Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Epidemiologia e Serviços de Saúde
versión impresa ISSN 1679-4974versión On-line ISSN 2237-9622
Epidemiol. Serv. Saúde vol.28 no.2 Brasília jun. 2019 Epub 29-Jul-2019
http://dx.doi.org/10.5123/s1679-49742019000200019
ORIGINAL ARTICLE
Human leptospirosis in Porto Alegre, Rio Grande do Sul, Brazil, 2007-2013: characterization of confirmed cases and spatial distribution*
1Secretaria de Estado da Saúde do Rio Grande do Sul, Escola de Saúde Pública, Porto Alegre, RS, Brasil
2Secretaria Municipal de Saúde de Porto Alegre, Coordenadoria Geral de Vigilância em Saúde, Porto Alegre, RS, Brasil
Objective:
to characterize confirmed human leptospirosis cases resident in Porto Alegre, Rio Grande do Sul, Brazil, between 2007 and 2013, and their spatial distribution.
Methods:
this was a descriptive study of cases registered on the Notifiable Diseases Information System; we investigated neighborhoods and areas in the catchment area of Health Units (US) with highest case occurrence, using spatial analysis as per the Kernel technique.
Results:
228 cases were confirmed in the period, with cumulative incidence of 2.3 cases/100,000 inhabitants; the majority were adult males (81.6%), economically active (82.5%) and had low schooling (45.8%); the main occupations were recyclable waste collector (15.8%) and builder/builder’s mate (15.2%); six priority US were identified for leptospirosis control and prevention actions.
Conclusion:
the epidemiological profile and spatial distribution of cases suggest that there continue to be environmental risk factors favoring human leptospirosis occurrence in these areas.
Keywords: Leptospirosis; Epidemiological Monitoring; Residence Characteristics; Epidemiology, Descriptive
Introduction
Leptospirosis is an acute febrile illness than can occur in humans or animals anywhere in the world.1 It is caused by bacteria of the Leptospira genus and is transmitted through contact with animal reservoirs2 and soil and water contaminated with their urine.3Leptospirae are spirochetes, of distinct serogroups and serovars, which infect mammals with consequences ranging from asymptomatic infections to serious illness.4 They penetrate the body through cut or scratched skin, or via mucous membrane of the mocth, nose and eyes,5 while person-to-person transmission is rare.1
In Brazil, leptospirosis has social and economic significance.6 Considered to be an important Public Health problem,7 leptospirosis is endemic in Brazil, appearing in rainy periods, especially in areas with flooding associated with large low-income agglomerations, inadequate sanitation conditions and high levels of rodent infestation.1 The highest incidence of leptospirosis occurs in tropical zones,8 resulting in high hospital costs and lost working days, as well as high lethality (up to 40%) in more serious cases. Its true incidence is unknown because of lack of information,8 a high proportion of subclinical infection9-11 and unavailability of diagnostic methods, thus hindering its detection.8
Immediate notification of leptospirosis is mandatory within 24 hours of a case being suspected or confirmed, as determined by Health Ministry Ordinance Consolidation Ordinance No. 4, dated September 18th 2017, which defines the list of diseases, conditions and Public Health events for which reporting is mandatory.
In Porto Alegre, RS, leptospirosis incidence between 1996 and 2007 varied between 0.85/100,000 inhabitants (2004) and 7.14/100,000 inhab. (2001), associated with the disorderly growth of the city, lack of environmental sanitation and public water supply, lack of sewers for domestic sewage and lack of waste management, thus increasing the problem of synanthropic rodent infestation.12
A survey conducted in 2007 found that 87.7% of confirmed cases needed to be hospitalized, 64.9% of which were icteric, suggest that mild cases were not reported.
In the past contracting leptospirosis was related to work environment. Some professions imply greater exposure to the disease’s etiological agent;1,12 however, environmental changes have now become important risk factors,6 reducing the importance of occupation as an exposure factor.
The objective of this study was to characterize confirmed cases of human leptospirosis resident in the municipality of de Porto Alegre, Rio Grande do Sul, Brazil, between 2007 and 2013, as well as it spatial distribution.
Methods
This is a descriptive study of confirmed leptospirosis cases conducted in the urban area of Porto Alegre, RS (30°01’58’’S and 51°13’48’’O), which according to the 2010 Demographic Census13 had a population of 1,409,351 inhabitants living in an area of 496,682km². Rio Grande do Sul is a strategic state within the Socthern Common Market (Mercosur), as its capital, Porto Alegre, is at the geographical center of the main roctes of the continent’s Socthern Cone, halfway between Buenos Aires / Montevideo and São Paulo / Rio de Janeiro. Porto Alegre is on the BR-290 and BR-116 federal highways and is thus connected to all the other Brazilian states and also to Uruguay and Argentina.14
In 2016, Porto Alegre officially had 81 districts, although there were still areas of its territory withoct an official name: the so-called Undefined Zones, known by the population according to their local names, as is the case of Morro Santana, Passo das Pedras and Aberta dos Morros. The municipality’s most populous districts are Rubem Berta (87,367 inhab.), Sarandi (59,707 inhab.), Restinga (51,569 inhab.) and Lomba do Pinheiro (51,415 inhab.).15
The Archipelago district, comprised of 16 islands under the jurisdiction of Porto Alegre, covers approximately 4,500ha which form the Jacuí Delta State Park, along with other islands belonging to neighboring municipalities. This region forms part of the state’s coastal lowlands and the Archipelago district is subject to annual flooding that paralyzes almost all human rural and urban activities in the region. The islands that have high concentrations of human septlements accounting for 90% of the district’s population are: Ilha Grande dos Marinheiros, Ilha das Flores, Ilha do Pavão and Ilha da Pintada.
In this study we used secondary data on confirmed autochthonous human leptospirosis cases living in Porto Alegre between 2007 and 2013. The data were retrieved from the Notifiable Diseases Information System (SINAN), using the NET version installed in 2007. The choice of the post-2007 period is justified by the difference in the database structure and variables in years prior to 2007 when the SINAN-Windows version was used.
Case confirmation by the epidemiological surveillance service was done based on clinical-laboratory and clinical-epidemiological criteria adopted by the Ministry of Health.1 This enabled us to obtain the number of leptospirosis cases per district. The municipal environmental surveillance service roctinely undertakes on-site investigation of confirmed cases and determines, jointly with the epidemiological surveillance service, the likely place of infection (LPI).
We analyzed 72 variables on the notification form relating to the person, time and place. The SINAN notification form has 2,428 codes for the ‘occupation’ variable. In our study, we selected 63 (2.6%) codes which we grouped together into 44 items based on the criterion of similarity, with the aim of achieving more accurate analysis.
We checked the notification forms of all autochthonous leptospirosis cases in Porto Alegre regarding completion of the variable field ‘risk situation occurring in the 30 days before onsep of the first symptoms’ - whether it had been completed, left blank or if this information was unknown. Analysis of this variable considered the 12 risk situations shown on the notification form (place with signs of rodents; direct contact with rodents; flood water or mud contact with/cleaning; rubbish/debris; contact with/cleaning of cesspool, grease trap or sewer; river, stream, lagoon or reservoir; waste land; animal rearing; water tank; planting/harvesting (farm work); grain/food storage; other). Notifications with this field left blank were excluded from the study.
All forms notifying leptospirosis were taken into consideration when checking the quality of the database in relation to how “clean” it was in terms of information completeness and consistency. Corrections of SINAN information are done by the City Health Department and, whenever possible, inconsistent data were corrected on the database.
We calculated the incidence and lethality coefficients of confirmed leptospirosis cases, where the denominator was the total number of cases identified in the population of Porto Alegre in 2010, according to the Brazilian Institute of Geography and Statistics (IBGE).13
With regard to the environmental analysis, the cases were distributed spatially and the information was organized so as to define areas with higher density of likely places of infection of leptospirosis cases. The regions with the highest concentration of places of infection were compared with those that have been historically described since the year 2000.
The spatial analysis involved georeferencing by LPI. Residential addresses and LPI addresses were qualified and georeferenced using street axes as spatial structures, in order to locate case occurrence by health center, using the cartographic database of Porto Alegre addresses provided by the municipality’s Data Processing Company (PROCEMPA). Georeferencing was supported by TerraView open software, version 4.2.1, developed by the National Space Research Institute (INPE).
This study took into consideration the studies of Barcellos et al.,3,16 adapted in order to analyze the highest density of likely places of infection by leptospirosis per health center located in the hotspots identified.
Following georeferencing, we built a Kernel map, with point density per km², adaptive radius, calculation according to density and quartic function, for the seven years under analysis, whereby clusters were identified.17 This technique generates a density surface in order to be able to view a concentration of events indicating some sort of spatial clustering.18
Imported cases, cases with unidentified LPI or cases the address of which could not be georeferenced were excluded from the environmental analysis.
The study project was approved by the Public Health School Research Ethics Committee (CEPS/ESP), part of the Rio Grande do Sul State Health Department - Certification of Submission for Ethical Appraisal (CAAE) No. 42311515.2.0000.5312 - and also by the Porto Alegre City Health Department Ethics Committee - CAAE No. 42311515.2.3001.5338.
Results
Between 2007 and 2013, among suspected leptospirosis cases held on SINAN, 228 were confirmed as residing in Porto Alegre and their LPI was also Porto Alegre. These cases were considered to be autochthonous. The highest percentage of these cases (86.4%) had been confirmed by the clinical-laboratory criterion: average of 33 cases/year, varying between 20 (2012) and 41 (2007), with cumulative incidence of 2.3 cases/100,000 inhabitants. (Figure 1).
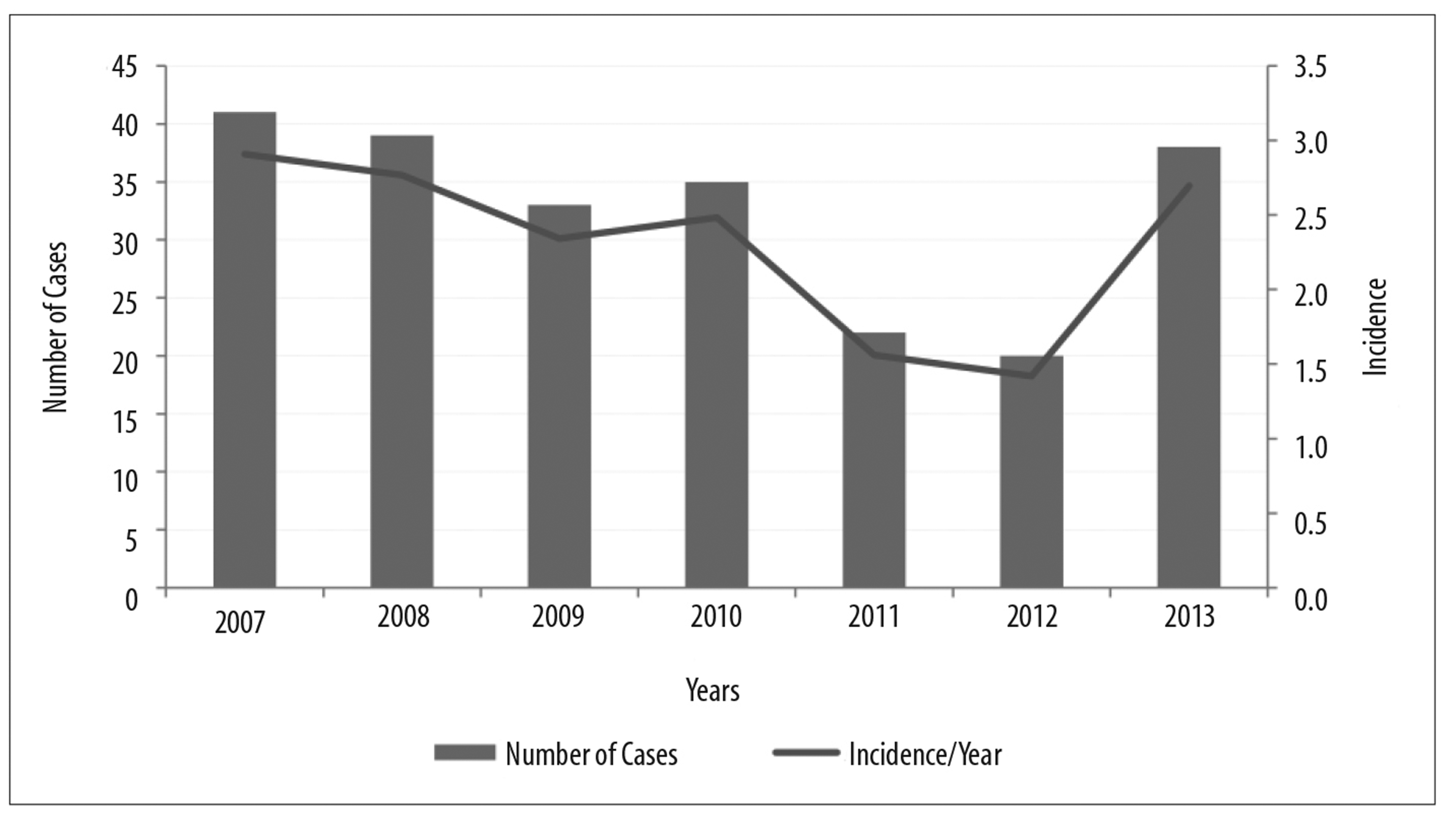
Figure 1 - Distribution and accumulated incidence (per 100,000 inhabitants) of autochthonous leptospirosis cases per year, Porto Alegre, Rio Grande do Sul, 2007-2013
81.6% of cases (186/228) were male and 82.5% (188/228) were of economically active age [15-59 years old], and average age was 37 years (minimum age 3 years and maximum age 73 years); 45.8% (98/214) had incomplete elementary education (Table 1).
Table 1 - Sociodemographic characteristics of autochthonous leptospirosis cases, Porto Alegre, Rio Grande do Sul, 2007-2013
| Characteristics | Total | % |
|---|---|---|
| Sex | ||
| Male | 42 | 18.42 |
| Female | 186 | 81.58 |
| Age range (in years) | ||
| 0-14 | 17 | 7.46 |
| 15-29 | 69 | 30.26 |
| 30-44 | 59 | 25.88 |
| 45-59 | 60 | 26.32 |
| ≥60 | 23 | 10.09 |
| Schooling | ||
| Illiterate | 2 | 0.93 |
| Incomplete elementary education | 98 | 45.79 |
| Complete elementary education | 30 | 14.02 |
| Incomplete high school education | 15 | 7.01 |
| Complete high school education | 14 | 6.54 |
| Incomplete higher education | 3 | 1.40 |
| Complete higher education | 4 | 1.87 |
| Unknown | 47 | 21.96 |
| Does not apply | 1 | 0.47 |
With regard to the clinical data, the most frequent signs and symptoms were: feber, 96.5% (219/227); myalgia, 85.0% (193/227); exhaustion, 77.0% (175/226); and headache, 75.1% (169/225). Although the most frequent signs and symptoms were mild, we found several severe cases, including those with jaundice (62.1%), kidney failure (35.8%) and respiratory changes (34.4%). These indicate progression to Weil’s syndrome.
With regard to care provided as cases progressed, 85.5% (n=227) were hospitalized, 26 of whom died. 88.5% of these deaths were male. On average there were four deaths per year; and lethality was 11.4% in the period studied.
In relation to the characteristics of the LPI of confirmed cases, 92.0% occurred in urban areas, 2.6% in peri-urban areas and less than 1% in rural areas; in 4.4% of cases, LPI information was recorded as ‘unknown’.
When analyzing the types of infection environments, we found that approximately half the cases occurred at home (48.0%), 27.8% at work, 10.6% in another environment and 4.9% during leisure, while for 8.9% this situation was unknown. There was one record withoct the infection environment field filled in even after the case had been investigated.
Regarding complementary data on cases, standing oct among the ‘occupation’ variable were recyclable waste collectors (15.8%) and builder/builder’s mate (15.2%) as those most frequently affected by leptospirosis, followed by housewives (8.2%), students (7.0%), retired people (5.7%) and domestic servant/general service employees (4.4%). No other professions exceeded 4%, and in 55.6% of these cases the profession was only mentioned once.
As for the ‘risk situation occurring in the 30 days before onsep of the first symptoms’ variable, 55.8% (n=226) of patients had been exposed to a place with signs of rodents, while 46.9% (n=226) had been in direct contact with rodents, 41.0% (n=227) had been in contact with flood water or mud and 32.7% (n=227) had been in contact with rubbish or debris (Table 2). Nine districts were identified as having leptospirosis cases: Archipelago (20 cases), Partenon (16), Sarandi (16), Lomba do Pinheiro (15), Rubem Berta (12), Restinga (9), São José (9), Bom Jesus (8) and Santa Tereza (7), corresponding to 60.0% of total cases, varying between 20 and seven cases. Porto Alegre’s other districts accounted for less than 2% of total cases.
Table 2 - Risk situation proportion of confirmed and recorded leptospirosis cases, Porto Alegre, Rio Grande do Sul, 2007-2013
| Risk situation | Total cases | Total | Risk situation | |||
|---|---|---|---|---|---|---|
| Yes | No | Unknown | Missing | n | (%) | |
| Place with signs of rodents | 126 | 85 | 15 | 2 | 226 | 55.8 |
| Direct contact with rodents | 106 | 104 | 16 | 2 | 226 | 46.9 |
| Flood water or mud | 93 | 120 | 14 | 1 | 227 | 41.0 |
| Rubbish or debris | 74 | 136 | 17 | 1 | 227 | 32.7 |
| Contact with/cleaning of cesspool, grease trap or sewer | 44 | 166 | 16 | 2 | 226 | 19.5 |
| River, stream, lagoon or reservoir | 41 | 170 | 15 | 2 | 226 | 18.1 |
| Waste land | 38 | 169 | 18 | 3 | 225 | 16.9 |
| Animal rearing | 38 | 172 | 16 | 2 | 226 | 16.8 |
| Water tank | 9 | 200 | 17 | 2 | 226 | 4.0 |
| Planting/harvesting (farm work) | 8 | 200 | 16 | 4 | 224 | 3.6 |
| Grain/food storage | 5 | 204 | 17 | 2 | 226 | 2.2 |
| Other | 40 | 163 | 19 | 6 | 222 | 18.0 |
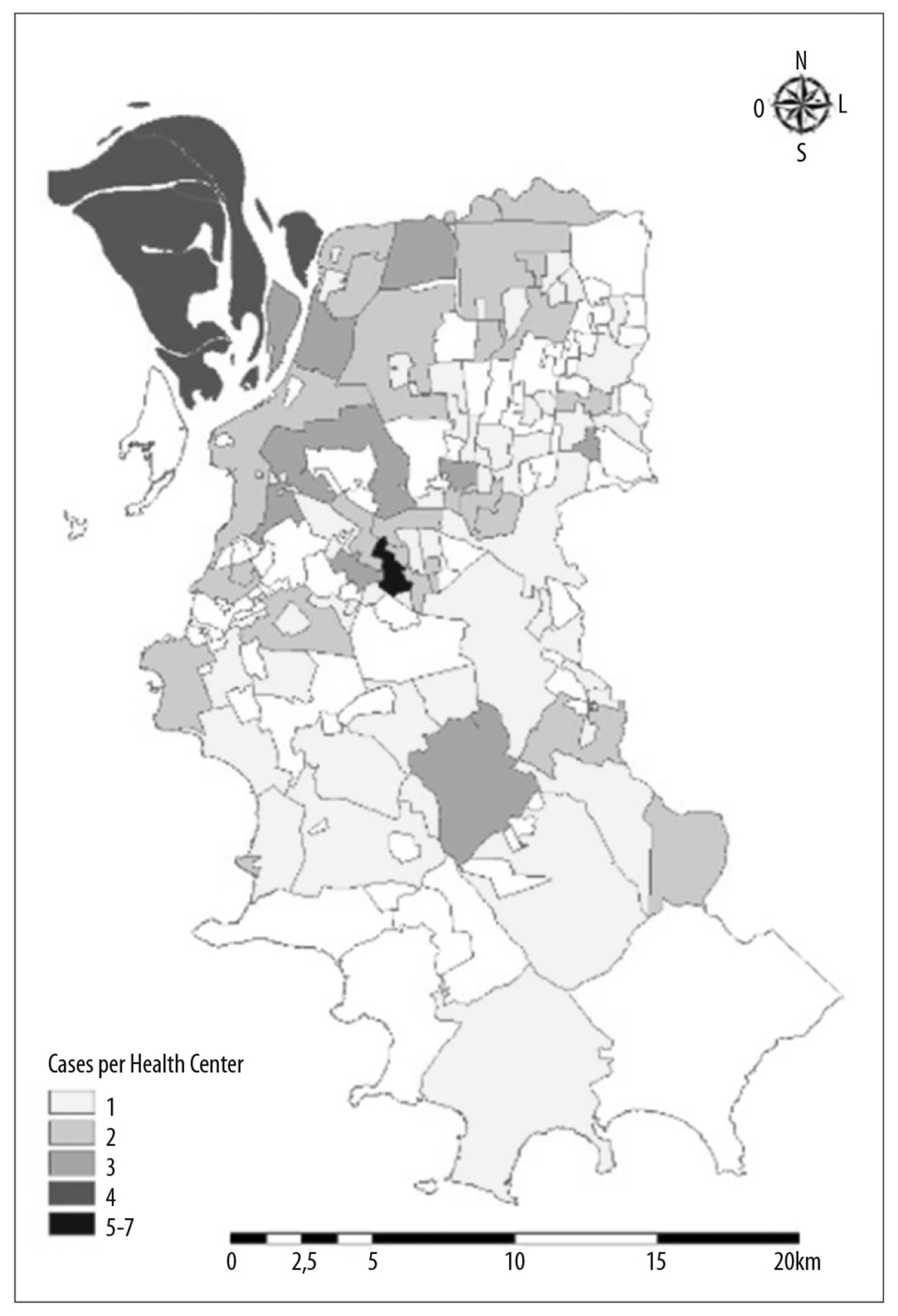
Figure 2 is a map of Porto Alegre by Health Center and shows density of leptospirosis cases per LPI, estimated using the Kernel ratio, per km². Of the total cases, 124 (54.4%) had valid addresses for the LPIs. The darker areas indicate higher case density.
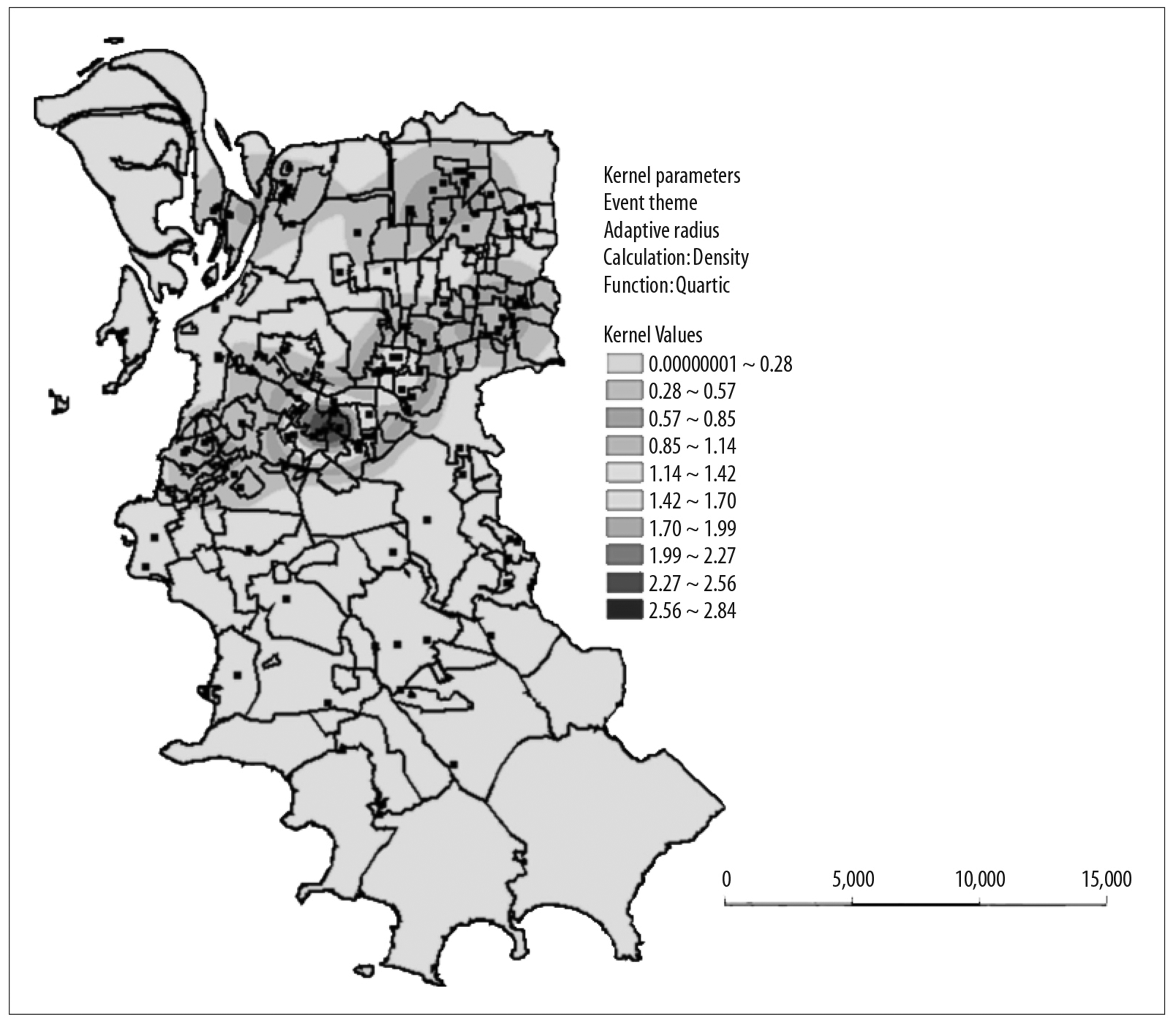
Figure 2 -Kernel map of the number of leptospirosis cases per likely place of infection, Porto Alegre, Rio Grande do Sul, 2007-2013
Porto Alegre has a total of 133 Health Center territories.19 The Kernel analysis showed that four Health Centers were part of the “hottest spots”, with three cases per km², namely: São Miguel, Bananeiras, Campo da Tuca and São José. The Ilha dos Marinheiros, Ilha do Pavão, Bom Jesus, Vila Pinto and Jardim Carvalho Health Centers also appeared in the analysis, although with fewer than three cases.
Complementing the Kernel analysis, Figure 3 shows leptospirosis case occurrence aggregated according to health service areas in Porto Alegre, per LPI. With results similar to those of the Kernel ratio, the São José Health Center has the largest number of cases. However, here the Archipelago district stands oct more and, although it was present in the Kernel analysis, it was not part of the “hotspot”. Two of the Archipelago’s islands, Ilha Grande dos Marinheiros and Ilha do Pavão, had the highest number of leptospirosis cases in the period studied.
Discussion
Leptospirosis cases recorded in Porto Alegre in the period studied occurred mainly among males of economically active age11 and individuals with incomplete elementary education. Contagion occurred mainly in urban areas and at home,11 with a tendency of more cases of people reporting the presence of signs of rodents or even direct contact with rodents. Standing oct among the main signs and symptoms were feber and myalgia, with jaundice in serious cases, requiring hospitalization and producing a lethality rate of 11.4%. Average lethality in Porto Alegre between 1995 and 2003 was 12.1%,20 similar to the rate we found in this study, whereas recent Ministry of Health studies indicate average lethality of 9% for Brazil as a whole.21
Considered to be a disease associated with poverty and common in developing countries,1,11,22-24 leptospirosis has the same national profile with regard to our demographic findings, given the schooling level of the cases which is a proxy of socio-economic status in Brazil:25 the highest proportion of infected people was found precisely among those with incomplete elementary education.
According to IBGE, all of Porto Alegre’s territory is considered to be an urban area. Small areas of the municipality, identified as peri-urban and rural, should be understand as being information biased by the patients themselves or by the person who assessed the place in question based on characteristics of the plot of land, micro-environment or other characteristics. Higher leptospirosis frequency in urban areas is a recorded fact:11 when evaluating the leptospirosis time series in Brazil (2000-2009), it was equally distributed, mainly in urban centers of the metropolitan regions of cities with large populations close to the Brazilian coast.
It is well known that leptospirosis affects populations exposed to infection owing to their occupation, often associated with contact with production livestock, sanitation workers, as well as following exposure to flooding.1,11 In Brazil leptospirosis is predominant among people who live or work in places with inadequate sanitation infrastructure and who are exposed to rodent urine. Similar to the finding of this study (36.6%), in 2007 Porto Alegre registered 36.0% of leptospirosis cases directly related to patients’ jobs,12 80% of whom worked as waste collectors and street sweepers. Indeed, occupation can be related to types of environment where infection occurs. In 2002, households accounted for the highest proportion of recorded infection environments (34%),26 similar to the findings of our study. However, consideration needs to be given to interpretation of a possible information bias: in the case of recyclable waste collectors, they take what they collect to their homes, thus causing confusion between work environment and household environment.
In the year 2000, leptospirosis octbreaks occurred in Porto Alegre arising from specific work situations (among soldiers during their activities) and also following flooding,27 thus modifying the homogenous pattern of the disease’s epidemiological data.28 In 2002, heavy rain contributed to the flooding factor.26 These are data which may possibly have been reflected in the years that followed. Moreover, the study conducted by Bello in 201223 found significant results linking leptospirosis to seasonal climatic factors (the ‘flood water or mud’ variable). This association reinforces the occurrence of octbreaks related to natural disasters and consequent increase in rainfall,11 accompanied by an increasing trend in the number of cases in the most affected environment, both in the work environment and in the household environment.
In Porto Alegre 5.2% of the population lives in regions with uncovered sewers, 11.8% in areas with no sewers19 and 6.0% with accumulated waste in the street, even though it is reported that 100% of the city’s waste is collected. The determinant factors mentioned, along with health surveillance, may be contributing to the profile of the leptospirosis situation remaining stable in the municipality, especially in the areas of the four Health Centers where leptospirosis cases are most frequent.
Taking Brazil as a whole, reports of high numbers of leptospirosis hospitalizations suggest that cases have been moderate to serious.1 In Porto Alegre, in the majority of cases the high hospitalization rate found may indicate lack of surveillance system sensitivity in identifying patients with initial symptoms of the disease;23 or this fact may be related to laboratory detection, given that diagnosis in Porto Alegre is performed by the Central State Laboratory (Lacen/RS), by means of serology tests confirming infection but withoct typifying serovars. It can be cogitated that hospitalized cases may have had infection with serovars frequently related to the most serious cases. In Brazil, as a general rule, the Icterohaemorrhagiae and Copenhageni serovars play this role,1 although this assumption could only be confirmed through more specific diagnosis.
We compared our findings of the highest number of cases per district with previous studies which performed time series analyses of the LPIs of leptospirosis cases in Porto Alegre between 1990 and 200026 and from 2001 to 2006 according to geographic distribution by district.29 The Partenon, Santa Tereza and Bom Jesus districts appeared in the two studies mentioned and also in our study as districts with the greatest concentration of cases; the São José,26 Rubem Berta29 andArchipelago29 districts were appeared in at least one of the studies mentioned and were also found in our study.
The result provided by complementary spatial analyses (Kernel analysis and case distribution according to Health Center and LPI) highlighted the Archipelago district with regard to case distribution analysis, in contrast to the Kernel analysis. This finding differs from the study of the decade comprising 1990-2000, when no cases were identified in the Archipelago district, suggesting the importance during evaluation of phenomena that provide evidence both of the same regions and also of different regions owing to the method used.17
An IBGE survey (2010) of the Archipelago district provided information on demographic growth according to participatory budget region from 2000 to 2010 and gave proof of an increase of 9.3% in the Island region.19 As a consequence of demographic growth there is increasing need for jobs and income. The Ilha Grande dos Marinheiros, Ilha das Flores and Ilha do Pavão islands have precarious urban infrastructure, are occupied by low-income families living in poorly built houses. The alternative local economic activity for many of these people is to work collecting recyclable waste.30 It is common for the local population to face difficulties owing to frequent flooding and this further reinforces the precarious nature of the majority of septlements there and, as a consequence, intensifies disorderly occupation of geologically unsuitable areas and results in a variety of environmental problems.
Even so, the inhabitants of these islands find alternative economic activities (collecting recyclable waste) on the Ilha Grande dos Marinheiros island. Although some formal recycling initiatives (both governmental and non-governmental) are being developed there, the number of informal jobs probably continues to be high. Many people turn their homes into sheds for storing the recyclable waste they collect. This fact - which causes this profession to be the most affected by leptospirosis - increases the likelihood of rodent proliferation and, consequently, contact with Leptospira contaminated environments. These is also the hypothesis of case notification having been improved in that region, principally because of the recent arrival of health professionals (doctors) at the local Health Centers who are highly aware in relation to identifying suspected leptospirosis cases.
Urban agglomeration, flooding, social vulnerability and risk occupations in the Island region can be considered to be some of the multifactorial determinants of the increased number of cases in that region. Also worthy of consideration is that certain ecological conditions, such as those found on the Islands, can be propitious to the circulation of peri-domestic rodents and thus contribute to the spread of leptospirosis.24
Spatial analysis - case clusters by Health Center shown by Kernel analysis - provided important information for the epidemiological and environmental surveillance services, as well as for the Health Center responsible for the territory. Once the most affected Health Centers are known, an integrated form of working between these sectors can be organized, by means of intervention in emergencies, obtaining resources intended to increase care capacity, as well as continuing training of local health workers.
A limitation in carrying oct this study was the identification of possible information bias in the filling in of several variables, resulting from confusion between work environment and home environment. Moreover, limitations were also found when assessing the ‘occupation’ variable: in 30.7% of cases, this information was either missing or the code had been adjusted according to the understanding of the person responsible for data entry when the field was filled in on the system. Another limitation relates to it being impossible to typify circulating serovars, thus preventing them from being related to the seriousness of the case or even with geographical predominance in a given area of the municipality.
It is better to analyze social questions locally, with precise knowledge of case LPIs, this being information widely used in spatial analyses. It is therefore important to highlight the need to improve the way in which the correct LPI is identified. Difficultly in determining these places is understandable when the patient has more than one exposure environment or when they do not have a fixed address (people who live on the streets). On the other hand, the disease notification form also does not have a specific field for filling in the LPI address, including street name and number and postcode. Withoct detailed and correct localization, it becomes difficult to adopt actions targeting a given location.
We conclude that trend analyses in relation to leptospirosis are important, especially Kernel spatial analysis of leptospirosis case distribution according to Health Center territory and LPI, although this analysis was based on just over half the addresses and this may have affected assessment of the true spatial distribution of the cases. This study identified that the priority regions, reported earlier, continue to have increased cases. It also highlighted a new region, namely the Archipelago district. Over time this district of Porto Alegre has aggregated more environmental risks of leptospirosis, mainly on the Ilha do Pavão and Ilha dos Marinheiros islands. Moreover, the repetition of cases in the same regions as previously described suggests that risk factors continue to exist there.
Identifying vulnerable areas by Health Center provides guidance to health service management as to actions in priority services, working on prevention in order to prepare in advance for cases occurring following heavy rain, or by means of actions targeting areas with more socio-economic problems. Once the most exposed groups have been identified, prevention and control measures must be put in place, encouraging increased occupational biosafety, along with improved hygiene and sanitation conditions for the population at greater risk of contracting leptospirosis.
Acknowledgements
Our thanks go to the Health Surveillance General Coordination sector (CGVS) of Porto Alegre City Health Department, especially its Managers, for allowing us to use the data and for the support provided. We thank the Communicable Diseases Surveillance team, within the epidemiology area of the Porto Alegre Health Surveillance service, for loaning the database for us to carry oct our study; as well as for their valuable contributions, especially Adelaide Pustai and Sônia Thiesen, in correcting data and suggestions given for enhancing our study. We thank the Rodent and Vector Surveillance Team, within the environmental area of the Porto Alegre Health Surveillance service, for the environmental information provided, for their help in the field and for their important contributions, especially Rosa Maria Jardim Carvalho. To the Integrated Health Residency, in particular with regard to health surveillance, of the Rio Grande do Sul Public Health School, for motivating us to produce this scientific article. To our esteemed colleague Márcio Heitor, for his bibliographical support. To Ivone Menegolla, for her epidemiological contribution and technical support. To Renata Mondini and Adriana Hans Fernandes, for their support throughoct the entire process. And our special thanks to Marco Antônio Barreto de Almeida, for his generous suggestions, patience and technical and emotional support to the authors of this article.
REFERENCES
1. Ministério da Saúde (BR). Secretaria de Vigilância em Saúde. Departamento de Vigilância Epidemiológica. Guia de vigilância epidemiológica [Internet]. 7. ed. Brasília: Ministério da Saúde; 2009 [citado 2019 maio 17]. 816 p. Disponível em: Disponível em: http://bvsms.saude.gov.br/bvs/publicacoes/guia_vigilancia_epidemiologica_7ed.pdf [ Links ]
2. Tassinari WS, Pellegrini DCP, Sabroza PC, Carvalho MS. Distribuição espacial da leptospirose no Município do Rio de Janeiro, Brasil, ao longo dos anos de 1996-1999. Cad Saúde Pública [Internet]. 2004 nov-dez [citado 2019 maio 17];20(6):1721-9. Disponível em: Disponível em: http://www.scielo.br/pdf/csp/v20n6/31.pdf . doi: 10.1590/S0102-311X2004000600031 [ Links ]
3. Barcellos C, Lammerhirt CB, Almeida MAB, Santos E. Distribuição espacial da leptospirose no Rio Grande do Sul, Brasil: recuperando a ecologia dos estudos ecológicos. Cad Saúde Pública [Internet]. 2003 set-out [citado 2019 maio 17];19(5):1283-92. Disponível em: Disponível em: http://www.scielo.br/pdf/csp/v19n5/17801.pdf . doi: 10.1590/S0102-311X2003000500007 [ Links ]
4. Perret C, Abarca K, Dabanch J, Solari V, Garcia P, Carrasco S, et al. Prevalencia y presencia de factores de riesgo de leptospirosis en una población de riesgo de la Región Metropolitana. Rev Méd Chile [Internet]. 2005 abr [citado 2019 maio 17];133(4):426-31. Disponível em: Disponível em: https://scielo.conicyt.cl/pdf/rmc/v133n4/art05.pdf . doi: 10.4067/S0034-98872005000400005 [ Links ]
5. WHO. World Health Organization. Leptospirosis [Internet]. 2018 [citado 2018 Nov 26]. Disponível em: Disponível em: http://www.who.int/topics/leptospirosis/en/ . [ Links ]
6. Ministério da Saúde (BR). Secretaria de Vigilância em Saúde. Leptospirose: o que é, causas, sintomas, tratamento, diagnóstico e prevenção [Internet]. Brasília: Ministério da Saúde ; 2014 [citado 2018 nov 26]. Disponível em: Disponível em: http://portalms.saude.gov.br/saude-de-a-z/leptospirose . [ Links ]
7. Ministério da Saúde (BR). Secretaria de Vigilância em Saúde. Departamento de Vigilância das Doenças Transmissíveis. Leptospirose: diagnóstico e manejo clínico [Internet]. Brasília: Ministério da Saúde ; 2014 [citado 2019 maio 17]. Disponível em: Disponível em: http://portalarquivos.saude.gov.br/images/pdf/2014/dezembro/02/Miolo-manual-Leptospirose-17-9-2014.pdf [ Links ]
8. Céspedes M. Leptospirosis: enfermedad zoonótica reemergente. Rev Peru Med Exp Salud Pública [Internet]. 2005 out-dez [citado 2019 maio 17];22(4):290-307. Disponível em: Disponível em: http://www.scielo.org.pe/pdf/rins/v22n4/a08v22n4.pdf [ Links ]
9. Bovet P, Yersin C, Merlen F, Davis CE, Perolat P. Factors associated with clinical leptospirosis: a population-based case-control study in the Seychelles (Indian Ocean). Int J Epidemiol [Internet]. 1999 Jun [citado 2019 May 17];28(3):583-90. Disponível em: Disponível em: https://academic.oup.com/ije/article/28/3/583/666233 . doi: 10.1093/ije/28.3.583 [ Links ]
10. Bharti AR, Nally JE, Ricaldi JN, Matthias MA, Dias MM, Lovett MA, et al. Leptospirosis: a zoonotic disease of global importance. Lancet Infect Dis [Internet]. 2003 Dec [citado 2019 May 17];3(12):757-71. Disponível em: Disponível em: https://www.thelancet.com/journals/laninf/article/PIIS1473-3099(03)00830-2/fulltext . doi: 10.1016/S1473-3099(03)00830-2 [ Links ]
11. Araújo WN. Aspectos epidemiológicos da leptospirose no Brasil, 2000 a 2009 e a avaliação do conhecimento e das atitudes sobre a doença em uma favela na cidade de Salvador, Bahia [tese]. Salvador: Fundação Instituto Oswaldo Cruz; 2010. Disponível em: https://www.arca.fiocruz.br/handle/icict/4324 [ Links ]
12. Thiesen SV, Rosado RM, Vargas CRB, Bertolo CV, Poitevin L. Aspectos relacionados à ocorrência de leptospirose em Porto Alegre no ano de 2007. Bol Epidemiol Porto Alegre [Internet]. 2008 ago [citado 2019 maio 17];10(38):1-4. Disponível em: Disponível em: http://lproweb.procempa.com.br/pmpa/prefpoa/cgvs/usu_doc/boletimepidemiologico-cgvs-sms-pmpa-38.pdf [ Links ]
13. Instituto Brasileiro de Geografia e Estatística. Pesquisa de informações básicas municipais [Internet]. Rio de Janeiro: Instituto Brasileiro de Geografia e Estatística; 2018 [citado 2018 abr 16]. Disponível em: Disponível em: https://cidades.ibge.gov.br/brasil/rs/porto-alegre/panorama . [ Links ]
14. Secretaria Municipal de Saúde (Porto Alegre). Distâncias [Internet]. Porto Alegre: Secretaria Municipal de Saúde; 2018 [citado 2018 dez 03]. Disponível em: Disponível em: http://www2.portoalegre.rs.gov.br/turismo/default.php?p_secao=262 . [ Links ]
15. Secretaria Municipal de Saúde (Porto Alegre). Criação e história dos bairros. [Internet]. Porto Alegre: Secretaria Municipal de Saúde; 2018 [citado 2018 nov 20]. Disponível em: Disponível em: http://www2.portoalegre.rs.gov.br/spm/default.php?p_secao=294 . [ Links ]
16. Barcellos C, Santos SM. Colocando dados no mapa: a escolha da unidade espacial de agregação e integração de bases de dados em saúde e ambiente através do geoprocessamento. Inf Epidemiol Sus [Internet]. 1997 jan-mar [citado 2019 maio 17];6(1):21-29. Disponível em: Disponível em: http://scielo.iec.gov.br/pdf/iesus/v6n1/v6n1a03.pdf . doi: 10.5123/S0104-16731997000100003 [ Links ]
17. Acosta LMW, Bassanesi SL. The Porto Alegre paradox: social determinants and tuberculosis incidence. Rev Bras Epidemiol [Internet]. 2014 Dec [citado 2019 May 17];17(Suppl 2):88-101. Disponível em: Disponível em: http://www.scielo.br/pdf/rbepid/v17s2/1415-790X-rbepid-17-s2-00088.pdf . doi: 10.1590/1809-4503201400060008 [ Links ]
18. Ministério da Saúde (BR). Secretaria de Vigilância em Saúde. Fundação Instituto Oswaldo Cruz. Introdução à estatística espacial para a saúde pública [Internet]. Brasília: Ministério da Saúde; 2007 [citado 2019 maio 17]. 120 p. Disponível em: Disponível em: http://www.escoladesaude.pr.gov.br/arquivos/File/TEXTOS_CURSO_VIGILANCIA/capacitacao_e_atualizacao_em_geoprocessamento_em_saude_3.pdf [ Links ]
19. Prefeitura Municipal de Porto Alegre. Anuário estatístico - 2012. Porto Alegre: Prefeitura Municipal de Porto Alegre; 2013. 332 p. [ Links ]
20. Thiesen SV, Bello MIMR, Ávila RC. Dados epidemiológicos da leptospirose em Porto Alegre. Bol Epidemiol Porto Alegre [Internet]. 2003 maio [citado 2019 maio 17];5(19):7. Disponível em: Disponível em: http://lproweb.procempa.com.br/pmpa/prefpoa/cgvs/usu_doc/boletimepidemiologico-cgvs-sms-pmpa-19.pdf [ Links ]
21. Ministério da Saúde (BR). Secretaria de Vigilância em Saúde. Situação epidemiológica/Dados [Internet]. Brasília: Ministério da Saúde; 2018 [citado 2018 maio 10]. Disponível em: Disponível em: http://portalms.saude.gov.br/saude-de-a-z/leptospirose/9805-situacao-epidemiologica-dados [ Links ]
22. Costa E, Costa YA, Lopes AA, Sacramento E, Bina JC. Formas graves de leptospirose: aspectos clínicos, demográficos e ambientais. Rev Soc Bras Med Trop. 2001 maio-jun [citado 2019 maio 17];34(3):261-7. Disponível em: Disponível em: http://www.scielo.br/pdf/rsbmt/v34n3/4994.pdf . doi: 10.1590/S0037-86822001000300006 [ Links ]
23. Bello MIMR. Perfil epidemiológico da leptospirose em Porto Alegre, no período de 2007 a 2010 em Porto Alegre, RS, Brasil [trabalho de conclusão de curso]. Porto Alegre: Fundação Instituto Oswaldo Cruz; 2012. [ Links ]
24. Schneider MC, Jancloes M, Buss DF, Aldighieri S, Bertherat E, Najera P, et al. Leptospirosis: a silent epidemic disease. Int J Environ Res Public Health [Internet]. 2013 Dec [citado 2019 May 17];10(12):7229-34. Disponível em: Disponível em: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3881163/ . doi: 10.3390/ijerph10127229 [ Links ]
25. Rede Interagencial de Informação para a Saúde (RIPSA). Indicadores básicos para a saúde no Brasil: conceitos e aplicações [Internet]. 2. ed. Brasília: Organização Pan-Americana da Saúde; 2008 [Internet]. 349 p. Disponível em: http://tabnet.datasus.gov.br/tabdata/livroidb/2ed/indicadores.pdf [ Links ]
26. Acosta LMW, Bello MIMR, Ávila RC. Priorizando áreas para ações preventivas à leptospirose em Porto Alegre. Bol Epidemiol Porto Alegre [Internet]. 2002 maio [citado 2019 maio 17];5(15):2-3. Disponível em: Disponível em: http://lproweb.procempa.com.br/pmpa/prefpoa/cgvs/usu_doc/boletimepidemiologico-cgvs-sms-pmpa-15.pdf [ Links ]
27. Acosta LMW. A vigilância da Leptospirose em Porto Alegre no ano 2000. Bol Epidemiol Porto Alegre [Internet]. 2001 fev [citado 2019 maio 17];4(10):8. Disponível em: Disponível em: http://lproweb.procempa.com.br/pmpa/prefpoa/cgvs/usu_doc/boletimepidemiologico-cgvs-sms-pmpa-10.pdf [ Links ]
28. Acosta LMW. O que está sendo observado na vigilância da Leptospirose em 2001. Bol Epidemiol Porto Alegre [Internet]. 2001 maio [citado 2019 maio 17];4(11):5. Disponível em: Disponível em: http://lproweb.procempa.com.br/pmpa/prefpoa/cgvs/usu_doc/boletimepidemiologico-cgvs-sms-pmpa-11.pdf [ Links ]
29. Henkes WE. Ecologia de paisagem da leptospirose em Porto Alegre entre 2001 - 2006 [trabalho de conclusão de curso]. Porto Alegre: Universidade Federal do Rio Grande do Sul; 2008. Disponível em: https://www.lume.ufrgs.br/bitstream/handle/10183/15428/000678453.pdf?sequence=1 [ Links ]
30. Secretaria Municipal de Saúde (Porto Alegre). Ilhas do Delta do Jacuí [internet]. Porto Alegre: Secretaria Municipal de Saúde; 2018 [citado 2018 nov 22]. Disponível em: Disponível em: http://www2.portoalegre.rs.gov.br/spm/default.php?reg=16&p_secao=46 [ Links ]
Received: June 21, 2018; Accepted: April 23, 2019











 texto en
texto en