INTRODUÇÃO
No Brasil, como estratégia de superar o modelo fragmentado de operar a atenção e a gestão da saúde, a organização das redes de atenção à saúde constituiu-se na premissa sobre a qual foram discutidas as propostas da reforma do Sistema Único de Saúde (SUS)1,2,3,4,5. A universalização do acesso, a descentralização/regionalização e a integração com a formação de redes de atenção são imperativos constitucionais que se tornaram diretrizes fundamentais à construção do SUS, consolidadas pela Constituição Federal de 19886,7,8.
Essa discussão se fortaleceu devido à capacidade das redes de melhorarem a efetividade dos sistemas de saúde, no que diz respeito à prática clínica, aos resultados alcançados, à avaliação dos usuários e ao custo3,7,9,10,11,12. As redes de atenção à saúde oferecem condições estruturalmente mais adequadas para a efetivação da integralidade da atenção e a racionalidade sistêmica na utilização dos recursos, reduzindo os custos8,10. Mendes7 classificou três elementos como os atributos de uma rede de atenção à saúde: a população, a estrutura operacional e o modelo de atenção à saúde.
Considerando os componentes acima descritos, destaca-se o papel da atenção primária à saúde como coordenadora da atenção e responsável pela referência e contrarreferência dos usuários aos pontos de atenção especializada de uma rede. Sua importância para o desempenho e a qualidade das redes de atenção à saúde tem sido relatada na literatura9,12,13,14.
Diante do crescente reconhecimento de que as redes de atenção à saúde constituem respostas eficientes frente às condições crônicas2,7,11, identificou-se a necessidade de se verificar, na literatura, a existência de um instrumento de pesquisa capaz de avaliar o estágio de desenvolvimento da rede de atenção à saúde bucal. Foi encontrado um instrumento que permite identificar o estágio de desenvolvimento das redes de atenção à saúde: Instrumento de Diagnóstico do Estágio de Desenvolvimento da Rede de Atenção à Saúde7.
O Instrumento em questão, no entanto, não aborda especificidades da área da saúde bucal, não sendo encontrado qualquer outro instrumento direcionado à avaliação do estágio de desenvolvimento da rede de atenção à saúde bucal.
Ter, na prática, um instrumento específico para avaliar o estágio de desenvolvimento da rede de atenção à saúde bucal é necessário e importante, pois esse tipo de ferramenta pode auxiliar na elaboração de políticas públicas voltadas para as especificidades de organização da saúde bucal. A versão saúde bucal do Instrumento de Diagnóstico do Estágio de Desenvolvimento da Rede de Atenção à Saúde foi adaptada por Leal et al.3.
Este estudo objetivou validar a versão saúde bucal do Instrumento de Diagnóstico do Estágio de Desenvolvimento da Rede de Atenção à Saúde no sistema público dos municípios/estados brasileiros.
MATERIAIS E MÉTODOS
AMOSTRA
O estudo foi realizado de agosto a dezembro de 2012 e contou com uma amostra de conveniência constituída pelos coordenadores municipais de saúde bucal de municípios do estado de Minas Gerais, Região Sudeste do Brasil. Minas Gerais possui atualmente 853 municípios15. Ser cirurgião dentista e exercer o cargo de coordenador municipal de saúde bucal foram considerados critérios de inclusão para a composição da amostra. Após a autorização da Secretaria de Estado de Saúde de Minas Gerais (SES-MG), foram selecionados 184 municipíos, considerando-se os critérios de inclusão, e o coordenador municipal de saúde bucal de cada um deles foi convidado a participar do estudo. O convite foi realizado via telefone ou e-mail. Os contatos dos possíveis participantes foram obtidos com as 28 Superintendências/Gerências Regionais de Saúde da SES-MG.
Os coordenadores municipais de saúde bucal que concordaram em participar receberam, por e-mail e/ou por intermédio das referências de saúde bucal da SES-MG, o Termo de Consentimento Livre e Esclarecido, um formulário sobre as características individuais do participante (idade, sexo, ter pós-graduação, tipo de vínculo empregatício, tempo de formado e tempo de coordenação de saúde bucal) e o questionário versão saúde bucal. Após assinatura do Termo e do preenchimento do formulário e do questionário, os participantes encaminharam todo o material por intermédio das referências de saúde bucal da SES-MG. O anonimato dos participantes foi garantido pela não identificação nominal e do município.
A fase de validação aconteceu após o término das etapas de adaptação do Instrumento3. Considerou-se uma significância estatística de p ≤ 0,05.
A versão saúde bucal seguiu a mesma estrutura do instrumento original no agrupamento por domínios, com convergência das questões incluídas em cada domínio, bem como a pontuação a ser atribuída7. O Instrumento apresentava 107 questões (Quadro 1) com quatro opções de resposta para cada item: 0 - não existência do que está sendo perguntado; 1 - funcionamento básico ou incipiente; 2 - funcionamento razoavelmente bom, mas insuficiente; 3 - existência em operação de forma ótima. Era composto por sete dimensões: população, atenção primária à saúde, pontos de atenção à saúde secundários e terciários, sistemas de apoio, sistemas logísticos, sistema de governança da rede e modelo de atenção à saúde.

Quadro 1 - Instrumento de Diagnóstico do Estágio de Desenvolvimento da Rede de Atenção à Saúde Bucal
No que diz respeito à interpretação dos resultados, a versão saúde bucal seguiu o instrumento original7. O resultado final poderia variar de 0 a 321 e foi obtido por meio da soma dos escores de 0 a 3 obtidos em cada uma das questões. O quadro 2 descreve a interpretação final dos escores.
PRÉ-TESTE COM UMA SUBAMOSTRA DA POPULAÇÃO-ALVO DO ESTUDO
A versão adaptada do Instrumento foi submetida a um pré-teste, com uma amostra de conveniência, em alguns municípios mineiros. Essa etapa foi realizada por meio do envio do Termo de Consentimento Livre e Esclarecido, do formulário individual e do questionário para 28 coordenadores municipais de saúde bucal, dentre os 184 relacionados, sendo realizada por intermédio da SES-MG.
Para a avaliação de confiabilidade teste-reteste, o questionário foi aplicado, duas vezes, aos mesmos participantes16,17,18,19. O material foi enviado em dois momentos distintos, denominados de fase I e II. Os participantes foram orientados a devolver o material em até uma semana (fase I) e receberam o questionário novamente após 10 dias (fase II), devendo enviá-lo de volta em seguida.
Foi obtido o retorno de 20 municípios nas fases I e II. As propriedades psicométricas do Instrumento (confiabilidade e validade) foram devidamente analisadas.
TESTE DE CAMPO
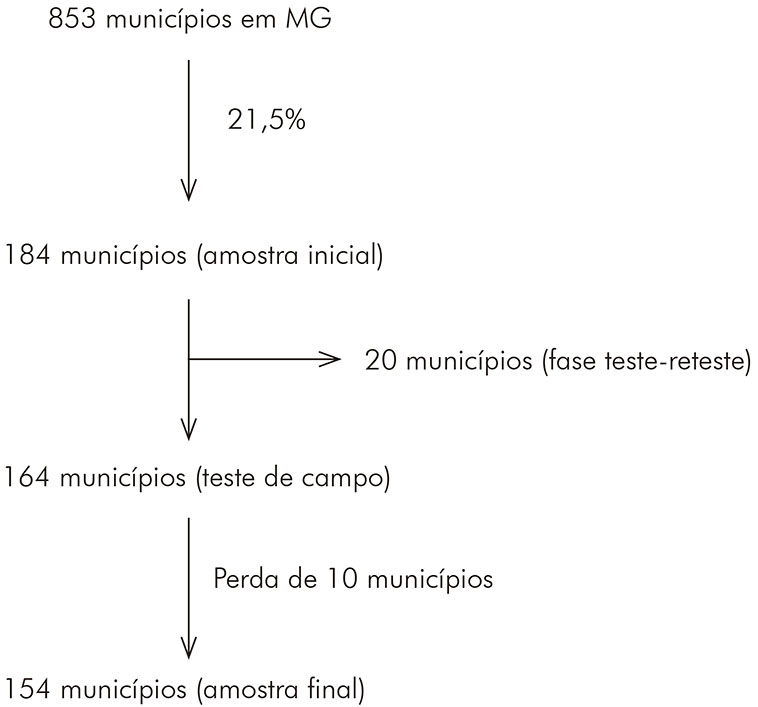
O material necessário para a coleta de dados foi enviado para 164 municípios com coordenadores municipais de saúde bucal. Cada município possuía um coordenador de saúde bucal. Foi obtido retorno de 154 municípios na fase I. As 10 perdas aconteceram porque sete coordenadores municipais não retornaram com os questionários e não justificaram o fato. Dois municípios, previamente selecionados, foram excluídos da amostra por não terem um coordenador de saúde bucal que fosse dentista no momento da coleta de dados; e outro município foi excluído devido à licença médica da coordenadora de saúde bucal (Figura 1).
ESTUDO DAS PROPRIEDADES PSICOMÉTRICAS DO INSTRUMENTO (CONFIABILIDADE E VALIDADE)
A fase de validação referiu-se à análise das propriedades psicométricas; ou seja, verificar a confiabilidade (consistência interna e estabilidade) e a validade do Instrumento adaptado (capacidade de mensurar efetivamente o que se propõe a medir). Os dados foram analisados por meio do software Statistical Package for the Social Sciences v20.0 (SPSS Inc, Chicago, IL, EUA).
Os valores de consistência interna do Instrumento foram estimados por meio do coeficiente alfa de Cronbach (verifica a homogeneidade do Instrumento); quando utilizado para comparar grupos, é considerado satisfatório com valores entre 0,70-0,8020. A consistência interna evidencia se todos os itens que compõem o Instrumento se relacionam, sendo analisado o comportamento de cada item e do total de itens17,19,21,22,23.
A estabilidade avaliada pelo teste-reteste foi determinada pelo cálculo do coeficiente de correlação intraclasse (CCI). A verificação da estabilidade é necessária para analisar se o Instrumento produz, consistentemente, resultados semelhantes ao ser aplicado em um mesmo indivíduo, em diferentes instantes de tempo, sem que tenha havido mudança real para o respondente9,11,22,24. O valor de CCI é considerado excelente se for maior que 0,74, bom se estiver de 0,60 a 0,74 e razoável se abranger de 0,40 a 0,5925.
A validade de constructo do Instrumento foi analisada por meio da correlação de Spearman. Para isso, foram calculadas correlações entre duas perguntas relacionadas à classificação global ("Considerando-se o estágio de desenvolvimento da rede de saúde bucal, há uma definição clara das necessidades de saúde bucal da população?" e "Considerando-se o estágio de desenvolvimento da rede de saúde bucal, há uma definição clara da realização das ações da atenção primária?") e o escore total e dos domínios. A validade discriminante foi avaliada pelo teste Mann-Whitney e obtida por meio da comparação do escore total e de cada domínio do Instrumento entre os grupos estudados. Foi considerado um intervalo de confiança (IC) de 95%. Durante a análise dos dados, foram considerados os critérios de Landis e Koch26 para a interpretação da concordância: -1,0 a 0 pobre; 0,01 a 0,20 discreta; 0,21 a 0,40 regular; 0,41 a 0,60 moderada; 0,61 a 0,80 substancial; 0,81 a 1,00 quase perfeita.
De acordo com a Resolução nº 466/2012 do Conselho Nacional de Saúde, este estudo foi aprovado pelo Comitê de Ética em Pesquisa da Universidade Federal de Minas Gerais em 27 de junho de 2012 (parecer nº 55044/2012).
RESULTADOS
A amostra final foi composta por 154 coordenadores municipais de saúde bucal na faixa etária de 23 a 69 anos. A média de idade dos participantes foi de 40,1 anos ±9,2. Verificou-se que a maior parte da amostra declarou ser do sexo feminino (64,3%), ter alguma especialização, mestrado ou doutorado (81,2%) e ser concursado (64,3%). O tempo médio de formado foi de 16,4 anos ±9,1 e de coordenação foi de 4,2 anos ±3,6.
CONFIABILIDADE DO INSTRUMENTO
O coeficiente alfa de Cronbach foi 0,97 para o escore total, variando de 0,77 a 0,94 para os domínios. Considerando-se a estabilidade do Instrumento, os resultados do teste-reteste mostraram que o escore total apresentou CCI de 0,88. Para os domínios, os valores
de CCI variaram de 0,83 a 0,91 (Tabela 1).
Tabela 1 - Resultado da análise de confiabilidade do Instrumento e dos domínios
| Variável | Número de itens | Alfa de Cronbach (N = 154) | CCI (IC 95%) (N = 140)* |
|---|---|---|---|
| Total do Instrumento | 107 | 0,97 | 0,88 (0,87-0,89) |
| Domínios | |||
| População | 11 | 0,87 | 0,91 (0,89-0,92) |
| Atenção primária à saúde | 15 | 0,88 | 0,87 (0,85-0,88) |
| Pontos de atenção à saúde secundários e terciários | 19 | 0,91 | 0,88 (0,86-0,89) |
| Sistemas de apoio | 15 | 0,77 | 0,86 (0,85-0,87) |
| Sistemas logísticos | 11 | 0,77 | 0,83 (0,80-0,85) |
| Sistema de governança da rede | 10 | 0,85 | 0,90 (0,89-0,93) |
| Modelo de atenção à saúde | 26 | 0,94 | 0,87 (0,86-0,88) |
* 140 coordenadores participaram da fase II.
VALIDADE DE CONSTRUCTO
A correlação de Spearman (r s) foi significante para os indicadores globais e os escores totais (p ≤ 0,001) e também para cada um dos domínios investigados (Tabela 2). A mensuração das concordâncias dos itens demonstrou valores de r s entre 0,25 e 0,81.
Tabela 2 - Análise da validade de constructo: correlações entre o escore total do Instrumento e o escore dos domínios, e indicador global sobre as necessidades de saúde bucal e ações de atenção primária (N = 154)
| Indicador global | ||||
|---|---|---|---|---|
| Necessidades de saúde bucal | Ações de atenção primária | |||
| r s | p* | r s | p* | |
| Total | 0,70 | < 0,001 | 0,55 | < 0,001 |
| Domínios | ||||
| População | 0,81 | < 0,001 | 0,53 | < 0,005 |
| Atenção primária à saúde | 0,64 | < 0,001 | 0,58 | < 0,001 |
| Pontos de atenção à saúde secundários e terciários | 0,29 | < 0,001 | 0,25 | < 0,011 |
| Sistemas de apoio | 0,47 | < 0,001 | 0,38 | < 0,021 |
| Sistemas logísticos | 0,37 | < 0,001 | 0,33 | < 0,001 |
| Sistema de governança da rede | 0,42 | < 0,001 | 0,29 | < 0,001 |
| Modelo de atenção à saúde | 0,59 | < 0,001 | 0,41 | < 0,001 |
* Significância para p ≤ 0,05.
VALIDADE DISCRIMINANTE
De acordo com a tabela 3, o escore total do Instrumento e os domínios "População", "Sistemas logísticos" e "Sistema de governança da rede" mostraram-se capazes de distinguir os grupos de coordenadores de acordo com o tempo de formado (p ≤ 0,05).
Tabela 3 - Análise da validade discriminante: escore total do Instrumento e escore dos domínios, de acordo com o tempo de formado em Odontologia dos participantes (N = 154)
| Grupo 1 (≤ 16 anos de formado) | Grupo 2 (> 16 anos de formado) | p* | |||
|---|---|---|---|---|---|
| (N = 79) | (N = 75) | ||||
| Média ± DP† | Mediana | Média ± DP† | Mediana | ||
| Total | 143,04 ± 41,14 | 126,000 | 123,31 ± 46,12 | 122,00 | 0,025 |
| Domínios | |||||
| População | 19,16 ± 4,68 | 18,00 | 15,17 ± 6,85 | 14,00 | < 0,001 |
| Atenção primária à saúde | 29,18 ± 7,32 | 28,00 | 26,55 ± 8,60 | 28,00 | 0,118 |
| Pontos de atenção à saúde secundários e terciários | 19,01 ± 11,42 | 19,00 | 20,12 ± 12,39 | 20,00 | 0,637 |
| Sistemas de apoio | 17,29 ± 6,40 | 15,00 | 15,20 ± 6,70 | 15,00 | 0,090 |
| Sistemas logísticos | 11,47 ± 4,95 | 12,00 | 8,04 ± 4,99 | 7,00 | < 0,001 |
| Sistema de governança da rede | 12,90 ± 5,08 | 13,00 | 8,53 ± 5,24 | 8,00 | < 0,001 |
| Modelo de atenção à saúde | 34,28 ± 15,43 | 32,00 | 29,19 ± 12,75 | 29,00 | 0,073 |
* Teste Mann-Whitney (significância para p ≤ 0,05); † DP: Desvio padrão.
DISCUSSÃO
Novas ideias exigem novas práticas, e, portanto, a adequação do processo de trabalho e a utilização de ferramentas de planejamento e organização dos serviços são fundamentais para a efetividade da atenção voltada à produção do cuidado e da saúde. A rede de atenção à saúde bucal, estruturada a partir da atenção primária, deve ser capaz de oferecer uma atenção de qualidade e integral aos usuários, por meio da identificação das necessidades de saúde bucal da população. Nesse sentido, faz-se necessária a realização do processo de validação de um instrumento direcionado à rede de atenção à saúde bucal.
Considerando-se o fato da proposta do presente estudo ser a validação de um questionário com especificidades relacionadas à saúde bucal e que o sucesso dependeria de uma adequada interpretação do mesmo, a formação em Odontologia dos coordenadores de saúde bucal foi considerada essencial3.
As propriedades psicométricas foram avaliadas de forma semelhante a outros estudos de validação17,18,19,21,22,25. A consistência interna da versão adaptada para a saúde bucal foi satisfatória para todos os domínios. A estabilidade do Instrumento foi verificada por meio do teste-reteste (aplicação do CCI para o escore total e para os domínios). Os resultados mostraram excelente estabilidade do Instrumento para o escore total e para os domínios. A validade de construto foi significante, sendo obtida por meio da análise do coeficiente de correlação de Spearman entre as duas perguntas referentes à classificação global (necessidade de saúde bucal e ações de atenção primária) e o escore total e dos domínios.
Quanto às questões globais (necessidade de saúde bucal e ações de atenção primária), a concordância do escore total do Instrumento foi maior quando comparada às necessidades de saúde bucal do que quando comparada às ações de saúde bucal, como visto na tabela 2. Provavelmente, essa situação aconteceu devido ao fato da ampla divulgação dos resultados de inquéritos epidemiológicos, como o SB Brasil 2003 e o SB Brasil 20106,24. Esses estudos mensuraram as necessidades de saúde bucal da população brasileira, o que possibilitou aos gestores adquirirem conhecimento sobre o quadro epidemiológico e as necessidades da população, bem como sobre as ações e serviços necessários para enfrentar esse quadro epidemiológico.
Os resultados obtidos entre o escore total do Instrumento e as ações de atenção primária podem ser explicados pelo fato da discussão de redes de atenção à saúde bucal ainda ser recente. Embora os pontos de atenção da rede sejam discutidos, as competências dos mesmos ainda geram conflitos de entendimento entre os gestores. Esse ponto também pode ser observado com relação ao domínio "Pontos de atenção à saúde secundários e terciários", que apresentou os menores resultados quando analisado por meio das duas questões globais. Além disso, a fragilidade do cumprimento das atribuições referentes ao nível da atenção primária é um dos motivos que interferem na inserção efetiva da saúde bucal na rede de atenção à saúde5,27,28.
A validade discriminante foi obtida pela comparação dos escores total e de cada dimensão do Instrumento adaptado, de acordo com o tempo de formado em Odontologia dos participantes. Os coordenadores de saúde bucal com menos tempo de formado (< 16 anos) apresentaram valores maiores no escore total do Instrumento e de alguns domínios. Além das discussões de rede serem recentes, provavelmente as faculdades de Odontologia, na tentativa de adaptar o currículo às demandas dos serviços públicos, inseriram, na grade curricular, nos últimos 20 anos, disciplinas voltadas à discussão do SUS, período esse referente ao início de implantação desse sistema de saúde. Essa abordagem acaba por promover nos alunos reflexões acerca das organizações dos serviços públicos de saúde, objetivando formar profissionais de saúde bucal aptos a trabalharem na clínica e na gestão desses serviços. Uma formação considerada tecnicista, muitas vezes, é acrítica, pouco reflexiva e segmentada, direcionada à inserção do profissional no mercado privado, com foco no atendimento curativo e individualizado.
Provavelmente, a ausência de conhecimentos baseados nas premissas do SUS, aliada a uma formação acadêmica curativa, acarretou um despreparo do profissional para uma atuação adequada dentro do sistema de saúde pública brasileiro. Essa situação pode comprometer a incorporação de novas práticas de atenção, dificultando o entendimento dos cirurgiões dentistas em relação à rede de atenção29,30. De acordo com Mello et al.5, essa formação ainda não foi adequada, efetivamente, ao Brasil, tanto no que diz respeito aos dados epidemiológicos da população quanto em relação ao modelo de atenção à saúde essencial para um bom desempenho do SUS, com a implantação das redes de atenção à saúde.
Além disso, a influência das estratégias e políticas do Ministério da Saúde, estados e municípios, objetivando a adequação da formação e qualificação dos trabalhadores de saúde às necessidades de desenvolvimento do SUS, deve ser levada em consideração nesse resultado. No estado de Minas Gerais, dentro de uma proposta de educação permanente em saúde, são desenvolvidas ações, junto aos municípios, voltadas para a discussão do quadro epidemiológico de saúde bucal no Estado e para a organização da atenção em saúde bucal na forma de rede31.
A ausência de contato direto entre o pesquisador e os participantes pode ser considerada uma limitação deste estudo. Não se tem a garantia de que o questionário tenha sido respondido pelos coordenadores municipais de saúde bucal.
CONCLUSÃO
O Instrumento de Diagnóstico do Estágio de Desenvolvimento da Rede de Atenção à Saúde Bucal foi considerado válido para ser utilizado entre os coordenadores de saúde bucal dos municípios/estados brasileiros. As propriedades psicométricas encontradas foram satisfatórias.
O Instrumento validado para a saúde bucal poderá auxiliar os gestores de saúde, em especial os de saúde bucal, a conhecerem melhor o estágio de desenvolvimento da rede de atenção à saúde bucal em seus municípios/estado. A partir desse conhecimento, medidas efetivas, relacionadas ao planejamento de ações e serviços voltados à área da saúde bucal, poderão ser tomadas.











 texto em
texto em