Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Revista Pan-Amazônica de Saúde
versão impressa ISSN 2176-6215versão On-line ISSN 2176-6223
Rev Pan-Amaz Saude v.2 n.3 Ananindeua set. 2011
http://dx.doi.org/10.5123/S2176-62232011000300002
ORIGINAL ARTICLE |ARTIGO ORIGINAL | ARTÍCULO ORIGINAL
Antidepressant use, pain severity and pain at multiple sites in patients with bruxism
Uso de antidepressivos, intensidade da dor e dor em locais múltiplos em pacientes com bruxismo
Uso de antidepresivos, intensidad del dolor y dolor en multiples locales en pacientes con bruxismo
Omar Franklin MolinaI; Zeila Coelho SantosI; Rise Consolação luata RankI; Bruno Ricardo Huber SimiãoII; Nayene Leocádia Manzutti EidII; Marcelo Bressan CorrêaIII; Karla Regina GamaIV
IFaculdade de Odontologia, Dor Orofacial e Odontopediatria, Centro Universitário UnirG, Gurupi, Tocantins, Brasil
IIFaculdade de Odontologia, Departamento de Prótese Dental e Clinica, Centro Universitário UnirG, Gurupi, Tocantins, Brasil
IIIDepartamento de Prótese e Implantes, Instituto Tocantinense Presidente Antônio Carlos, Araguaína, Tocantins, Brasil
IVDepartamento de Odontologia Clinica UNIRG, Gurupi, Tocantins, Brasil
Endereço para correspondência
Correspondence
Dirección para correspondencia
ABSTRACT
OBJECTIVE: The aim of this study was to compare the duration, pain severity, painful complaints and antidepressant use in patients with craniomandibular disorders (CMDs) and bruxing and control subjects.
MATERIAL AND METHODS: Clinical evaluation, questionnaires for pain, bruxism and antidepressant use, self-report of signs and symptoms and history regarding pain and muscle palpation were used to evaluate 389 patients presenting with CMDs and bruxing behavior and 69 controls.
RESULTS: The mean age of the experimental group was 33.3 years. The duration of the chief complaint was not different in the bruxism and CMD patients (Kruskal-Wallis test p = 0.13, which is non-significant). Severe pain was more frequently observed in the severe bruxing behavior subgroup (Chi-squared test for trends p = 0.01, significant). Patients with severe bruxism had used or were using more antidepressants than patients with mild or moderate bruxism and non-CMD control subjects (Chi-squared test for independence p = 0.006, significant). A greater number of pain complaints was observed in the severe bruxing behavior group (Kruskal-Wallis test p = 0.0001, extremely significant).
CONCLUSIONS: Patients with severe bruxism presented with a history of pain. Antidepressant use increased from the mild to the severe bruxing behavior group. In addition, the severe group demonstrated a greater number of painful complaints.
Keywords: Temporomandibular joint disorders; Bruxism; Facial pain; Antidepressant agents.
RESUMO
OBJETIVOS: Comparar a duração, a severidade da dor, sua ocorrência em locais múltiplos e o uso de antidepressivos por pacientes com distúrbios craniomandibulares (DCMs) e bruxismo com indivíduos de um grupo controle.
MATERIAIS E MÉTODOS: Avaliação clínica; questionários sobre dor, bruxismo e uso de antidepressivos; autorrelato de sinais e sintomas; e histórico relacionado à dor e palpação muscular em 389 indivíduos com DCMs e bruxismo e 69 controles.
RESULTADOS: A idade média do grupo experimental foi de 33,3 anos. A cronicidade da queixa principal não diferiu entre os grupos com DCMs e bruxismo (teste de Kruskal-Wallis p = 0.13, considerado não significante). Dor intensa foi observada mais frequentemente no subgrupo com bruxismo severo (teste do Chi-quadrado para análise de tendências p = 0.01, considerado significante). Os indivíduos com bruxismo severo haviam usado ou estavam usando mais antidepressivos quando comparados com os outros grupos com bruxismo leve ou moderado e com o grupo controle (teste do Chi-quadrado p = 0.006, muito significante). Um número bem maior de queixas de dor foi registrado no grupo com bruxismo severo (teste de Kruskal-Wallis p = 0.0001, extremamente significante).
CONCLUSÃO: Os pacientes com bruxismo severo relataram histórico de dor. O uso de antidepressivos aumentou com a severidade do bruxismo. O número de locais com dor, a severidade da dor e o uso de antidepressivos aumentou com a severidade do bruxismo.
Palavras-chave: Distúrbios Temporomandibulares; Bruxismo; Dor Facial, Agentes Antidepressivos.
RESUMEN
OBJETIVOS: Comparar la duración, la severidad del dolor, su ocurrencia en múltiples locales y el uso de antidepresivos por pacientes con disturbios cráneomandibulares (DCMs) y bruxismo en individuos de un grupo control.
MATERIALES Y MÉTODOS: Evaluación clínica; cuestionarios sobre dolor, bruxismo y uso de antidepresivos; relato de señales y síntomas; e histórico relacionado al dolor y al palpado muscular en 389 individuos con DCMs y bruxismo y 69 controles.
RESULTADOS: La edad promedio del grupo experimental fue de 33,3 años. La cronicidad de la queja principal no fue diferente entre los grupos con DCMs y bruxismo (prueba de Kruskal-Wallis p = 0.13, considerado no significativo). Se observó dolor intenso con más frecuencia en el subgrupo con bruxismo severo (prueba de Chi-cuadrado para análisis de tendencias p = 0.01, considerado significativo). Los individuos con bruxismo severo habían usado o estaban usando más antidepresivos cuando comparados a otros grupos con bruxismo leve o moderado y con el grupo control (prueba de Chi-cuadrado p = 0.006, muy significativo). Un número mucho mayor de quejas de dolor se registró en el grupo con bruxismo severo (prueba de Kruskal-Wallis p = 0.0001, altamente significativo).
CONCLUSIÓN: Los pacientes con bruxismo severo relataron histórico de dolor. El uso de antidepresivos aumentó con la severidad del bruxismo. El número de locales con dolor, la severidad del dolor y el uso de antidepresivos aumentó con la severidad del bruxismo.
Palabras clave: Disturbios temporomandibulares; Bruxismo; Dolor facial; Agentes antidepresivos.
INTRODUCTION
Craniomandibular disorders (CMDs) is a collective term describing a number of signs and symptoms involving the temporomandibular joints (TMJs), masticatory muscles and other anatomic structures of the stomatognathic system1. Major signs and symptoms of CMDs include pain, impairment of jaw movements, joint sounds, tenderness to palpation of the masticatory muscles and headaches2. Bruxing behavior is the habit of grinding, clenching, bracing or gnashing the teeth with no functional purpose, which occurs during the day, at night or both3. Nocturnal bruxing behavior is a complex motor and neurophysiological disorder thought to occur during transition to lighter sleep stages, but high amplitude parafunctions occur predominantly during REM sleep4. Bruxing behavior can be classified into different sub-types based on the following specific characteristics: strain, severity, association with sleep and depression, destructiveness and pain5,6. The current literature suggests that patients with CMDs can also be categorized into subgroups depending on whether they exhibit bruxing behavior1,7,4,8. Pain in the orofacial region predisposes patients to significant discomfort, suffering and psychosocial morbidity and is often classified into acute and chronic9.
Chronic pain patients exhibit a frustrating medical and dental picture, multiple physical diagnoses, pain, costly invasive treatments, repeated doctor visits and long-term medication use10. Classification of pain as acute or chronic is a subjective phenomenon associated with the interaction of psychological and physiologic variables. Bruxism may be related to psychological and psychosocial variables including anxiety and depression. The severe form of bruxism is characterized by the presence of early morning pain, tiredness and hypertrophy in the region of the masseter muscle11. One study12 reported that baseline depression is a common finding in the majority of patients presenting with chronic facial pain, temporomandibular disorders and bruxing behavior. Anxiety is a feature of acute pain, and chronic pain is frequently characterized by depression, addictive behaviors, substance abuse and eating disorders13. Chronic pain in the orofacial region occurs frequently and yet remains a significant problem that has been subjected to a variety of treatment modalities14. Chronic pain patients are more difficult to diagnose and treat. They may become obsessed, hypochondriacal and worried about any sensation they perceive in their bodies15. They are also more likely to use the health care system, take greater amounts of medication including antidepressants, have multiple drug dependencies and addictions, and present with higher stress scores and partial or permanent disability15.
Patients with chronic facial pain and temporomandibular disorders may present with somatization, "learned helplessness", various types of headaches including tension-type headache and mild, moderate, severe and extreme bruxing behavior16. Additionally, these patients may become discouraged after repeated treatment failures16, and these negative outcomes may contribute to increased use of antidepressants and other drugs. Depression is defined as the pervasive inability to experience pleasure and is characterized by a loss of energy and vitality, retardation, lowered interest, ambitions and responsiveness to environmental events of interpersonal interest15. It is often associated with symptoms of stress and anxiety, and stress and associated oral jaw behaviors commonly cause signs and symptoms of temporomandibular joint disorders (TMDs). Depressive symptoms cause patients to feel overwhelmed and demoralized from the perception of helplessness, hopelessness and lack of control17. Depression and anxiety secondary to chronic pain occur more frequently in women and are commonly associated with jaw and facial pain18. Myofascial pain patients with more than one diagnosis may present more severe pain and more severe bruxing behavior. In addition, chronic myogenic disorders, including myofascial pain, are associated with depression19.
Recent studies in a group of chronic facial pain patients reported substantial evidence of symptoms of anxiety and depression20. One study4 described different subgroups of bruxing behavior patients. One of these subgroups has been shown to be more impaired clinically and psychologically. Sleep bruxism may cause a number of signs and symptoms including pain in diverse components of the masticatory system, and antidepressants are frequently used in the management of such parafunction21. Evaluating the duration and intensity of pain, anatomic sites of pain and antidepressant use in patients with CMDs and severe bruxism is fundamental to better characterize severe bruxism; therefore, the objective of this study is twofold. First, we wanted to test the hypothesis that patients with more severe bruxism and CMD have a longer history of pain and that they present with more severe pain and pain in more anatomic sites compared to patients with mild and moderate bruxism and control subjects. Second, we wanted to assess antidepressant use in CMD patients categorized by the degree of severity of bruxism.
MATERIALS AND METHODS
Information about the frequency of signs and symptoms of CMDs, headaches, presence and severity of bruxing behavior, and medication use including antidepressants was obtained and reviewed retrospectively from a population of patients with CMDs and bruxing behavior who had been consecutively referred to a Center for the Study of CMDs and Facial Pain UNIRG-Tocantins over a period of five years. The group consisted of 340 females and 49 males, and the mean age of the group was 33.3 years (range 13-70, SD: 11.6). The control group consisted of patients referred to the same center for routine dental treatment during the same time. The patients in this group were not seeking treatment for CMDs. The group consisted of 69 subjects, including 49 or 71.0% females with a mean age of 30.0 years (range 16-66, SD: 10.9). CMD patients and control subjects were examined consecutively over the same period of time. A comprehensive protocol was initially used to diagnose and classify patients into mild, moderate or severe bruxing behavior and to characterize the pain complaints based on anatomic site, severity, duration and past/present antidepressant medication use. A brief description of the protocol is as follows:
1 - A set of questionnaires.
2 - History of signs and symptoms
3 - Clinical examination including palpation of muscle and joints, evaluation of jaw movements, analysis of the occlusion, identification of trigger points and patterns of referred pain. We also used diagnostic biomechanical tests to evaluate the presence of specific internal derangements of the temporomandibular joints.
4 - The visual analogue scale (VAS) from 0 (no pain at all) to 10 (the most intense pain) was used to evaluate the severity of pain in patients with CMDs and bruxing behavior and control subjects when pain was the chief complaint. The working definition of the severity of pain was mild (1-3 points), moderate (4-7 points) and severe (8-10 points). Once patients were diagnosed with CMDs, a part of the comprehensive questionnaires was also used to evaluate the presence of bruxing behavior (diurnal, nocturnal or both). Specific criteria to diagnose patients with CMDs were presented in a previous study2. All the patients diagnosed with CMDs and bruxing behavior met the criteria for CMDs and bruxism and were actively seeking treatment. Many patients had been taking self-prescribed drugs, including analgesics and muscle relaxants to reduce muscle pain, joint pain and/or headaches, before the first visit for examination and diagnosis. A section of one of the questionnaires was used to gather data about past/present medication use, including antidepressants. Once the comprehensive questionnaires and clinical examination were completed, all patients were allocated to subgroups of CMDs and mild bruxism, CMDs and moderate bruxism, CMDs and severe bruxism, and non-CMDs/non-bruxism (controls). The specific criteria for the specific subgroups were as follows:
1 - Observation of teeth with visible wear on facets.
2 - History (last six months) of noises, suggesting nocturnal bruxism, according to a report by a friend, relative and/or spouse.
3 - Patient's report of catching himself/herself clenching his/her teeth diurnally.
4 - Patient's report of diurnal tension/stiffness in the masseter muscles.
5 - Patient's account of muscle tension/stiffness along the masseter muscles on awakening in the morning.
6 - Patient's report of awakening while grinding or clenching at night.
7 - Noticeable hypertrophy of the masseter and/or temporalis muscle.
8 - A clinical and subjective report of fatigue of the masseter muscles on awakening.
9 - Patient's report of fatigue of the masseter muscles during the day.
10 - Patient's report of jaws locking on awakening at night or in the morning
11 - Report of cervical pain on awakening in the morning.
12. Patient's report of facial pain on awakening in the morning, specifically of the masseter and/or the temporalis muscles;
13 - Patient's report of body fatigue and/or a feeling of having slept poorly during the previous night.
14 - Toothache or feeling of dental discomfort in the morning.
15 - Patient's report of frequent dislocation of dental restorations.
Patients scoring 3-5 points, 6-10 points and 11-15 points in the above list of 15 items were classified as mild, moderate and severe bruxism, respectively. The scale of severity was designed and developed with the understanding that it would be validated or at least clinically acceptable in future epidemiological findings of patients with CMDs and bruxing behavior if these patients demonstrated higher frequencies of specific joint and muscle disorders with increasing severity of bruxism. The severity of pain in the CMD patients and control subjects presenting with a chief complaint of pain (52 in the mild, 84 in the moderate, 182 in the severe and 10 in the control groups) was evaluated using the VAS scale. Pain sites and the severity of pain in adjacent anatomic areas were also recorded in CMD patients and control subjects. Patients and control subjects who agreed to participate in the study signed a formal consent. The study was approved by the School of Dentistry (number 003-2011).
Statistical analysis: We used the Chi-squared test to assess for independence of groups when proportions were compared and for trends to evaluate a trend comparing various groups when using proportions, non-parametric ANOVA (Kruskal-Wallis) followed by post hoc tests to evaluate for possible significant differences when more than two groups were compared and finally Bartlett's test as a pre-test to evaluate the homogeneity of the variance.
RESULTS
The results of this study are shown in tables 1 through 5. Table 1 summarizes the demographic data of 389 patients with CMDs and bruxing behavior and 69 non-CMD non-bruxing behavior controls.
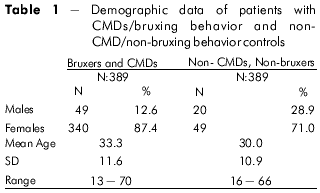
Table 2 shows additional demographic data of patients with CMDs and bruxing behavior classified by the severity of bruxing behavior.
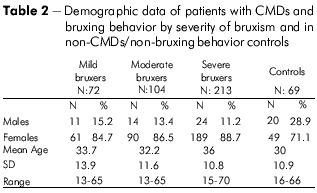
Table 3 provides data on the duration of the chief pain complaint in the subgroups of 52 mild, 84 moderate and 182 severe bruxers and 10 control non-bruxers presenting with pain. The mean duration of the pain complaint was 59 months in the mild, 54.8 in the moderate, 68.6 in the severe and 60.9 in the non-bruxer controls. Kruskal-Wallis test (p = 0.130) showed no statistically significant difference in the duration of the pain complaint.
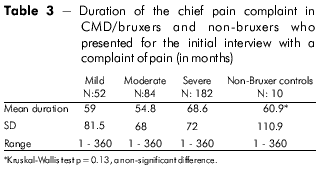
Table 4 demonstrates the frequencies of mild, moderate and severe pain and the history of past and present use of antidepressants in bruxers and CMD patients and in control subjects. The frequencies of mild pain were 7.7%, 7.1% and 6.6% in the mild, moderate and severe groups of bruxers, respectively. The frequencies of moderate pain were 59.6%, 55.6% and 43.4%, respectively, in the same groups. The frequencies of severe pain were 32.7%, 36.9% and 50% in the mild, moderate and severe bruxing behavior groups, respectively. There was a statistically significant difference in the severity of pain in the three subgroups of bruxers (Chi-squared for independence, p = 0.02 and Chi-squared for trends, p = 0.01). There was no statistically significant difference in the frequency of severe pain in the mild and moderate groups and in the moderate and severe groups (p = 0.06). However, there was a statistically significant difference in the severity of pain between the mild and severe bruxing behavior groups (p = 0.02).
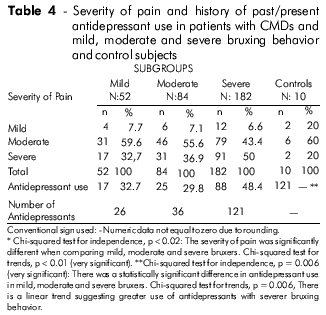
Interestingly, the frequency of mild pain in the subgroups of CMDs and bruxing behavior was very low, suggesting that most CMD and bruxing behavior patients are more likely to seek treatment when the pain is moderate or severe. Only 10 subjects in the control group had a complaint of pain and most of them reported that the pain was moderate. Two subjects reported mild pain and two other individuals reported severe pain. Because only some subjects reported pain in this group, a comparison with the bruxing behavior groups could be meaningless.
The same table shows that 17 patients or 32.7% in the mild group, 25 patients or 29.8% in the moderate group and 88 patients or 48.4% in the severe group reported a history of past/present antidepressant use (Chi-square test for independence, p = 0.006, Chi-squared for trends, p = 0.006, extremely significant difference).
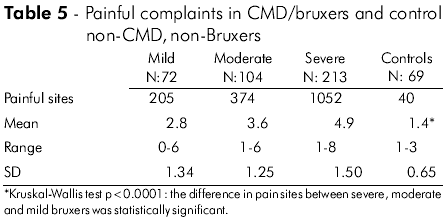
Table 5 shows that the mean number of painful sites in the mild, moderate and severe CMD and bruxing behavior groups was 2.8, 3.6 and 4.9, respectively. A one-way analysis of variance was also performed to assess a possible significant difference in the number of painful complaints (Table 5) between the CMD and bruxing behavior groups. Because F = 71.953 and p < 0.0001, we can state that there was a statistically significant difference between the three groups of bruxers regarding painful complaints. Additionally, the post hoc test supported the findings that, regarding painful sites, mild bruxers were different compared to moderate bruxers (p < 0.01), moderate bruxers were different compared to severe bruxers (p < 0.001), and mild bruxers were also different compared to severe bruxers (p < 0.001).
DISCUSSION
MEAN DURATION OF THE PAIN COMPLAINT
The mean duration of the chief pain complaint was longer in the severe bruxing behavior group, and although the difference was not significant, a longer duration of the pain complaint may be a major characteristic of severe bruxers. A longer duration of pain and depression are closely interrelated, as depression renders the subject more vulnerable to physical and emotional trauma22. Increased muscle tension in severe bruxers may cause more damage to muscles, nerves and joints, thereby creating a vicious cycle responsible for a longer duration of pain. One study23 indicated that high-level muscle tension may facilitate sensitization of pain pathways, which may partially be responsible for a longer duration of pain. It is also likely that bruxers presenting a longer duration of their pain complaint are presenting with chronic bruxism. In one study3, chronic bruxers had higher scores on the somatic and muscle tension scales. Chronic muscle tension may be a contributing factor for a longer duration of pain, which in severe bruxers may also be associated with psychosocial factors including anxiety, psychosomatic tendencies, depression and persistent oral jaw behaviors3,24.
SEVERE PAIN
In the current study, the frequency of severe pain increased with the severity of bruxing behavior (Chi-square test for trends, p = 0.01). The frequency of more severe pain in bruxers was only significantly different (p < 0.02) between the mild and the severe bruxing behavior groups. There was no statistically significant difference in the severity of pain when comparing the mild and moderate groups (Chi-squared test, p = 0.06). Interestingly, only a few patients in all sub-groups presented for the initial interview with a complaint of mild pain, suggesting that most bruxers and patients with CMDs only seek active treatment when the pain has reached a certain intensity. It may be that severer bruxism is characterized by a combination of severe pain, depression and a greater number of pain sites adjacent and distant to the masticatory system. This assumption was at least partially supported by one study25 demonstrating that patients presenting with higher scores for depression report more severe pain, more numerous clinical symptoms and seek more consultations with physicians. In the current study, not all bruxers had a complaint of CMD pain during the initial interview. Thus, the results of this investigation are in accordance with a previous study6 reporting that some CMDs and patients with bruxing behavior had pain complaints while others did not and that some of them reported higher pain scores. It is apparent that the intensity of pain in bruxers varies widely. This difference may be related to the pain duration, scores in somatization, depression, stress, pain from single and multiple sites, cognitive factors, lower pain thresholds and the forces that are generated on the masticatory structures reflecting intensity of muscle activity6.
NUMBER OF PAIN COMPLAINTS
We found that the number of pain complaints increased with the severity of bruxing behavior. The severe bruxing behavior group demonstrated more pain sites and the difference was statistically significant (p < 0.0001). That type of pain may be the result of strong neuromuscular forces applied to the masticatory system or a tendency toward somatization in bruxers and CMD patients. In cases of severe bruxism, the damaging consequences reach beyond damage to the teeth, pain may be of a longer duration and multiple symptoms may occur26. Additional support for the relationship between severe bruxism and a greater number of pain sites comes from a study24 that compared severe bruxism and sleep architecture and reported that 60-80% of the bruxers had pain in multiple sites, including the TMJs and masticatory muscles. A previous investigation25, reported positive and significant correlations between severe bruxism and depression and between severe bruxism and a greater number of painful sites. Although pain at multiple sites was studied in another investigation27, this is the first study that compared pain sites in subgroups of bruxers.
ANTIDEPRESSANT USE
We found that compared to mild and moderate bruxers, severe bruxers had used or were using more antidepressant medication at the time of the first interview, and the difference was statistically significant (Chi-squared test for independence = 13,1932, p < 0.006). Of the 318 patients with CMDs and bruxing behavior with pain, 130 or 40.8% (or 33.4% of all bruxers with or without pain) had a history of past or present antidepressant use. The results showed no statistically significant difference in antidepressant use between mild and moderate bruxers. The frequency of antidepressant use reported in the current study is very similar to the reported frequency of 35.7% in a previous study involving a group of patients with CMDs and headaches in which 73% were bruxers28. Bruxers and individuals with CMDs may be more prone to depression and more severe bruxism is more commonly equated with depression resulting in a stronger tendency to use antidepressant medication. This line of reasoning has been partially supported by a previous study29 indicating that antidepressants can help control nocturnal bruxism, particularly in periods of exacerbation. When severe bruxism is left untreated, it can lead to tooth destruction, temporomandibular dysfunction, headache and depression, thereby resulting in a higher need for antidepressant medication use30 including selective serotonin reuptake inhibitors. Psychological factors including stress, anxiety and depression play a role in the etiopathogenesis of bruxism11 and lead to the use of antidepressants in individuals with this disorder. In cases of sleep bruxism, clonazepam may the drug of choice because it may be improve sleep, depression and anxiety symptoms31.
CONCLUSIONS
Based on the results of the current investigation and data from previous studies, we conclude that more severe bruxers present with a longer history of pain and the severity of pain increases from mild to moderate and severe bruxing behavior groups. The number of local and distant pain sites also increases with the severity of bruxism. Additionally, severe bruxers have more pain complaints, which may indicate somatization or a state of general physical and emotional distress. In addition, they also use antidepressant medication more commonly.
REFERENCES
1 Lobbezoo-Scholte AM, Leeuw JR, Steenks MH, Bosman F, Buchner R, Olthoff LW. Diagnostic subgroups of craniomandibular disorders patients Part I: self-report data and clinical findings. J Orofac Pain. 1995 Winter;9(1):24-36. [Link]
2 Molina OF, Santos Jr, Nelson SJ, Nowlin T. A clinical study of specific signs and symptoms of CMD in bruxers clasified by the degree of severity. Cranio. 1999 Oct;17(4):268-79. [Link]
3 Kampe T, Edman G, Bader G, Tagdae T, Karlsson S. Personality traits in a group of subjects with longstanding bruxing behavior. J Oral Rehab. 1997 Aug;24(8):588-93. [Link]
4 Bader G, Lavigne GJ. Sleep bruxism: overview of an oromandibular sleep movement disorder. Sleep Med Ver. 2000 Feb;4(1):27-43. [Link]
5 Molina OF, Gaio DC, Cury MDN, Cury SE, Gimenez SRM, Salomão EC, et al. Uma análise crítica dos sistemas de classificação sobre o bruxismo: implicações com o diagnóstico, severidade e tratamento dos sinais e sintomas de DTM associados com o hábito. JBA. 2002; jan-mar;2(5):61-9. [Link]
6 Dao TT, Lund JP, Lavigne GJ. Comparison of pain and quality of life in bruxers and patients with myofascial pain of the masticatory muscles. J Orofac Pain. 1994;8(4):350-56.
7 Tan EK, Chan LL, Chang HM. Severe bruxism following basal ganglia infarcts: insights into pathophysiology. J Neurol Sci. 2004 Feb;217(2):229-32.
8 Dworkin SF. Behavioral characteristics of temporomandibular disorders. In: Sessle BJ, Bryant PS, Dione RA, editors. Temporomandibular disorders and related pain conditions. Seattle: IASP Press; 1995. p. 175-92.
9 Harkins SW, Bush FM, Price DD, Hamer RM. Symptoms report in orofacial pain patients. Clin J Pain. 1991 Jun;7(2):102-8.
10 Fricton J. Myogenous temporomandibular disorders: diagnosis and management considerations. Dent Clin N Amer. 2007 Jan;51(1):61-83.
11 Balatsouras D, Kaberos A, Psaltakos V, Papaliakos E, Economou N. Bruxism: two case reports. Acta Othorinolarongol Ital. 2004 Jun;24(3):165-70. [Link]
12 Yap AU, Dworkin SF, Chua EK, List T, Tan KB, Tan HH. Prevalence of temporomandibular disorders subtypes, psychological distress and psychological dysfunction in asian patients. J Orofac Pain. 2003 Winter;17(1 ):21-8. [Link]
13 Gatchell RJ, Garofalo PJ, Ellis E, Holt C. Major psychological disorders in acute and chronic TMD: an initial examination. J Am Dent Assoc. 1996 Sep;127(9):1365-70.
14 DeNucci DJ, Sobiski C, Dionne RA. Triazolan improves sleep but fails to alter pain in TMD patients. J Orofac Pain. 1998 Spring;12(2):116-23. [Link]
15 Fricton JR, Olsen T. Predictors of outcome for treatment of temporomandibular disorders. J Orofac Pain. 1996 Winter;10(1):54-65. [Link]
16 Molina OF, Peixoto MG, Eid NLM, Aquilino RN, Rank RCIC. Headache and bruxing behavior types in Craniomandibular Disorders (Cmds) patients. Rev Neurocienc. 2011;19(3):449-57.
17 Rodin G, Craven J, Littlefield C. Depression in the medically ILL: An integrated approach. New York: Brunner/Mazel; 1991.
18 Saheeb BD, Otakpor AN. Co-morbid psychiatric disorders in Nigerian patients suffering temporomandibular joint pain and dysfunction. Niger J Clin Pract. 2005 Jun;8(1):23-8.
19 Rossetti L, Pereira ACR, Rossetti PH, Conti PC. Association between rhythmic masticatory muscle activity during sleep and masticatory myofascial pain: a polysomnographic study. J Orofac Pain. 2008 Summer;22(3):190-200.
20 Brown FF, Robinson ME, Riley JL, Gremillion HA. Pain severity, negative affect, and microstressors as predictors of life interference in TMD patients. Cranio. 1996 Jan;14(1):63-70.
21 Huynh N, Manzini C, Rompré PH, Lavigne GJ. Weighing the potential effectiveness of various treatments for sleep bruxism. J Can Dent Assoc. 2007 Oct;73(8):727-31.
22 Lautenbacher S, Krieg SJ. Pain perception in psychiatric disorders: a review of the literature. J Psychiatr Res. 1994 Mar-Apr;28(2):109-22.
23 Glaros AG, Williams K, Lausten L. The role of parafunctions, emotions and stress in predicting facial pain. J Am Dent Assoc. 2005 Apr;136(4):451-8.
24 Boutros NN, Montgomery MT, Nishioka G, Hatch JP. The effect of severe bruxism on sleep architecture. a preliminary report. Clin Electroencephalogr. 1993 Apr;24(2):59-62.
25 Franklin MO, Pablo TG, Raphael A, Rise R, Zeila CS, Wilson CED, et al. Depression, pain, and site: a clinical comparison study in mild, moderate, severe and extreme bruxers. Rev Neurocienc. 2007 Jan-Mar;15(1):10-17.
26 Clark GT, Ram S. Four oral motor disorders: bruxism, dystonia, dyskinesia and drug-induced dystonic extrapyramidal reactions. Dent Clin North Am. 2007 Jan;51(1):225-43.
27 Dworkin SF, Von Korff M, LeResche L. Multiple pains and psychiatric disturbances. Arch Gen Psychiatry. 1990 Mar;47(3):239-44.
28 Reik L Jr, Hale M. The temporomandibular joint pain dysfunction syndrome: a frequent cause of headache. Headache. 1981 Jul;21(4):151-6.
29 Hoz-Aizpurua JL, Díaz ED, LaTouche R, Mesa J. Sleep bruxism. Conceptual review and update. Med Oral Patol Cir Bucal. 2011 Mar;16(2):e231-8.
30 Jankovic J. Disease-oriented approach to botulinum toxin. Toxicon. 2009;54:614-623. [Link]
31 Saletu A, Parapatics S, Saletu B, Anderer P, Prause W, Putz H, et al. On the pharmacotherapy of sleep bruxism: placebo-controlled polysomnographic and psychometric studies with clonazepan. Neuropsychobiol. 2005;51(4):214-25.
 Correspondence / Correspondência / Correspondencia:
Correspondence / Correspondência / Correspondencia:
Omar Franklin Molina
Faculdade de Odontologia
(Dor Orofacial e Odontopediatria) UNIRG
Avenida Pará no 1544
CEP: 77400-020
Gurupi - Tocantins - Brasil
Email: ofrank.nyork.harvard.texas@hotmail.com
Received / Recebido em / Recibido en: 14/6/2011
Accepted / Aceito em / Aceito en: 29/11/2011













