Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Epidemiologia e Serviços de Saúde
versão impressa ISSN 1679-4974versão On-line ISSN 2237-9622
Epidemiol. Serv. Saúde vol.30 no.2 Brasília 2021 Epub 30-Abr-2021
http://dx.doi.org/10.1590/s1679-49742021000200002
Original Article
The effect of laboratory testing on COVID-19 monitoring indicators: an analysis of the 50 countries with the highest number of cases*
1Universidade Federal de Minas Gerais, Departamento de Medicina Preventiva e Social, Belo Horizonte, MG, Brasil
2Fundação Instituto Oswaldo Cruz, Centro de Integração de Dados e Conhecimentos para Saúde, Salvador, BA, Brasil
3Universidade Federal da Bahia, Instituto de Saúde Coletiva, Salvador, BA, Brasil
Objective
To analyse how testing the population influences the health indicators used to monitor the COVID-19 pandemic in the 50 countries with the highest number of diagnosed cases.
Methods
This was an ecological study using secondary data retrieved on 8/19/2020. Cumulative incidence, mortality rate, case-fatality rate, and proportion of positive tests were calculated. The data were described and presented graphically, with their respective Spearman Correlation Coefficients.
Results
The testing rate varied enormously between countries. Cumulative incidence and the proportion of positive tests were correlated with the number of tests, while the mortality rate and case-fatality rate showed low correlation with this indicator.
Conclusion
Most countries do not test enough to ensure adequate monitoring of the pandemic, and this is reflected in the quality of the indicators. Expanding the number of tests is essential, but it needs to be accompanied by other measures, such as isolation of diagnosed cases and contact tracing.
Keywords: Coronavirus Infections; Health Status Indicators; Testing Strategies; Incidence; Mortality; SARS-CoV-2
Introduction
Between the first case of the novel coronavirus disease (COVID-19) being identified and August 19, 2020, more than 22 million cases were diagnosed, and 781,000 deaths were reported worldwide.1
The high spreading power of the coronavirus causing the disease, SARS-CoV-2, and the growing number of cases reinforce the importance of understanding the epidemiological situation in a country or region in order to plan the most appropriate responses.2 Accordingly, laboratory testing to diagnose infection is of paramount importance to ascertain the infection’s magnitude, control and monitoring.
Testing can be used to (i) identify the active presence of the virus by detecting its genome in upper and lower respiratory tract samples, with the real-time reverse transcription polymerase chain reaction (real-time RT-PCR) test being the most adopted; testing also allows (ii) detection of specific antibodies in blood samples, the presence of which is indicative of previous infection, the latter being serologic tests, functionally simpler and frequently used in epidemiological surveys.3
Despite the importance testing has for controlling SARS-CoV-2 infection, the strategies employed vary among different countries and epidemic stages.4 Asian countries already affected by other respiratory epidemics, such as Taiwan and Hong Kong (China), and others, such as New Zealand, Iceland, Monaco, and Germany, have adopted broader strategies, usually testing suspects with mild symptoms to identify and isolate cases and track their respective contacts.5
Other countries, due to budget constraints, population size or the plans of the current government, have adopted more limited strategies.5 In such circumstances, testing has been restricted to people with severe symptoms, those who have had contact with a confirmed case and those belonging to ‘high-risk’ groups; or to a combination of these and other criteria.6 This has happened in the European countries most affected by the epidemic, in the United States and Japan, and in low and middle-income Asian, African and Latin American countries.
The testing strategies adopted influence the estimated number of SARS-CoV-2 infections and deaths. Therefore, the strategies adopted affect the quality of health indicators that are essential for planning and executing actions aimed at controlling the pandemic.2,7
This article aimed to analyze how population testing influences the health indicators used to monitor the COVID-19 pandemic in the 50 countries with the highest number of diagnosed cases.
Methods
This survey consists of an ecological study performed on secondary data. The 50 countries with the highest number of COVID-19 diagnosed cases were selected, reported as at August 19, 2020, the date on which the data were retrieved. Testing data were obtained from the Worldometers website (https://www.worldometers.info/coronavirus/).
Worldometers is a website that analyzes, validates and aggregates data from thousands of real-time sources, including official websites of ministries of health and/or other government bodies, social media accounts of government officials and, eventually, information from important and reliable news channels, whose data is available before being published on official websites. In Worldometers, the information available does not distinguish between the type of test performed (RT-PCR or serologic), which is why in this document, when referring to testing for SARS-CoV-2, both RT-PCR and serologic tests are addressed.
COVID-19 cases and deaths were obtained from the European Center for Disease Control website.1 The case definition varies from country to country: some consider ‘confirmed cases’ to be only those with laboratory diagnosis, while others consider ‘COVID-19 cases’ to be both those with laboratory diagnosis and those identified by clinical-epidemiological criteria. This document considers ‘diagnosed COVID-19 cases’, regardless of the diagnostic criteria used. In turn, the 2019 population estimates were obtained from the World Bank (https://data.worldbank.org/indicator/SP.POP.TOTL).
Based on these data, the following indicators were calculated:
testing rate (number of tests performed, per one million inhabitants);
cumulative incidence (number of diagnosed cases divided by local population, presented per one million inhabitants);
mortality rate (number of deaths from the disease divided by the local population, presented per one million inhabitants);
case fatality rate (number of deaths per number of registered cases, expressed as a percentage); and
proportion of positive tests (number of positive tests per number of tests performed, expressed as a percentage).
Descriptive analyses and graphical representations (scatter diagrams) of cumulative incidence, mortality rate, fatality rate and proportion of positive tests in relation to each country’s testing rate were performed. For each scatter plot, a linear line representing the expected values of the indicator analyzed for the test rate is estimated. A 95% confidence interval (95% CI) is superimposed on this straight line and shown in gray. The linear or logarithmic scale used in the graphs was selected to permit a more accurate view of the trends.
The data did not show normal distribution (Shapiro-Wilk: p-value<0.001), which is why Spearman’s correlation coefficient was used to evaluate the correlations between the number of tests and the selected health indicators (cumulative incidence, mortality rate, fatality rate and proportion of positive tests). The data were processed and analyzed by the ggplot28 statistical package in R version 4.0.1.9
Results
Figure 1 shows how many tests were performed per one million inhabitants. A first group of countries that performed more than 100,000 tests per one million inhabitants was comprised, for the most part, of countries in Western Europe, countries in Asia with high gross domestic product (GDP) per capita, Canada, the United States and Chile. The United Arab Emirates and Bahrain stood out in this group, for presenting test coefficients much higher than the others, above 550,000 tests per one million inhabitants. Sweden, France, Holland, Turkey, Romania, Poland, Brazil, Peru, Panama, China, Oman and South Africa were distributed in an intermediate block, between 100 and 50,000 tests per one million inhabitants. Those with the lowest number of tests performed, i.e., less than 50,000 tests per one million inhabitants, are the majority of Latin American countries, Asian countries with lower GDP per capita and Japan, besides Nigeria and Egypt.
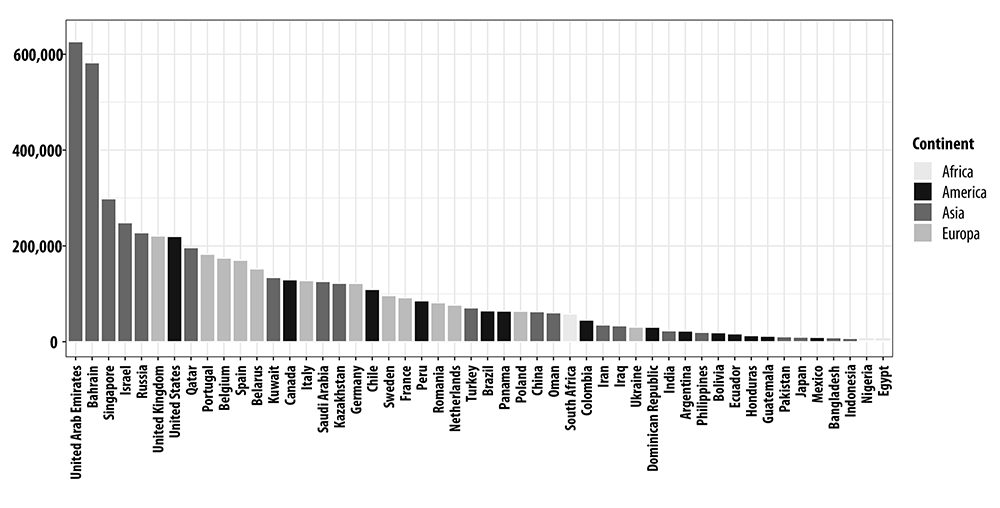
Figure 1 Number of SARS-CoV-2 diagnostic tests per one million inhab. in the 50 countries with the highest COVID-19 case numbers, as at August 19, 2020
Figure 2A shows that cumulative incidence increased with the number of tests performed per one million inhabitants. (ρxy = 0.558), while Figure 2B shows the low correlation between mortality and the number of tests performed per one million inhabitants. (ρxy = 0.253). Most Latin American countries had higher than expected cumulative incidence and mortality rates, according to their testing rates. As for the European countries studied, their cumulative incidence rates were close to expected for countries with the corresponding testing rate; their mortality rate, however, was higher than expected, in general. Most Asian countries that were evaluated, constituting the group with the highest levels of COVID-19 testing, had cumulative incidence rates close to expected, but mortality rates lower than that of other nations with the same test rates.
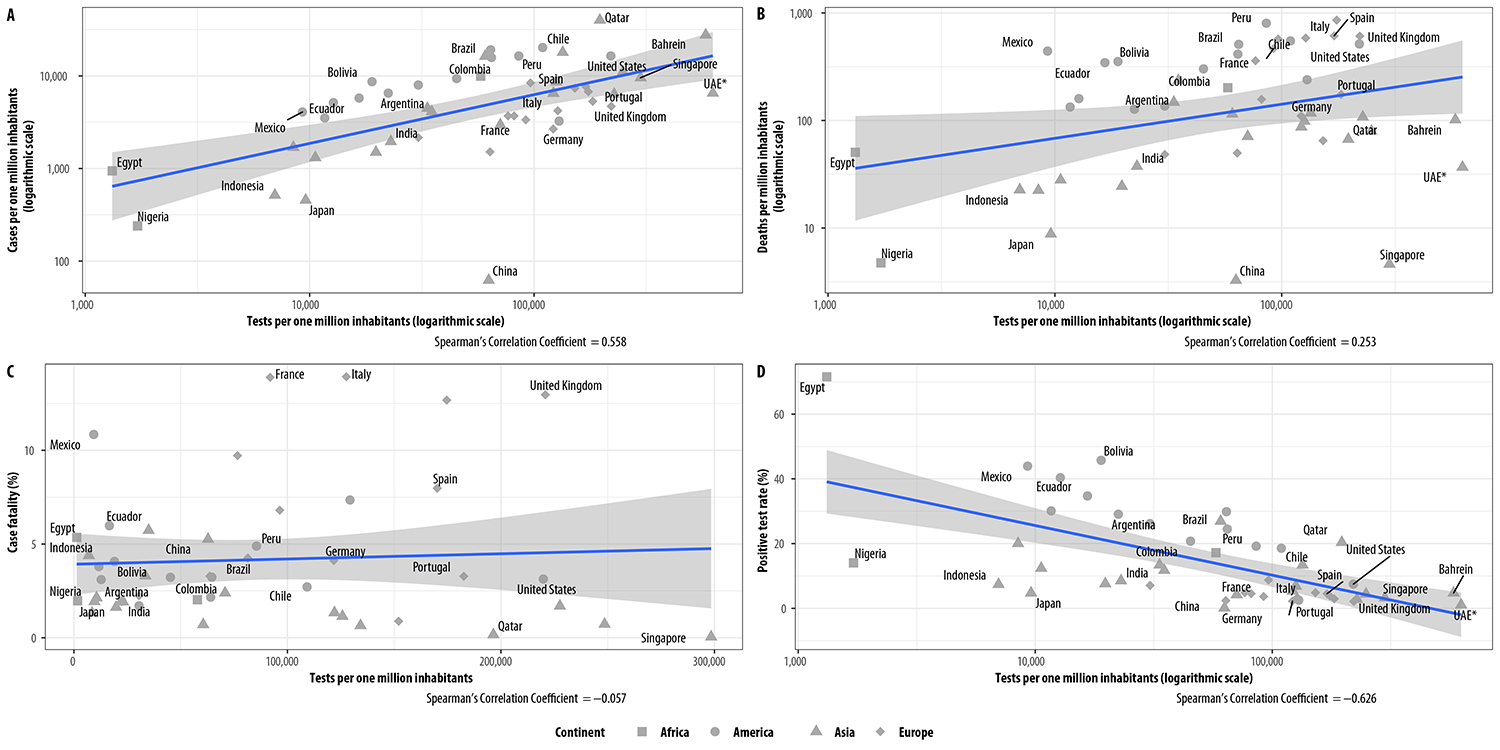
a) Bahrain and United Arab Emirates excluded for being outliers (very high test numbers); *United Arab Emirates.
Figure 2 Relation between tests performed and COVID-19 monitoring indicators (A, diagnosed cases per one million inhab.; B, deaths per one million inhab.; C, fatality;a and D, proportion of positive tests) in the 50 countries with the greatest case numbers of the disease, as at August 19, 2020
Figure 2C shows that there was no correlation between the fatality rate and testing per one million inhab. (ρxy = -0.057). European countries such as France, Italy, Belgium, Netherlands and United Kingdom, and Mexico, in North America, stood out for having much higher-than-expected fatality rates, according to their testing rates.
Lastly, in Figure 2D, it is possible to observe the decrease in the proportion of positive tests as the number of tests performed increased (ρxy = -0.626). Countries like Egypt, Bolivia and Mexico presented a high proportion of positive tests. In Brazil, the proportion was 24.5% for the period studied.
Discussion
The results of this study indicate that the testing rate varied immensely among the 50 countries with the highest number of diagnosed cases. There were countries that performed more than 550,000 tests per one million inhabitants, such as the United Arab Emirates and Bahrain, and others that performed less than 1,350 tests per one million inhabitants, such as Egypt. The findings show that some epidemiological indicators, such as cumulative incidence and positive test proportion, are correlated to the number of tests performed for diagnosis of infection, whereas the mortality and fatality rates showed low correlation with this indicator.
Some countries, among the 50 observed, reported low population testing rates. These are low and middle-income countries, located in Latin America, Asia and Africa, where the epidemic started more recently, when compared to European countries. The exception was Japan. The low number of tests performed per one million inhabitants in these countries may be related to resource prioritization, directed only towards severe cases, as occurs in Mexico,10 or to difficulty in expanding testing capacity, as occurs in Egypt11 and Nigeria.12
On the other hand, countries that have already performed a number of tests corresponding to more than half their population, such as the United Arab Emirates and Bahrain, stand out. It is possible that previous experiences of these countries with the Middle East Respiratory Syndrome (MERS) left them better prepared to accommodate the demands generated by subsequent outbreaks of respiratory viruses such as SARS-CoV-2.13 However, the high testing rate did not prevent these countries from being among the 50 with the highest number of cases. This is possibly due to the lack of coupling extensive testing with non-pharmacological control measures, although the recent drop in the number of daily cases in these countries1 may indicate that the more comprehensive testing employed contributes to the decline observed.
The data analyzed showed a moderate correlation between the testing rate and cumulative incidence. It is expected that as more tests are performed, more cases will be diagnosed. China seems to emerge as an exception to this pattern: despite having expanded its testing strategy, allowing RT-PCR to be performed even for people with low suspicion of COVID-19, an expressive low cumulative incidence rate was maintained, compared to other countries with the same testing rate. This behavior can be explained by the combination of the growing number of diagnostic tests performed and isolation of new cases.14 This type of behavior has also been noticed in countries that have been successful in combating the epidemic, despite not being among the 50 with the highest number of cases, such as New Zealand,15 South Korea6 and Iceland.16 In the case of China, previous experiences with MERS and severe acute respiratory syndrome (SARS) may also have contributed to it having a pattern different from the others.14 Moreover, it is important to consider that in February 2020, when China was reaching the highest number of daily cases to date, the diagnostic tests developed were submitted to emergency approval procedures. This may have impacted on a considerable percentage of false negative results, which may also explain, albeit partially, China’s lower cumulative incidence.14,17
The mortality rate was positively correlated with testing, as was cumulative incidence, although with less magnitude. Some European countries, where cumulative incidence was within expectations, presented COVID-19 mortality rates above those of countries with equivalent test rates. Several factors could contribute to this result, such as older age of the population and therefore the presence of comorbidities.18,19 Higher mortality in Western European countries may also be related to better investigation of deaths than of cases.20 Moreover, a change in the criteria for defining death or the difficulty in attesting to death from COVID-19 can interfere with these estimates. An example of this possibility lies in Italy, where researchers have reported difficulty in differentiating deaths directly caused by SARS-CoV-2 from deaths due to other causes, in individuals only infected with the virus. This fact is attributed to the presence of significant comorbidities in the vast majority of those diagnosed with COVID-19 who died: 98.8% had at least one comorbidity; and 48.6%, three or more.21
However, when comparing mortality rates, other factors must be considered, such as the moment in the epidemic. It can be noticed that countries with wider testing, such as China and Singapore, have mortality rates comparable to those of Nigeria, which came in second place among countries that tested less among the 50 with the highest number of cases assessed in this study. A low mortality rate does not necessarily reflect success in controlling the pandemic.22
Case fatality rate had low correlation with testing. If both cases (including asymptomatic cases) and deaths were adequately identified, COVID-19 fatality would be expected to be close to 1%;23 with few exceptions, the vast majority of countries reported a rate above this value. In some European countries such as France, Italy, the United Kingdom, Belgium and the Netherlands, as well as Mexico, this indicator is above 10%.
Fatality is influenced by demographic structure (countries with a higher proportion of elderly tend to present higher case fatality rate) and by national health system organization. A Public Health system that is better prepared to identify and isolate cases and treat those in need, will account for lower case fatality rate. Also, countries that identify deaths better than cases tend to present higher case fatality rate.20 In relation to this indicator, Brazil is close to the expected given its testing rate. In view of the country’s current scenario, it is possible to assume that the Brazilian result comes from widespread underreporting of both deaths and cases of SARS-CoV-2 infection.
Regarding the positive result test proportion, it was found that the higher the test rate, the lower this proportion. Some countries, such as Egypt, Mexico and Bolivia, showed a high positive test proportion, above 40%, indicating that only the most severe patients are tested, namely those seeking outpatient or hospital medical assistance. In addition, a high positive test proportion indicates that a country is not able to measure the actual extent of virus spread in its territory.24
The The World Health Organization (WHO) recommends: for a country to start relaxing quarantine and social distancing, the positive test rate should be 5% at the most for no less than 14 days.24 Latin American countries seem far from meeting this goal, since all of them have a positive test proportion of around 20% or more. Examples of this are Mexico and Brazil, which face similar problems, starting from the federal government’s refusal to recognize the pandemic as a Public Health problem, and therefore not tackling it through health policies, coordinated across ministries, jointly with their federative units.25,26 Both countries test only serious cases, despite Brazil’s slowly increasing testing rate: 64,593 tests per one million inhabitants when this report was concluded. Mexico (9,281 tests per one million inhabitants) continues to be one of the countries that least tests among the 50 with the highest number of diagnosed cases.22 Even in a testing scenario that falls short of what is necessary, and where there is a high percentage of positive tests - Mexico (43.9%) and Brazil (24.5%) - both countries have adopted measures to gradually reopen the economy that are not supported by epidemiological data or WHO recommendations.24 This deficient testing, verified in other Latin American nations as well, combined with prioritizing laboratory diagnosis for the severely symptomatic, may explain the higher than expected cumulative incidence and mortality rates when compared to other countries with a similar testing rate.
A low testing rate is one of the factors that can result in an underestimated number of infected people and therefore lower quality health indicators.2,7 Studies have shown that the mortality rate would be a more reliable indicator compared to incidence and case fatality,7,27 since the number of SARS-CoV-2 infection cases are generally more underestimated than the number of deaths from COVID-19.20
Adequate testing, which includes mild symptomatic and asymptomatic individuals, is crucial for the accurate and valid assessment of health indicators. A prediction study on data from 42 countries published in early April 2020 showed that a 10% increase in SARS-CoV-2 testing would lead to an increase of approximately 9% in the number of new cases, and a 9% reduction in case fatality rate.28 Using graph analysis, another study found that the testing strategy conducted in Italy identified a significant portion of the difference between case fatality rate in that country and others, such as China.29 The supposed shift from a narrower testing policy (which favors people with severe symptoms, prior contact with a confirmed case, belonging to a ‘high-risk’ group; or the combination of these and other criteria)6 to one with broader criteria and mass population testing, would result in greater detection of SARS-CoV-2 infected people, directly impacting better quality of health indicators. This change, moreover, would culminate in higher COVID-19 incidence and mortality.
The important role played by epidemiological surveillance in relation to the quality of COVID-19 indicators is worth stressing, as it is essential to obtain accurate information and draw a real picture of the health problem, as well as actions and interventions needed to address and solve it. Epidemiological surveillance is especially capable of assisting in COVID-19 case identification, through surveillance of the contacts of diagnosed and suspected cases, active surveillance at the Primary Care level of the Brazilian National Health System (SUS) and awareness as to the importance of prompt and correct case notification by professionals engaged in fighting the pandemic. As such, the quality of health indicators is also influenced - strongly - by epidemiological surveillance actions, essential for Public Health.30
Although this study presents important considerations on the impact of laboratory testing on the COVID-19 pandemic follow-up indicators, it has some limitations. The first is the quality of the available data, which do not distinguish the type of test performed (RT-PCR or serologic test). Some countries administer both tests for different purposes: whereas RT-PCR is employed to diagnose active infections, serologic tests are used to monitor past infections. However, it is not possible to guarantee whether these tests have been used adequately. The study’s second limitation is the difficulty in comparing data from countries that adopt different testing strategies, with greater or lesser involvement of serologic tests in the total of confirmed cases. Since SARS-CoV-2 is an emerging infectious agent and the available assays are not yet fully accurate for diagnosing infection, the consistency of laboratory results can be poor, which limits the conclusions than can be drawn. A third limitation of the study is that even very broad testing strategies, such as those adopted in some Asian countries, do not test the entire population. Given that a significant proportion of those infected develop subclinical infection, all indicators presented may be underestimated (cumulative incidence) or overestimated (mortality and case fatality rates). As the fourth and last limitation to consider, it must be taken into account that cases do not reflect solely those diagnosed by laboratory tests. Some countries have adopted clinical-epidemiological criteria in their case definition, which can further obscure the results found.
Despite the heterogeneity identified in the population testing rate and inconsistencies in the data, the survey results indicate that the vast majority of countries do not test sufficiently to ensure the quality of health indicators relative to COVID-19 and enable the planning of a safe return to normal social life throughout and after the pandemic. Low testing rates can result in underestimating the number of SARS-CoV-2 infected individuals and COVID-19 deaths. Health care managers need to be aware of how infection testing and surveillance are reflected in the quality of health indicators and their impact on health action planning. It is therefore necessary to provide more testing for the population in order to adequately monitor the epidemic’s extent. Only through reliable data will economic reopening policies be responsibly and safely planned for society, thus reducing the odds of new virus transmission waves and spread of the disease.
The conclusion is that the availability of more tests for the population is, on its own, insufficient to improve the quality of health indicators. This strategy must be supported by other measures, such as isolation of diagnosed cases and tracing their respective contacts. To achieve this, it is important that SUS Primary Care and Health Surveillance be well structured. Countries such as Brazil, served by a highly capillary health system, can make use of existing network and its Family Health Strategy, for following-up on COVID-19 cases and mapping their recent contacts.
Acknowledgment
To ‘Rede CoVida - Ciência, Informação e Solidariedade’ [‘CoVida Network - Science, Information and Solidariety’], for facilitating the meeting between the authors and the opportunity for rich discussions that led to this study being idealized, as well as their suggestions, which contributed to the improvement of several aspects of this article.
REFERENCES
1. Centro Europeu de Prevenção e Controle de Doenças. COVID-19 pandemic [Internet]. Solna: Centro Europeu de Prevenção e Controle de Doenças; 2020 [cited 2020 Aug 20]. Available from: https://www.ecdc.europa.eu/en/covid-19-pandemic [ Links ]
2. Lachmann A, Jagodnik KM, Giorgi FM, Ray F. Correcting under-reported COVID-19 case numbers: estimating the true scale of the pandemic. medRxiv [Internet]. 2020 Apr [cited 2020 Jun 8]. Available from: https://doi.org/10.1101/2020.03.14.20036178 [ Links ]
3. Tang Y-W, Schmitz JE, Persing DH, Stratton CW. Laboratory diagnosis of COVID-19: current issues and challenges. J Clin Microbiol [Internet]. 2020 [cited 2020 Jun 16];58(6):e00512-20. Available from: https://jcm.asm.org/content/58/6/e00512-20 [ Links ]
4. Red Argentina Pública de Evaluación de Tecnologías Sanitarias. Diferentes tipos de tests y estrategias diagnósticas en el contexto de pandemia por COVID-19 [Internet]. [S.l.]: Red Argentina Pública de Evaluación de Tecnologías Sanitarias; 2020 [citado 2020 jun 8]. Disponível em: http://www.femeba.org.ar/documentos/download/4792-diferentes-tipos-de-tests-y-estrategias-diagnosticas-en-el-contexto-de-pandemia-por-covid-19-redarets-04-2020.pdf [ Links ]
5. Cohen J, Kupferschmidt K. Countries test tactics in ‘war’ against COVID-19. Science [Internet]. 2020 Mar [cited 2020 Jun 8];367(6484):1287-8. Available from: https://www.sciencemag.org/lookup/doi/10.1126/science.367.6484.1287 [ Links ]
6. Richterich P. Severe underestimation of COVID-19 case numbers: effect of epidemic growth rate and test restrictions. medRxiv [Internet]. 2020 Apr [cited 2020 Jun 8]. Available from: http://medrxiv.org/lookup/doi/10.1101/2020.04.13.20064220 [ Links ]
7. Rajgor DD, Lee MH, Archuleta S, Bagdasarian N, Quek SC. The many estimates of the COVID-19 case fatality rate. Lancet Infect Dis [Internet]. 2020 Jul [cited 2020 Jun 8]:20(7):776-7. Available from: https://doi.org/10.1016/S1473-3099(20)30244-9 [ Links ]
8. Wickham H. ggplot2: elegant graphics for data analysis. 2nd ed. Cham: Springer; 2016. [ Links ]
9. R Core Team. R: A language and environment for statistical computing [Internet]. Vienna, Austria: R Foundation for Statistical Computing; 2020 [cited 2020 Dec 8]. Available from: https://www.R-project.org/ [ Links ]
10. Martínez-Anaya C, Ramos-Cervantes P, Vidaltamayo R. Coronavirus, diagnóstico y estrategias epidemiológicas contra COVID-19 en México. Educación Química [Internet]. 2020 [citado 2020 jun 8];31(2):12-22. Disponível em: http://dx.doi.org/10.22201/fq.18708404e.2020.2.75378 [ Links ]
11. Organização Mundial de Saúde - OMS. WHO delegation concludes COVID-19 technical mission to Egypt [Internet]. Cairo: Organização Mundial de Saúde Escritório Regional para o Mediterrâneo Oriental; 2020 [citado 2020 jun 15]. Available from: http://www.emro.who.int/media/news/who-delegation-concludes-covid-19-technical-mission-to-egypt.html [ Links ]
12. Onyeaghala AA, Olajide I. Managing COVID-19 outbreak in Nigeria: matters arising. Clin Chem Lab Med [Internet]. 2020 Jul [cited 2020 Jul 21];58(10):1645-50. Available from: https://doi.org/10.1515/cclm-2020-0748 [ Links ]
13. Shammah A, Budoor H, Suad M, Alahmadi, Richard K, Maha S, et al. Middle east respiratory syndrome corona virus (MERS-CoV): levels of knowledge and Awareness in Bahrain. KLS [Internet]. 2018 Oct [cited 2020 Aug 24];4(6):98. Available from: https://doi.org/10.18502/kls.v4i6.3094 [ Links ]
14. Organização Mundial de Saúde - OMS. Report of the WHO-China joint mission on coronavirus disease 2019 (COVID-19) [Internet]. Genebra: Organização Mundial de Saúde; 2020 [cited 2020 Jun 15]. Available from: https://www.who.int/docs/default-source/coronaviruse/who-china-joint-mission-on-covid-19-final-report.pdf [ Links ]
15. Cousins S. New Zealand eliminates COVID-19. Lancet [Internet]. 2020 May [cited 2020 Jun 15];395(10235):1474. Available from: https://doi.org/10.1016/S0140-6736(20)31097-7 [ Links ]
16. Gudbjartsson DF, Helgason A, Jonsson H, Magnusson OT, Melsted P, Norddahl GL, et al. Spread of SARS-CoV-2 in the Icelandic population. N Engl J Med [Internet]. 2020 Jun [cited 2020 Aug 24];382(24):2302-15. Available from: http://www.nejm.org/doi/10.1056/NEJMoa2006100 [ Links ]
17. Wang Y, Kang H, Liu X, Tong Z. Combination of RT-qPCR testing and clinical features for diagnosis of COVID-19 facilitates management of SARS-CoV-2 outbreak. J Med Virol [Internet]. 2020 Feb [cited 2020 Oct 19];92(6):538-9. Available from: https://doi.org/10.1002/jmv.25721 [ Links ]
18. Promislow DEL. A geroscience perspective on COVID-19 mortality. J Gerontol [Internet]. 2020 Apr [cited 2020 Jul 22];75(9):e30-3. Available from: https://doi.org/10.1093/gerona/glaa094 [ Links ]
19. Yang J, Zheng Y, Gou X, Pu K, Chen Z, Guo Q, et al. Prevalence of comorbidities and its effects in patients infected with SARS-CoV-2: a systematic review and meta-analysis. Int J Infect Dis [Internet]. 2020 Mar [cited 2020 Jul 22];94:91-5. Available from: https://doi.org/10.1016/j.ijid.2020.03.017 [ Links ]
20. Rudnicki WR, Piliszek R. Estimate of Covid-19 prevalence using imperfect data. medRxiv [Internet]. 2020 Apr [cited 2020 Jun 9]. Available from: https://doi.org/10.1101/2020.04.14.20064840 [ Links ]
21. Boccia S, Ricciardi W, Ioannidis JPA. What other countries can learn from Italy during the COVID-19 pandemic. JAMA Intern Med [Internet]. 2020 Apr [cited 2020 Jun 8];180(7):927-8. Available from: https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/2764369 [ Links ]
22. Worldometers. COVID-19 Coronavirus pandemic [Internet]. [S.l.]: Worldometers; 2020 [cited 2020 Aug 19]. Available from: https://www.worldometers.info/coronavirus / [ Links ]
23. Moriarty LF, Plucinski MM, Marston BJ, Kurbatova EV, Knust B, Murray EL, et al. Public health responses to COVID-19 outbreaks on cruise ships - worldwide, February-March 2020. MMWR Morb Mortal Wkly Rep [Internet]. 2020 Mar [cited 2020 Jun 8];69(12):347-52. Available from: http://dx.doi.org/10.15585/mmwr.mm6912e3 [ Links ]
24. Johns Hopkins Coronavirus Resource Center. Which U.S. States meet Recommended positivity levels? [Internet]. Baltimore: Johns Hopkins Coronavirus Resource Center; 2020 [cited 2020 Aug 19]. Available from: https://coronavirus.jhu.edu/testing/testing-positivity [ Links ]
25. Agren D. Mexican president López Obrador draws doctors’ ire. Lancet [Internet]. 2020 May [cited 2020 Jul 16];395(10237):1601. Available from: https://doi.org/10.1016/S0140-6736(20)31198-3 [ Links ]
26. The Lancet. COVID-19 in Brazil: “So what?” Lancet [Internet]. 2020 May [cited 2020 Aug 19];395(10235):1461. Available from: https://doi.org/10.1016/S0140-6736(20)31095-3 [ Links ]
27. Hallal PC. Worldwide differences in COVID-19-related mortality. Ciênc saúde coletiva [Internet]. 2020 Jun [cited 2020 Jun 8];25(suppl 1):2403-10. Available from: https://doi.org/10.1590/1413-81232020256.1.11112020 [ Links ]
28. Asahi K, Undurraga EA, Wagner R. Benchmarking the CoVID-19 pandemic across countries and states in the USA under heterogeneous testing. medRxiv [Internet]. 2020 May [cited 2020 Jun 8]. Available from: http://medrxiv.org/lookup/doi/10.1101/2020.05.01.20087882 [ Links ]
29. Barone-Adesi F, Ragazzoni L, Schmid M. Investigating the determinants of high case-fatality rate for coronavirus disease 2019 in Italy. Disaster Med Public Health Prep [Internet]. 2020 Apr [cited 2020 Jun 8];1-2. Available from: https://doi.org/10.1017/dmp.2020.106 [ Links ]
30. Ibrahim NK. Epidemiologic surveillance for controlling Covid-19 pandemic: types, challenges and implications. J Infect Public Health [Internet]. 2020 Nov [cited 2020 Oct 2];13(11):1630-8. Available from: https://doi.org/10.1016/j.jiph.2020.07.019 [ Links ]
Received: September 08, 2020; Accepted: November 25, 2020











 texto em
texto em 
 Curriculum ScienTI
Curriculum ScienTI

