265 | 1.7 |
| No information | 78,246 | 58.4 |
a) proportion of hospitalizations for ambulatory care-sensitive conditions (HACSC) in relation to total of hospitalized patients.
b) FHS: Family Health Strategy.
c) SD: standard deviation.
FHS coverage was 66.9% for the state of Rondônia as a whole, progressing from 60.4% in 2012 to 71.3% in 2016 (Table 1). However, this service had still not been implanted in two municipalities; eight municipalities had 100% FHS coverage ; while in the remaining municipalities FHS coverage varied considerably, from 35.8 to 100%. The municipalities of Porto Velho (11.4%), Ji-Paraná (8.3%), Rolim de Moura (6.6%), Cacoal (5.9%) and Vilhena (5.2%) were those that most recorded HACSC in the period, totaling 37.4% of all hospitalizations (Table 2). The HACSC rate per municipality varied from 21.8/1,000 to 228.9/1,000 inhab. in the period, being higher in the municipalities of Cerejeiras (228.9/1,000 inhab.), Santa Luzia d' Oeste (198.0/1,000 inhab.), Alta Floresta d'Oeste (197.0/1,000 inhab.), Cabixi (190.1/1,000 inhab.) and Novo Horizonte do Oeste (157.0/1,000 inhab.). For the state of Rondônia as a whole, the hospitalization rate due to HACSC was 75.0/1,000 inhab. in the period analyzed (Table 2).
Table 2 - Distribution, per municipality of residence, of the Family Health Strategy coverage, number and rate of hospitalizations for ambulatory care-sensitive conditions, Rondônia, 2012-2016
| Municipality of residence | FHSa coverage in 2016 (%) | HACSCb | Population in 2016 | HACSC rate (per 1,000 inhab.) | |
|---|---|---|---|---|---|
| N | % | ||||
| Alta Floresta d’Oeste | 68.6 | 5,025 | 3.8 | 25,506 | 197.0 |
| Alto Alegre dos Parecis | 91.7 | 2,082 | 1,6 | 13,993 | 148.8 |
| Alto Paraíso | 83.9 | 1,496 | 1.1 | 20,569 | 72.7 |
| Alvorada d’Oeste | 100.0 | 1,554 | 1.2 | 16,902 | 91.9 |
| Ariquemes | 55.3 | 5,422 | 4.0 | 105,896 | 51.2 |
| Buritis | 62.8 | 1,719 | 1.3 | 38.450 | 44.4 |
| Cabixi | 97.5 | 1,196 | 0.9 | 6,289 | 190.1 |
| Cacaulândia | 90.3 | 421 | 0.3 | 6,414 | 65.6 |
| Cacoal | 70.6 | 7,910 | 5.9 | 87,877 | 90.0 |
| Campo Novo de Rondônia | 89.5 | 1,634 | 1.2 | 14,354 | 113.8 |
| Candeias do Jamari | 84.1 | 758 | 0.6 | 24,719 | 30.6 |
| Castanheiras | 97.1 | 259 | 0.2 | 3,583 | 72.2 |
| Cerejeiras | 93.8 | 4,112 | 3.1 | 17,959 | 228.9 |
| Chupinguaia | - | 423 | 0.3 | 10.364 | 40.8 |
| Colorado do Oeste | 92.5 | 2,772 | 2.1 | 18,639 | 148.7 |
| Corumbiara | 98.5 | 365 | 0.3 | 8,659 | 42.1 |
| Costa Marques | 82.5 | 777 | 0.6 | 17,400 | 44.6 |
| Cujubim | 47.6 | 583 | 0.4 | 21,720 | 26.4 |
| Espigão d’Oeste | 73.8 | 3,371 | 2.5 | 32.712 | 103.0 |
| Governador Jorge Teixeira | 100.0 | 963 | 0.7 | 9,933 | 96.9 |
| Guajará-Mirim | 72.2 | 5,902 | 4.4 | 47,048 | 125.4 |
| Itapuã do Oeste | 66.9 | 225 | 0.2 | 10.310 | 21.8 |
| Jaru | 37.1 | 5,334 | 4.0 | 55,806 | 95.5 |
| Jí-Paraná | 76.0 | 11,117 | 8.3 | 131.560 | 84.5 |
| Machadinho d’Oeste | 72.8 | 2,194 | 1.6 | 37,899 | 57.9 |
| Ministro Andreazza | 94.6 | 1,396 | 1.0 | 10,786 | 129.4 |
| Mirante da Serra | 84.1 | 1,430 | 1.1 | 12,308 | 116.2 |
| Monte Negro | 89.2 | 1,805 | 1.3 | 16,032 | 112.6 |
| Nova Brasilândia d’Oeste | 79.6 | 3,191 | 2.4 | 21,670 | 147,2 |
| Nova Mamoré | 73.3 | 2,119 | 1.6 | 28,255 | 75.0 |
| Nova União | 88.5 | 555 | 0.4 | 7,796 | 71.2 |
| Novo Horizonte do Oeste | 67.9 | 1,595 | 1.2 | 10,161 | 157.0 |
| Ouro Preto do Oeste | 86.6 | 5,364 | 4.0 | 39,840 | 134.6 |
| Parecis | 86.0 | 581 | 0.4 | 5.802 | 100.1 |
| Pimenta Bueno | 63.9 | 4,562 | 3.4 | 37,786 | 120.7 |
| Pimenteiras do Oeste | - | 310 | 0.2 | 2.410 | 128.6 |
| Porto Velho | 54.0 | 15,258 | 11.4 | 511,219 | 29.8 |
| Presidente Médici | 92.6 | 2,301 | 1.7 | 22,337 | 103.0 |
| Primavera de Rondônia | 98.5 | 289 | 0.2 | 3,456 | 83.6 |
| Rio Crespo | 88.1 | 129 | 0.1 | 3,829 | 33.7 |
| Rolim de Moura | 79.1 | 8,861 | 6.6 | 56,664 | 156.3 |
| Santa Luzia d’Oeste | 100.0 | 1,655 | 1.2 | 8,362 | 198.0 |
| São Felipe d’Oeste | 97.7 | 256 | 0.2 | 5,994 | 42.7 |
| São Francisco do Guaporé | 100.0 | 1,397 | 1.0 | 16,636 | 84.0 |
| São Miguel do Guaporé | 53.5 | 2,444 | 1.8 | 19,353 | 126.2 |
| Seringueiras | 100.0 | 1,025 | 0.8 | 11,619 | 88.2 |
| Teixeirópolis | 100.0 | 470 | 0.4 | 4,778 | 98.3 |
| Theobroma | 100.0 | 569 | 0.4 | 10,575 | 53.8 |
| Urupá | 81.6 | 633 | 0.5 | 12,687 | 49.9 |
| Vale do Anari | 35.8 | 431 | 0.3 | 9,633 | 44.74 |
| Vale do Paraíso | 100.0 | 798 | 0.6 | 7,961 | 100.2 |
| Vilhena | 84.6 | 6,920 | 5.2 | 93,745 | 73.8 |
| Rondônia | 66.9 | 133,958 | 100.0 | 1,787,279 | 75.0 |
a) FHS: Family Health Strategy.
b) HACSC: hospitalizations for ambulatory care-sensitive conditions.
The municipality of Porto Velho, which had low FHS coverage (54.0%), had a high proportion (11.4%) of HACSC in the period. However, municipalities with total FHS coverage (100%) were found, in general, to have low proportions (<1.5%) of HACSC in the period. Notwithstanding, the HACSC rate was not aligned with FHS coverage in the state: for example, municipalities with 100% FHS coverage, such as Alvorada d'Oeste, Governador Jorge Teixeira, Santa Luzia d'Oeste, Teixeirópolis and Vale do Paraíso had HACSC rates above 90/1,000 inhab. in the period analyzed (Table 2).
The annual percentage rate of hospital admissions showed a progressive reduction in the period studied, being 16.2, 16.4, 17.1, 14.5 and 12.5 per 1,000 inhab. in 2012, 2013, 2014, 2015 and 2016, respectively (Table 3). Although a progressive decrease in the HACSC proportion was seen in the five years analyzed (Table 1), this reduction was not statistically correlated to the elevation of global FHS coverage in the state (Spearmans correlation coefficient = -0.60; p = 0.285) (Figure 1).
Table 3 - Hospitalizations for ambulatory care-sensitive conditions according to hospitalization year and causes, Rondônia, 2012-2016
| Year/Cause | N | Rate (per 1,000 inhab.) |
|---|---|---|
| Hospitalization Year | ||
| 2012 | 27,695 | 16.2 |
| 2013 | 28,359 | 16.4 |
| 2014 | 29,860 | 17.1 |
| 2015 | 25,687 | 14.5 |
| 2016 | 22,357 | 12.5 |
| Total period | 133,958 | 75.0 |
| Preventable Diseases | Frequency (per 1,000 admissions) | |
| Whooping cough | 129 | 1.0 |
| Acute hepatitis B | 162 | 1.2 |
| Mumps | 72 | 0.5 |
| Tetanus | 16 | 0.1 |
| Diphtheria | 6 | 0.04 |
| Meningitis | 4 | 0.03 |
| Measles | 3 | 0.02 |
| Other causes | ||
| Urinary tract infection | 25,270 | 188.6 |
| Bacterial gastroenteritis and complications | 23,871 | 178.2 |
| Diabetes mellitus | 10,256 | 76.6 |
| Lung diseases | 9,922 | 74.1 |
| Arterial hypertension | 8,966 | 66.9 |
| Skin and subcutaneous infection | 8,965 | 66.9 |
| Heart failure | 8,841 | 66.0 |
| Ear, nose and throat infections | 6,704 | 50.1 |
| Cerebrovascular diseases | 5,769 | 43.1 |
| Asthma | 4,920 | 36.7 |
| Diseases related to pregnancy and childbirth | 4,311 | 32.2 |
| Epilepsies | 2,993 | 22.3 |
| Bacterial pneumonias | 2,584 | 19.3 |
| Pelvic inflammatory disease | 2,504 | 18.7 |
| Malaria | 1,873 | 13.9 |
| Angina | 1,845 | 13.8 |
| Gastrointestinal ulcer | 1,428 | 10.7 |
| Nutritional deficiencies | 1,154 | 8.6 |
| Pulmonary tuberculosis | 635 | 4.7 |
| Anemia | 574 | 4.3 |
| Rheumatic fever | 122 | 0.9 |
| Syphilis | 22 | 0.2 |
| Extrapulmonary tuberculosis | 20 | 0.2 |
| Ascariasis | 17 | 0.1 |
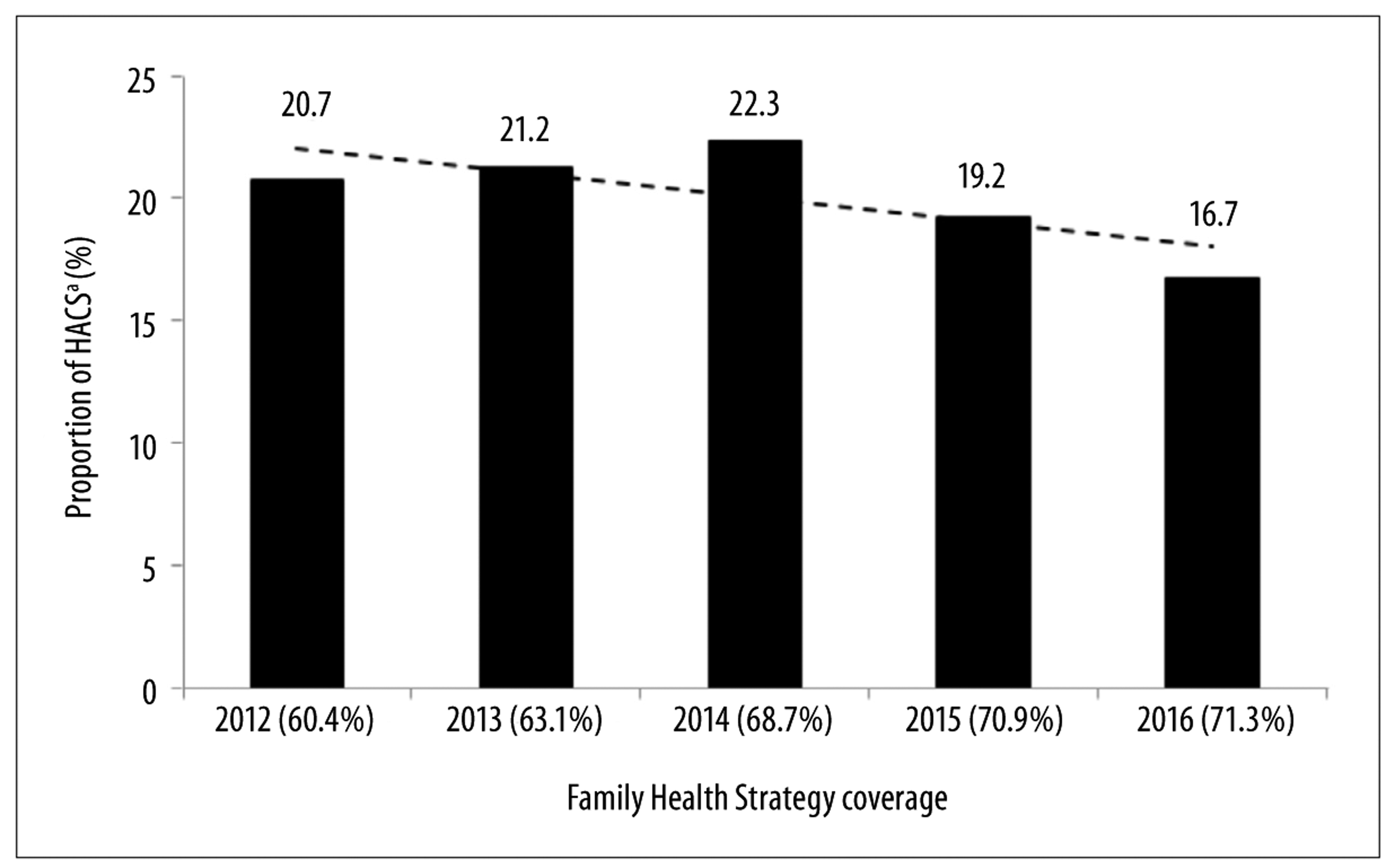
a) HACSC: Hospitalizations for ambulatory care-sensitive conditions.
Note: Spearmans correlation coefficient = -0.60; p = 0.285.
Figure 1 Time trend of the proportion of hospitalizations for ambulatory care-sensitive conditions and Family Health Strategy coverage, Rondônia, 2012-2016
The main causes of HACSC in the period analyzed were related to infections of the urinary tract, which accounted for 188.6/1,000 HACSC. Also standing out was bacterial gastroenteritis and its complications, which accounted for 178.2/1,000 HACSC. Among chronic diseases that can be controlled in PHC, diabetes mellitus (76.6/1,000), arterial hypertension (66.9/1,000), infections of the skin and subcutaneous tissue (66.9/1,000) and heart failure (66.0/1,000) were the conditions most frequently leading to HACSC. Lung diseases (74.1/1,000) and ear, nose and throat infections (50.1/1,000) were the next most prevalent groups of causes in the period. Also worthy of highlight are vaccine-preventable diseases, the frequency of which was considerable among HACSC in Rondônia (Table 3).
Of all the HACSC occurring between 2012 and 2016, 121,365 (90.6%) were classified as urgent hospital admissions and 12,593 (9.4%) as elective admissions. General medicine (68.0%) and pediatric (26.3%) hospitalizations predominated. Average length of inpatient stay was 3.9 days (SD: 5.9). A total of 130,952 (97.8%) patients did not require intensive treatment during the hospitalization period and only 2.9% of them evolved to death (Table 4).
Table 4 - Clinical characteristics of 133,958 patients hospitalized for ambulatory care sensitive conditions, Rondônia, 2012-2016
| Characteristics | N | % |
|---|---|---|
| Length of stay (days) | ||
| None | 1,846 | 1.4 |
| 1-3 | 94,157 | 70.3 |
| 4-7 | 25,339 | 18.9 |
| 8-15 | 8,493 | 6.3 |
| >15 | 4,123 | 3.1 |
| Mean (SDa) | 3.9 (5.9) | 16,7 |
| Nature of hospitalization | ||
| Elective | 12,593 | 9.4 |
| Urgency | 121,365 | 90.6 |
| Medical specialty | ||
| Surgery | 3,322 | 2.5 |
| Obstetrics | 4,044 | 3.3 |
| General medicine | 91,136 | 68.0 |
| Chronic | 6 | 0.01 |
| Phthisiology | 202 | 0.2 |
| Pediatrics | 35,248 | 26.3 |
| Need for intensive treatment | ||
| Yes | 3,006 | 2.2 |
| No | 130,952 | 97.8 |
| Evolution to death | ||
| Yes | 3,939 | 2.9 |
| No | 130,019 | 97.1 |
a) SD: standard deviation.
Discussion
This study found a high overall rate of HACSC in the state of Rondônia during the five-year period between 2012 and 2016. In the analysis stratified by municipalities, we found high HACSC rates in multiple locations, reaching rates higher than 50 hospitalizations/1,000 inhab. Despite this, we highlight the slight but progressive reduction in HACSC, together with a gradual increase in FHS coverage in Rondônia during the period analyzed. The same panorama was found in other Brazilian states in the early 2000s, when the proportion of HACSC was generally greater than 20%, although it has reduced in recent years.12-14
A study conducted in Brazil’s Federal District, with the purpose of analyzing the coefficients of hospitalizations for ambulatory care-sensitive conditions in 2008, showed that 20% of the total number of hospitalizations related to ACSC.15 In another study conducted in São Paulo in 2011, 15.9% of hospitalizations were related to care-sensitive conditions.16 High HACSC frequencies have also been reported by Caldeira et al.,12 Ferreira et al.13 and Mendonça,14 reaching proportions of between 20 and 45%. The high frequency of HACSC observed in this and previous studies can be interpreted as a deficiency in the quality and effectiveness of PHC, especially in regions where FHS is not yet fully implemented.4,17 In addition, compared to frequencies found in other Latin American countries, the HACSC frequency found in Rondônia is worrying. Analysis of 39 million hospital admissions in Argentina, Colombia, Costa Rica, Ecuador, Mexico and Paraguay found 14.3% HACSC, with rates ranging from 10.8% (Costa Rica) to 21.6% (Colombia).18
The reduction in the proportion and the rate of HACSC observed over the course of the five-year period selected followed the trend found for Brazil as a whole and for some states where primary care is better structured.19-22 The Family Health Strategy, recognized as an effective strategy for organizing and building the capacity of Primary Health Care, has been considered to be one of the major determinants of this reduction.17,24 Indeed, the increase in local and regional FHS coverage appears to be associated with the reduction in HACSC, even though the classic problems linked to primary health care continue to exist, such as economic, social and political factors, as well as certain problems proper to health services, which are capable of influencing the risk of hospitalization.25-27
Small municipalities with 100% FHS coverage showed high proportions of HACSC recorded in the period studied. It is known that FHS coverage is inversely proportional to population size. However, previous studies have shown that HACSC rates increase as municipal population size decreases.25 A likely explanation for this apparent discrepancy would be the lower problem-solving capacity of health services in smaller municipalities. Lack of specialized infrastructure and capacity to respond to the various health situations of service users, ultimately leads to hospitalization for all health conditions, regardless of whether or not they are primary care-sensitive conditions.17,25 In general, small-sized municipalities play a local role, attending to the basic needs of the population, and depend on medium or large size municipalities for various services, in particular higher complexity health services.28,29 Similarly, the high proportion of urgent HACSC suggests that access to hospitalization occurs through services other than PHC services.30
We found a considerable proportion of HACSC in children aged under 9 years old (42.8%), possibly related to higher prevalence of gastroenteritis and other acute infections, transmitted by food and water, in the context of the Northern Region. Despite some progress with treated water and sewage collection and treatment services, basic sanitation is very lacking in Rondônia.10 A similar result was found by Caldeira et al.12 in Montes Claros, in the state of Minas Gerais, where the proportion of HACSC in the pediatric age group was 41.4% whereby, according the authors of that study, children, and in particular breastfed babies, are more susceptible to diseases and are a greater cause of concern for their families and health professionals, so that the latter are more inclined to recommend hospitalization. Other explanations for the proportion found in this age group would be limited access to health services and difficulties faced by primary care professionals in managing the clinical conditions of younger children.12
The profile of the causes that lead to HACSC in Rondônia was quite varied. The most frequent health conditions found do not differ from the expected, according to a systematic review on the theme: the studies included in the review highlighted that the main diagnoses leading to HACSC in Brazil are urinary tract infections, gastroenteritis, bacterial pneumonia and heart failure.7 It is also important to highlight that HACSC in Rondônia included various vaccine-preventable diseases. For example, 16 patients were hospitalized because of tetanus. These findings, together with non-communicable chronic diseases (diabetes mellitus and arterial hypertension), are conditions that can be controlled in primary health care and, therefore, also point to a deficit in quality of care at the most basic level of health care.3
Although all the results found in the analysis of HACSC in Rondônia were consistent with those of several other Brazilian studies, some limitations of our study should be emphasized. For example, we only analyzed HACSC at public hospitals or private SUS outsourced hospitals. This probably underestimated this indicator, above all because a considerable portion of Rondônia’s population lives far away from large urban centers and for them hospital services are still predominantly private. Another limitation of this study refers to information about the diagnosis that led to the hospitalization which was collected only from SUS hospital admission authorization forms. This document is open to criticism, since the cause of hospitalization often differs from the definitive diagnosis, i.e., the diagnosis at the time of hospital discharge.12 Moreover, as the assessment of the relationship between FHS expansion and HACSC was based on secondary data, it may not be accurate, since it addresses the situation in the municipality as a whole, not stating whether the hospitalized individuals were previously treated in PHC/FHS facilities. In addition, there is a limitation due to underreporting on SIH/SUS, possible classification problems in relation to the ICD-10 codes used, and possible double or triple counting of the same patient, because the system does not allow identification of readmissions.
The results of our study showed a high frequency of HACSC in Rondônia. Although there was a slight increase in FHS coverage between 2012 and 2016, this increase was not accompanied by significant changes in the frequency of hospitalizations for ambulatory care-sensitive conditions in Rondônia. It is expected that the information produced, which has been summarized here, can serve as an alert and concern for Rondônia’s health authorities and, consequently, encourage the implementation of measures to increase Family Health Strategy coverage in all the municipalities of Rondônia state.
Referências
1. Starfield B. Atenção primária: equilíbrio entre necessidades de saúde, serviços e tecnologia [Internet]. Brasília: Organização das Nações Unidas para a Educação, a Ciência e a Cultura; Ministério da Saúde; 2002 [citado 2018 nov 7]. 726 p. Disponível em: Disponível em: http://bvsms.saude.gov.br/bvs/publicacoes/atencao_primaria_p1.pdf [ Links ]
2. Shi L, Samuels ME, Pease M, Bailey WP, Corley EH. Patient characteristics associated with hospitalizations for ambulatory care sensitive conditions in South Carolina. South Med J. 1999 Oct;92(10):989-98. [ Links ]
3. Rede Interagencial de Informações para a Saúde. Indicadores básicos para a saúde no Brasil: conceitos e aplicações [Internet]. 2. ed. Brasília: Organização Pan-Americana da Saúde; 2008 [citado 2018 nov 7]. 349 p. Disponível em: Disponível em: http://tabnet.datasus.gov.br/tabdata/livroidb/2ed/indicadores.pdf [ Links ]
4. Alfradique ME, Bonolo PF, Dourado I, Lima-Costa MF, Macinko J, Mendonça CS, et al. Internações por condições sensíveis à atenção primária: a construção da lista brasileira como ferramenta para medir o desempenho do sistema de saúde (Projeto ICSAP - Brasil). Cad Saúde Pública. 2009 jun; 25(6):1337-1349. doi: 10.1590/S0102-311X2009000600016 [ Links ]
5. Brasil. Ministério da Saúde. Portaria MS/SAS no 221, de 17 de abril de 2008. Define que a lista brasileira de internações hospitalares por condições sensíveis à atenção primária será utilizada como instrumento de avaliação da atenção primária e/ou utilização da atenção hospitalar, podendo ser aplicada para avaliar o desempenho do sistema de saúde nos âmbitos Nacional, Estadual e Municipal. Diário Oficial da República Federativa do Brasil, Brasília (DF), 2008 abr 18; Seção 1:70. [ Links ]
6. Ministério da Saúde (BR). Secretaria de Atenção à Saúde. Departamento de Atenção Básica. Política nacional de atenção básica [Internet]. Brasília: Ministério da Saúde; 2012 [citado 2018 nov 7]. 110 p. Disponível em: Disponível em: http://189.28.128.100/dab/docs/publicacoes/geral/pnab.pdf [ Links ]
7. Santos FC. Internações por condições sensíveis à atenção primária: uma revisão da produção indexada na biblioteca virtual em saúde, 2005-2014 [dissertação]. Porto Alegre (RS): Universidade Federal do Rio Grande do Sul; 2015. [ Links ]
8. Fontenelle LF. Estratégia saúde da família e internações por condições sensíveis à atenção primária (CSAP): revisão sistemática da literatura [dissertação]. Ribeirão Preto (SP): Universidade de São Paulo; 2011. [ Links ]
9. Rehem TCMSB, Oliveira MRF, Amaral TCL, Ciosak SI, Egry EY. Internações por condições sensíveis à atenção primária em uma metrópole brasileira. Rev Esc Enferm USP. 2013 ago;47(4):884-90. doi: 10.1590/S0080-623420130000400016 [ Links ]
10. Instituto Brasileiro de Geografia e Estatística. Site [Internet]. 2018 [citado 2018 nov 7]. Disponível em: Disponível em: https://www.ibge.gov.br/ [ Links ]
11. Ministério da Saúde (BR). Datasus. Informações de saúde [Internet]. 2012 [citado 2017 nov 25]. Disponível em: Disponível em: http://tabnet.datasus.gov.br/cgi/tabnet [ Links ]
12. Caldeira AP, Fernandes VBL, Fonseca WP, Faria AA. Internações pediátricas por condições sensíveis à atenção primária em Montes Claros, Minas Gerais, Brasil. Rev Bras Saúde Mater Infant. 2011 jan-mar;11(1):61-71. doi: 10.1590/S1519-38292011.0001.00007 [ Links ]
13. Ferreira JBB, Borges MJG, Santos LL, Forster AC. Internações por condições sensíveis à atenção primária à saúde em uma região de saúde paulista, 2008 a 2010. Epidemiol Serv Saúde. 2014 jan-mar;23(1):45-56. doi: 10.5123/S1679-497420140001.00005 [ Links ]
14. Mendonça CS. Uso das Internações por Condições Sensíveis à Atenção Primária para a avaliação da Estratégia Saúde da Família em Belo Horizonte/MG [dissertação]. Porto Alegre (RS): Universidade Federal do Rio Grande do Sul; 2009. [ Links ]
15. Junqueira RMP, Duarte EC. Internações hospitalares por causas sensíveis à atenção primária no Distrito Federal, 2008. Rev Saúde Pública. 2012 out;46(5):761-8. doi: 10.1590/S0034-89102012000500001 [ Links ]
16. Torres RL, Rehem TCMSB, Egry EY, Ciosak SI. O panorama das internações por condições sensíveis à Atenção Primária em um distrito de São Paulo. Rev Esc Enferm USP. 2011 dez;45(2):1661-6. [ Links ]
17. Nedel FB, Facchini LA, Martin-Mateo M, Vieira LAS, Thumé E. Programa saúde da família e condições sensíveis à atenção primária, Bagé (RS). Rev Saúde Pública. 2008 dez;42(6):1041-52. doi: 10.1590/S0034-89102008000600010 [ Links ]
18. Guanais F, Gómez-Suárez R, Pinzón L. Series of avoidable hospitalizations and strengthening primary health care: primary care effectiveness and the extent of avoidable hospitalizations in Latin America and the Caribbean [Internet]. Inter-American Development Bank; 2012 [cited 2017 Nov 25]. Disponível em: Disponível em: http://services.iadb.org/wmsfiles/products/Publications/37846490.pdf [ Links ]
19. Dourado I, Oliveira VB, Aquino R, Bonolo P, Lima-Costa MF, Medina MG, et al. Trends in primary health care-sensitive conditions in Brazil: the role of the Family Health Program (Project ICSAP-Brazil). Med Care. 2011 Jun;49(6):577-84. doi: 10.1097/ MLR.0b013e31820fc39f [ Links ]
20. Boing AF, Vicenzi RB, Magajewski F, Boing AC, Moretti-Pires RO, Peres KG, et al. Redução das internações por condições sensíveis à atenção primária no Brasil entre 1998-2009. Rev Saúde Pública. 2012 abr;46(2):359-66. doi: 10.1590/S0034- 89102012005000011 [ Links ]
21. Macinko J, Dourado I, Aquino R, Bonolo PF, Lima-Costa MF, Medina MG, et al. Major expansion of primary care in Brazil linked to decline in unnecessary hospitalization. Health Aff (Millwood). 2010 Dec;29(12):2149-60. doi: 10.1377/hlthaff.2010.0251 [ Links ]
22. Macinko J, Oliveira VB, Turci MA, Guanais FC, Bonolo PF, Lima-Costa MF. The influence of primary care and hospital supply on ambulatory care-sensitive hospitalizations among adults in Brazil, 1999-2007. Am J Public Health. 2011 Oct;101(10):1963-70. doi: 10.2105/AJPH.2010.198887 [ Links ]
23. Mendonça SS, Albuquerque EC. Profile of hospital admissions for primary care sensitive conditions in Pernambuco State, Brazil, 2008-2012. Epidemiol Serv Saúde. 2014 Jul-Sep;23(3):463-74. doi: 10.5123/S1679-49742014000300009 [ Links ]
24. Caminal J, Starfield B, Sánchez E, Casanova C, Morales M. The role of primary care in preventing ambulatory care sensitive conditions. Eur J Public Health. 2004 Sep;14(3):246-51. [ Links ]
25. Nedel FB, Facchini LA, Martín M, Navarro A. Características da atenção básica associadas ao risco de internar por condições sensíveis à atenção primária: revisão sistemática da literatura. Epidemiol Serv Saúde. 2010 jan-mar;19(1):61-75. doi: 10.5123/S1679-4974201.00001.00008 [ Links ]
26. LentsckI MH, Latorre MRDO, Mathias TAF. Tendência das internações por doenças cardiovasculares sensíveis à atenção primária. Rev Bras Epidemiol. 2015 abr-jun;18(2):372-384. doi: 10.1590/1980-5497201500020007 [ Links ]
27. Venancio SI, Rosa TEC, Sanches MTC, Shigeno EY, Souza JMP. Efetividade da estratégia saúde da família sobre indicadores de saúde da criança no Estado de São Paulo. Rev Bras Saúde Mater Infant. 2016 jul-set;16(3):271-81. doi: 10.1590/1806-93042016000300004 [ Links ]
28. Henrique F, Calvo MCM. Grau de implantação do Programa Saúde da Família e indicadores sociais. Ciênc Saúde Coletiva. 2009 out;14(Suppl 1):1359-65. doi: 10.1590/S1413-81232009000800008 [ Links ]
29. Akaishi AG. Desafios do planejamento urbanohabitacional em pequenos municípios brasileiros. Rev Risco. 2011;14(2):41-50. doi: 10.11606/issn.1984-4506.v0i14p41-50 [ Links ]
30. Cardoso CS, Pádua CM, Rodrigues-Júnior AA, Guimarães DA, Carvalho SF, Valentin RF, et al. Contribuição das internações por condições sensíveis à atenção primária no perfil das admissões pelo sistema público de saúde. Rev Panam Salud Publica. 2013 out;34(4):227-34. [ Links ]
Received: January 01, 2018; Accepted: September 11, 2018











 texto em
texto em 
 Curriculum ScienTI
Curriculum ScienTI

