ORIGINAL ARTICLE | ARTIGO ORIGINAL | ARTÍCULO ORIGINAL
Annual frequency and distribution of tuberculosis resistance in the public health laboratory network of Pará State, Brazil
Frequência e distribuição anual de resistência da tuberculose na rede de laboratórios de saúde pública do Estado do Pará, Brasil
Frecuencia y distribución anual de resistencia de la tuberculosis en la red de laboratorios de salud pública del Estado de Pará, Brasil
Maria Luiza LopesI; Emilyn Costa ConceiçãoI; Ricardo José de Paula Souza e GuimarãesII; Ana Roberta Fusco da CostaIII; Karla Valéria Batista LimaIII
]]> IPrograma de Pós-graduação em Biologia Parasitária da Amazônia, Universidade do Estado do Pará, Belém, Pará, BrasilCorrespondence
Endereço para correspondência
Dirección para correspondencia
ABSTRACT
This study described the frequency and variety of multidrug-resistant tuberculosis (MDR-TB) cases in Pará State, Brazil. In order to record the epidemiology and spacial distribution of the disease, antimicrobial susceptibility testing (AST) and the proportion method were used. The AST was performed on 848 samples at the Instituto Evandro Chagas and a central public health laboratory in that State. Of all patients enrolled in the study, 358 (42.2%) were resistant to at least one antituberculosis (anti-TB) drug. The percentage of primary, acquired resistance and combined MDR-TB was 30.4%, 69.3% and 42.2% respectively. MDR-TB was detected in 223 (26.3%) samples. Primary MDR-TB was found in 14% of previously treated patients, while 48% exhibited acquired resistance and 62% exhibited combined resistance. Of all age groups, from 25 to 36 years old (mean age 38.7 ± 15) showed the highest proportion of resistant cases (26.3%). Seven cities in the State presented 59.6% of the cases documented in the study. These findings reflect the poor quality of the healthcare for patients in these cities. We further suggest that clinicians need to observe their patients more directly during treatment and test them more often for anti-TB drug sensitivity. The number of TB cases in Pará did not vary significantly during the period studied, but researchers did notice a slight increase in the proportion of drug-resistant cases related to the total number of cases reported in Pará. This change in the resistance rates reflects the need to improve the quality of health services for TB care. A concentration of TB cases was observed in some municipalities and in the neighborhoods of the Belém City.
]]> Keywords: Mycobacterium tuberculosis; Tuberculosis; Multidrug-resistant; Rifampicin; Isoniazid.RESUMO
Este estudo descreveu a frequência e variedade de casos de tuberculose multirresistente (TBMR) no Estado do Pará, Brasil. A fim de registrar a epidemiologia e a distribuição espacial da doença, foram utilizados testes de suscetibilidade antimicrobiana (TSA) e do método proporcional (MP). O TSA foi realizado em 848 amostras no Instituto Evandro Chagas e em um laboratório central de saúde pública naquele Estado. De todos os pacientes incluídos no estudo, 358 (42,2%) eram resistentes a pelo menos um medicamento antituberculose (anti-TB). A porcentagem das resistências primária, adquirida e TBMR foi de 30,4%, 69,3% e 42,2%, respectivamente. A TBMR foi detectada em 223 (26,3%) amostras. A TBMR primária foi encontrada em 14% dos pacientes tratados anteriormente, enquanto que 48% apresentaram a resistência adquirida e 62% exibiram resistência combinada. De todos os grupos etários, o de 25-36 anos (média de idade de 38,7 ± 15) apresentou a maior proporção de casos resistentes (26%). Sete cidades do Estado apresentaram 59,6% dos casos documentados no estudo. Estes resultados refletem a baixa qualidade dos cuidados de saúde com os doentes nestas cidades. Observa-se ainda, a necessidade de maiores cuidados dos médicos para com os pacientes durante o tratamento e realização, com maior frequência, dos testes de sensibilidade aos medicamentos anti-TB. O número de casos de TB no Pará não variou significativamente durante o período estudado, porém os pesquisadores notaram um ligeiro aumento na proporção de casos resistentes aos medicamentos relacionados com o número total de casos notificados no Estado. Esta mudança nas taxas de resistência reflete a necessidade de melhorar a qualidade dos serviços de saúde para a atenção à TB. A concentração de casos de tuberculose foi observada em alguns municípios e nos bairros da Cidade de Belém.
Palavras-chave: Mycobacterium tuberculosis; Tuberculose; Resistência a Múltiplos Medicamentos; Rifampicina; Isoniazida.
RESUMEN
Este estudio describe la frecuencia y variedad de casos de tuberculosis multirresistente (TBMR) en el Estado de Pará, Brasil. Con la finalidad de registrar la epidemiología y distribución espacial de la enfermedad, se utilizaron pruebas de susceptibilidad antimicrobiana (PSA) y el método proporcional (MP). El PSA fue realizado en 848 muestras del Instituto Evandro Chagas y en un laboratorio central de salud pública del Estado. De todos los pacientes incluidos en este estudio, 358 (42,2%) eran resistentes a, por lo menos, un medicamento antituberculosis (anti-TB). El porcentaje de resistencia primaria, adquirida y TBMR fue de 30,4%, 69,3% y 42,2%, respectivamente. Se detectó TBMR en 223 (26,3%) muestras. Se encontró TBMR primaria en 14% de los pacientes con tratamiento previo, mientras que un 48% presentó resistencia adquirida y 62% combinada. De todos los grupos etarios, el de 25-36 años (promedio de edad 38,7 ± 15) presentó la mayor proporción de casos resistentes (26%). Siete ciudades del Estado concentraron el 59,6% del total de casos documentados en el estudio. Estos resultados reflejan la baja calidad de cuidados en salud con los enfermos en estas ciudades. También observamos, la necesidad de mayores cuidados por parte de los médicos durante el tratamiento realizado, con mayor frecuencia, de exámenes de sensibilidad a medicamentos anti-TB. El número de casos de TB en Pará no varió significativamente durante el periodo estudiado, sin embargo, los investigadores notaron un ligero aumento en la proporción de casos resistentes a medicamentos relacionados al número total de casos notificados en el Estado. Este cambio en las tasas de resistencia refleja la necesidad de mejorar la calidad de los servicios de salud para la atención de TB. La concentración de casos de tuberculosis se observó en algunos municipios y barrios de la Ciudad de Belém.
Palabras clave: Mycobacterium tuberculosis; Tuberculosis; Resistencia a Múltiples Medicamentos; Rifampicina; Isoniazida.
INTRODUCTION
]]> One of the biggest problems to tuberculosis (TB) control is multidrug-resistant tuberculosis (MDR-TB). While drug-susceptible TB is effectively treated in most patients, MDR-TB treatment has a success rate of less than 50%, with high mortality and costs1,2. Globally, in the period from 1994 to 2010, MDR-TB was observed in 3.4% of all new TB cases and 19.8% of previously treated cases. The highest global rates of MDR-TB ever reported were documented in 2009 and 2010, justifying continued surveillance of tubercular patients in different countries3. The data about MDR-TB in previously treated individuals (acquired MDR-TB) reflect poor adherence to therapy, whereas primary cases of MDR-TB reflect infection transmission in the community.In another report, published in 2000 by the World Health Organization (WHO), the worldwide prevalence of MDR-TB was given as 7.6%, with an acquired resistance rate of 0.06%. In 2010, the worldwide prevalence had fallen to 5.4%, but acquired resistance had risen to 0.36%. The global rates of acquired resistance in 2000 and 2010 were both lower than the rates obtained in two earlier investigations conducted in Brazil4,5. The first of these Brazilian studies, which was conducted in 1996-1997, found that 8.5% of new TB cases were resistant to any drug, and that 21%of previously treated patients were also resistant. The rates of primary and acquired MDR-TB were 1.1% and 7.9%, respectively, among patients who received pre-treatment6. Data obtained in the Second National Inquiry on Resistance to Anti-TB Drugs, performed on 4,421 patients from seven states, put rates of primary resistance and acquired multidrug resistance at 1.4% and 7.5% respectively. In this more recent study, rates of primary and acquired MDR-TB remained at levels similar to those of the 1996-1997 study. Results of studies developed in some individual Brazilian states, however, have varied considerably. The rates of primary and acquired MDR-TB in the City of Porto Alegre, Rio Grande do Sul State, were 2.2% and 12.0% respectively5. Researching data collected from 2000 to 2006 in Mato Grosso State by Marques et al7 reported primary and acquired rates of MDR-TB of 1.6% and 20.3% respectively. Previous studies performed by the Instituto Evandro Chagas (IEC) from July 2002 to June 2003 in the School Health Centre of Marco (a type 2 Reference Unit for the treatment of TB located in Belém) detected resistance to any drug in 16% of evaluated cases and primary resistance in 14% of evaluated cases (own unpublished data). Located in the Brazilian Amazon Region, Pará State ranks in third position among all Brazilian states in the number of TB cases and fourth in the number of MDR-TB cases. However, epidemiological information at the local level remains poor. The purpose of this study was to provide a fuller epidemiological profile regarding TB resistance of the State. In pursuit of that goal, this study used routine laboratory results from the IEC and the Central Laboratory of the State of Pará (LACEN/PA), in order to determine the frequency of antimicrobial resistance, its epidemiological traits and spatial distribution.
MATERIALS AND METHODS
This study was conducted in Pará State, Brazil, which has a population of 7,443,904 million individuals and presented a TB case rate of 47.5 per 100,000 individuals in 20108. An ecological study was conducted using data from 848 susceptibility tests, which were performed on 848 tuberculosis patients who met the indicated criteria for such tests: i) receiving retreatment after failure of the bacteriological standard treatment; ii) experiencing recidivism of the disease; iii) beginning treatment after abandoning it; iv) being suspected of primary resistance; v) having contact with a resistant TB case; vi) being a health professional exposed to TB; vii) being HIV positive; viii) living on the street; ix) being medically confined; x) being in long-term care facilities; xi) being a member of indigenous population; and xii) being attended in hospitals where do not adopt biosecurity measures9. Cases treated between 2005 and 2010 were included in this study. All of susceptibility tests for Mycobacterium tuberculosis in Pará were performed by the Public Health Laboratory Network of Pará (constituted by IEC and LACEN/PA) and included tests for resistance to rifampicin (R), isoniazid (H), streptomycin (S), pyrazinamide (Z), ethambutol (E) and ethionamide (Et).
A TB case was defined as one for M. tuberculosis complex culture-confirmed. A case of tuberculosis was defined as drug resistant (DR-TB) for any type of resistance detected. MDR-TB was defined as resistant to at least H and R. Poly-resistance was defined as resistant for two or more drugs in addition to H and R. Primary DR-TB was defined as the presence of resistant strains of M. tuberculosis in a newly diagnosed patient who had either never received TB drugs or had received them for less than one month. Acquired DR-TB was defined as the presence of strains in patients who had previously received at least one month of TB therapy. Combined resistance was used to refer to all cases in which resistance was found, no matter the treatment history of the disease. Prevalence was calculated by dividing the number of positive cases with the total number of cases tested10.
Data regarding each individual's sex, age, district, and status before getting into the program (new case, relapse, failure or abandonment) and were collected by searching patient files from three sources: the Bacteriology and Mycology Section/IEC of the Hospital Universitário João de Barros Barreto, the School Health Centre of Marco and LACEN/PA.
The proportion method recommended by the Brazilian Ministry of Health was used to evaluate data9. Susceptibility tests were conducted on Lowenstein-Jensen medium. Antibiotics were applied in the recommended critical concentrations of 0.2 µg/mL for H, 40.0 µg/mL for R, 2.0 µg/mL for E, 25.0 µg/mL for Z, 4.0 µg/mL for S and 20.0 µg/mL for Et.
The spatial distribution of patients in the study was analysed using the Kernel smoothing technique, a nonparametric method used to estimate the number of events per unit area in each cell of a regular grid covering the overall area. The clusters were defined as a geographically bound, non-random group11,12. A bandwidth of 1 km was used for estimating the Kernel density of MDR-TB patients. The results were depicted graphically using thematic maps.
The ethical clearance for this study was granted by the IEC (CAAE: 0002.0.072.000-11) on May 25, 2011.
]]>RESULTS
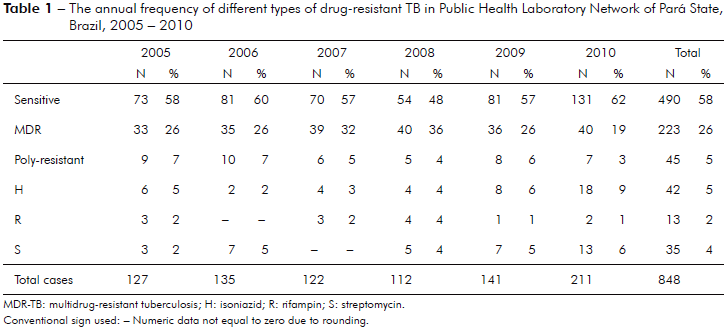
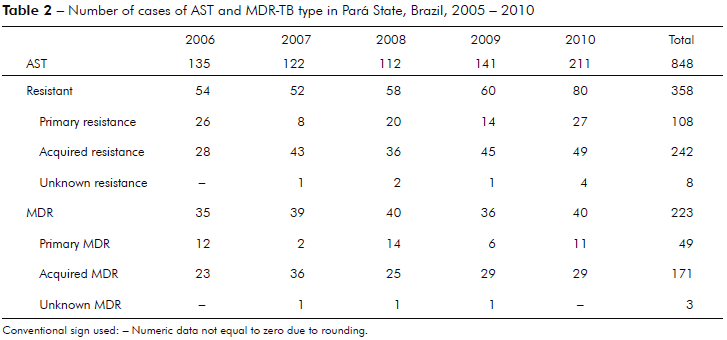
Samples taken from 848 tubercular patients were tested for drug susceptibility, 358 (42.2%) showed some form of resistance. The annual number of cases for different types of DR-TB is shown in table 1. The number of TB cases received to AST and the resistance type (Table 2). In some cases, with the isolation of M. tuberculosis resistant to drugs, there was no information about any kind of previous treatment for TB (unknown resistance or unknown MDR). The frequency for primary, acquired and combined DR-TB were 30.4%, 69.3% and 42.2% respectively. MDR-TB was observed in 223 (26.3%) patients. During the study period, there were 17,983 officially reported TB cases in Pará State. In this context, the MDR-TB prevalence was 1.2%. The rates for primary, acquired and combined MDR-TB were 13.7%, 47.7% and 62.3% respectively.

Of the patients studied, 62.5% were men, and the average age of the population was 38.7 ± 15 years old. The age group most frequently found in the study was from 25 to 34 years old, which together represented 224 (26%) of all cases in the study. Overall, 79% of patients with TB and 80% of patients with MDR-TB were between the ages of 15 and 54 years old.
Seven cities (Abaetetuba, Ananindeua, Belém, Bragança, Castanhal, Marituba and Santarém) were responsible for 59.6% (133/223) of all MDR-TB cases. Of these cases, 43.0% occurred in Belém (96 MDR-TB cases/438 TB cases), followed by 8.1% in Ananindeua (18/70), 2.7% in Marituba (6/18), 3.1% in Castanhal (7/14), 2.2% in Barcarena (5/11), 2.2% in Santarém (5/11), 2.7% in Cametá (6/10) and 0.5% in Abaetetuba (1/8). The districts in Belém with the highest numbers of cases were Guamá (14 MDR-TB cases/45 TB cases), Jurunas (9/41), Sacramenta (10/33), Marco (5/32), Pedreira (3/27), Icoaraci (3/26), Terra Firme (6/24) and Marambaia (4/22).
Spacialization was performed on 483 georeferenced cases of TB. Out of these cases, 59.6% were found to be drug-susceptible, 25.1% were found to be MDR-TB and 15.3% were found to be resistant TB without also being MDR-TB3. All other cases lacked either the geographical coordinates or the complete addresses needed for accurate georeferencing. Figure 1A evidences the spatial distribution of tuberculosis cases in Pará State and in figure 1B, Belém stands out as the Municipality where the largest number of cases occurred.
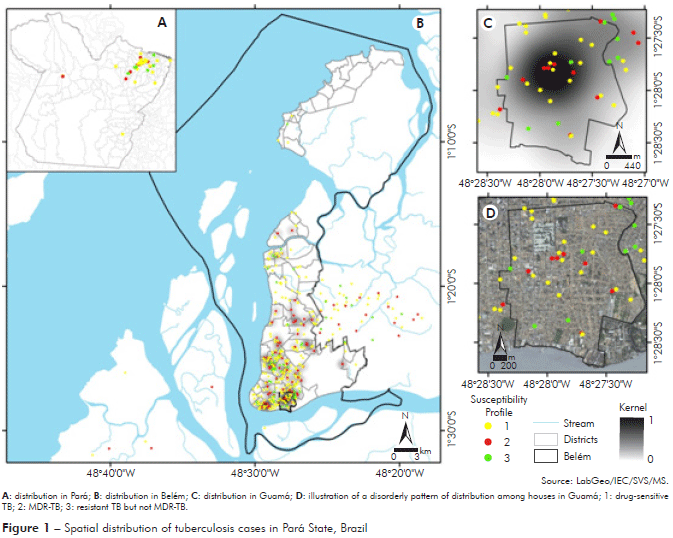
The result of applying Kernel smoothing technique to the points where type 2 TB (MDR) was found can be seen in figure 1B. Among many results observed in this figure, what stands out with the greatest intensity is a hotspot situated in the neighborhood of Guamá (Figure 1C). Figure 1D shows the SPOT satellite image of Guamá, where an inordinate distribution of cases can be noticed.
]]> DISCUSSION
Over the past decade, Brazil has experienced between 70,000 to 80,000 new TB cases a year. However, data from the Ministry of Health show that for the first time, the number of new TB cases fell below 70,000. And in 2011, there were only 36 cases of the disease for every 100,000 inhabitants, as opposed to the 42.8 cases recorded for every 100,000 inhabitants in 200113.
By 2010, there were 607 diagnosed cases of MDR-TB reported in Brazil, as opposed to 334 cases in 2001. It represents an increase of 82% during the years analyzed. From 2009 to 2010, the growth was very significant, as 47% more cases were diagnosed14.
Problems arise when patients are improperly treated or fail to take their prescribed medications appropriately. Cases in which patients are retreated (following relapse or readmission after abandonment) are the ones most likely to lead to an unfavorable outcome, especially among individuals who have already received more than 30 days of treatment.
In Ceará State, the combined MDR-TB rate for the population studied was 17.7% (266/1500)15. The prevalence rates of primary and acquired resistance in the Federal District of Brasília were 9.2% and 15.8% respectively. For MDR-TB, they were 1.0% and 0%, respectively, during the period from 1995 to 199716.
To ensure that resistance is diagnosed as early as possible, the WHO and the Brazilian Ministry of Health recommend that healthcare providers conduct culture and sensitivity testing on all patients who undergo retreatment. In keeping with this recommendation, completion of culture examinations grew 156% in retreatment cases from 2001 to 2010, and was 24% higher than it had been in the last recorded year.
Data presented in this study were obtained mainly from cases of recurrence, abandonment and death, and samples were sent for culture and susceptibility testing to reference laboratories in Pará State (IEC and LACEN/PA). This may account for the high prevalence of resistant TB in this population. Previous studies have revealed great variation in the levels of resistance detected. Such disparities may be product of different study methodologies used by different laboratories5,7,15,16,17,18.
The first vigilance inquiry into resistance, performed by WHO and the International Union Against Tuberculosis and Lung Disease, found the following distribution of tuberculosis cases: rates of primary, acquired and combined MDR-TB were 4.6%, 22.2% and 8.0%, respectively, in Argentina; in Peru, they were 2.5%, 15.7% and 4.5% respectively. The second inquiry found that rates of primary, acquired and combined MDR-TB remained high, with respective levels of 3.0%, 12.3% and 4.3% for Peru and 2.5%, 16.7% and 3.5% for Puerto Rico.
Knowledge of initial drug resistance is impaired by the absence of susceptibility testing in diagnosed cases. Failure to perform or obtain the results of such tests increases the odds of inappropriate treatment, as well as giving multidrug-resistant bacilli more time to disseminate themselves in the community9,19. The development of MDR-TB worsens disease prognosis and increases the government's cost of treatment more than 30-fold. This represents an increase in the average cost of treatment from US$120 (for primary drug-sensitive TB) to US$3,200 (for MDR-TB). Furthermore, MDR-TB can be transmitted during the bacillary phase if appropriate therapy is not administered.
In our report, the studied population was predominantly male, as it has been in studies conducted previously by others7,15,17. Regarding the age distribution of cases, 79.4% (673/848) and 80.1% (180/223) of individuals with TB and MDR-TB, respectively, belonged to the 15 to 54 year old age group, which is considered an economically active group. Although TB infection rates remain high among the elderly, the current study observed that the number of cases in individuals as old as 24 years overlapped with the number of cases among elderly individuals.
]]> The capital of the State and the Municipalities of Abaetetuba, Ananindeua, Castanhal and Marituba had been previously reported by the high prevalence of TB from 2006 to 200820.The thematic map produced with TB and MDR-TB data showed the distribution of cases, according to an endemic area. Many MDR-TB cases are associated with poverty areas with high population density and poor sanitation. In 1996, the situation of the high number of TB cases in the district of Guamá was known by the managers of TB control programs in Belém, because Guamá was one of the neighborhoods chosen for collection of material for the First National Survey of Resistance. The diagnosis and treatment of new TB cases without intervention habits, and misery situation, seem to have little impact on reducing the number of new cases. Costa Neto21 reported that any intervention for TB control conducted in Vila do Rosário, Duque de Caxias, Rio de Janeiro State, for many years, had little effect on the frequency of cases, as if an external reservoir to the region was responsible by the ongoing contamination of people. With poor nutrition and deficient immune system, the presence of the agent is inevitable.
Regarding the cases of MDR-TB observed in the age group with the highest incidence (25-34 years old), it was observed that there was a slight increase in the number of cases for 2007. The subsequent decrease in the number documented of MDR-TB cases may be related to a three-month interruption of sensitivity testing at the IEC and the replacement of medical staff at the State Health Reference Unit.
The control of MDR-TB depends on, among other factors, the early diagnosis of resistance, appropriate therapy, improving the patient's awareness of treatment, and interrupting transmission. The knowledge of the local epidemiological situation is the first step in raising awareness in areas with the largest agglomeration of cases.
Studies conducted in other countries have demonstrated that, with the help of educational interventions, patients have come to better understand information about TB, as well as showing notable improvement with respect to treatment adherence. Dick and Lombard22 evaluated the relationship between health-education approaches and adherence to TB treatment in two health clinics, with one receiving the intervention and one serving as a control. In the clinic that received the intervention (which took the form of an educational pamphlet), researchers found fewer indicators that treatment had been abandoned than were found in the control group.
Improving health literacy is an ongoing project. The more this process is strengthened, the better patients' health reflexes will be. An informative booklet about the conduct of patients and contact people was developed and evaluated by the authors23. The booklet provides information on TB and its prevention, concept, main symptoms, recommendations for the most effective use of medicines and suggestions of habits that can speed up the treatment and prevent transmission. The distribution of booklets will have the partnership of the Secretariat of Health Pará State (SESPA) and its impact on treatment and outcome of cases, as well as searching the Health Unit by contact people will be evaluated.
CONCLUSION
According to previous studies, the total number of TB cases in Pará State did not vary significantly during the study period. There was, however, a slight increase in the number of drug-resistant cases in proportion to the total number of cases reported to the State. The rates for primary, acquired and combined MDR-TB in this study were high when compared to the rates documented in previous inquiries. These resistance rates reflect the need to improve the quality of health services for patients with tuberculosis. Seven Municipalities accounted for 59.6% of the total cases in the present study. A concentration of cases in neighborhoods in the City of Belém was also observed.
]]> ACKNOWLEDGMENTS
The authors thank to the Director of LACEN/PA, Drs. Sebastião Licínio Lira dos Santos and Zelinda Habbid, for giving data related to the sensitivity test conducted at LACEN from 2008 to 2010 and Andréa Pantoja Melo for technical assistance.
FINANCIAL SUPPORT
This study was supported by the Instituto Evandro Chagas, Coordenação de Aperfeiçoamento de Pessoal de Nível Superior (CAPES) and the Programa de Pós-graduação em Biologia Parasitária/Universidade Estadual do Pará.
REFERENCES
1 World Health Organization. Multidrug and extensively drug-resistant TB (M/XDR-TB): 2010 global report on surveillance and response. Geneva: WHO; 2010. [Link]
2 Gandhi NR, Moll A, Sturm AW, Pawinski R, Govender T, Lalloo U, et al. Extensively drug-resistant tuberculosis as a cause of death in patients co-infected with tuberculosis and HIV in a rural area of South Africa. Lancet. 2006 Nov;368(9547):1575-80. Doi: 10.1016/S0140-6736(06)69573-1 [Link]
3 Zignol M, van Gemert W, Falzon D, Sismanidis C, Glaziou P, Floyd K, et al. Surveillance of anti-tuberculosis drug resistance in the world: an updated analysis, 2007-2010. Bull World Health Organ. 2012 Feb;90(2):111-9. Doi: 10.2471/BLT.11.092585 [Link]
]]> 4 World Health Organization. Global tuberculosis report 2012 [Internet]. Geneva: WHO; 2012 [cited 2012 Jul 27]. Available from: http://apps.who.int/iris/bitstream/10665/75938/1/9789241564502_eng.pdf.5 Kritski AL. Multidrug-resistant tuberculosis emergence: a renewed challenge. J Bras Pneumol. 2010 Mar-Apr;36(2):157-8. Doi: 10.1590/ S1806-37132010000200001 [Link]
6 Braga JU, Barreto AMW, Hijjar MA. Inquérito epidemiológico da resistência às drogas usadas no tratamento da tuberculose no Brasil 1995-97. Parte III: principais resultados. Bol Pneumol Sanit. 2003 jan-jun;11(1):76-81.
7 Marques M, Cunha EAT, Ruffino-Neto A, Andrade SMO. Perfil de resistência de Mycobacterium tuberculosis no estado de Mato Grosso do Sul, 2000-2006. J Bras Pneumol. 2010 mar-abr;36(2):224-31. Doi: 10.1590/S1806-37132010000200011 [Link]
8 Ministério da Saúde (BR). Secretaria de Vigilância em Saúde. Série histórica de incidência de tuberculose no Brasil 2012. Brasília: Ministério da Saúde; 2012.
9 Ministério da Saúde (BR). Secretaria de Vigilância em Saúde. Departamento de Vigilância Epidemiológica. Manual nacional de vigilância laboratorial da tuberculose e outras micobactérias. Brasília: Ministério da Saúde; 2008. 436 p. [Link]
10 Pablos-Méndez A, Raviglione MC, Laszlo A, Binkin N, Rieder HL, Bustreo F, et al. Global surveillance for antituberculosis-drug resistance, 1994-1997. N Engl J Med. 1998 Jun;338(23):1641-9. [Link]
11 Bailey TC, Gtroll AC. Interactive spatial data analysis. Harlow: Longman; 1995. 413 p.
12 Esri. Essays on geography and GIS. Vol. 5. Redlands: Esri Press; 2012. 82 p. [Link]
13 Ministério da Saúde (BR). Secretaria de Vigilância em Saúde. Sistema de Informação de Agravos de Notificação. Série histórica da taxa de incidência da tuberculose. Brasil, Regiões e Unidades Federadas de residência por ano de diagnóstico (1990 a 2011). Brasília: Ministério da Saúde; 2012.
]]> 14 Ministério da Saúde (BR). Secretaria de Vigilância em Saúde. Departamento de Vigilância Epidemiológica. Programa nacional de controle da tuberculose [Internet]. Brasília: Ministério da Saúde; 2012 [citado 2012 jul 27]. Disponível em: http://bvsms.saude.gov.br/bvs/publicacoes/ProgramaTB.pdf.15 Barroso EC, Rodrigues JLN, Pinheiro VGF, Campelo CL. Prevalência da tuberculose multirresistente no Estado do Ceará, 1990-1999. J Pneumol. 2001 nov-dez;27(6):310-4. Doi: 10.1590/S0102-35862001000600004 [Link]
16 Alvarez TA, Rodrigues MP, Viegas C. Prevalence of drug-resistant Mycobacterium tubeculosis in patients under intermittent or daily treatment. J Bras Pneumol. 2009 Jun;35(6):555-60. Doi: 10.1590/S1806-37132009000600009 [Link]
17 Hiiiar MA, Procópio MJ, Freitas LMR, Guedes R, Bethlem EP. Epidemiologia da tuberculose: importância no mundo, no Brasil e no Rio de Janeiro. Pulmão RJ. 2005;14(4):310-4. [Link]
18 Bastos GM, Cezar MC, Mello FCQ, Conde MB. Prevalência de resistência primária em pacientes com tuberculose pulmonar sem fatores de risco conhecidos para resistência primária. J Bras Pneumol. 2012 nov-dez;38(6):733-9. Doi: 10.1590/S1806-37132012000600008 [Link]
19 Ministério da Saúde (BR). Secretaria de Vigilância em Saúde. Manual de recomendações para o controle da tuberculose no Brasil. Brasília: Ministério da Saúde; 2011. (Série A. Normas e manuais técnicos). [Link]
20 Ribeiro WA. Tuberculose: um perfil epidemiológico dos municípios de Belém e Ananindeua-PA no período de 2006 a 2008. Rev Para Med. 2011 jan-mar;25(1):1-7. [Link]
21 Costa-Neto C. Vila Rosário e a Cadeia da Miséria: a caminho da eliminação da tuberculose. Rev Bras Pneumol Sanit. 2007 dez;15(1):15-28. [Link]
22 Dick J, Lombard C. Shared vision: a health education project designed to enhance dherence to anti-tuberculosis treatment. Int J Tuberc Lung Dis. 1997 Apr;1(2):181-6. [Link]
23 Apolinario D, Braga RCOP, Magaldi RM, Busse AL, Campora F, Brucki S, et al. Short assessment of health literacy for portuguese-speaking adults. Rev Saude Publica. 2012 Jul;46(4):702-11. Doi: 10.1590/S0034-89102012005000047 [Link]
]]>
 Correspondence /Correspondência / Correspondencia:
Correspondence /Correspondência / Correspondencia:
Karla Valéria Batista Lima
Instituto Evandro Chagas,
Seção de Bacteriologia e Micologia
Rodovia BR 316, km 7, s/n.
Bairro: Levilândia CEP: 67030-000
Ananindeua-Pará-Brasil
E-mail: karlavaleria_2007@hotmail.com
]]>