Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Epidemiologia e Serviços de Saúde
versão impressa ISSN 1679-4974versão On-line ISSN 2237-9622
Epidemiol. Serv. Saúde vol.29 no.2 Brasília 2020 Epub 29-Abr-2020
http://dx.doi.org/10.5123/s1679-49742020000200016
ORIGINAL ARTICLE
Prevalence and factors associated with maternal breastfeeding in the first hour of life in full-term live births in southwest Bahia, Brazil, 2017*
1Universidade Federal da Bahia, Instituto Multidisciplinar em Saúde, Vitória da Conquista, BA, Brazil
2Faculdade de Tecnologia e Ciências, Departamento de Nutrição, Jequié, BA, Brazil
3Universidade Federal de Pelotas, Departamento de Medicina Social, Pelotas, RS, Brazil
4Universidade Federal de Juiz de Fora, Departamento de Nutrição, Juiz de Fora, MG, Brazil
Objective:
to analyze prevalence and factors associated with maternal breastfeeding in the first hour of life (MBFFHL) in full-term live births in Vitória da Conquista, BA, Brazil.
Methods:
this was a cohort-nested cross-sectional study; data were collected between February and August 2017 using a questionnaire answered by mothers as well as medical records; hierarchical multivariable analysis with Poisson regression was used.
Results:
the study included 388 mother-liveborn baby pairs; MBFFHL prevalence was 49.5%; outcome was associated with maternal education ≥12 years (PR=0.63 - 95%CI 0.46;0.87), prenatal guidance on child holding and positioning (PR=1.44 - 95%CI 1.07;1.95), liveborn baby taken to its mother soon after delivery (PR=1.41 - 95%CI 1.04;1.92), mother and baby kept together in the same room (PR=2.42 - 95%CI 1.09;5.36), and delivery at a Baby-Friendly Hospital (PR=2.43 - 95%CI 1.72;3.43).
Keywords: Breast Feeding; Cross-Sectional Studies; Prenatal Care; Hospitals, Maternity; Hospital Care; Postpartum Period
Introduction
Maternal breastfeeding in the first hour of life (MBFFHL) is a practice recommended in the ‘fourth step for successful maternal breastfeeding set by the Baby-Friendly Hospital Initiative (BFHI)’, which refers to promoting immediate and uninterrupted skin-to-skin contact between mother and baby, as well as helping mothers to initiate breastfeeding as early as possible following birth.1
Immediately after delivery, the newborn baby is alert and ready to begin breastfeeding as it is capable of moving itself to the breast/nipple region and sucking within the first 60 minutes of life.2 Following this period, many babies enter the sleeping stage,3 which hinders breastfeeding and increases the likelihood of food compliments being prescribed.4
MBFFHL is associated with longer duration of breastfeeding5 and with reduction in neonatal mortality.6 The benefits of starting breastfeeding early are related both to the components of breast milk and also to the contact between mother and baby. MBFFHL favors receipt of colostrum, which contains bioactive immunological factors intended to provide the baby with immunological protection, preventing its intestines from being colonized by pathogenic microorganisms.7 ‘Skin-to-skin’ contact between mother and baby shortly after childbirth contributes to the baby’s skin being colonized by its mother’s microbiota, as well as contributing to cardiorespiratory and body temperature stabilization.8 Furthermore, placing the baby on the breast soon after birth minimizes separation, favors the establishment of a bond of affection between mother and child, potentializes release of oxytocin and the baby learns to suckle more efficiently, thus satisfying it and making it want to suckle again.9
According to data from national surveys carried out in 153 high and middle to low-income countries in 2010, only half the babies there were breastfed during the first hour of life.10 In Brazil, data from the 2006 National Demography and Health Survey revealed that 42.9% of babies were breastfed during the first hour of life.11 The results of the II Maternal Breastfeeding Prevalence Survey in 2008, showed a significant increase in MBFFHL prevalence (67.7%).12
The literature points to diverse factors influencing time to first breastfeeding, some of which are risk factors for not breastfeeding in the first hour of life: maternal age below 25 years; low maternal schooling; cesarean section; gestational age under 37 weeks.13 Inadequate obstetric care and mother and baby not being kept together in the same room following childbirth also interfere negatively with MBFFHL.14
In Brazil, particularly in the Northeast region, literature about MBFFHL prevalence and associated factors is still scarce.13-15 Identifying factors that influence the practice of MBFFHL is of fundamental importance for informing the definition of strategies for formulating and implementing Public Health policies aimed at encouraging maternal breastfeeding being started early. Within this context, this study aims to analyze MBFFHL prevalence and associated factors in Vitória da Conquista, Bahia, Brazil.
Methods
An analytical cross-sectional study was conducted, nested within a cohort entitled ‘Accompaniment of maternal breastfeeding and complementary feeding of children aged under 1 year old’, comprised of mothers resident in the municipality of Vitória da Conquista, in Southwest Bahia. Data was collected for the cohort from all the municipality’s maternity hospitals; subsequent follow-up occurred by means of household visits when babies were 30 days, 6 months and 12 months old. This article presents information relating to the cohort baseline (data collected at maternity hospitals).
According to Brazilian Institute of Geography and Statistics (IBGE) data for the year 2019, Vitória da Conquista is the third largest city in the state of Bahia and the fourth largest in the interior of the Northeast region, with a population of 341,597 inhabitants, 89.5% of whom live in the city’s urban area. In 2010, the city had a Municipal Human Development Index (HDI-M) of 0.678, as well as being a health service referral center for around 80 municipalities in Bahia state and 16 in the north of Minas Gerais state.16
The population studied was comprised of puerperal woman and liveborn babies hospitalized in the postpartum period in all of the municipality’s maternity hospitals. Vitória da Conquista has four maternity hospitals: one public; one private; and two that provide services to both National Health System (SUS) patients and to private system patients. Of the four maternity hospitals, only the public one has been accredited and received the seal of the Baby-Friendly Hospital Initiative.
Mothers residents in Vitória da Conquista, with healthy liveborn babies, that were not twins and with gestational age equal to or greater than 37 weeks were eligible for the cohort study. The exclusion criteria were: (i) children born with malformations hindering breastfeeding; (ii) mothers with the human immunodeficiency virus (HIV); and (iii) mothers resident in the rural area of Vitória da Conquista, because of the logistic limitations for following up on the participants in the next stages of the study.
The study sample was comprised of puerperal women and newborn babies assessed at the cohort study baseline. In order to calculate the size of this sample, we took the number of live births in 2016 in Vitória da Conquista (n=5,541) and 58% prevalence of breastfeeding in the first hour of life in Vitória da Conquista,17 with 5% precision and a 95% confidence interval (95%CI). This resulted in a minimum sample size of 351 mother-baby pairs. In this study, the power of the sample was calculated a posteriori, taking a 95%CI; the power of the explanatory variables studied varied between 76.5 and 100%.
The data were collected between February and August 2017, by researchers trained beforehand in administering the questionnaire and gathering information from medical records. Mothers who had had babies during the 24 hours prior to the day on which data were collected were identified at the maternity hospitals and their medical records were assessed in relation to the eligibility criteria. Mothers and newborn babies who met the criteria for participation in the study were selected at random in order to chose three pairs of mothers/liveborn babies each day; if there were only three pairs or fewer who met the inclusion criteria, all of them were invited to take part. The selection criterion of three pairs a day from each maternity hospital was established in order to make follow-up feasible. The researchers visited puerperal women eligible for the study at their hospital beds. The questionnaire they were invited to answer was comprised of questions about sociodemographic, prenatal and childbirth conditions as well as conditions relating to breastfeeding.
The outcome variable was MBFFHL and this information was requested of mothers by asking the following question:
“Did your baby breastfeed in the first hour of life after it was born?”
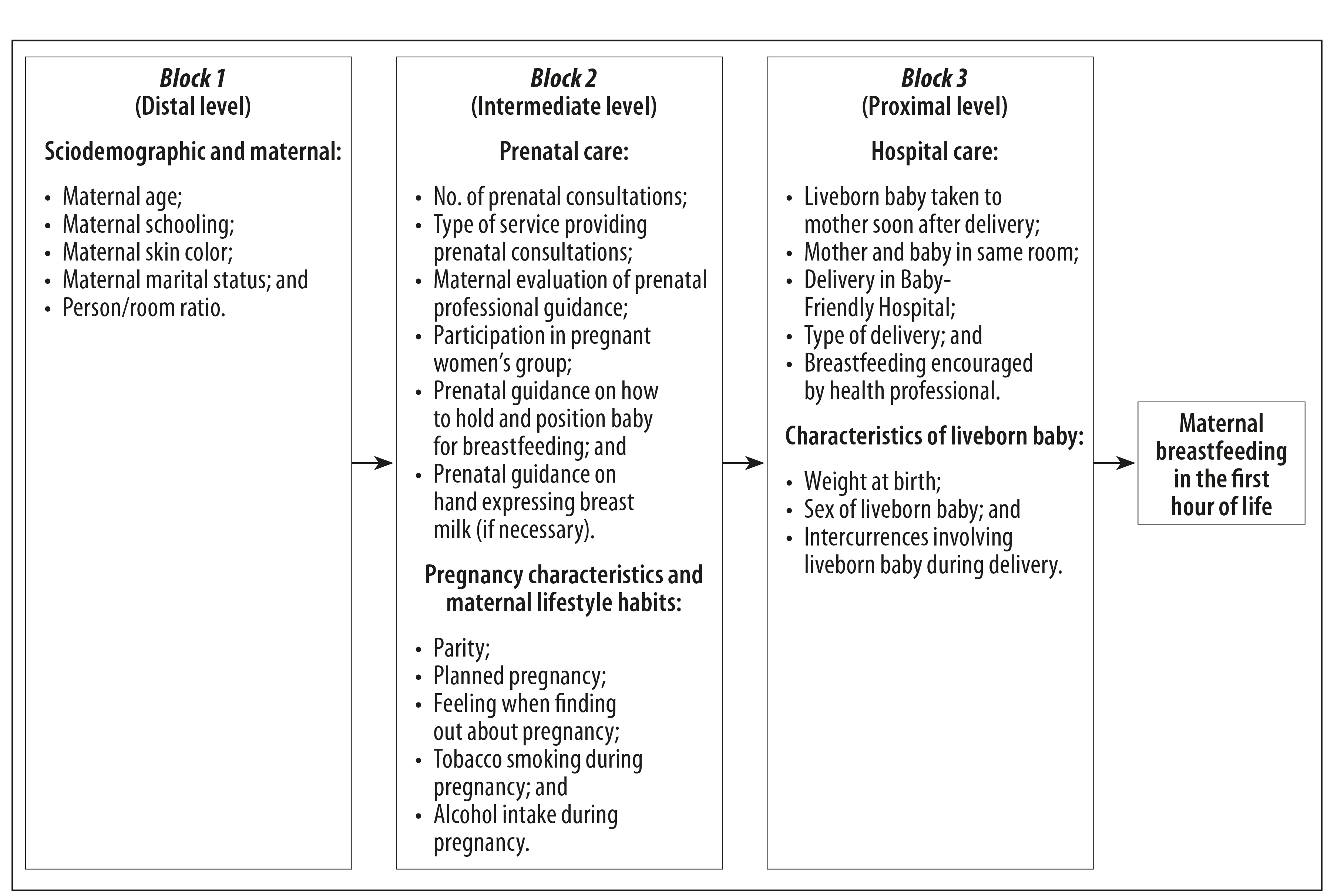
The independent variables were grouped into three blocks, according to the hierarchical conceptual model adapted from Boccolini et al.18 (Figure 1), and categorized as described below.
Block 1 (distal level) comprised the sociodemographic and maternal variables:
maternal age (in years: <20; 20-34; ≥35);
maternal schooling (in years of study: 0-4; 5-8; 9-11; ≥12 years);
maternal race/skin color (white/yellow; black; brown);
maternal marital status (no partner; has a partner); and
person/room ratio (<1; ≥1).
Block 2 (intermediate level) was comprised of variables regarding prenatal care, pregnancy characteristics and maternal lifestyle habits:
number of prenatal consultations (≥6; <6);
type of service where prenatal consultations took place (public; private);
maternal evaluation of professional guidance given during prenatal care (dissatisfactory; satisfactory);
participation in pregnant women’s groups (no; yes);
prenatal guidance on how to hold and position the baby for breastfeeding (no; yes);
prenatal guidance on hand expressing breast milk (if necessary) (no; yes);
parity (primipara; multipara);
planned pregnancy (no; yes);
satisfaction with finding out about pregnancy (dissatisfied; satisfied);
tobacco smoking during pregnancy (no; yes); and
alcohol intake during pregnancy (no; yes).
Block 3 (proximal level), comprising variables relating to hospital care and characteristics of the newborn baby:
liveborn baby taken to its mother soon after delivery (no; yes);
mother and baby kept together in the same room (no; yes);
child delivery at a Baby-Friendly Hospital (no; yes);
type of delivery (vaginal; cesarean);
breastfeeding encouraged, by health professionals (no; yes);
weight at birth (in grams: ≥2,500; <2,500);
sex of liveborn baby (female; male); and
intercurrences involving liveborn baby during delivery (no; yes).
The statistical analyses were performed with the aid of Stata version 13.0 (StataCorp, College Station, Texas, USA). In order to characterize the study population, the categorical variables were described using absolute and relative frequencies, while the quantitative variables were described by measures of central tendency and dispersion. Pearson’s chi-square test with a 5% significance level was used to check for differences in MBFFHL proportions in relation to the study’s independent variables, as well as the difference in MBFFHL prevalence between the municipality’s maternity hospitals.
Analysis of factors associated with MBFFHL was performed using Poisson regression with robust variance. Firstly crude analysis was performed estimating crude prevalence ratios and respective 95%CI. Variables with a p-value of less than 0.20 were included in the multivariable analysis, in a hierarchical manner, according to the conceptual model levels.
The distal level variables were included in the first stage of the multivariable analysis (model 1). The intermediate level variables were included in the second stage, adjusted by the significant variables (p≤0.05) of the distal level (model 2). The proximal level variables were included in the third stage, adjusted by the significant variables (p≤0.05) from the previous levels (model 3). Variables having p≤0.05 in each regression model were considered to be significantly associated with MBFFHL. The Akaike criterion was adopted for comparison between models. Maternity hospital type was not included in the adjusted analysis, because of collinearity with the ‘Baby-Friendly Hospital’ variable.
The research project was submitted to and approved by the Human Research Ethics Committee of the Multidisciplinary Health Institute, Federal University of Bahia (CEP-Seres Humanos/IMS/UFBa): Protocol No. 1.861.163, issued on December 12th 2016. The study was conducted in accordance with the ethical standards established by the 1964 Declaration of Helsinki and its subsequent alterations. Even before approval by CEP-Seres Humanos/IMS/UFBa, all the maternity hospitals were informed of the objective of the study and signed an official letter consenting to data collection. All participants who agreed to take part in the study signed a Free and Informed Consent form as a condition for being interviewed.
Results
Out of a total of 421 puerperal women invited to take part in the study, 388 were interviewed. Refusals accounted for 7.8%. The mothers’ mean age was 27.7 years (standard deviation [SD] = 6.5), varying between 14 and 44 years. The majority of these women lived with a steady partner (78.3%), 58.5% stated that their skin color was brown and 46.7% had between 9 and 11 years of schooling (Table 1).
Table 1 - Prevalence and crude prevalence ratio of maternal breastfeeding in the first hour of life, according to sociodemographic and maternal characteristics (n=388), Vitória da Conquista, Bahia, 2017
| Variable | n (%)a | Prevalence of MBFFHL (%)b | PR (crude)c | 95%CId | p-valuee |
|---|---|---|---|---|---|
| Maternal age (in years) | 0.997 | ||||
| <20 | 44 (11.3) | 50.0 | 1.00 | ||
| 20-34 | 275 (70.9) | 49.5 | 0.99 | 0.72;1.36 | |
| ≥35 | 69 (17.7) | 49.3 | 0.99 | 0.67;1.44 | |
| Maternal schooling (in years of study) | 0.034 | ||||
| 0-4 | 47 (12.1) | 63.8 | 1.00 | ||
| 5-8 | 56 (14.4) | 55.4 | 0.87 | 0.63;1.19 | |
| 9-11 | 181 (46.7) | 49.2 | 0.77 | 0.59;1.00 | |
| ≥12 | 104 (26.8) | 40.4 | 0.63 | 0.46;0.87 | |
| Maternal race/skin color | 0.297 | ||||
| White/yellow | 93 (24) | 49.5 | 1.00 | ||
| Black | 68 (17.5) | 57.4 | 1.16 | 0.87;1.55 | |
| Brown | 227 (58.5) | 47.1 | 0.95 | 0.74;1.22 | |
| Maternal marital status | 0.890 | ||||
| No partner | 84 (21.7) | 48.8 | 1.00 | ||
| Has a partner | 304 (78.3) | 49.7 | 1.02 | 0.80;1.30 | |
| Person/room ratio | 0.008f | ||||
| <1 | 323 (83.3) | 46.8 | 1.00 | ||
| ≥1 | 65 (16.8) | 63.1 | 1.35 | 1.08;1.68 | |
a) Sample description: n = absolute value; % = frequency.
b) MBFFHL: maternal breastfeeding in the first hour of life.
c) PR: prevalence ratio.
d) 95%CI: 95% confidence interval.
e) Poisson regression with robust variance estimator.
f) p<0.01.
In relation to characteristics of prenatal care, pregnancy and maternal lifestyle habits, the majority of the mothers were found to have had six or more prenatal consultations (80.2%), 47.7% were primipara and 4.6% reported having smoked during pregnancy (Table 2).
Table 2 - Prevalence and crude prevalence ratio of maternal breastfeeding in the first hour of life, according to characteristics of prenatal care, pregnancy and maternal lifestyle habits (n=388), Vitória da Conquista, Bahia, 2017
| Variable | n (%)a | Prevalence of MBFFHL (%)b | PR(crude)c | 95%CId | p-valuee |
|---|---|---|---|---|---|
| Number of prenatal consultations | 0.031 | ||||
| ≥6 | 311 (80.2) | 47.0 | 1.00 | ||
| <6 | 77 (19.8) | 59.7 | 1.27 | 1.02;1.58 | |
| Type of service providing prenatal consultations | 0.007f | ||||
| Public | 268 (69.4) | 54.1 | 1.00 | ||
| Private | 118 (30.6) | 38.1 | 0.70 | 0.55;0.91 | |
| Maternal evaluation of health professional guidance given during prenatal care | 0.045g | ||||
| Dissatisfactory | 52 (13.5) | 34.6 | 1.00 | ||
| Satisfactory | 334 (86.5) | 51.5 | 1.49 | 1.01;2.19 | |
| Participation in pregnant women’s group | 0.115 | ||||
| No | 281 (72.6) | 47.0 | 1.00 | ||
| Yes | 106 (27.4) | 55.7 | 1.18 | 0.96;1.46 | |
| Prenatal guidance on how to hold and position the baby for breastfeeding | 0.009f | ||||
| No | 82 (30.6) | 39,0 | 1.00 | ||
| Yes | 186 (69.4) | 58.1 | 1.49 | 1.11;2.00 | |
| Prenatal guidance on hand expressing breast milk (if necessary) | 0.020g | ||||
| No | 163 (60.8) | 46.6 | 1.00 | ||
| Yes | 105 (39.2) | 61.0 | 1.31 | 1.04;1.64 | |
| Parity | 0.021g | ||||
| Primipara | 185 (47.7) | 43.2 | 1.00 | ||
| Multipara | 203 (52.3) | 55.2 | 1.28 | 1.04;1.57 | |
| Planned pregnancy | 0.663 | ||||
| No | 220 (56.7) | 50.5 | 1.00 | ||
| Yes | 168 (43.3) | 48.2 | 0.96 | 0.78;1.17 | |
| Feeling when finding out about pregnancy | 0.463 | ||||
| Dissatisfied | 55 (14.8) | 54.6 | 1.00 | ||
| Satisfied | 318 (85.2) | 49.4 | 0.91 | 0.69;1.18 | |
| Tobacco smoking during pregnancy | 0.072 | ||||
| No | 370 (95.4) | 48.7 | 1.00 | ||
| Yes | 18 (4.6) | 66.7 | 1.37 | 0.97;1.93 | |
| Alcohol intake during pregnancy | 0.169 | ||||
| No | 360 (92.8) | 48.6 | 1.00 | ||
| Yes | 28 (7.2) | 60.7 | 1.25 | 0.91;1.71 | |
a) Sample description: n = absolute value; % = frequency.
b) MBFFHL: maternal breastfeeding in the first hour of life.
c) PR: prevalence ratio.
d) 95%CI: 95% confidence interval.
e) Poisson regression with robust variance estimator.
f) p<0.01.
g) p<0.05.
With regard to hospital care and liveborn baby characteristics, 50.5% of deliveries occurred in the Baby-Friendly Hospital, 53.1% of live births were male and 4.6% were born with low weight (Table 3).
Table 3 - Prevalence and crude prevalence ratio of maternal breastfeeding in the first hour of life, according to hospital care and liveborn infant characteristics (n=388), Vitória da Conquista, Bahia, 2017
| Variable | n (%)a | Prevalence of MBFFHL (%)b | PR(crude)c | 95%CId | p-valuee |
|---|---|---|---|---|---|
| Liveborn baby taken to its mother soon after delivery | <0.001f | ||||
| No | 141 (36.3) | 28.4 | 1 | ||
| Yes | 247 (63.7) | 61.5 | 2.17 | 1.64;2.87 | |
| Mother and baby kept in the same room | <0.001f | ||||
| No | 66 (17) | 12.1 | 1 | ||
| Yes | 322 (83) | 57.1 | 4.71 | 2.44;9.10 | |
| Child delivery at a Baby-Friendly Hospital | <0.001f | ||||
| No | 192 (49.5) | 22.9 | 1 | ||
| Yes | 196 (50.5) | 75.5 | 3.29 | 2.51;4.32 | |
| Type of delivery | <0.001f | ||||
| Vaginal | 181 (46.7) | 60.2 | 1 | ||
| Cesarean | 207 (53.3) | 40.1 | 0.67 | 0.54;0.82 | |
| Breastfeeding encouraged, by health professionals | 0.055 | ||||
| No | 53 (13.7) | 35.9 | 1 | ||
| Yes | 334 (86.3) | 51.8 | 1.44 | 0.99;2.10 | |
| Weight at birth (in grams) | 0.072 | ||||
| ≥2,500 | 370 (95.4) | 48.7 | 1 | ||
| <2,500 | 18 (4.6) | 66.7 | 1.37 | 0.97;1.93 | |
| Sex of liveborn baby | 0.411 | ||||
| Female | 182 (46.9) | 47.3 | 1 | ||
| Male | 206 (53.1) | 51.5 | 1.09 | 0.89;1.33 | |
| Intercurrences involving liveborn baby during delivery | 0.635 | ||||
| No | 374 (96.4) | 49.7 | 1 | ||
| Yes | 14 (3.6) | 42.9 | 0.86 | 0.47;1.59 | |
a) Sample description: n = absolute value; % = frequency.
b) MBFFHL: maternal breastfeeding in the first hour of life.
c) PR: prevalence ratio.
d) 95%CI: 95% confidence interval.
e) Poisson regression with robust variance estimator.
f) p<0.01.
MBFFHL prevalence in the total sample was 49.5% (95%CI 44.5;54.5%). A discrepancy was found between the maternity hospitals with regard to the practice of MBFFHL, varying between 14.3 and 75.5% (p<0.001). MBFFHL was most prevalent at the (public) Baby-Friendly Hospital: 75.5% (95%CI 68.9;81.1%). At the private maternity hospital, MBFFHL prevalence was 36.2% (95%CI 24.6;49.6%), while at the other two hospitals, which provide both public and private services, prevalence was 14.3% (95%CI 6.8;27.6%) and 18.8% (95%CI 11.7;28.8%). No statistically significant difference was found in MBFFHL prevalence rates at the two hospitals that provide both public and private services (data not shown).
Based on the results of the crude analysis, only the ‘maternal schooling’ and ‘person/room ratio’ variables from block 1 were included in the multiple analysis (Table 1). Nearly all the block 2 variables were included in the multivariable analysis, with the exception of ‘planned pregnancy’ and ‘feeling when finding out about pregnancy’ (Table 2). As for the block 3 variables, the following were included in the multiple model: liveborn baby taken to its mother soon after delivery; mother and baby in the same room; delivery in a Baby-Friendly Hospital; type of delivery; encouragement of breastfeeding, by health professionals; and weight at birth (Table 3).
In the multivariable analysis (Table 4), MBFFHL was found to be associated with: maternal schooling, with lower MBFFHL prevalence among babies of mothers with 12 or more years of study (PR=0.63 - 95%CI 0.46;0.87), compared to the babies of mothers with between 0 and 4 years of schooling; receipt of prenatal guidance on how to hold and position the baby for breastfeeding (PR=1.44 - 95%CI 1.07;1.95); liveborn baby taken to its mother soon after delivery (PR=1.41 - 95%CI 1.04;1.92); mother and baby in the same room (PR=2.42 - 95%CI 1.09;5.36); and child delivery in a Baby-Friendly Hospital (PR=2.43 - 95%CI 1.72;3.43).
Table 4 - Multivariable analysis of factors associated with maternal breastfeeding in the first hour of life (n=388), Vitória da Conquista, Bahia, 2017
| Block/variable | Model 1 | Model 2 | Model 3 | |||
|---|---|---|---|---|---|---|
| PRa | 95%CIb | PRa | 95%CIb | RPa | IC95% b | |
| Block 1 | ||||||
| Maternal schooling (in years of study) | ||||||
| 0-4 | 1.00 | |||||
| 5-8 | 0.87 | 0.63;1.19 | ||||
| 9-11 | 0.77 | 0.59;1.00 | ||||
| ≥12 | 0.63 | 0.46;0.87c | ||||
| Block 2 | ||||||
| Prenatal guidance on how to hold and position the baby for breastfeeding | ||||||
| No | 1.00 | |||||
| Yes | 1.44 | 1.07;1.95c | ||||
| Block 3 | ||||||
| Liveborn baby taken to its mother soon after delivery | ||||||
| No | 1.00 | |||||
| Yes | 1.41 | 1.04;1.92c | ||||
| Mother and baby in the same room | ||||||
| No | 1.00 | |||||
| Yes | 2.42 | 1.09;5.36c | ||||
| Child delivery at a Baby-Friendly Hospital | ||||||
| No | 1.00 | |||||
| Yes | 2.43 | 1.72;3.43c | ||||
| Comparison using Akaike criterion | 658.12 | 466.66 | 427.16 | |||
a) PR: prevalence ratio.
b) 95%CI: 95% confidence interval.
c) p<0.05.
Note:
Model 1: adjusted by sociodemographic and maternal variables (block 1).
Model 2: adjusted by block 1 variables and by variables related to prenatal care, pregnancy characteristics and maternal lifestyle habits (block 2).
Model 3: adjusted by block 1 and block 2 variables and variables related to hospital care and liveborn baby characteristics (block 3).
Discussion
Practically half the infants in the sample were breastfed in the first hour of life. This outcome was significantly associated with maternal schooling ≥12 years, receipt of prenatal guidance on how to hold and position the baby for breastfeeding, liveborn baby taken to its mother soon after delivery, mother and baby in the same room and child delivery in a Baby-Friendly Hospital.
This study found MBFFHL prevalence in Vitória da Conquista similar to prevalence estimated in high and middle to low-income countries in 2010 (50%).10 However, the prevalence rate we found was lower than both the national prevalence rate (67.7%) and the Northeast region prevalence rate (66.9%); as well as being lower than that of the municipality itself (58%) as found by the II Maternal Breastfeeding Prevalence Survey in 2008.12,16 However, it is important to highlight that in this study information about MBFFHL was collected directly from mothers in the first 24 hours after childbirth, whereas the Ministry of Health survey gathered information about the time maternal breastfeeding started through interviews with mothers of infants under 1 year old, 71.3% of whom were more than 3 months old.12 This implies the possibility of memory bias, possibly capable of overestimating MBFFHL prevalence.
The World Health Organization (WHO)19 classifies as ‘reasonable’ MBFFHL prevalence in the range of 50 to 89%, this being the reason why the entire population of this study was classified in this category; although when they were stratified according to the maternity hospitals studied, the classifications were found to be different. The prevalence found at the Baby-Friendly Hospital was classified as ‘good’ (prevalence of between 50 and 89%), whereas for the exclusively private maternity hospital and the maternity hospitals providing public and private services, MBFFHL prevalence rates were classified as ‘reasonable’ (30 to 49%) and ‘poor’ (0 to 29%), respectively. As such, it can be seen that the differences between the maternal breastfeeding programs adopted by these institutions were reflected in differences in MBFFHL prevalence.
With regard to the determinants of MBFFHL, the results of this study showed that a higher level of maternal schooling was associated with lower MBFFHL prevalence, contrary to several international studies that point to maternal schooling as being a protection factor against non-MBFFHL.13 On the other hand, the study conducted by Silveira, Albernaz & Zuccheto,20 involving a sample of 2,741 mothers/liveborn babies in the city of Pelotas, RS, in 2002/2003, found that the greater maternal schooling, the greater the relative risk of not breastfeeding in the first hour of life.
It is possible that the association found between maternal schooling and MBFFHL is the result of using a hierarchical analysis model in this study, whereby the effects of schooling were adjusted by the variables on the same level and not by variables related to hospital care, considered to be more proximal to the outcome. When analyzing the relationship between maternal schooling and child delivery at the Baby-Friendly Hospital, lower child delivery frequency was found at this hospital among mothers with more schooling (p<0.001) (data not shown). As such, the lower proportion of deliveries at the Baby-Friendly Hospital among mothers with more schooling could explain, at least in part, lower MBFFHL prevalence among women with more schooling.
With regard to the variables related to prenatal care, receipt of guidance on how to hold and position the baby for breastfeeding was found to be positively associated with MBFFHL. During the period around childbirth, women, especially primipara women, are seen to be more insecure, meaning that they have not yet gained certain abilities, such as knowledge, practice and posture necessary for the act of breastfeeding, reinforcing the idea that this practice is not instinctive but rather learned.21 Prior knowledge on how to hold and position the baby for breastfeeding may favor starting maternal breastfeeding early.
In this study, two important actions in the postpartum period were found to be associated with greater MBFFHL prevalence: the liveborn baby having been taken to its mother soon after birth; and mother and baby being in the same room after delivery.
The fact of taking the liveborn baby to its mother following childbirth and the impact of this on MBFFHL prevalence was also found in the study conducted by Boccolini et al. between 1999 and 2001,18 with a representative sample of 8,397 parturient women in maternity hospitals in Rio de Janeiro, RJ: MBFFHL prevalence was 38% lower among liveborn babies who were not taken to their mothers as soon as they were born.
It is noteworthy that hospital routines are determinants for maternal breastfeeding being started and, in this setting, health professionals are the protagonists of health care and it is their responsibility to carry out actions aimed at maternal care that favor the timely start of breastfeeding.22
As in this study, the importance for MBFFHL of mother and baby being in the same room was also shown by Sá et al.,14 in a study conducted with 1,027 mothers and infants under 1 year old who took part in the second stage of a poliomyelitis vaccination campaign in the Federal District in 2011. They found MBFFHL prevalence 72% lower among women who were not kept in the same room as their babies in the postpartum period.
Studies have pointed to the beneficial influence of being in the same room on maternal breastfeeding, providing the mother with greater security regarding holding and positioning the baby for breastfeeding, as well as being a space for greater interaction between puerperal women and health professionals. The latter can make use of this environment to approach issues fundamental to greater efficacy of breastfeeding.23,24
Childbirth in a hospital accredited by the Baby-Friendly Hospital Initiative - (BFHI) - was associated with greater MBFFHL prevalence, corroborating results of previous studies.15,20 Ever since BFHI was launched in 1991, it has served as a motivating force for maternity hospitals worldwide to implement policies and practices in support of breastfeeding.1 BFHI has been responsible for significant improvements in the rates of starting breastfeeding and its duration, whereby the positive repercussion of implementing the initiative has been confirmed by studies conducted in several different countries, regardless of the cultural contexts there.25-27
This study has some limitations that need to be considered. Owing to the fact of it not having originally been designed to assess MBFFHL, some information relating to this practice, which could have enriched the analysis and discussion of the theme, was not gathered: whether breastfeeding took place in the delivery room, which health professional took the baby to the mother’s breast, characteristics of holding and positioning the baby for breastfeeding, among others. Moreover, the possibility cannot be ruled out of imprecision and potential error in classifying the information about how much time elapsed before first breastfeeding, given that this data was estimated by the mothers. On the other hand, this problem was minimized by conducting the interviews at the maternity hospitals within the first 24 hours following childbirth.
The longitudinal design of the study from which this report originated enables further studies to be carried out in order to assess the impact of MBFFHL on other mother and child health outcomes, thus collaborating with the advancement of scientific literature on the subject.
Breastfeeding prevalence in the first hour of life, in the municipality of Vitória da Conquista, BA, was classified as ‘good’, according to WHO definitions, and MBFFHL was associated with maternal factors, prenatal care and hospital care.
In conclusion, this evidence suggests that MBFFHL prevalence is influenced by institutional policies, as well as by procedures adopted by health professionals in the prenatal and postpartum periods. Implementation of prenatal care and hospital routines that favor the early starting of maternal breastfeeding reveal themselves to be fundamental to the extent that they can impact directly on this outcome. Similarly, the need stands out for the Baby-Friendly Hospital Initiative to be scaled up, in view of just how strongly the practices adopted by institutions accredited by this initiative contribute to promoting maternal breastfeeding in the first hour of life.
REFERENCES
1. World Health Organization. United Nations Children's Fund. Implementation guidance: protecting, promoting and supporting breastfeeding in facilities providing maternity and newborn services - the revised Baby-friendly Hospital Initiative [Intermet]. Geneva: WHO/UNICEF; 2018 [cited 2020 Mar 9]. 47 p. Available from: Available from: https://www.who.int/nutrition/publications/infantfeeding/bfhi-implementation/en/ [ Links ]
2. Righard L, Alade MO. Effect of delivery room routines on success of first breast- feed. Lancet [Internet[. 1990 Nov [cited 2020 Mar 9];336(8723):1105-7. Available from: Available from: https://doi.org/10.1016/0140-6736(90)92579-7 [ Links ]
3. Widström AM, Lilja G, Aaltomaa-Michalias P, Dahllöf A, Lintula M, Nissen E. Newborn behaviour to locate the breast when skin-to-skin: a possible method forenabling early self-regulation. Acta Paediatr [Internet]. 2011 Jan [cited 2020 Mar 9];100(1):79-85. Available from: Available from: https://doi.org/10.1111/j.1651-2227.2010.01983.x [ Links ]
4. Lopes FO, Oliveira MIC, Brito AS, Fonseca VM. Fatores associados ao uso de suplementos em recém-natos em alojamento conjunto no Município do Rio de Janeiro. Ciênc Saúde Coletiva [Internet]. 2013 fev [citado 2020 mar 9];18(2):431-9. Disponível em: Disponível em: https://doi.org/10.1590/S1413-81232013000200014 [ Links ]
5. Murray EK, Ricketts S, Dellaport J. Hospital practices that increase breastfeeding duration: results from a population-based study. Birth [Internet]. 2007 Sep [cited 2020 Mar 6];34(3):202-11. Available from: Available from: https://doi.org/10.1111/j.1523-536X.2007.00172.x [ Links ]
6. Khan J, Vesel L, Bahl R, Martines JC. Timing of breastfeeding initiation and exclusivity of breastfeeding during the first month of life: effects on neonatal mortality and morbidity - a systematic review and meta-analysis. Matern Child Health J [Internet]. 2015 Mar [cited 2020 Mar 6];19(3):468-79. Available from: Available from: https://doi.org/10.1007/s10995-014-1526-8 [ Links ]
7. Chirico G, Marzollo R, Cortinovis S, Fonte C, Gasparoni A. Antiinfective properties of human milk. J Nutr [Internet]. 2008 Sep [cited 2020 Mar 6];138(9):1801S-6S. Available from: Available from: https://doi.org/10.1093/jn/138.9.1801S [ Links ]
8. Moore ER, Bergman N, Anderson GC, Medley N. Early skin-to-skin contact for mothers and their healthy newborn infants. Cochrane Database Syst Rev [Internet]. 2016 May [cited 2020 Mar 6];CD003519. Available from: Available from: https://doi.org/10.1002/14651858.CD003519.pub3 [ Links ]
9. Galvão DMPG. Promoção da amamentação na primeira hora após o parto. Rev Nursing. 2009;242:07-12. [ Links ]
10. Victora CG, Bahl R, Barros AJ, França GV, Horton S, Krasevec J, et al. Breastfeeding in the 21st century: epidemiology, mechanisms, and lifelong effect. Lancet [Internet]. 2016 [cited 2020 Mar 6];387(10017):475-90. Available from: Available from: https://doi.org/10.1016/S0140-6736(15)01024-7 [ Links ]
11. Ministério da Saúde (BR). Pesquisa nacional de demografia e saúde da criança e da mulher - PNDS 2006: dimensões do processo reprodutivo e da saúde da criança [Internet]. Brasília: Ministério da Saúde; 2009 [citado 2020 mar 6]. 300 p. Disponível em: Disponível em: http://bvsms.saude.gov.br/bvs/publicacoes/pnds_crianca_mulher.pdf [ Links ]
12. Ministério da Saúde (BR). Secretaria de Atenção à Saúde. II Pesquisa de prevalência de aleitamento materno nas capitais brasileiras e Distrito Federal [Internet]. Brasília: Ministério da Saúde; 2009 [citado 2020 mar 6]. 108 p. Disponível em: Disponível em: http://bvsms.saude.gov.br/bvs/publicacoes/pesquisa_prevalencia_aleitamento_materno.pdf [ Links ]
13. Esteves TMB, Daumas RP, Oliveira MIC, Andrade CADF, Leite IC. Fatores associados à amamentação na primeira hora de vida: revisão sistemática. Rev Saúde Pública [Internet]. 2014 ago [citado 2020 mar 6];48(4):697-708. Disponível em: Disponível em: https://doi.org/10.1590/S0034-8910.2014048005278 [ Links ]
14. Bandeira de Sá NN, Gubert MB, Santos WD, Santos LMP. Fatores ligados aos serviços de saúde determinam o aleitamento materno na primeira hora de vida no Distrito Federal, Brasil, 2011. Rev Bras Epidemiol [Internet]. 2016 set [citado 2020 mar 6];19(3):509-24. Disponível em: Disponível em: https://doi.org/10.1590/1980-5497201600030004 [ Links ]
15. Esteves TMB, Daumas RP, Oliveira MIC, Andrade CAF, Leite IC. Fatores associados ao início tardio da amamentação em hospitais do Sistema Único de Saúde no Município do Rio de Janeiro, Brasil, 2009. Cad Saúde Pública [Internet]. 2015 nov [citado 2020 mar 6];31(11):2390-400. Disponível em: Disponível em: https://doi.org/10.1590/0102-311X00123114 [ Links ]
16. Instituto Brasileiro de Geografia e Estatística. Cidades e Estados [Internet]. Rio de Janeiro: Instituto Brasileiro de Geografia e Estatística; 2019 [citado 2019 out 24]. Disponível em: Disponível em: https://www.ibge.gov.br/cidades-e-estados/ba/vitoria-da-conquista.html [ Links ]
17. Ministério da Saúde (BR). Secretaria de Atenção à Saúde. Pesquisa de prevalência de aleitamento materno em municípios brasileiros [Internet]. Brasília: Ministério da Saúde; 2010 [citado 2020 mar 6]. 63 p. Disponível em: Disponível em: http://www.redeblh.fiocruz.br/media/pamuni.pdf [ Links ]
18. Boccolini CS, Carvalho ML, Oliveira MIC, Vasconcellos AGG. Fatores associados à amamentação na primeira hora de vida. Rev Saúde Pública [Internet]. 2011 nov [citado 2020 mar 6];45(1):69-78. Disponível em: Disponível em: https://doi.org/10.1590/S0034-89102010005000051 [ Links ]
19. Ministério da Saúde (BR). Secretaria de Atenção à Saúde. Saúde da criança: aleitamento materno e alimentação complementar [Internet]. 2. ed. Brasília: Ministério da Saúde; 2015 [citado 2020 mar 6]. 181 p. (Cadernos de Atenção Básica ; n. 23). Disponível em: Disponível em: http://189.28.128.100/dab/docs/portaldab/publicacoes/saude_crianca_aleitamento_materno_cab23.pdf [ Links ]
20. Silveira RB, Albernaz E, Zuccheto LM. Fatores associados ao início da amamentação em uma cidade do sul do Brasil. Rev Bras Saúde Matern Infant [Internet]. 2008 mar [citado 2020 mar 6];8(1):35-43. Disponível em: Disponível em: https://doi.org/10.1590/S1519-38292008000100005 [ Links ]
21. Monteiro JCS, Gomes FA, Nakano MAS. Percepção das mulheres acerca do contato precoce e da amamentação em sala de parto. Acta Paul Enferm [Internet]. 2006 dez [citado 2020 mar 6];19(4):427-32. Disponível em: Disponível em: https://doi.org/10.1590/S0103-21002006000400010 [ Links ]
22. Sampaio ARR, Bousquat A, Barros C. Contato pele a pele ao nascer: um desafio para a promoção do aleitamento materno em maternidade pública no Nordeste brasileiro com o título de Hospital Amigo da Criança. Epidemiol Serv Saúde [Internet]. 2016 jun [citado 2020 mar 6];25(2):281-90. Disponível em: Disponível em: https://doi.org/10.5123/s1679-49742016000200007 [ Links ]
23. Beck AMO, Assunção KO, Barbosa LR, Gomes E. Influência do ambiente hospitalar nos aspectos relacionados ao aleitamento materno. Rev Soc Bras Fonoaudiol [Internet]. 2012 dez [citado 2020 mar 6];17(4):464-8. Disponível em: Disponível em: https://doi.org/10.1590/S1516-80342012000400017 [ Links ]
24. Rodrigues AP, Padoin SMM, Guido LA, Lopes LLD. Fatores do pré-natal e do puerpério que interferem na autoeficácia em amamentação. Esc Anna Nery [Internet]. 2014 jun [citado 2020 mar 6];18(2):257-61. Disponível em: Disponível em: https://doi.org/10.5935/1414-8145.20140037 [ Links ]
25. Caldeira AP, Gonçalves E. Assessment of the impact of implementing the Baby- Friendly Hospital Initiative. J Pediatr [Internet]. 2007 Mar-Apr [cited 2020 Mar 6];83(2):127-32. Available from: Available from: https://doi.org/10.1590/S0021-75572007000200006 [ Links ]
26. Labbok MH. Global Baby-Friendly Hospital Initiative monitoring data: update and discussion. Breastfeed Med [Internet]. 2012 Aug [cited 2020 Mar 6];7(4):210-22. Available from: https://doi.org/10.1089/bfm.2012.0066 [ Links ]
27. Hawkins SS, Stern AD, Baum CF, Gillman MW. Compliance with the Baby- Friendly Hospital Initiative and impact on breastfeeding rates. Arch Dis Child Fetal Neonatal Ed [Internet]. 2014 Mar [cited 2020 Mar 6];99(2):138-43. Available from: Available from: http://dx.doi.org/10.1136/archdischild-2013-304842 [ Links ]
*Manuscript originated from the final Nutrition Course assignment entitled ‘Prevalence of maternal breastfeeding in the first hour of life and associated factors’, submitted by Priscilla Keylla Santos Sousa to the Multidisciplinary Health Institute, Federal University of Bahia (IMS/UFBa), Anísio Teixeira Campus, in 2018.
Received: October 25, 2019; Accepted: February 18, 2020











 texto em
texto em