Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Epidemiologia e Serviços de Saúde
versão impressa ISSN 1679-4974versão On-line ISSN 2237-9622
Epidemiol. Serv. Saúde vol.28 no.2 Brasília jun. 2019 Epub 29-Jul-2019
http://dx.doi.org/10.5123/s1679-49742019000200008
ORIGINAL ARTICLE
Evaluation of the Program to Combat Neglected Diseases in controlling schistosomiasis mansoni in three hyperendemic municipalities, Pernambuco, Brazil, 2014*
1Instituto de Medicina Integral Prof. Fernando Figueira, Grupo de Estudos de Gestão e Avaliação em Saúde, Recife, PE, Brasil
2Secretaria Estadual de Saúde, Secretaria Executiva de Vigilância em Saúde, Recife, PE, Brasil
3Universidade Federal de Pelotas, Departamento de Medicina Social, Pelotas, RS, Brasil
4Universidade Federal de Pelotas, Departamento de Enfermagem em Saúde Coletiva, Pelotas, RS, Brasil
Objective:
to evaluate the implementation of schistosomiasis mansoni control actions under the Program to Combat Neglected Diseases in three municipalities in Pernambuco state, Brazil.
Methods:
implementation analysis was done in 2014, considering the following components - management, epidemiological surveillance, patient care, laboratorial support and health education -; direct observation and interviews were carried out with managers and technical personnel at the state, regional, and municipal levels.
Results:
partial implementation was found in municipalities A and B 69.7%; 62.2%, while there was full implementation in municipality C 79.5%; contextual weaknesses were found in communication between management levels, insufficient technical-management autonomy of decentralized levels, and professional staff job instability; potentialities identified were - continuing education, political articulation, knowledge about the program, and performance evaluation.
Conclusion:
contextual categories related to development and implementation stood out for their positive influence on the degree of implementation in the municipalities; we recommend intervention in the weaknesses found, in order to ensure program sustainability and institutionalization.
Keywords: Schistosomiasis; Public Health Surveillance; Health Programs and Plans; Health Evaluation
Introduction
Schistosomiasis is a neglected disease and is related to poverty. Its magnitude is higher among parasitic diseases due to its serious consequences when manifested in its clinical forms. In the Americas, Brazil has the highest concentration of registered cases. These are distributed over 19 states and 2 million people are estimated to be infected. Of these, 80% live in Northeast region, with high prevalence along the coast and river basins.1 Given this scenario, the Brazilian Ministry of Health has alerted as to the need to identify sanitary conditions favoring fresh water contamination. Monitoring these conditions is important to support actions to control and reduce prevalence of infection, occurrence of its hepatosplenic form and deaths from this disease.2-5
In 2016, schistosomiasis was still considered endemic in 103 of the 185 municipalities in Pernambuco state, with concentration in Zona da Mata Norte and Zona da Mata Sul, and the Metropolitan Region of Recife, capital of Pernambuco. Locations with 10% to 50% of positive serological diagnosis were identified in these three regions. From 2008 to 2014, 473 hospitalizations owing to the disease were recorded, while in the period from 2009 to 2013 the average number of deaths in the state reached 171. These data represent the highest rates of hospitalization and mortality from the disease among Brazilian states in the periods mentioned.6.7
The main Brazilian government standardized strategies to control the disease are: i schistosomiasis case definition; ii notification; iii proper use of a specific computerized system and the flow of information that it favors; iv epidemiological research; v stool examination; vi transmission areas classification; vii health education actions; and viii treatment in endemic localities using orally administered praziquantel.4
In 2011, Pernambuco government launched the Program to Combat Neglected Diseases SANAR in that state. At that time, seven communicable diseases including schistosomiasis were selected and included on the international agenda. In essence, the SANAR program stands out from other Ministry of Health actions in two aspects: i the strengthening of selective treatment actions, with effective involvement in positive case surveillance, diagnosis and treatment activities by Family Health Strategy professional teams, with encouragement of weekly active surveillance; and ii the adoption of collective treatment with praziquantel for all individuals over 2 years of age in localities with positivity rates equal to or greater than 10%.8-10
By 2014, actions to combat schistosomiasis via SANAR had been implemented in 30 municipalities considered to be priority. There was significant impact on schistosomiasis morbidity and mortality in the same period in Pernambuco: schistosomiasis prevalence, which in 2010 was 17% on average in hyperendemic areas, fell to 4.4% in 2014. In 2010, 10,889 positive cases were registered, representing 6.1% positivity and 205 deaths; in 2014, these numbers had fallen to 8,713 positive cases, 3.4% positivity and 175 deaths.10
Considering the importance of knowledge about the mechanisms created under SANAR and the possibility of their replication in other contexts with a similar epidemiological situation, the purpose of this article was to evaluate the implementation of actions to control schistosomiasis mansoni by the program in three municipalities of Pernambuco.
Methods
This is an evaluation study involving implementation analysis11 regarding the influence of the context on the level of schistosomiasis control action implementation under the SANAR program. Our research strategy was a multilevel study of multiple cases conducted in 2014.
The study was carried out in three municipalities identified here by the letters A, B and C in the state of Pernambuco, Brazil, which met the following inclusion criteria: environmental conditions favorable to the endemic situation continuing; collective treatment; and average positivity rate above 20%. Municipality A, located in the Metropolitan Region of Recife, has a territorial area of 527.107km², demographic density of 152.98 inhabitants per km², an estimated population of 94,533 inhabitants and municipal human development index IDHM of 0.619. Municipalities B and C, located in the Zona da Mata region, have respectively: territorial area of 342.201 km² and 160.477km²; demographic density of 183.07 inhabitants/km² and 86.87 inhab./km²; an estimated population of 68,281 and 15,683 inhabitants; and IDHM of 0.632 and 0.530.12
The evaluation was developed in three stages as outlined below:
Stage 1 - Construction of the logic model and judgment matrix for SANAR program schistosomiasis control actions.
The logic model was developed in order to understand the correlations between schistosomiasis control action structure, process and expected results, based on institutional documents relating to infection control Figure 1. Based on the logic model, we built a judgment matrix: i structure and process indicators; ii judgment parameters; iii means of verification for each indicator; and iv the score for judging the indicators, which was defined based on institutional documents or documents available in the literature. The rating given to each selected indicator considered its degree of importance, using a scale from zero to four Figure 2. In order to enhance construct validity, the model and the matrix were submitted to specialist appraisal, as recommended by McLaughlin and Jordan.13
Legenda:
SANAR: Program to combat neglected diseases.
Figure 1 - Logic model for schistosomiasis control actions under the Program to Combat Neglected Diseases, Pernambuco, 2014

a SE: Score expected.
Legend:
PCE: Schistosomiasis Control Program.
SISPCE: Schistosomiasis Control Information System.
FHU: Family Health Unit.
eESF: Family Health team.
TC: collective treatment.
TS: selective treatment.
Figure 2 - Judgment Matrix for schistosomiasis control actions under the Program to Combat Neglected Diseases, Pernambuco, 2014
Stage 2 - Implementation level classification
At this stage of the study, the indicators listed in the matrix were used in primary data collection, by means of systematic observation and administering a structured questionnaire with Primary Health Care coordinators and Schistosomiasis Control Program PCE coordinators, Family Health Team eESF professionals and endemic disease health workers in the three municipalities.
We used a system of scores for the implementation level analysis, attributing scores to indicators according to their relationship with schistosomiasis prevalence reduction. The design of this score system was based on a reference document, namely the SANAR Program Monitoring Handbook for Schistosomiasis.14 As such, the scores for the indicators were added together, divided by the expected score and multiplied by 100. This proportion was framed into quartiles which defined implementation level as follows: implemented 75%-100%; partially implemented 50%-74.9%; critically implemented 25%-49.9%; and not implemented 0%-25%.
Stage 3 - Context and influence evaluation
In order to evaluate the context, we built an analysis matrix, as per the political-contingent model.15 We analyzed attributes of the political and structural context, represented in this study by the following dimensions: “Implementation and Development” knowledge and priority given to the program, “Openness level” institutional dialog and co-responsibility and “Sustainability” maintenance and sustainability strategies. Once these dimensions had been established, we defined categories of analysis which were used as a source of information for primary data collection. We conducted semi-structured interviews with managers of the Pernambuco State Health Department SES/PE, municipal Primary Health Care and Health Surveillance managers and technicians; and with managers of the Regional Health Divisions RS, whereby RS1 was correlated to Municipality A and RS2 was responsible for Municipalities B and C.
The semi-structured interviews and document appraisal were submitted to content analysis;16 and the information was classified according to three types of situation identified in relation to the sources of evidence adapted from the classification proposed by Alves et al., namely:17
- Positive convergence C+ of sources, benefiting program implementation;
- Divergence D between sources, characterizing situations of unconsolidated change, although potentially favorable to implementation; and
- Negative convergence C- between sources, expressing situations unfavorable to program implementation.
The study project was approved by the Ethics Research Committee of the Faculdade de Medicina da Universidade de Pelotas CEP/FAMED/UFPel: Report No. 772,632, dated August 30th, 2014. Prior to the interviews, subjects were asked to sign a Free and Informed Consent form, whilst guaranteeing their right not to participate and guaranteeing the privacy of their personal data.
Results
Definition of level of implementation involved the participation of three Brazilian National Health System municipal Primary Care coordinators, three PCE coordinators, 56 Family Health team professionals and 85 endemic disease health workers from the three municipalities. Context evaluation involved two state health service managers Health Surveillance Executive Secretary and SANAR coordinator, two regional health division managers, three municipal Primary Health coordinators and three municipal Health Surveillance coordinators. There were no losses or refusals to cooperate with the study.
Only Municipality C was classified as implemented 79.5%. In the Structure dimension, the “material resources” component had the best implementation level, particularly in Municipality C 95.6%. Regarding the process dimension, Municipality A achieved 100% implementation for the “management” component, while “epidemiological surveillance” actions achieved better percentages in Municipalities B 75.1% and C 80.4% Table 1.
Table 1 - Implementation level of schistosomiasis control components, by process and structure dimension in priority municipalities of the Program to Combat Neglected Diseases, Pernambuco, 2014
| Components, by dimension | Implementation level % | ||
|---|---|---|---|
| Municipalities | |||
| A | B | C | |
| Structure | |||
| Human resources | 56.4 | 43.5 | 79.0 |
| Material resources | 87.6 | 67.4 | 95.6 |
| Implementation level % | 69.7 | 53.7 | 86.1 |
| Process | |||
| Management | 100.0 | 73.9 | 73.9 |
| Epidemiological Surveillance | 51.0 | 75.1 | 80.4 |
| Patient care and laboratory support | 53.3 | 68.8 | 66.6 |
| Health education | 66.5 | 32.5 | 33.2 |
| Implementation level % | 69.7 | 70.6 | 72.8 |
| Implementation level: Structure + process % | 69.7 | 62.2 | 79.5 |
Note: SANAR implementation level classification: implemented = 75% to 100%; partially implemented = 50% to < 75%; critically implemented = 25% to < 50%; and not implemented = 0% to < 25%.
In the “human resources” component, while the indicators related to the existence of professionals in management positions Primary Health Care and Epidemiological Surveillance received a maximum score, the existence of PCE and SANAR advisors working on schistosomiasis control actions obtained the maximum score and zero in Municipalities A and B, respectively. Regarding “material resources”, the availability of vehicles and spreadsheets for control actions was fully scored only in Municipality C, and medication availability did not obtain the maximum score in Municipality A. In the “management” component, only Municipality A obtained the maximum score for professional training indicators. In the “epidemiological surveillance” component, all municipalities carried out data input, although they did not send documentation after collective treatment evaluation. In addition, Municipality A did not carry out sample surveys. The indicators for the existence of a referral network for severe cases “patient care and outpatient support” component and for educational activities for more vulnerable people “health education” component achieved partial scores in the three municipalities Table 2.
Table 2 - Indicator and component score and implementation level %, related to schistosomiasis control actions in priority municipalities of the Program to Combat Neglected Diseases, Pernambuco, 2014
| Indicator | ES | SO/IL % | ||
|---|---|---|---|---|
| Municipalities | ||||
| A | B | C | ||
| Structure | ||||
| Human resources | ||||
| Existence of staff responsible for Primary Health Care | 3 | 3 | 3 | 3 |
| Existence of staff responsible for epidemiological surveillance, environmental monitoring and/or endemic disease control | 3 | 3 | 3 | 3 |
| Existence of laboratory professionals | 3 | 3 | 3 | 3 |
| Existence of PCE and SANAR advisors on schistosomiasis control actions | 3 | 3 | 0 | 1.5 |
| Existence of SISPCE typist | 4 | 4 | 4 | 4 |
| Proportion of FHU professionals in priority locations for CT in the municipality trained in collective treatment | 4 | 0 | 0 | 4 |
| Proportion of Family Health team professionals in the municipality trained in selective treatment | 4 | 0 | 0 | 4 |
| Proportion of Family Health team professionals in the municipality trained in clinical management | 2 | 0 | 0 | 2 |
| Proportion of Family Health team professionals in the municipality trained in health surveillance | 2 | 0 | 0 | 0 |
| Proportion of Family Health teams in the municipality with full staff and sufficient number thereof | 2 | 0 | 0 | 0 |
| Existence of art educators | 2 | 1.5 | 0.5 | 0 |
| Subtotal | 32 | 17.5 | 13.5 | 24.5 |
| Implementation level % | 56.4 | 43.5 | 79.0 | |
| Material resources | ||||
| Availability of spreadsheets used in schistosomiasis control actions | 2 | 1.5 | 1.5 | 2 |
| Number of items of the work kit available to primary health care professionals | 1 | 0.5 | 0.5 | 0.5 |
| Vehicle availability | 2 | 1.5 | 1.5 | 2 |
| Availability of medication prazinquantel | 4 | 2.6 | 4 | 4 |
| Collection pots availability | 4 | 4 | 4 | 4 |
| Physician scales availability | 4 | 4 | 2 | 4 |
| Educational material availability | 2 | 2 | 2 | 1.5 |
| Adequate facilities for slide reading and preparation | 4 | 4 | 0 | 4 |
| Subtotal | 23 | 20.2 | 15.5 | 22 |
| Implementation level % | 87.6 | 67.4 | 95.6 | |
| Process | ||||
| Management | ||||
| Professional training in collective treatment performed | 4 | 4 | 4 | 4 |
| Professional training in selective treatment performed | 4 | 4 | 4 | 4 |
| Professional training in clinical management performed | 3 | 3 | 1.5 | 1.5 |
| Training in laboratory diagnosis performed | 3.5 | 3.5 | 1.75 | 1.75 |
| Refresher course on use of SISPCE held | 2.5 | 2.5 | 1.25 | 1.25 |
| Subtotal | 17 | 17 | 12.5 | 12.5 |
| Implementation level % | 100 | 74.0 | 73.9 | |
| Epidemiological Surveillance | ||||
| Collective treatment in hyperendemic areas performed | 4 | 4 | 4 | 4 |
| Proportion of localities with collective treatment performed | 3 | 1.5 | 3 | 3 |
| Collective treatment actions monitored | 4 | 4 | 2.6 | 4 |
| Official documentation submitted to municipality health department after collective treatment | 2 | 0 | 2 | 2 |
| Sample survey conducted | 4 | 0 | 4 | 4 |
| Proportion of localities that carried out the sample survey in the planned period 4 months | 3 | 0 | 0 | 0 |
| Periodic data input to SISPCE | 3.5 | 3.5 | 3.5 | 3.5 |
| Official documentation submitted to municipality health department following collective treatment evaluation | 2 | 0 | 0 | 0 |
| Subtotal | 25.5 | 13 | 19.2 | 20.5 |
| Implementation level % | 51 | 75.1 | 80.4 | |
| Patient care and laboratory support | ||||
| Selective treatment actions monitored | 4 | 2.66 | 4 | 2.66 |
| Existence of referral network for serious schistosomiasis cases in operation for the municipality | 3.5 | 2.3 | 1.16 | 2.33 |
| Subtotal | 7.5 | 4.0 | 5.1 | 5.0 |
| Implementation level % | 53.3 | 68.8 | 66.6 | |
| Health education | ||||
| Municipal Health Department support to educational activities for more vulnerable populations | 2 | 0.6 | 1.3 | 1.3 |
| Elaboration of educational material for schistosomiasis control actions | 2 | 2 | 0 | 0 |
| Subtotal | 4 | 2.66 | 1.3 | 1.3 |
| Implementation level % | 66.5 | 32.5 | 32.5 | |
Legend:
PCE: Schistosomiasis Control Program
SISPCE: Schistosomiasis Control Information System
FHU: Family Health Unit
eESF: Family Health team
TC: collective treatment
TS: selective treatment
SO: score obtained
IL: implementation level
ES: expected score
Note: SANAR implementation level classification: implemented = 75% to 100%; partially implemented = 50% to < 75%; critically implemented = 25% to < 50%; and not implemented = 0% to < 25%.
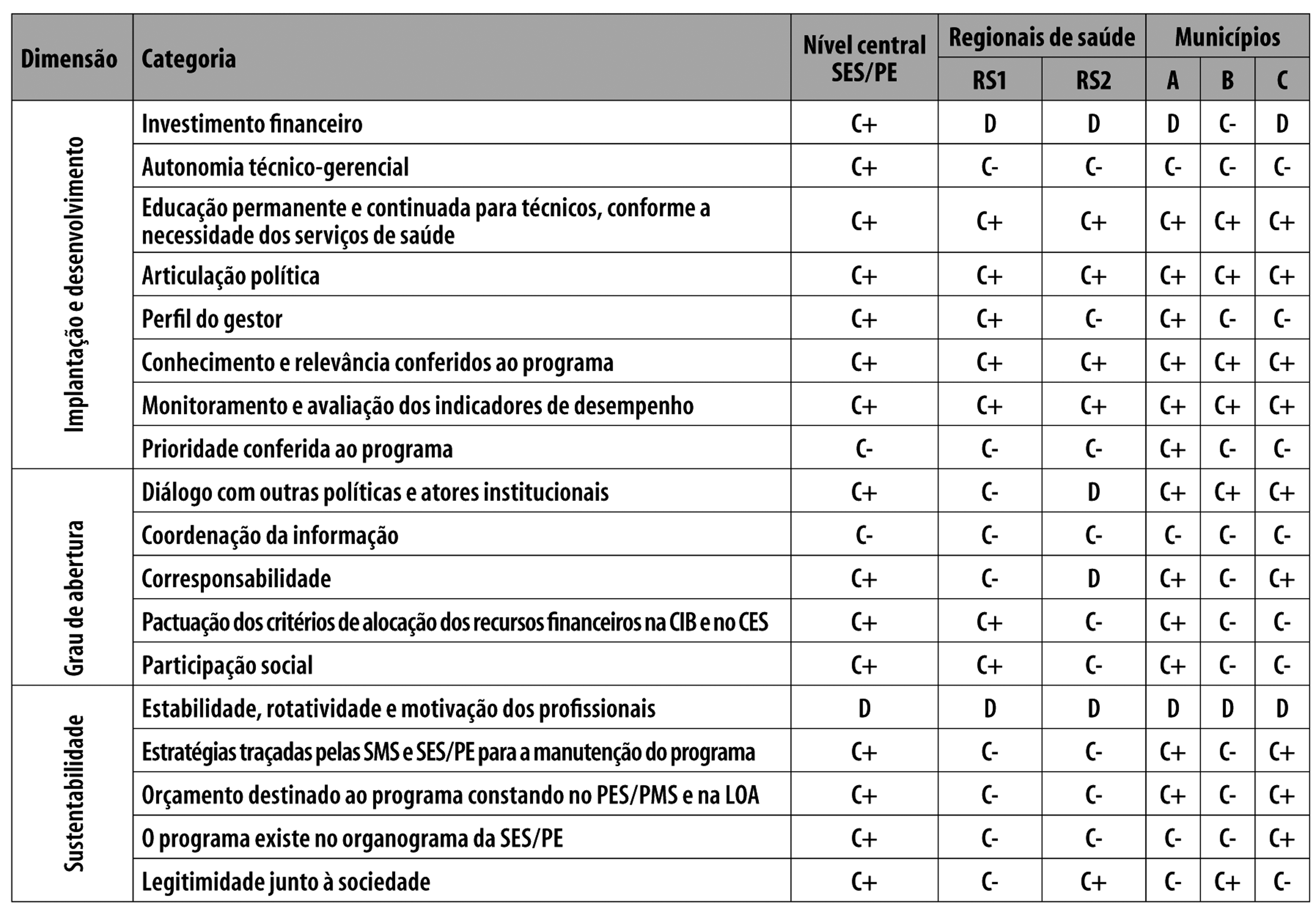
Regarding the political-contingent context, in the Implementation and Development dimension, respondents from the Pernambuco State Health Department, from RS1 and from the Municipal Health Departments had professional Public Health qualifications and had worked in Health Surveillance management for one to five years. Nevertheless, all interviewees recognized the importance of the program, and participated in indicator monitoring and evaluation by means of periodic meetings C+. The program lost priority because of lack of exclusively allocated professionals, the emergence of outbreaks and, at the same time, material resources shortage C-. Exceptionally, Municipality A had a specific professional for PCE, with the aim of expanding actions in non-endemic areas C+ Figure 3.
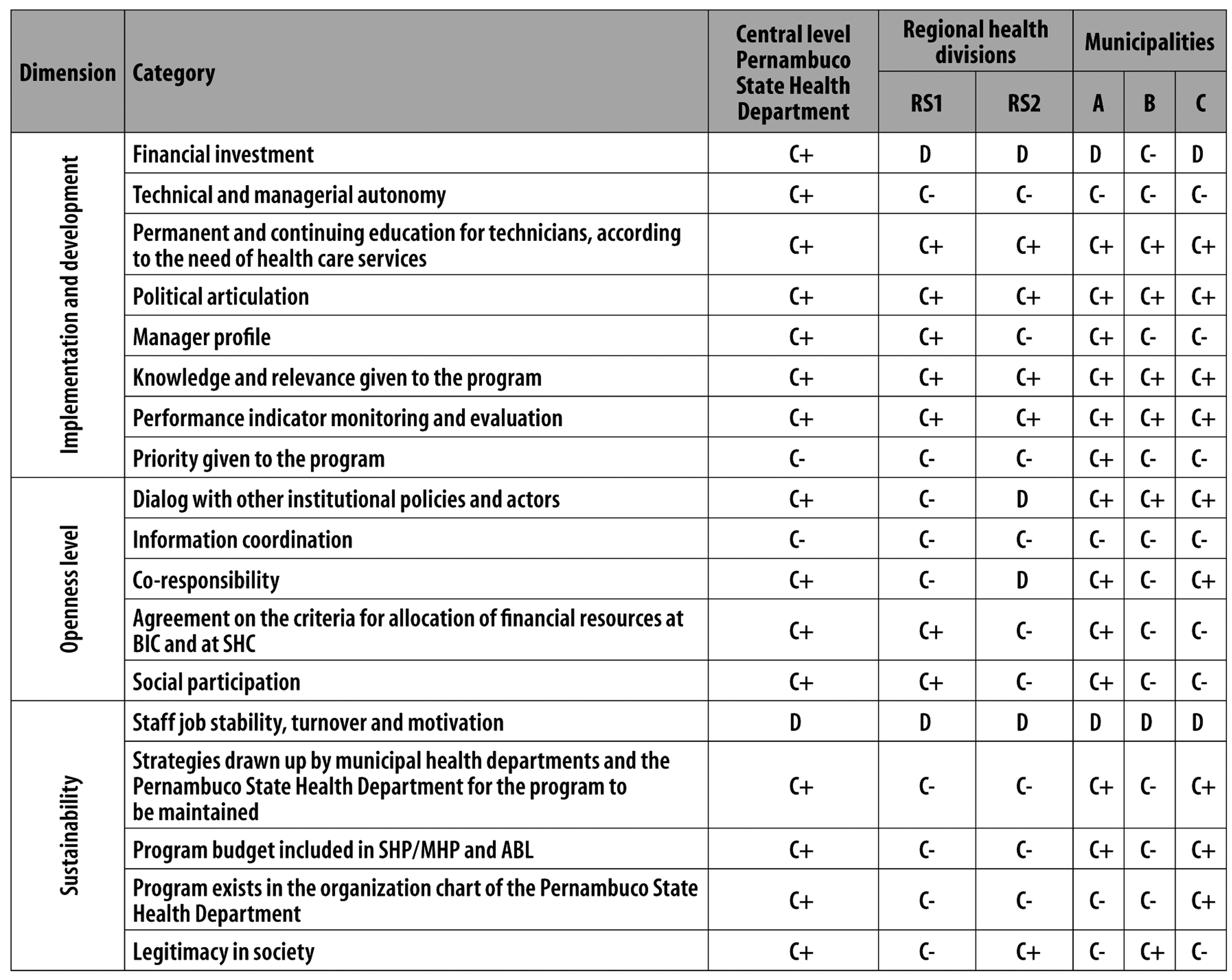
Legend:
BIC: Bipartite Intermanagerial Commission.
SHC: State Health Council.
SHP State Health Plan.
MHP: Municipal Health Plan.
ABL: Annual Budget Law.
C+: Positive convergence of evidence sources in relation to the criterion.
D: Divergence of evidence sources in relation to the criterion.
C-: Negative convergence of evidence sources in relation to the criteria.
Figure 3 - Analysis of the political-contingent context of the Schistosomiasis Control Program in priority municipalities of the Program to Combat Neglected Diseases, Pernambuco, 2014
Regarding the level of political articulation and technical and managerial autonomy, Pernambuco State Health Department considered that it respected the independence of regional health divisions and municipal health departments and their participation in local planning, when making agreements on targets and indicators C+. However, program management by the state on the other levels was found to be vertical, without due autonomy being given to regional divisions or municipal departments but rather treating them as executors of actions planned by the state C-. On the other hand, regional divisions and municipal departments promoted intermunicipal and intersectoral articulations education, infrastructure, social action, educational and research institutions, for joint planning, implementation of education actions, laboratory tests, evaluation and dissemination of the program C+.
The provision of permanent education by the Pernambuco State Health Department was considered the strong point of the program C+. There were no specific resources, but state funding guaranteed the development of established action plans C+. A structural shortage was found for the regional divisions and Municipalities A and B, although available resources contributed to action development D.
In relation to the Openness Level dimension, the interviewees recognized the fragility of information coordination between the bodies involved C-. The Pernambuco State Health Department undertook a situational diagnosis, with the aim of planning the intervention based on a schistosomiasis control reference center; and it publicized the program to other governmental entities, community leaders and Health Councils C+. This dialog was not perceived by RS1, which saw it only as “demands” made by the central level, and highlighted the weak linkage between Health Surveillance and Primary Health Care in the municipalities C-. RS2 noted the same situation, though it fostered dialog by means of planning meetings with the municipalities D. The municipalities perceived communication by sectors of their respective Municipal Health Department with institutions such as city councils, and with referral centers, with regard to planning, publicizing actions and performing laboratory tests C+.
Co-responsibility in action development was perceived by the Pernambuco State Health Department, through partnerships for the development of technologies, particularly the proposal for medication to treat the disease in children C+. RS2 noted that actions were shared with the state level, while the co-responsibility with the municipalities was in the process of consolidation: in the case of uncommitted municipalities, however, RS2 carried out actions to ensure continuity of the work D. We identified co-responsibility of the municipal planning board of Municipality A with the program; and between Health Surveillance and Primary Health Care in Municipality C, with regard to the training of community health agents. Regarding the sharing of actions with society, Pernambuco State Health Department and RS1 reported the existence of dialog with the Health Councils C+; however, neighborhood association participation in the planning of actions and SANAR program presentation to city councils were reported only in Municipality A C+.
In relation to program sustainability, we found that the program was included in the Pernambuco State Health Department and Municipality C organization charts. Both of hese and Municipality A has a budget allocated for the program in the State and Municipal Health Plans. SANAR was also included in the Annual Budget Law, approved by the Legislative Assembly of the state of Pernambuco C+. Pernambuco State Health Department has also planned strategies for maintaining the program: fundraising; articulation with other state sectors; monitoring and evaluation; and development of strategies for health education, in the face of the challenge of popular beliefs. We found that geoprocessing is used Municipality A for mapping critical areas, in addition to partnerships with other municipal departments for discussion of the local environmental situation C+.
Despite some efforts made to ensure staff job stability, low turnover and motivation, some unfavorable situations were found D: turnover of some staff, due to technicians being transferred to political positions RS2; and demotivation, given the difficulties of municipal infrastructure C. Especially with regard to professional motivation, in Municipality A, lack of guaranteed wage equality- at the time only 30% had job stability - caused large staff turnover. Despite lack of staff, the state team was found to be motivated by the stimulus of becoming more qualified, doing research, being awarded prizes and mass media publicizing of the program.
The legitimacy of its actions as seen by society was perceived to be positive by state health managers, as a result of recreational actions carried out in collective treatment target locations, with adherence by individuals from those communities and neighboring communities C+. Municipality C perceived little legitimacy: local educational actions were not followed by sanitation improvements C-.
Discussion
State health management was found to indicate a converging context for the SANAR program implementation in most of the categories analyzed. The other actors pointed out certain contradictions in the discourse of respondents from the Pernambuco State Health Department, whereby we found partial consistency between the responses of regional managers and those of the municipalities located in their respective regions. Interviewed technicians and managers acknowledged the program’s relevance, its activities and priorities. Furthermore, results observed in the municipalities and in the regional health divisions were similar to those of studies conducted both in Pernambuco18 and at national level,19 as regards the shortage of skilled professionals dedicated to achieving information quality, shortage of supplies and available vehicles. Despite the obstacles, state investment in continuing education was widely observed, converging positively for the implementation of health professional training actions, as well as their being valued in the division of responsibilities within SANAR as an institution.19
There was a favorable context for financial investment for the achievement of program actions, according to the respondents from Pernambuco State Health Department and from Municipality C, reflecting the epidemiological surveillance component being classified as “implemented” in this municipality. In Municipalities A and B, carrying out partial sample surveys and failure to send official documentation following evaluation of collective treatment are similar to findings of other studies carried out in the states of Pernambuco20,21 and Minas Gerais.22 In contrast, underreporting was not found in any of the three municipalities, which periodically input cases to the Schistosomiasis Control Program Information System.
Monitoring actions were favorable to program implementation. This result was also pointed out by another study involving two municipalities in the Zona da Mata region in Pernambuco.20 This finding is consistent with state management priorities, which uses participatory methodology in its monitoring practice, involving state and municipal actors in Monitoring Panel implementation. This action has the potential to promote municipal autonomy:
[...] besides informing decision-making, monitoring is understood as a reflective practice capable of promoting individual and institutional learning, continuous improvement of management processes, greater transparency and accountability.23
Despite this, some regional and municipal managers perceived monitoring as “account rendering” and this is possibly one of the reasons for them reporting technical and managerial autonomy as being incipient.
However, we found some degree of autonomy in as far as municipal managers dialog with other sectors, this being a favorable aspect for program implementation. This intersectoral interaction is important due to diverse approaches having the potential for positive influence on the disease’s social determinants. In this sense, a survey published in 2015 is worthy of attention.24 It was carried out in hyperendemic areas elected by SANAR - including areas of municipalities covered in this study -, which found the existence of partial or no piped water, sanitary facilities, septic tanks and sewage collection and treatment. This reality could be different if intersectoral articulation were more consolidated.19
Interaction with research institutions, mainly undertaken by Pernambuco State Health Department and by Municipality A, was the object of consultancy services carried out by the Ministry of Social Development and Fight against Hunger in partnership with the Oswaldo Cruz Foundation. This included incentives from agencies that support studies on neglected diseases; as well as continuing education in Pernambuco and other states.25
Intrasectoral communication between Health Surveillance and Primary Health Care was seen as an unfavorable context, resembling the findings of Albuquerque, Mota and Felisberto.18 This fact is associated with the incipient organization of the referral network, as perceived by all three municipalities. The planning of emergency hospitals to assist severe cases, accessible to endemic areas, would favor care comprehensiveness without affecting the continuity of wider health policies, such as SANAR.26
Community leaders should have their political participation guaranteed in the Municipal Health Councils, in planning control actions and awareness raising about the disease’s impact.22 However, social participation in this way was seen to be weak by most bodies covered by the study. This partially corroborates the findings of Westphal et al.27 when studying civil society participation in the agreement of health promotion action agendas in the Brazilian Southeast region, even though decisions were centralized by the government. Also related to community participation, besides contributing to the program sustainability because of their potential to add legitimacy, program educative actions were evaluated as unsatisfactory by all three municipalities. This highlights, yet again, the fragility of health education about schistosomiasis, considering the spelling mistakes, inadequate nomenclature, illustrations and recommendations, as well as inaccuracies in the description of the disease cycle by most educational materials evaluated by Massara et al.,28 intended to approach a disease defined by the same authors as “silent and despised”.
Evaluation of sustainability found situations converging on implementation of the intervention, especially in contexts noted by Pernambuco State Health Department and by Municipality C. However, staff turnover and insufficiency were considered to be difficulties in this sense. In relation to staff turnover, Stancato and Zilli29 evaluate the issue as a reflection of unsatisfactory work conditions, lack of physical, social and emotional security, and professional demotivation. In our study, inadequate physical conditions were also mentioned; however, technicians and managers were motivated to work on the schistosomiasis control actions planned by the SANAR program.
It is important to highlight that this evaluation can be replicated in other scenarios, besides being able to be adapted to neglected diseases in general: its design has shown itself to be appropriate not only for the structure and composition of the Schistosomiasis Control Program, but also for the general guidelines for the control of other diseases provided for in the Program to Combat Neglected Diseases.
Finally, some contradictory discourses among the informants from various management levels should be considered. In addition, although the focus of this article was limited to the year 2014 as the study period, cross-sectional evaluation research may suffer the influence of program performance in previous years.
It is evident that this study has brought explanatory information on the weaknesses and strengths of schistosomiasis control actions. Given the recognized pioneerism of SANAR in Brazil, attention is drawn to the possibility of this study contributing to the establishment of sustainable Brazilian public policies to combat neglected diseases, especially in municipal health care services.
REFERENCES
1. Katz N. Inquérito Nacional de Prevalência da Esquistossomose mansoni e Geo-helmintoses. Belo Horizonte: CPqRR; 2018. 76 p. Disponível em: https://www.arca.fiocruz.br/handle/icict/25662 [ Links ]
2. Pordeus LC, Aguiar LR, Quinino LRM, Barbosa CS. A ocorrência das formas aguda e crônica da esquistossomose mansônica no Brasil no período de 1997 a 2006: uma revisão de literatura. Epidemiol Serv Saude. 2008 jul-set;173:163-75. [ Links ]
3. Ministério da Saúde BR, Secretaria de Vigilância em Saúde. Departamento de Vigilância em Doenças Transmissíveis. Plano integrado de ações estratégicas de eliminação da hanseníase, filariose, esquistossomose e oncocercose como problema de saúde pública, tracoma como causa de cegueira e controle das geohelmintíases: plano de ação 2011-2015. Brasília: Ministério da Saúde; 2012. [ Links ]
4. Ministério da Saúde BR, Secretaria de Vigilância em Saúde. Departamento de Vigilância das Doenças Transmissíveis. Vigilância da esquistossomose mansoni: diretrizes técnicas. 4. ed. Brasília: Ministério da Saúde; 2014. [ Links ]
5. Saucha CVV, Silva JAM, Amorim LB. Condições de saneamento básico em áreas hiperendêmicas para esquistossomose no estado de Pernambuco em 2012. Epidemiol. Serv. Saúde [Internet]. 2015 Set [citado 2017 Out 05];243:497-506. Disponível em: Disponível em: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S2237-96222015000300497&lng=pt Doi: http://dx.doi.org/10.5123/S1679-49742015000300015 [ Links ]
6. Barbosa CS, Souza GEC, Campos JV, Oliveira FJM, Silva MMC, Oliveira ECA, et al. Morbidity of mansoni schistosomiasis in Pernambuco - Brazil: Analysis on the temporal evolution of deaths, hospital admissions and severe clinical forms 1999-2014, Acta tropica 2016 Dez;164:10-16. Doi: https://doi.org/10.1016/j.actatropica.2016.06.024 [ Links ]
7. Secretaria Estadual de Saúde Pernambuco. Perfil Socioeconômico, Demográfico e Epidemiológico. Recife: Secretaria Estadual de Saúde; 2016. [ Links ]
8. Secretaria Estadual de Saúde Pernambuco. Programa de Enfrentamento das Doenças Negligenciadas no Estado de Pernambuco/SANAR - 2011-2014. Recife: Secretaria Estadual de Saúde; 2013. [ Links ]
9. World Health Organization. Preventive chemotherapy in human helminthiasis: coordinated use of anthelminthic drugs in control interventions: a manual for health professionals and programme managers. Geneva: WHO Library; 2006. [ Links ]
10. Pernambuco. Secretaria Estadual de Saúde. A Renovação da Saúde Pública em Pernambuco 2007/2014: Sistematização da Experiência. Recife: Secretaria Estadual de Saúde; 2014. 116 p. [ Links ]
11. Champange F, Brousselle A, Hartz Z, Contandriopoulos A-P, Denis J-L. A análise de implantação. In: Champange F, Brousselle A, Hartz Z, Contandriopoulos A-P, Denis J-L. organizadores. Avaliação: conceitos e métodos. Rio de Janeiro: Editora FIOCRUZ; 2011. p. 217-238. [ Links ]
12. IBGE - Instituto Brasileiro de Geografia e Estatística [Internet]. Cidades [citado 2018 Ago 06]. Disponível em: Disponível em: https://cidades.ibge.gov.br/brasil/pe/panorama [ Links ]
13. Mclaughlin JA, Jordan GB. Evaluation and Program Planning Logic models: a tool for telling your program's performance story. New Yor; n. 22; 1999; p. 65-72. [ Links ]
14. Secretaria Estadual de Saúde Pernambuco. Cadernos de Monitoramento do Programa Sanar: Esquistossomose, Vol.1. Recife: Secretaria Estadual de Saúde; 2013. 23p. [ Links ]
15. Denis J, Champagne F. Análise de implantação. In: Hartz ZMA. Avaliação em saúde: dos modelos conceituais à prática na análise de implantação de programas. Rio de Janeiro: Fiocruz; 1997. p. 49-88. [ Links ]
16. Bardin L. L’Analyse de contenu. Editora: Presses Universitaires de France, 1977. Bardin L. Ánálise de conteúdo. SP: Edições 70, 2011. [ Links ]
17. Alves CKA, Carvalho EF, Cesse Eduarda AP, Natal S, Bezerra LCA, Felisberto E. Análise da implantação de um programa com vistas à institucionalização da avaliação em uma Secretaria Estadual de Saúde. Rev Bras Saude Mater Infant. 2010 nov 16;10Suppl 1:145-56. [ Links ]
18. Albuquerque AC, Mota ELA, Felisberto E. Descentralização das ações de vigilância epidemiológica em Pernambuco, Brasil. Cad Saude Publica, Rio de Janeiro. 2015 abr;314:861-73. [ Links ]
19. Tibirica SHC, Guimaraes FB, Texeira MTB. A esquistossomose mansoni no contexto da política de saúde brasileira. Cienc Saude Coletiva. 2011; 16 supl. 1:1375-81. [ Links ]
20. Quinino LRM, Samico I, Barbosa C. Avaliação do grau de implantação do programa de controle da esquistossomose em dois municípios da Zona da Mata de Pernambuco, Brasil. Cad Saude Coletiva. 2010;18:536-44. [ Links ]
21. Melo MISB. Análise da implantação das ações de controle da esquistossomose na estratégia de saúde da família: um estudo de caso em localidade litorânea vulnerável do estado de Pernambuco [Dissertação]. Recife PE: Fundação Instituto Oswaldo Cruz, Centro de Pesquisas Aggeu Magalhães; 2015. [ Links ]
22. Quites HFO, Abreu MNS, Matoso LF, Gazzinelli A. Avaliação das ações de controle da esquistossomose na Estratégia de Saúde da Família em municípios do Vale do Jequitinhonha em Minas Gerais. Rev Bras Epidemiol. 2016 abr-jun;192:375-89. [ Links ]
23. Costa JMBS, Felisberto E, Bezerra LCA, Cesse EAP, Samico IC. Monitoramento do desempenho da gestão da vigilância em saúde: instrumento e estratégias de uso. Cienc Saude Coletiva [Internet]. 2013 mai [citado 2018 Jan 26];185:1201-16. Disponível em: Disponível em: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1413-81232013000500002&lng=en Doi: http://dx.doi.org/10.1590/S1413-81232013000500002 [ Links ]
24. Saucha CVV, Silva JAM, Amorim LB. Condições de saneamento básico em áreas hiperendêmicas para esquistossomose no estado de Pernambuco em 2012. Epidemiol Serv Saude [Internet]. 2015 set [citado 2018 Jan 04];243:497-506. Disponível em: Disponível em: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S2237-96222015000300497&lng=en Doi: http://dx.doi.org/10.5123/S1679-49742015000300015 [ Links ]
25. Araújo-Jorge T, Matraca M, Moraes Neto A, Trajano V, D´Andrea P, Fonseca A. Doenças negligenciadas, erradicação da pobreza e o Plano Brasil Sem Miséria. In: Campello T, Falcão T, Costa PV. O Brasil sem miséria. Brasília: MDS; 2014; p. 703-724. [ Links ]
26. Vidal LM, Barbosa AS, Ribeiro RMC, Silva LWSS, Vilela ABA, Prado FO. Considerações sobre esquistossomose mansônica no município de Jequié, Bahia. Revista de Patologia Tropical. 2011 out-dez;404:367-82. [ Links ]
27. Westphal MF, Fernandez JCA, Nascimento PR, Zioni F, André LM, Mendes R, et al. Práticas democráticas participativas na construção de agendas sociais de desenvolvimento em municípios do Sudeste brasileiro. Ambient Soc [Internet]. 2013 jun [citado 2018 Jan 04];162:103-28, Disponível em: Disponível em: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1414-753X2013000200007&lng=pt&nrm=iso. Acessos em 02 jan. 2018 . doi: http://dx.doi.org/10.1590/S1414-753X2013000200007 [ Links ]
28. Massara CL, Murta FLG, Enk MJ, Araújo AD, Modena CM, Carvalho OS. Caracterização de materiais educativos impressos sobre esquistossomose, utilizados para educação em saúde em áreas endêmicas no Brasil. Epidemiol Serv Saude [Internet]. 2016 set [citado 2017 dez 21]; Disponível em: Disponível em: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S2237-96222016000300575&lng=en&nrm=iso doi: http://dx.doi.org/10.5123/s1679-49742016000300013 [ Links ]
29. Stancato K, Zilli PT. Fatores geradores da rotatividade dos profissionais de saúde: uma revisão da literatura. Rev Adm Saude. 2010 abr-jun;1247:87-99. [ Links ]
Received: May 15, 2018; Accepted: February 17, 2019











 texto em
texto em 
 Curriculum ScienTI
Curriculum ScienTI

