Servicios Personalizados
Revista
Articulo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares en
SciELO
Similares en
SciELO
Compartir
Epidemiologia e Serviços de Saúde
versión impresa ISSN 1679-4974versión On-line ISSN 2237-9622
Epidemiol. Serv. Saúde vol.30 no.2 Brasília 2021 Epub 28-Mayo-2021
http://dx.doi.org/10.1590/s1679-49742021000200016
ORIGINAL ARTICLE
Population with high cardiovascular risk receiving drug therapy and counseling: Brazil’s status regarding the global goal, 2014-2015
1Universidade Federal de Minas Gerais, Departamento de Enfermagem Materno-Infantil e Saúde Pública, Belo Horizonte, MG, Brasil
2Universidade Federal de Minas Gerais, Faculdade de Medicina, Belo Horizonte, MG, Brazil
3Universidade Federal de Minas Gerais, Escola de Enfermagem, Belo Horizonte, MG, Brazil
4Ministério da Saúde, Departamento de Análise em Saúde e Vigilância de Doenças não Transmissíveis, Brasília, DF, Brazil
5Organização Mundial da Saúde para as Américas, the Pan American Health Organization Regional Office, Washington, DC, The United States
Objective:
To estimate the prevalence of high cardiovascular risk (CVR), the proportion of people with high CVR who receive treatment and counseling, and to investigate the sociodemographic factors associated with this outcome, in Brazil.
Methods:
This was a cross-sectional study, using subsample data from the National Health Survey, collected via biochemical tests, in 2014-2015. Poisson regression was used.
Results:
The proportion of high CVR in men was 11.2% (95%CI 9.6;12.9), and 10.4% (95%CI 9.2;11.8%) in women. In the group with high CVR, 68.8% (95%CI 63.7;73.4%) received counseling, 59.3% (95%CI 54.2;64.3%) received medication, and 55.6% (95%CI 50.4;60.7%) received both. In the multivariate analysis, receiving treatment and counseling was associated with being aged 50 years and over, and poor/very poor self-rated health (PR=1.26 - 95%CI 1.06;1.51).
Conclusion:
The proportion of people with high CVR who had received treatment and counseling was over 50%.
Keywords: Cardiovascular Diseases; Secondary Prevention; Public Health; Cross-Sectional Studies.
Introduction
Cardiovascular diseases are a group of diseases that affect the heart and blood vessels, and are the leading cause of death globally.1 They accounted for 18 million deaths in 2016, 44.0% of deaths from chronic noncommunicable diseases (NCDs), and 31.0% of all causes of death worldwide. The majority of deaths attributed to them have occurred in low- and middle-income countries.1 Studies point to an unequal distribution of NCDs and cardiovascular diseases, due to social determinants such as poverty, low schooling, insufficient income,2,3 urbanization, stress, and population ageing, in addition to behavioral and metabolic risk factors.1-4
Public policies are necessary to control modifiable risk factors, such as tobacco consumption, harmful alcohol use, too much salt in the diet, unhealthy eating habits and sedentary lifestyle, and biological factors such as the presence of systemic arterial hypertension, diabetes mellitus and hyperlipidemia.1,4,5 Identification of people at high cardiovascular risk or with pre-existing cardiovascular diseases, resulting from the presence of risk factors, is a priority action for early detection and management of these risks. Health policies are needed to encourage the creation of environments conducive to healthy, accessible and available choices for the population. These policies should be based on strategies that motivate people to adopt and maintain healthy behaviors, such as counseling, and on the use of medications and especially hypertension and diabetes control.1,4
In order to reduce the burden of NCDs and the high number of premature deaths, global commitments have been established to address cardiovascular diseases, including (i) the Global Action Plan for the Prevention and Control of NCDs, proposed by the World Health Organization (WHO),4 and (ii) the United Nations (UN) 2030 Agenda for Sustainable Development, with its Sustainable Development Goals.6 Both initiatives have included the goal of reducing premature mortality from NCDs. The Global Action Plan, adopted by all UN Member States as a priority, included a specific goal: to have implemented counseling and drug treatment measures for 50% of people at cardiovascular risk.1,4,5
This study is justified in view of the relevance and impact of cardiovascular diseases on the population and health services, and the unprecedented nature of monitoring this goal for Brazil. Its objective was to estimate the prevalence of high cardiovascular risk (CVR), the proportion of people with high CVR receiving treatment and counseling, and to investigate the sociodemographic factors associated with this outcome in Brazil.
Methods
This was a cross-sectional study, with secondary data on biochemical tests performed as part of the National Health Survey (PNS).
The first edition of the PNS, in 2013, was conducted by the Brazilian Institute of Geography and Statistics (IBGE) in partnership with the Ministry of Health, and covered approximately 64 million Brazilian households.7 The 2013 PNS was complemented in 2014-2015, with the collection of biological samples from a subsample, comprised of 12 million households, for biochemical tests.7-11
The subsample in question, consisting of 25% of the census tracts selected for the 2013 PNS, followed PNS sample stratification, with probability inversely proportional to the difficulty of collecting samples.11 The sampling plan used was cluster sampling, in three stages of selection: the primary sampling units (PSU) corresponded to the sectors or composition of selected census tracts; in the second stage, a fixed number of permanent private households (10 to 14) was selected by simple random sampling in each PSU; and in the third stage, a resident aged 18 years or older, also randomly selected, was selected from an eligible list made at the time of the interview.11 Taking 25% of the census tracts for laboratory tests and assuming a non-response rate of 20%, the expected number of individuals with laboratory data was approximately 12 million.11 In Brazil as a whole, biochemical tests were performed on 8,952 individuals; more details are available in a specific publication.11 Figure 1 shows the sample building flow and losses during the process.
Data collection for biochemical tests occurred at participants' homes, performed by agents from contracted laboratories and strictly following the current standards for the collection, transport and processing of biological material.11 Laboratory data and responses to interviews served to make up the CVR calculation algorithm proposed by the WHO.12,13 The following mean cut-off points were adopted: (i) diabetes - glycated hemoglobin ≥6.5% for both sexes - and (ii) total cholesterol >160 mg/dl for biochemical information. In the older age groups, the cut-off points were lower. Further details on the cut-off points adopted, according to age group, sex, cholesterol level, glycated hemoglobin level and smoking or not, are available in published documents.13
The study participants were individuals aged 40 years or over who agreed to sample collection for biochemical tests during the interview, as Figure 1 also illustrates.
People with high CVR were identified by the answers to the following questions:
"Have you ever been diagnosed with heart disease, such as heart attack, angina, heart failure or other heart disease, by any doctor?"
"Have you ever been diagnosed with stroke, by any doctor?"
In the algorithm used for the calculation of CVR, the following variables were considered: age; sex; blood pressure; smoking status (current smoker or who quit smoking at least one year before evaluation); total cholesterol; and diabetes.1,8-10 Blood pressure was measured by a digital device three times, taking the mean measurements, as previously recommended.14
The proportional reference measure of high CVR (>30%) followed the WHO recommendation and considered, in the construction of the algorithm, variables such as sex, age, total cholesterol and HDL cholesterol measurements, treated and untreated systemic arterial pressure, being a smoker (yes; no) and having diabetes (yes; no).12 Different calculations were performed for men and women, and specific risks were calculated by sex and age. Cut-off point details used for the calculation of CVR can be found in other publications.13
The indicator for Goal 8 of the Global Action Plan for the Prevention and Control of NCDs was adopted in order to calculate the proportion of the sample, in accordance with the WHO protocol.1,4,5 This goal is related to national health system capacity to respond to cardiovascular diseases and it establishes at least half (50%) of eligible people with high CVR having received treatment and counseling, including glycemic control, to prevent heart attack and stroke.5 The proportion of eligible people was adopted in this calculation, i.e., aged ≥40 years, with high CVR or preexisting cardiovascular disease, self-reported in the PNS; and among those who had high CVR, those who had received treatment and counseling, including glycemic control, according to sex.
Receiving 'treatment' was defined as self-reporting of receiving drug therapy for cardiovascular diseases, according to the answers to the PNS questionnaire. Thus, the positive answers to the following questions were considered:
"Have you taken medication for high blood pressure (hypertension) in the last two weeks?"
"In the last two weeks have you ‘taken oral sugar-lowering medications for diabetes?' or 'Have you used insulin?'"
A 'positive response' for counseling was considered to be confirmation of having received at least one recommendation from the doctor or another health professional, such as maintaining healthy eating lifestyle, reducing daily salt intake, maintaining healthy weight, practicing physical activity, quitting smoking, reducing alcohol consumption, regular follow-up, among other specific questions for each of the following diseases: hypertension, diabetes and cholesterol.
A descriptive analysis of the indicators was performed, and the prevalence of high CVR was presented according to sex. The proportion of the population with high CVR who reported having received (i) treatment, (ii) counseling and (iii) both treatment and counseling, were analyzed according to sociodemographic variables. The variables used in this analysis were:
Sex (male; female);
Age (years: 40 to 49; 50 to 59; 60 to 69; 70 or over);
Region of residence (North; Northeast; Southeast; South; Midwest);
Race/skin color (categorized as: black and brown; other [white, indigenous and yellow]);
Schooling (subdivided between those who had not completed elementary school [without education or incomplete elementary school] and those with at least complete elementary school [complete elementary school, incomplete or complete high school, complete or incomplete higher education]);
Self-rated health (divided between [i] those who reported poor or very poor health and [ii] the group with fair, good or very good health); and
Having private health insurance (yes; no).
Then, the prevalence ratios (PR) of the population with high CVR or preexisting disease were estimated according to sociodemographic variables and their respective 95% confidence intervals 95%CI.
In the multivariate analysis, the PRs were estimated using the Poisson15 regression model with robust variance for the population with CVR, according to sex, age, schooling, race/skin color, health insurance, self-rated health and region of residence in the country of residence. Initially, the crude PR was estimated and then the multivariate analysis was performed, including the whole set of variables studied, and adjusted PR was estimated. The analyses were performed using Stata software, version 14, with the survey command, using post-stratification weights, according to sex, age, schooling and region of residence, because of collection losses. This process is also detailed in other publications.11
The PNS project was approved by the National Research Ethics Committee/National Health Council (Conep/CNS): in its Opinion No. 328,159, issued on June 26, 2013. All participants were consulted and once they had been informed, they agreed to participate in the research by signing the Free and Informed Consent Form. The results were given to the service users by the contracted laboratory and in cases of results outside the reference range, they were instructed to seek medical assistance in the public health system. In cases of high risk, service users were contacted directly by the contracted laboratory or the Ministry of Health for immediate care.11
Results
The study analyzed information from the PNS biochemical database (n=8,952) and included individuals aged 40 years or older (n=5,319). Table 1 shows sampling distribution by sex, among people with high or low CVR, according to sociodemographic variables.
The proportion of women with high CVR was 10.4% (95%CI 9.2;11.8), and high CVR increased with age: 4.2% (95%CI 3.0;5.9) among those aged 40 to 49 years and 22.2% (95%CI 18.1;26.8) among those aged 70 or older. Regarding education, the proportion of CVR was higher in women with incomplete elementary education, 13.4% (95%CI 11.6;15.6), and those of white race/skin color and race skin color other than black/brown, 11.2% (95%CI 9.3;13.5). CVR prevalence did not differ whether or not they had private health insurance. In women with poor/very poor self-rated health, the proportion of high CVR was 22.3% (95%CI 17.5;28.0), being higher in the Southern region, 14.9% (95%CI 11.9;18.7), compared to the other macro-regions in the country (Table 1).
The proportion of men with high CVR was 11.2% (95%CI 9.6;12.9), and as with women prevalence increased with age: 3.5% (95%CI 1.9;6.1) between 40 and 49 years old, and 24.9% (95%CI 19.8;30.8) at 70 years of age or over; and was also higher in men with low schooling. No differences were observed in relation to race/skin color or having private health insurance. The proportion of high CVR was greater in men with poor/very poor self-rated health, 23.0% (95%CI 17.0;30.4), and also in men living in the Southern region (Table 1).
Of the total number of people, of both sexes, with high CVR, 68.8% (95%CI 63.7;73.4) received counseling, 59.3% (95%CI 54.2;64.3) received treatment with medications, while 55.6% (95%CI 50.4;60.7) received both. Among women, specifically, 70.8% (95%CI 64.3;76.6) received counseling, 63.0% (95%CI 56.3;69.2) received treatment with medication and 59.1% (95%CI 52.4;65.5) received both. Among men, 66.5% (95%CI 58.5;73.7) received counseling, 55.3% (95%CI 47.4;63.0) received treatment, and 51.8% (95%CI 44.0;59.6) received both (Table 2).
Figure 2 shows the proportion of individuals with high CVR who received treatment and counseling. There was an increase in the proportion of the provision of both services as age increased: close to 30.0% in individuals aged 40 to 49 years, reaching around 65.0% in those aged 70 years and over. Among men, the proportion of those who received treatment and counseling reached 51.8%, and among women, 59.1%, with no significant difference. In the Midwest region, considering both sexes, more than 63% received both, treatment and counseling, although without statistical difference in relation to the other macro-regions. There was no difference in the proportion of CVR between those who did or did not have private health insurance, those who received or did not receive treatment and counseling, nor between educational levels and categories of race/skin color. Those who received treatment and counseling for high CVR corresponded to approximately 70.0% in the population with poor/very poor self-rated health (Figure 2).
In Table 3, the analysis is presented by the sex of people with high CVR, according to sociodemographic variables. When considering the 40 to 49 year old age group as a reference, high CVR was observed among women at 50 and 59 (PR=1.69 - 1.09;2.63), 60 to 69 (PR=3.11 - 2.06;4.69) and 70 years old or over (PR=4.61 - 95%CI 3.07;6.94); however it was higher among men at 50 to 59 (PR=2.48 - 1.29;4.75), 60 to 69 (PR=4.37 - 2.33;8.18) and 70 years old or over (PR=6.29 - 95%CI 3.41;11.62), in comparison to men aged 40-49 years. There was no difference in prevalence of high CVR according to education level, race/skin color and having private health insurance for both sexes. Men who had rated their health as poor/very poor, also had high CVR (PR=1.74 - 95%CI 1.24;2.45), in the same way as women (PR=2.04 - 95%CI 1.53;2.71), when compared to those of both sexes who self-rated their health status as fair/good/very good. The Southern region had the highest prevalence of high CVR, both for men (PR=1.72 - 95%CI 1.03;2.89) and for women (PR=1.80 - 95%CI 1.23;2.64) (Table 3).
Table 4 shows the results of the crude and adjusted analyses for people with high CVR who received both treatment and counseling, by sociodemographic variables. In the crude analysis, there was statistically significant association between high CVR and adequate case management in those aged 50-59 (PR=1.80 - 95%CI 1.08;3.01), 60- 69 (PR=2.05 - 95%CI 1.25;3,3,35) and 70 years old or over (PR=2.31 - 95%CI 1.42;3.74); and between high CVR and poor/very poor self-rated health (PRb=1.26 - 95%CI 1.05;1.53). In the multivariate model, after adjustments for all sociodemographic variables, there was no difference, according to sex, in the use of both measures. Treatment/counseling included, to a greater extent, men and women aged 50-59 (PRa=1.89 - 95%CI 1.14;3.13), 60-69 (PRa=2.28 - 95%CI 1.39;3,73) and 70 years old or over (PRa=2.56 - 95%CI 1.57;4.16), compared to those of both sexes aged 40-49 years. For those who rated their health as poor/very poor PRa was 1.26 (95%CI 1.06;1.51). The analyses did not show association between high cardiovascular risk and adequate case management - treatment/counseling - according to region, education, private health insurance or race/skin color (Table 4).
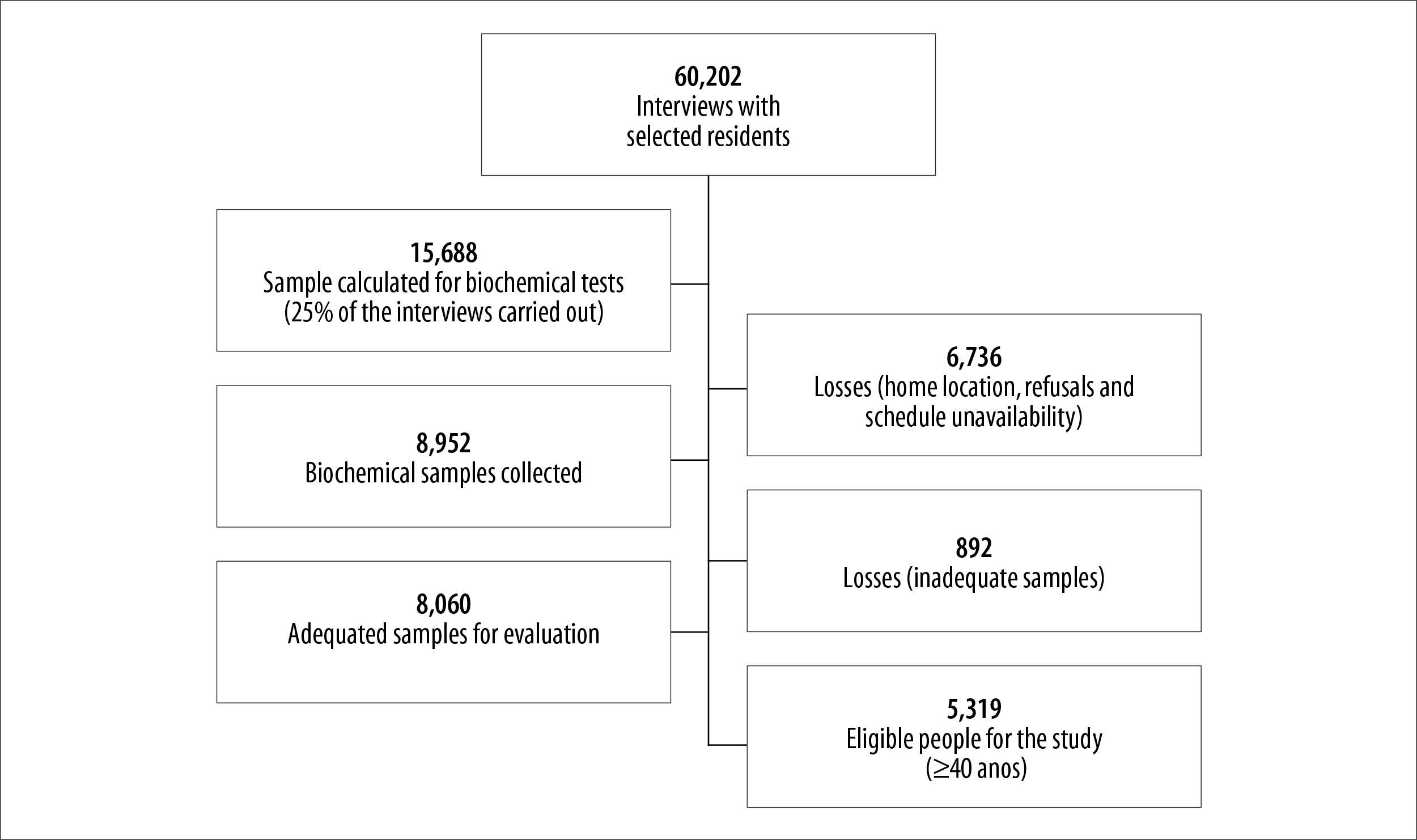
Source: National Health Survey (PNS).
Figure 1 - Sample recruitment and inclusion process of the National Health Survey, Brazil, 2014-2015
Table 1 - Prevalence of cardiovascular risk low or high, or diagnosis of cardiovascular disease according to sociodemographic variables, by sex, based on data from the National Health Survey (n = 5,319), Brazil, 2014-2015
| Variables | Women (n=3.080) | Men (n=2.239) | ||
|---|---|---|---|---|
| Low | High | Low | High | |
| % (95%CI)a | % (95%CI)a | % (95%CI)a | % (95%CI)a | |
| Total | 89.6 (88.2;90.8) | 10.4 (9.2;11.8) | 88.8 (87.1;90.4) | 11.2 (9.6;12.9) |
| Age (years) | ||||
| 40-49 | 95.7 (94.1;97.0) | 4.2 (3.0;5.9) | 96.5 (93.9;98.1) | 3.5 (1.9;6.1) |
| 50-59 | 92.4 (89.9;94.3) | 7.6 (5.7;10.1) | 90.9 (87.8;93.3) | 9.1 (6.7;12.2) |
| 60-69 | 85.6 (82.0;88.5) | 14.4 (11.5;18.0) | 83.7 (79.2;87.3) | 16.3 (12.7;20.8) |
| ≥70 | 78.0 (73.2;81.9) | 22.2 (18.1;26.8) | 75.1 (69.2;80.2) | 24.9 (19.8;30.8) |
| Education | ||||
| Incomplete elementary education | 86.6 (84.4;88.4) | 13.4 (11.6;15.6) | 86.8 (84.4;89.0) | 13.2 (11.0;15.6) |
| Complete elementary education | 92.8 (90.9;94.3) | 7.2 (5.7;9.1) | 91.1 (88.4;93.2) | 8.9 (6.8;11.6) |
| Race/skin color | ||||
| White and other | 88.8 (86.5;90.7) | 11.2 (9.3;13.5) | 87.6 (84.8;90) | 12.4 (10;15.2) |
| Black or Brown | 90.5 (88.7;92.0) | 9.5 (8.0;11.3) | 90.2 (88;92.0) | 9.8 (8.0;12.0) |
| Health insurance | ||||
| No | 88.6 (86.9;90.1) | 11.4 (9.9;13.1) | 89.0 (87;90.7) | 11.0 (9.3;13.0) |
| Yes | 91.7 (89.1;93.7) | 8.3 (6.3;10.9) | 88.4 (84.5;91.4) | 11.6 (8.6;15.5) |
| Self-rated health | ||||
| Poor/very poor | 77.7 (72.0;82.5) | 22.3 (17.5;28.0) | 77.0 (69.6;830.) | 23.0 (17.0;30.4) |
| Fair/good/very good | 91.0 (89.6;92.2) | 9.0 (7.8;10.4) | 89.8 (88.0;91.4) | 10.2 (8.6;12.0) |
| Region | ||||
| North | 92.2 (89.8;94.1) | 7.8 (5.9;10.2) | 93.3 (90.6;95.3) | 6.7 (4.7;9.4) |
| Northeast | 89.7 (87.7;91.4) | 10.3 (8.6;12.3) | 90.0 (87.6;92.0) | 10.0 (8.0;12.4) |
| Southeast | 90.9 (88.3;92.9) | 9.1 (7.1;11.7) | 88.6 (85.2;91.3) | 11.4 (8.7;14.8) |
| South | 85.1 (81.3;88.1) | 14.9 (11.9;18.7) | 85.8 (81.1;89.5) | 14.2 (10.5;18.9) |
| Midwest | 88.6 (84.8;91.6) | 11.4 (8.4;15.2) | 89.0 (84.5;92.3) | 11.0 (7.7;15.5) |
a)95%CI: 95% confidence interval.
Table 2 - Proportion of individuals with high cardiovascular risk or diagnosed with cardiovascular disease and who received counseling, drug treatment or both, by sex (n=564), based on data from the National Health Survey, Brazil, 2014-2015
| Variables | Total | Women | Men |
|---|---|---|---|
| % (95%CI)a | % (95%CI)a | % (95%CI)a | |
| Counseling | |||
| No | 31.2 (26.6;36.3) | 29.2 (23.4;35.7) | 33.5 (26.3;41.5) |
| Yes | 68.8 (63.7;73.4) | 70.8 (64.3;76.6) | 66.5 (58.5;73.7) |
| Drug treatment | |||
| No | 40.7 (36.4;46.6) | 37.0 (30.8;43.7) | 44.7 (37;52.6) |
| Yes | 59.3 (54.2;64.3) | 63.0 (56.3;69.2) | 55.3 (47.4;63.0) |
| Drug treatment and counseling | |||
| No | 44.4 (49.6;39.3) | 40.9 (34.5;47.6) | 48.2 (40.4;56.0) |
| Yes | 55.6 (50.4;60.7) | 59.1 (52.4;65.5) | 51.8 (44;59.6) |
a)95%CI: 95% confidence interval.
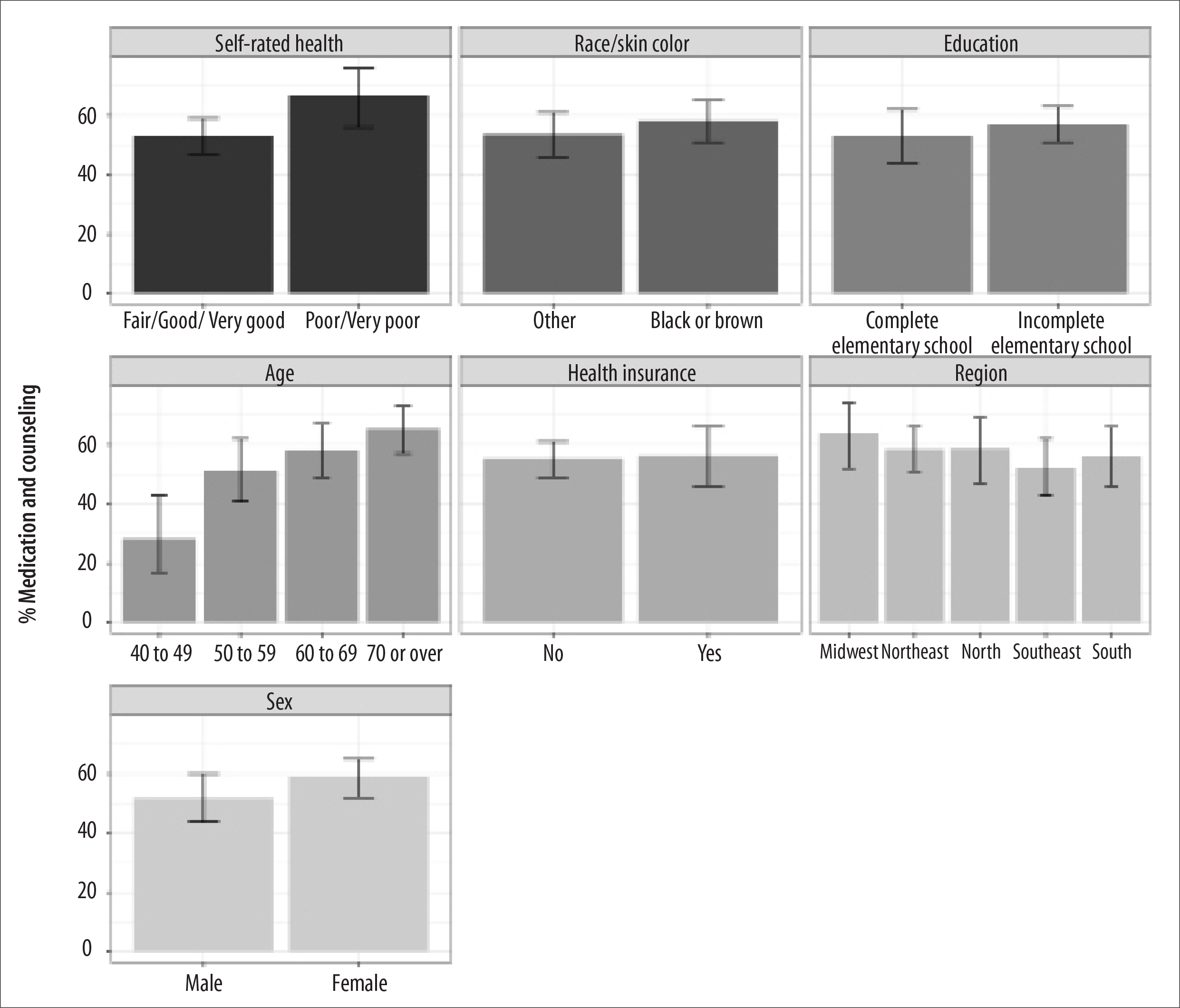
Figure 2 - Proportion of individuals at high cardiovascular risk who received treatment or counseling, according to sociodemographic variables, based on data from the National Health Survey (n=564), Brazil, 2014-2015
Table 3 - Prevalence ratio of the association between high cardiovascular risk and sociodemographic variables, by sex, based on data from the National Health Survey (n=5,319), Brazil, 2014-2015
| Variable | Women (3.080) | Men (2.059) | ||||
|---|---|---|---|---|---|---|
| PRa | 95%CIb | p-value | PRa | 95%CIb | p-value | |
| Age (years) | <0.01c | <0.01c | ||||
| 40-49 | 1.00 | - | 1.00 | - | - | |
| 50-59 | 1.69d | (1.09;2.63) | 0.02 | 2.48d | (1.29;4.75) | 0.01 |
| 60-69 | 3.11d | (2.06;4.69) | <0.01 | 4.37d | (2.33;8.18) | <0.01 |
| ≥70 | 4.61d | (3.07;6.94) | <0.01 | 6.29d | (3.41;11.62) | <0.01 |
| Education | ||||||
| Incomplete elementary education | 1.00 | - | - | 1.00 | - | - |
| Complete elementary education | 1.13 | (0.84;1.5) | 0.42 | 1.12 | (0.79;1.57) | 0.53 |
| Race/skin color | ||||||
| Black or brown | 1.00 | - | - | 1.00 | - | - |
| White and other | 1.09 | (0.83;1.42) | 0.53 | 1.13 | (0.82;1.55) | 0.46 |
| Health insurance | ||||||
| No | 1.00 | - | - | 1.00 | - | - |
| Yes | 0.8 | (0.58;1.1) | 0.17 | 1.04 | (0.73;1.47) | 0.83 |
| Self-rated health | ||||||
| Poor/very poor | 2.04d | (1.53;2.71) | <0.01 | 1.74 | (1.24;2.45) | <0.01 |
| Fair/good/very good | 1.00 | - | - | 1.00 | - | - |
| Region | <0.01c | 0.03c | ||||
| North | 1.00 | - | - | 1.00 | - | - |
| Northeast | 1.17 | (0.84;1.61) | 0.36 | 1.28 | (0.86;1.91) | 0.22 |
| Southeast | 1.12 | (0.78;1.62) | 0.54 | 1.42 | (0.91;2.2) | 0.12 |
| South | 1.80d | (1.23;2.64) | 0.00 | 1.72d | (1.03;2.89) | 0.04 |
| Midwest | 1.49d | (1.01;2.21) | 0.05 | 1.57 | (0.97;2.53) | 0.07 |
a) PR: prevalence ratio; b) 95%CI: 95% confidence interval; c) Global variable p-value; d) PR with significant value.
Note: Estimated PRs based on the Poisson model: incidence rate ratio (IRR) option.
Table 4 - Crude and adjusted prevalence ratios and 95% confidence interval of the association between high cardiovascular risk and appropriate management, according to sociodemographic variables obtained by Poisson regression (n=564), based on data from the National Health Survey, Brazil, 2014-2015
| Variable | Bivariate | Multivariate | ||||
|---|---|---|---|---|---|---|
| PRa | 95%CIb | p-value | PRa | 95%CIb | p-value | |
| Sex | ||||||
| Female | 1.14 | (0.94;1.38) | 0.17 | 1.13 | (0.95;1.35) | 0.17 |
| Male | 1.00 | - | 1.00 | - | - | |
| Age (years) | <0.01c | <0.01c | ||||
| 40-49 | 1.00 | - | - | 1.00 | - | - |
| 50-59 | 1.80d | (1.08;3.01) | 0.02 | 1.89d | (1.14;3.13) | 0.01 |
| 60-69 | 2.05d | (1.25;3.35) | <0.01 | 2.28d | (1.39;3.73) | <0.01 |
| ≥70 | 2.31d | (1.42;3.74) | <0.01 | 2.56d | (1.57;4.16) | <0.01 |
| Education | ||||||
| Incomplete elementary education | 1.00 | - | - | 1.00 | - | - |
| Complete elementary education | 0.93 | (0.76;1.15) | 0.51 | 1.17 | (0.96;1.44) | 0.12 |
| Race/skin color | ||||||
| Black or brown | 1.09 | (0.91;1.3) | 0.37 | 1.13 | (0.93;1.37) | 0.23 |
| White and other | 1.00 | - | - | 1.00 | - | - |
| Health insurance | ||||||
| No | 1.00 | - | - | 1.00 | - | - |
| Yes | 1.02 | (0.82;1.26) | 0.88 | 1.02 | (0.82;1.27) | 0.85 |
| Self-rated health | ||||||
| Poor/very poor | 1.26d | (1.05;1.53) | 0.01 | 1.26d | (1.06;1.51) | 0.01 |
| Fair/good/very good | 1.00 | - | - | 1.00 | - | - |
| Region | 0.81c | 0.40c | ||||
| North | 1.00 | - | - | 1.00 | - | - |
| Northeast | 1.00 | (0.79;1.25) | 0.97 | 0.98 | (0.78;1.21) | 0.83 |
| Southeast | 0.89 | (0.68;1.16) | 0.38 | 0.88 | (0.67;1.14) | 0.33 |
| South | 0.95 | (0.74;1.24) | 0.72 | 1.01 | (0.77;1.32) | 0.95 |
| Midwest | 1.09 | (0.84;1.41) | 0.52 | 1.06 | (0.83;1.37) | 0.64 |
a) PR: prevalence ratio; b)95% CI: 95% confidence interval; c) global variable p-value; d) PR with significant value.
Note: Estimated PRs based on the Poisson model: incidence rate ratio (IRR) option.
Discussion
For the first time, the indicator for Goal 8 of the WHO Global Action Plan for the Prevention and Control of NCDs was estimated, namely: at least half of the population with CVR >30% receiving treatment and counseling for cardiovascular disease prevention. The results show that in 2014-2015, in Brazil, the prevalence of CVR >30% was higher in men, elderly, with complete elementary schooling, white race/skin color and poor/very poor self-rated health. Among those with high CVR, more than half received treatment and counseling. Receiving treatment and counseling was associated with being 50 years old or over, and poor/very poor self-rated health.
Countries have committed to adopting and meeting the goal for treatment and counseling of people with CVR >30% with the aim of preventing diseases and reducing cardiovascular events and deaths. There is evidence that this measure is cost-effective, by directing public investment toward priority people,16 and of great relevance for planning and management in each country, in addition to serving to verify whether countries are directing efforts to reduce premature mortality due to NCDs and thus contribute to the achievement of the goal established in the 2030 Agenda for Sustainable Development, as adopted by all UN Member States.6 The present study indicates that between 2014 and 2015, Brazil achieved the goal of identifying and treating the population with high CVR, which may contribute to the reduction of mortality due to NCDs in the country.
The monitoring of actions directed towards Goal 8 for treatment of NCDs, described in this study, contributes to the monitoring of global goals for NCDs, as well as to the achievement of the goal of reducing mortality due to NCDs defined in the 2030 Agenda. WHO recognizes the importance of the commitments made by the countries, established in the Global Action Plan for the Prevention and Control of NCDs and their goals as defined in the Global Monitoring Framework, especially their policies to reduce tobacco and alcohol consumption, reduce unhealthy diet and physical inactivity, and health service response to cases of diabetes mellitus and systemic arterial hypertension.16 The inclusion of NCDs in the 2030 Agenda provides an opportunity to advance this commitment, invest in intersectoral policies and expand the regulatory agenda for tobacco and alcohol use, physical activity, healthy eating, for prevention, detection, control, treatment and rehabilitation of diseases.6
Progress in controlling NCDs occurs slowly. Studies show that to achieve the goal of reducing deaths by 30%, this reduction should be -2.7% per year. The fact is that only 35 countries have performed satisfactorily in order to achieve this goal, while more than 90 countries have reported increasing or stagnating national rates.17 Brazil had participated in the group of countries with satisfactory results for achieving the goals of reducing NCDs; however, after 2015, mortality rates stagnated and fluctuated with an increasing trend,18 this being why monitoring the goals of identification, treatment and counseling of the population with CVR is a relevant action to reduce deaths from cardiovascular diseases in the country. This study pointed out, for the first time, the initiatives carried out to achieve this goal, with its baseline drawn for the biennium 2014-2015.
Other studies indicate that the commitment taken on by member states, through the 2030 Agenda, to establish policies to reduce premature mortality from NCDs, will bring significant gains in longevity and life expectancy at the global level.19 Among the measures implemented are the organization of surveillance and monitoring of NCDs and their risk factors, prevention actions, early detection and treatment programs.5,17,18 Brazil launched its Strategic Action Plan to Combat NCDs in 2011 and instituted a set of information systems and surveys, including the PNS, by contemplating biochemical measures and anthropometric data collection, not only to allow the monitoring of NCDs and their risk factors20, but also to monitor and estimate the possibility of achieving the current goal.
This study, given its purpose of contributing to the identification of the percentage reached among the population at higher risk and directing health efforts to the target population, constitutes a cost-effective measure to be used by all countries.17,18 The NCD Task Force study compares cost in relation to effectiveness of measures to reduce NCDs, based on prevention and treatment actions. Investments of US $120 billion - or $1.5 per inhabitant/year - would be needed for signatory countries to meet the 2030 Agenda goals.17 In 20 countries, three measures to reduce mortality from NCDs were compared and all proved cost-effective, although with variations in values. Regulatory measures to restrict tobacco, salt and industrialized foods had the lowest estimated cost. Drug treatment for CVD was more costly, up to five times higher than tobacco regulatory measures and nine times higher than salt restriction measures, although cost-benefit rates were similar.17 Therefore, although treatment costs are high, they are cost-effective for populations with high CVR.
Brazil has implemented regulatory measures to curb tobacco use,20,21 measures to encourage healthy eating, and has proposed voluntary agreements to reduce sodium consumption,22,23 in addition to free access to medicines in Primary Health Care and as a co-payment initiative through the 'Brazilian Popular Pharmacy Program’.20,24,25 However, it is necessary to make these actions sustainable, and to advance with monitoring and identification of the population with high CVR.
According to the WHO, the ability of the countries to identify individuals at high cardiovascular risk and treat them is, low. Many individuals receive drug treatment based on the presence of a single CVR factor, such as high blood pressure or high cholesterol, or association between both diagnoses. It is possible that these people have received drug therapy for many years and may definitely not be a priority for these interventions.4 PNS data indicate that more than 80.0% of people with hypertension and 90.0% with diabetes have reported medication use.26,27 Low- and middle-income countries, in particular, have limited capacity to achieve the goals shown here, the challenges of which cannot be overcome with strategies restricted only to the Health sector. In Brazil, although access to medicines is universal and the list provided by Primary Health Care (PHC) and the Brazilian Popular Pharmacy includes medicines for prevention of cardiovascular diseases,28 the present study indicated out that there is still inability to identify and prioritize the population at high CVR. Research indicates high prevalence of treatment for a population with a single disease: approximately 80.0% of people with diabetes or hypertension have reported treatment 'in the last two weeks'.26,27 Certainly, this is a challenge: to identify and treat the population with high CVR.
A WHO study shows that the proportion of countries that achieved at least half of the population with CVR >30% receiving treatment and counseling was generally low all over the world: about 30% in European countries; 25% in the Western Pacific region and Eastern Mediterranean; around 10% in the Americas; and less than 3% in Africa.28 Studies indicate that the greatest risks of dying from NCDs are found in Sub-Saharan Africa and in the male populations of Central Asia and Eastern Europe.1
There were no differences in the identification and treatment of people with high CVR in relation to private health insurance, educational level or region of residence in Brazil. Previous studies of the PNS had already concluded that people with NCD, regardless of schooling and private health insurance, did not present differences in the proportion of hospitalizations due to NCDs. Differences were found, however, regarding the number of consultations and increased disabilities in the population with low education.29 Among users of the Brazilian National Health System (SUS),30 greater home care by family health strategy (FHS) teams, greater access to medicines through the Brazilian Popular Pharmacy or in primary health centers was found.25 These results show the scope of the SUS in health care for the Brazilian population, especially the low-income population.29,30
Standing out among the limitations of this study is that the biochemical study and the PNS household surveys were not simultaneous, given the long time elapsed between the questionnaire being administered and the samples being collected for testing: the interviews were conducted between 2013-2014, while the samples were collected between 2014-2015.11 There was a high proportion of losses, resulting from difficulty in locating the address and the selected resident’s refusal for their biological material to be collected, in addition to operational difficulties in transporting the material to the clinical analysis laboratory. It is worth mentioning that the losses due to the resident’s refusal may have generated greater participation of people with some preexisting disease. To minimize and correct the consequences of selection bias, post-stratification methods were used based on the total PNS sample.11 It should also be emphasized that the information on the use of medicines was self-reported by the participants, and that the questions about medications included in the PNS questionnaire were generic, such as [...] have you used medications to treat hypertension? diabetes mellitus?, without the medications being specified.
In 2019, a new proposal for the analysis of CVR was published by WHO. Nevertheless, the authors of this study opted for the previous recommendation that had been published in 2007,12 considering that it has been widely used by the WHO since 2015 to assess which member countries have reached the goal of at least 50% of people with high CVR receiving treatment and counseling, as defined in the Global Action Plan for NCDs. It is worth mentioning that this goal had never been calculated in the Brazilian context.
Therefore, it is recommended that CVR be monitored in an integrated way, with priority for the treatment of people who require greater health service care.10 Thus, this recommendation implies the due review of primary health care practices in Brazil, given that this study found that just over half of the population analyzed and with high CVR received treatment and counseling. Although the WHO goal was reached, including above the performance of most countries,1 the PNS data, the calculations performed and their results are very worrying.
Taking these results, it could be concluded that about half of the people with CVR >30% received treatment and counseling measures, evidencing the achievement of Goal 8 of the Global Action Plan for the Prevention and Control of NCDs in Brazil. It is worth emphasizing that there was no association between receiving treatment and schooling, having private health insurance, race/skin color or macro-region of residence in the country.
Finally, it is worth mentioning that addressing cardiovascular diseases requires an intersectoral response, and efforts to identify people and populations with high CVR, these being priorities for the prevention of these diseases through the provision of counseling and treatment. Identifying populations with high cardiovascular risk and having therapeutic measures available to them may contribute to achieving the goals established by the 2030 Agenda for Sustainable Development, defined by the United Nations, especially the 30% reduction in premature mortality from chronic non-communicable diseases.
REFERENCES
1. World Health Organization. Noncommunicable diseases country profiles 2018. Geneva: WHO; 2018 [citado 22 jan.2021]. Disponível em:Disponível em:https://apps.who.int/iris/handle/10665/274512 . [ Links ]
2. Souza MFM, Malta DC, França EB, Barreto ML. Transição da saúde e da doença no Brasil e nas unidades federadas durante os 30 anos do Sistema Único de Saúde. Cienc Saude Colet. 2018;23(6):1737-50. doi: 10.1590/1413-81232018236.04822018. [ Links ]
3. Harper S, Lynch J, Smith GD. Social determinants and the decline of cardiovascular diseases: understanding the links. Annu Rev Public Health. 2011;32:39-69. doi: 10.1146/annurev-publhealth-031210-101234. [ Links ]
4. World Health Organization. Global NCD target prevent heart attacks and strokes through drug therapy and counselling. Geneva: WHO; 2016 [citado em 22 jan. 2021]. Disponível em: Disponível em: https://www.who.int/beat-ncds/take-action/policy-brief-drug-theraphy.pdf . [ Links ]
5. World Health Organization. Global action plan for the prevention and control of noncommunicable diseases 2013-2020. Geneva:WHO; 2013 [citado 22 jan. 2021]. Disponível em: Disponível em: http://apps.who.int/iris/bitstream/10665/94384/1/9789241506236_eng.pdf . [ Links ]
6. Organização das Nações Unidas Brasil. Transformando nosso mundo: a agenda 2030 para o desenvolvimento sustentável. [citado 15 fev. 2020]. Disponível em: Disponível em: https://nacoesunidas.org/pos2015/ . [ Links ]
7. Szwarcwald CL, Malta DC, Pereira CA, Vieira MLFP, Conde WL, Souza Júnior PRB, et al. Pesquisa nacional de saúde no Brasil: concepção e metodologia de aplicação. Cienc Saude Colet. 2014;19(2):333-42. doi: 10.1590/1413-81232014192.14072012. [ Links ]
8. Malta DC, Szwarcwald CL, Silva Júnior JB. Primeiros resultados da análise do laboratório da pesquisa nacional de saúde. Rev Bras Epidemiol. 2019;22(Supl 2):e190001.Supl.2. doi: 10.1590/1980-549720190001.supl.2. [ Links ]
9. Malta DC, Duncan BB, Schmidt MI, Machado IE, Silva AG, Bernal RTI, et al. Prevalência de diabetes mellitus determinada pela hemoglobina glicada na população adulta brasileira, pesquisa nacional de saúde. Rev Bras Epidemiol. 2019;22(Suppl 2):e190006.Supl 2. doi.org/10.1590/1980-549720190006.supl.2. [ Links ]
10. Malta DC, Szwarcwald CL, Machado IE, Pereira CA, Figueiredo AW, Sá ACMG, et al. Prevalência de colesterol total e frações alterados na população adulta brasileira: pesquisa nacional de saúde. Rev Bras Epidemiol. 2019;22(Supl 2):e190005.Supl.2. doi: 10.1590/1980-549720190005.supl.2. [ Links ]
11. Szwarcwald CL, Malta DC, Souza Júnior PRB, Almeida WS, Damacena GN, Pereira CA, et al. Exames laboratoriais da Pesquisa Nacional de Saúde: metodologia de amostragem, coleta e análise dos dados. Rev Bras Epidemiol. 2019;22(Supl2.):e190004.Supl.2. doi: 10.1590/1980-549720190004.supl.2. [ Links ]
12. World Health Organization. Noncommunicable diseases global monitoring framework: indicator definitions and specifications. Geneva: WHO; 2014 [citado 22 jan. 2021]. Disponível em: Disponível em: https://www.who.int/nmh/ncd-tools/indicators/GMF_Indicator_Definitions_Version_NOV2014.pdf . [ Links ]
13. World Health Organization. WHO/ISH risk prediction charts. Geneva: WHO; 2007 [citado 22 jan. 2021]. Disponível em: Disponível em: http://www.who.int/cardiovascular_diseases/guidelines/PocketGL.ENGLISH.AFR-D-E.rev1.pdf [ Links ]
14. Malta DC, Santos NB, Perillo RD, Szwarcwald CL. Prevalence of high blood pressure measured in the Brazilian population, national health survey, 2013. Sao Paulo Med J. 2016;134(2):163-70. doi: 10.1590/1516-3180.2015.02090911. [ Links ]
15. Thompson ML, Myers JE, Kriebel D. Prevalence odds ratio or prevalence ratio in the analysis of cross-sectional data: what is to be done? Occup Environ Med. 1998;55(4):272-7. doi: 10.1136/oem.55.4.272. [ Links ]
16. World Health Organization. “Best Buys” tackling NCDs: best buys and other recommended interventions for the prevention and control of noncommunicable diseases. Geneva: WHO; 2017 [citado 22 jan. 2021]. Disponível em: Disponível em: https://www.who.int/ncds/management/WHO_Appendix_BestBuys.pdf . [ Links ]
17. Bertram MY, Sweeny K, Lauer JA, Chisholm D, Sheehan P, Rasmussen B, et al. Investing in non-communicable diseases: an estimation of the return on investment for prevention and treatment services. Lancet. 2018 May 19;391(10134):P2071-8. doi: 10.1016/S0140-6736(18)30665-2. [ Links ]
18. NCD Countdown 2030 collaborators. NCD Countdown 2030: worldwide trends in non-communicable disease mortality and progress towards Sustainable Development Goal target 3.4. Lancet 2018 Sept 22;392(10152):P1072-88. doi: 10.1016/S0140-6736(18)31992-5. [ Links ]
19. Cao B, Bray F, Ilbawi A, Soerjomataram I. Effect on longevity of one-third reduction in premature mortality from non-communicable diseases by 2030: a global analysis of the Sustainable Development Goal health target. Lancet Glob Health. 2018;6(12):e1288-e12296. doi: 10.1590/1980-5497201700040009. [ Links ]
20. Malta DC, Silva MMA, Moura L, Morais Neto OL. A implantação do Sistema de Vigilância de Doenças Crônicas Não Transmissíveis no Brasil, 2003 a 2015: alcances e desafios. Rev Bras Epidemiol. 2017;20(4):661-75. doi: 10.1590/1980-5497201700040009. [ Links ]
21. Malta DC, Silva AG, Machado IE, Sá ACMGN, Santos FM, Prates EJS, et al. Tendências de indicadores relacionados ao tabagismo nas capitais brasileiras entre os anos de 2006 e 2017. J Bras Pneumol. 2019;45(5):e20180384. doi: 10.1590/1806-3713/e20180384. [ Links ]
22. Ministério da Saúde (BR). Guia alimentar para a população brasileira. MS; 2014 [citado 22 jan.2021]. Disponível em: Disponível em: https://bvsms.saude.gov.br/bvs/publicacoes/guia_alimentar_populacao_brasileira_2ed.pdf . [ Links ]
23. Jaime PC, Delmuè DCC, Campello T, Silva DO, Santos LMP. A look at the food and nutrition agenda over thirty years of the unified health system. Cienc Saude Colet. 2018;23(6):1829-36. doi: 10.1590/1413-81232018236.05392018. [ Links ]
24. Malta DC, Morais NOL, Silva MMA, Rocha D, Castro AM, Reis AAC, et al. Política Nacional de Promoção da Saúde (PNPS): capítulos de uma caminhada ainda em construção. Cienc Saude Colet. 2016;21(6):1683-94. doi: 10.1590/1413-81232015216.07572016. [ Links ]
25. Costa KS, Tavares NUL, Mengue SS, Pereira MA, Malta DC, Silva JJB. Obtenção de medicamentos para hipertensão e diabetes no Programa Farmácia Popular do Brasil: resultados da pesquisa nacional de saúde, 2013. Epidemiol Serv Saude. 2016;25(1):33-44. doi: 10.5123/s167949742016000100004. [ Links ]
26. Malta DEC, Stopa SR, Andrade SSCA, Szwarcwald CL, Silva Júnior JB, Reis AAC. Cuidado em saúde em adultos com hipertensão arterial autorreferida no Brasil segundo dados da pesquisa nacional de saúde, 2013. Rev Bras Epidemiol. 2015;18(Supl 2):109-22. doi: 10.1590/1980-5497201500060010. [ Links ]
27. Malta DC, Iser BPM, Chueiri PS, Stopa SR, Szwarcwald CL, Schmidt MI, et al. Cuidados em saúde entre portadores de diabetes mellitus autorreferido no Brasil, pesquisa nacional de saúde, 2013. Rev Bras Epidemiol. 2015;18(Supl 2):17-32. doi: 10.1590/1980-5497201500060003. [ Links ]
28. World Health Organization. Assessing national capacity for the prevention and control of noncommunicable diseases: report of the 2017 global survey. Geneva: WHO; 2017 [citado 22 jan. 2021]. https://apps.who.int/iris/bitstream/handle/10665/276609/9789241514781eng.pdf . [ Links ]
29. Malta DC, Bernal RTI, Lima MG, Araújo SSC, Silva MMA, Freitas MIF, et al. Doenças crônicas não transmissíveis e a utilização de serviços de saúde: análise da pesquisa nacional de saúde no Brasil. Rev Saude Publica. 2017;51(Supl 1):4s. doi: 10.1590/s1518-8787.2017051000090. [ Links ]
30. Stopa SR, Malta DC, Monteiro CN, Szwarcwald CL, Goldbaum M, Cesar CLG. Acesso e uso de serviços de saúde pela população brasileira, pesquisa nacional de saúde 2013. Rev Saude Publica. 2017;51(Supl 1):3s. doi: 10.1590/s1518-8787.2017051000074. [ Links ]
*Deborah Carvalho Malta receives a productivity scholarship from the National Council for Scientific and Technological Development/Ministry of Science, Technology and Innovation (CNPq/MCTI); Fabiana Martins Dias de Andrade receives a PhD scholarship from the Coordination for the Improvement of Higher Education Personnel/Ministry of Education (CAPES/MEC). The study received support from the Health Surveillance Secretariat of the Ministry of Health (SVS/MS): TED Process No. 147/2018.
Received: June 14, 2020; Accepted: November 20, 2020











 texto en
texto en 


