Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Revista Pan-Amazônica de Saúde
versão impressa ISSN 2176-6215versão On-line ISSN 2176-6223
Rev Pan-Amaz Saude v.2 n.1 Ananindeua mar. 2011
http://dx.doi.org/10.5123/S2176-62232011000100010
REVIEW ARTICLE
Ventilatory support in the treatment of Influenza A H1N1 in an intensive care unit
Soanne Chyara da Silva SoaresI; Lila Teixeira de Araújo JanahúII
ICentro Universitário do Pará, Belém, Pará, Brasil
IIEscola Superior da Amazônia, Belém, Pará, Brasil
Endereço para correspondência
Correspondence
Dirección para correspondencia
ABSTRACT
The pandemic caused by the virus Influenza A H1N1 has challenged health agents in intensive care units because of the early respiratory complications that jeopardize the patients' medical prognosis. Dealing with the influenza of this new century constitutes a major challenge nowadays. This study aims to perform a literature review on ventilatory support indicated for the treatment of influenza A H1N1 in intensive care units. Morbidity and mortality of any disease are associated with its severity. In the case of influenza A H1N1, they depend on aspects related to the emergence of new strains, the hosts, the delay in making the correct diagnosis and treating the disease adequately, and the mistaken identification of its possible complications. Common complications are: acute respiratory failure, acute respiratory distress syndrome and sepsis. As acute respiratory failure is observed, initial ventilatory support can be performed through non-invasive oxygen therapy with values <5L/min. If no clinical improvement is observed, the disease can evolve rapidly to acute respiratory distress syndrome and sepsis. In this case, continuity of any type of noninvasive mechanical ventilation is contraindicated, intubation and invasive mechanical ventilation must be started, and protective ventilation is the recommended procedure.
Keywords: Influenza A Virus, H1N1 Subtype; Respiration, Artificial; Intensive Care Units; Respiratory Insufficiency; Respiratory Distress Syndrome, Adult; Influenza, Human.
INTRODUCTION
A widespread influenza A H1N1 pandemic began in 2009, and by April 2010, at least 17,483 deaths had been reported worldwide. The World Health Organization (WHO) classified the pandemic as alert level 6 to reflect the need to prevent this new variety of influenza1. This variety is considered new because there were other waves of epidemics during the 20th century. The H1N1 Spanish flu (1918-1919) affected 50% of the world's population and killed 20 to 50 million people; influenza A H2N2 (19571958) caused 70 deaths in the USA; and influenza A H3N2, which appeared in 1968, killed 1 to 4 million people2,3.
In Brazil, 46,100 cases had been reported by February 2010. In total, 2,051 of those patients died, and 75% of them developed chronic illnesses4.
According to the Brazilian Health Ministry, influenza A H1N1 is characterized by mild illness with low lethality. In 2010 the WHO classified countries as "without any occurrence of cases", "in transition", or "with sustained transmission". Brazil was included in the last category4.
The influenza A H1N1 virus may have undergone genetic recombination and could generate new waves of epidemics in the future with different virulence rates. If these changes have in fact occurred, the demand for outpatient and hospital assistance might increase in response to increases in both the severity of the disease and the number of deaths5. To deal with this possibility, health-care professionals must be aware of their role and the pertinent interventions at all levels of health-care assistance.
The current challenge is to determine the appropriate way to treat this new flu. Many studies have been devoted to influenza A H1N1 in high-complexity health care settings because the advances in intensive care have made it possible to reduce its mortality rates.
OBJECTIVE
The objective of this study is to perform a literature review on the treatment of influenza A H1N1 with ventilatory support in Intensive Care Units (ICUs).
MATERIAL AND METHODS
This is a systematic review of literature that covers the appropriate ventilatory support for the treatment of influenza A H1N1 in ICUs through a survey of scientific articles from the following resources: Public Medline (PUBMED), the Latin-American and Caribbean Center of Information on Health Sciences (BIREME-Regional Library of Medicine/PAHO/WHO), Latin-American and Caribbean Literature on Health Sciences (LILACS), Medical Literature Analysis and Retrieval System Online (MEDLINE), Brazil's Ministry of Health, and corresponding books. The following search terms were used: influenza A H1N1, intensive care unit, acute respiratory failure, and acute respiratory distress syndrome.
DISCUSSION
MORBIDITY AND MORTALITY
Influenza is a disease that causes morbidity and mortality worldwide. Its pathogenesis is directly related to airway and lung infection after contact with infected respiratory secretions from coughing, sneezing, or other means5. The most common signs and symptoms are described in table 1.
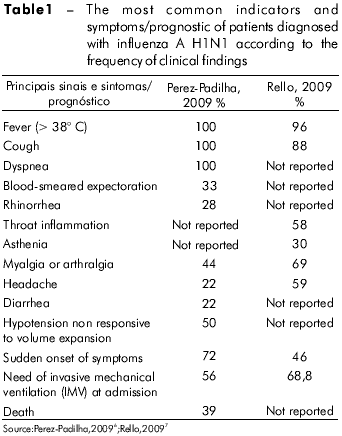
The severity of influenza illness depends on several factors, such as the virulence of the agent, characteristics inherent to the host, delays in diagnosis and, consequently, in treatment, and misidentification of possible complications2.
The following groups and individuals with pre-existing health conditions are at a higher risk for influenza A H1N1 infection: indigenous people, pregnant women, children younger than 2 years old, elderly individuals over 60 years old, immunosuppressed individuals (due to organ transplant, leukemia, neoplasia, chemotherapy, or AIDS), and patients with chronic diseases (chronic kidney failure, diabetes, cardiovascular diseases, obesity, or liver disease)2,5.
PRIMARY COMPLICATIONS
The disease severity and mortality are directly related to the complications associated with influenza A H1N1 infection. The primary complications are directly associated with the body's response to infection with the influenza virus and can range from mild to systemic and severe, including sepsis. Respiratory complications, such as acute respiratory failure (ARF), might appear at the onset of the disease and quickly progress to acute respiratory distress syndrome (ARDS). Therefore, admission to the ICU is indicated for any acute organ dysfunction related to the flu in combination with respiratory distress2.
ACUTE RESPIRATORY FAILURE
The influenza virus can damage the parenchyma of the lungs, leading to hypoxemic forms of ARF with tachycardia, dyspnea, tachypnea, and sometimes cyanosis, which can lead to stupor8,9. The initial symptoms typically cause patients to seek assistance in outpatient facilities, which then refer them to hospitals where more accurate tests can be performed.
ARF can be diagnosed based on clinical symptoms and gasometrical tests that indicate a PO2<60 mmHg or a PCO2>50 mmHg9,10. Once ARF is diagnosed, a multidisciplinary health-care team should monitor the clinical signs and administer increasingly higher oxygen concentrations until the patient's oxygen saturation level is higher than 90%2.
Non-invasive mechanical ventilation (NIMV) is a therapeutic approach for ventilatory support that can be employed to improve gas exchange and decrease the probability of secondary complications associated with invasive techniques11. In patients with ARF of unknown etiology, NIMV can be used to correct hypoxemia by means of CPAP (continuous positive airway pressure), PEEP (positive end-expiratory pressure), and alveolar recruitment maneuvers12.
If the patient with H1N1 does not improve after oxygen therapy (oxygen supplementation greater than 5 L/min to maintain an oxygen saturation level greater than 90%), NIMV is contraindicated; misguided use might worsen the prognosis because this disease is known to progress quickly from ARF to ARDS, which is a serious condition requiring intensive care. In addition to respiratory complications, attention must be paid to cardiovascular complications such as arterial hypotension, which, together with other symptoms, might lead to shock. At this point, the importance of monitoring the patient is clear because if the patient does not improve, intubation and invasive mechanical ventilation must begin immediately. Therefore, it should be stressed that NIMV is contraindicated for patients that are diagnosed with or are suspected to have H1N12.
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS)
ARDS is a serious disease that initially presents as an acute lung lesion and is characterized by diffuse alveolar damage due to non-cardiogenic pulmonary edema arising from an increase in the permeability of the alveolar-capillary membrane of the lung. Diffuse pulmonary infection is a factor that directly predisposes patients to ARDS, whereas sepsis indirectly predisposes patients to ARDS9,12,13,14.
Despite intense research on ARDS, the mortality rates remain high. reaching approximately 30% to 40% and, in some instances, 60% to 80%11.
To diagnose ARDS associated with influenza A H1N1, the following criteria must be fulfilled: acute onset of lung affection (1 to 3 days), bilateral lung radiological infiltrate consistent with non-cardiogenic pulmonary edema14, PAO2/FiO2 of less than 200, capillary pressure of less than 18 mmHg, lack of left ventricle dysfunction on either clinical or echocardiographic examination2,9,11,13. It is worth stressing that interstitial and alveolar edema and alveolar collapse cause alterations in pulmonary compliance, and high inspiratory pressure is then required to open the collapsed alveoli9,11.
After the diagnosis worsens from ARF to ARDS, invasive mechanical ventilation (IMV) must be started immediately. The literature indicates that the ventilator parameters in these patients must correspond to a protective ventilation pattern (low tidal volume of approximately 6 mL/Kg) that restricts airway pressure to less than 35 cmH2O. PEEP can be adjusted to approximately 10 cmH2O or by titration of 2 cmH2O from the inflection point of the respiratory system pressure-volume curve. Combined with other modalities of intensive care, a protective ventilation strategy reduces the mortality rate by approximately 30% to 40%12.
SEPSIS
Another complication of influenza A H1N1 is sepsis, which is one of the most severe manifestations. The clinical and immunopathogenic features of sepsis amplify the initial damage. Thus, early diagnosis and treatment are crucial to achieve a satisfactory outcome5. The intensity of the inflammatory response and the severity of organ dysfunction define the clinical manifestations of sepsis. Several organs/systems might be affected by sepsis, including the central nervous system (e.g., septic encephalopathy), the lungs (e.g. ARDS), the kidneys (e.g., acute renal failure), the gastrointestinal system (e.g. organ ischemia), the cardiovascular system (arterial hypotension), and others12.
As a rule, patients with sepsis generally exhibit multiple organ failure. In a study by Rello7, 75% of infl uenza A H1N1 patients developed sepsis. Nevertheless, it is worth noting that progression to this level is often because of comorbidities or other factors (obesity, diabetes, or pregnancy).
Antimicrobial drugs must be started immediately to treat sepsis, and well-established guidelines must be followed to limit damage to microcirculation. This approach, together with protective ventilation, minimizes further damage to the functional units of the lungs. Therefore, ventilatory support should be started as it would be for ARDS because the two conditions are usually associated12.
EVIDENCE ON VENTILATORY SUPPORT
According to the Consenso Brasileiro de Ventilação Mecânica (Brazilian Consensus on Mechanical Ventilation), ventilatory support aims to maintain a sufficient degree of gas exchange and avoid lung damage associated with ventilation13.
Several authors have published case reports that establish how to clinically manage and initiate ventilatory support for influenza A H1N1 patients. Yokoyama15 reported the case of a 44-year-old obese female patient who was diagnosed with influenza A H1N1 and manifested signs of ARF. The patient was initially started on oxygen therapy. Due to her clinical progression, she was transferred to the ICU, where she was subjected to non-invasive ventilatory support (BIPAP and CPAP). According to Yokoyama, the progressive improvement in this patient was due to drug therapy (olsetamivir), but no data was reported regarding the patient's response to NIMV. However, this may be an isolated case because other literature reports discourage the use of NIMV in these patients to avoid respiratory complications and progression to ARDS2. Patients subjected to NIVM improved only temporarily and have a reduced respiratory effort; however, all of these patients required intubation and IMV because NIVM does not hinder progression to ARDS16.
Rello demonstrated that 68.8% of patients with influenza A HIN1 infection need invasive ventilatory support, which supports the findings of Perez-Padilha, who reported a rate of 55.5%. In the Rello study, 41.17% of the patients exhibited complications such as ARDS. Additionally, the PaO2/FIO2 ratio average was 164 and 53 after IMV in the surviving and non-surviving groups, respectively. None of the previous studies discuss the ventilator modes and modalities used6,7. However, the Consenso Brasileiro de Ventilação Mecânica recommends ventilation modes with limited pressure and a decreasing flow wave because it provides better distribution of air in the lungs, generates lower airway pressure levels, and reduces respiratory effort. Special attention must be paid to tidal volume because it is not ensured by this ventilator mode13.
Respiratory failure is quite common in rapidly progressing influenza A H1N1, and 10% to 30% of patients require intensive care3. IVM is complex in these patients and requires specialized knowledge and equipment. Kaufman reported six case studies on this disease and found that low tidal volume (6 mL/Kg ideal body weight) and a high PEEP (15-20 cmH2O) and pressure-limited ventilator mode must be applied, which supports the Consenso Brasileiro de Ventilação Mecânica13.
Protective mechanical ventilation (volume controlled; TV 6 mL/Kg; Pplateau ≤ 30 cmH2O; BR: 6-35 ipm/min; I:E = 1:1 - 1:3) improves survival rates, has fewer complications, requires a shorter duration of MV, and reduces the mortality by approximately 34% to 58% in ARDS patients compared to conventional ventilation (volume controlled; TV 12 mL/Kg; Pplateau ≤ 50 cmH2O; BR: 6 - 35 ipm/min)3,17,18.
Alveolar recruitment maneuvers were reported to be crucial for improving ventilation in ARDS patients. Previous studies have indicated that procedures employing progressive PEEP and 15 cmH2O inspiratory pressure delta might be required to maintain proper function of the alveolar units. Time since disease onset also influences treatment success; the earlier treatment is started, the higher the odds of success13,18.
The efficiency of conventional IMV is not sufficient for ARDS patients because acceptable clinical standards are difficult to maintain even in combination with other strategies such as ventilation in the prone position, high-frequency ventilation (HFV), or supplementation with nitric oxide. Extracorporeal membrane oxygenation was shown to be more appropriate for treatment of ARDS because it improves survival by up to 71%. However, this finding should not discourage the use of other therapeutic approaches in clinical practice19,20.
CONCLUSION
We conclude that patients with influenza A H1N1 exhibit frequent respiratory complications. These respiratory complications require ventilatory support and oxygen therapy during acute respiratory failure, whereas invasive mechanical ventilation and protective ventilation are indicated for the treatment of acute respiratory distress syndrome and sepsis.
REFERENCES
1 World Health Organization. Global Alert and Response. Pandemic H1N1 2009. Pandemic H1N1 update 2009 [monography on the Internet]. 2010 May. Available from: http://www.who.int/csr/disease/swineflu/en/index.html
2 Associação de Medicina Intensiva Brasileira. Abordagem racional dos pacientes adultos com complicações decorrentes da nova gripe-H1N1 admitidos em unidades de terapia intensiva. São Paulo: AMIB; 2009. 7 p. [Link]
3 Hui DS, Lee N, Chan PKS. Clinical management of pandemic 2009 Influenza A(H1N1) infection. Chest [Internet]. 2009 Dec [cited 2010 Apr 21];137;916-25. Available from: http://chestjournal.chestpubs.org/content/137/4/916.full.html
4 Ministério da Saúde (BR). Secretaria de Vigilância Sanitária. Emergência de Saúde Pública de Importância Internacional. Protocolo de manejo clínico de síndrome respiratória aguda grave – SRAG [Internet]. 2010 maio [citado 2010 maio 05]. Dísponivel em: http://portal.saude.gov.br/portal/arquivos/pdf/protocolo_manejo_influenza_22_04.pdf
5 Ministério da Saúde (BR). Secretaria de Vigilância Sanitária. Emergência de Saúde Pública de Importância Internacional. Protocolo para o enfrenta mento à pandemia de influenza pandêmica H1N1 2009: ações da atenção primária à saúde [Internet]. 2010 maio [citado 2010 maio 05]. Disponível em: http://portal.saude.gov.br/portal/arquivos/pdf/protocolo_atencao_basica_25_03_10.pdf
6 Perez-Padilla R, Zamboni DR, Ponce LS. Working Group on Influenza. Pneumonia and respiratory failure from swine-origin influenza A H1N1 in Mexico. N Engl J Med [Internet]. 2009 Aug [cited 2010 Apr 21];361:680–9. Available from: [PubMed: 19564631]
7 Rello J, Rodríguez A, Ibañez P. Intensive care adult patients with severe respiratory failure caused by Influenza A H1N1v in Spain. Crit Care [Internet]. 2009 Sep [cited 2010 Apr 21]; 13(5):148. Available from: http://ccforum.com/content/13/5/R148
8 Auler Junior JOC, Amaral RVG. Assistência ventilatória mecânica. São Paulo: Atheneu; 2006. 472 p.
9 West JB. Fisiopatologia pulmonar moderna. 6. ed. São Paulo: Manole; 2004. 214 p.
10 Machado MGR. Bases da fisioterapia respiratória: terapia intensiva e reabilitação. Rio de Janeiro: Guanabara Koogan; 2008. 555 p.
11 Nery lE, Fernandes ALG, Perfeito JAJ, organizadores. Guias de medicina ambulatorial e hospitalar da UNIFESP: pneumologia. São Paulo: Manole; 2006. 756 p.
12 Knobel E. Condutas no paciente grave. 3. ed. São Paulo: Atheneu; 2006. 1628 p.
13 Amato MBP, Carvalho CRR, Ísola A, Vieira S, Rotman V, Moock M, et al. Ventilação mecânica na Lesão Pulmonar Aguda (LPA)/Síndrome do Desconforto Respiratório Agudo (SDRA ). J Bras Pneumol. 2007;33 Suppl 2:S119-27. [Link]
14 Mollura DJ, Asnis DS, Crupi RS, Conetta R, Feigin DS, Bray M, et al. Imaging Findings in a Fatal Case of Pandemic Swine-Origin Influenza A H1N1. AJR Am J Roentgenol [Internet]. 2009 Dec [cited 2010 Apr 21];193(6):1486-7. Available from: http://www.ajronline.org/cgi/content/full/193/6/1500
15 Yokoyama T, Tsushima K, Ushiki A, Kobayashi N, Urushihata K, Koizumi T, et al. Acute lung injury with alveolar hemorrhage due to a novel swine-origin influenza A (H1N1) virus. Intern Med [Internet]. 2010 Nov [cited 2009 Apr 21];49(5):427-30. Available from: http://pesquisa.bvsalud.org/h1n1/resources/resources/mdl-20190477
16 Kaufman MA, Duke GJ, McGain F, French C, Aboltins C, Lane G, et al. Life-threatening respiratory failure from H1N1 influenza 09 (human swine influenza). Med J Aust [Internet]. 2009 Aug [cited 2010 Apr 21];191(3):154-6. Available from: http://www.ncbi.nlm.nih.gov/pubmed/19645645?dopt=Abstract
17 The Acute Respiratory Distress Syndrome Network. Ventilation with Lower Tidal Volumes as Compared with Traditional Tidal Volumes for Acute Lung Injury and the Acute Respiratory Distress Syndrome. N Engl J Med [Internet]. 2000 May [cited 2010 Apr 29];342:1301-8. Available from: http://content.nejm.org/cgi/content/full/342/18/1301
18 Fan E, Wilcox ME, Brower RG, Stewart TE, Metha S, Lapinsky SE, et al. Recruitment Manuevers for Acute Lung Injury: systematic Review. Am J Respir Crit Care Med [Internet]. 2008 Sep [cited 2010 Apr 21];178:1156-63. Available from: http://ajrccm.atsjournals.org/cgi/pmidlookup?view=long&pmid=18776154
19 Hubmayr RD, Farmer JC. Shoud we "rescue" patients with 2009 influenza A H1N1 and lung injury from conventional mechanical ventilation? Chest [Internet]. 2010 May [cited 2010 May 3];137(4):745-7. Available from: http://chestjournal.chestpubs.org/content/137/4/745.full.html
20 Grasselli G, Foti G, Patroniti N, Giuffrida A, Cortinovis B, Zanella A, et al. A case of ARDS associated with influenza A - H1N1 infection treated with extracorporeal respiratory support. Minerva Anestesiol [Internet]. 2009 Dec [cited 2010 Apr 21];75(12):741-5. Available from: [PubMed 19940827]
 Correspondência / Correspondence / Correspondencia:
Correspondência / Correspondence / Correspondencia:
Soanne Chyara da Silva Soares
Endereço- Tv. 14 de Abril, 1186, Apto: 311,
Belém- PA- Brasil,
CEP:66063-140.
Tel: 091-3249-9592.
Email:soanne_chyara@yahoo.com.br
Recebido em / Received / Recibido en: 23/6/2010
Aceito em / Accepted / Aceito en: 6/4/2011











 texto em
texto em 

