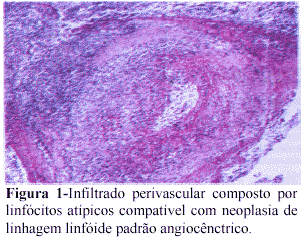
Granulomatose Linfomatóide - relato de caso1
Lymphomatoid Granulomatosis - case report
Ana Cristina Araújo Lemos da SilvaI; José Maria Abreu JuniorII; João Carlos SaldanhaIII; Meire C. F. CalilIV; Marcella Nara NunesV
IMédica Patologista. Professora Auxiliar de Ensino da Disciplina de Patologia Especial da UFTM
IIMédico Residente de Patologia da UFTM ]]>
IIIMédico Patologista do Hospital Escola da UFTM e do laboratório Jorge Furtado
IVMédica Hematologista do Hospital Escola da UFTM
VGraduanda do curso de medicina da UFTM
RESUMO
OBJETIVO: descrever um caso com manifestações clínicas e achados histopatológicos de Granulomatose Linfomatóide (GL), uma rara doença linfoproliferativa das células B, angiocêntrica e angiodestrutiva associada ao vírus Epstein-Barr (EBV). A apresentação clínica mais comum é no pulmão, podendo acometer qualquer órgão, sendo os achados extra-pulmonares as principais manifestações nestes casos.
RELATO DO CASO: mulher de 65, com lesão cutânea vulvar e que evoluiu com quadro neurológico associado a lesão expansiva envolvendo parênquima cerebelar, sem alterações pulmonares.
CONSIDERAÇÕES FINAIS: pelo seu prognóstico e capacidade de ser confundida com outras vasculites a GL impõe-se como um importante diagnóstico diferencial destas doenças.
SUMMARY
INTRODUCTION: this report describe a case of Lymphomatoid Granulomatosis (LG,s a rare linfoproliferative disorder of B cell showing angiocentric growth and destructive behaviour caused by Epstain-Barr virus (EBV). The predominant clinical presentations are confined to the pumonary system, however ; extra-pumonary manifestations can sometimes be the main feature of the dieseses.
METHOD: here we report a 65 year old female, with a skin vulvar lesion, and another in cerebelus, without pulmonary diesese.
CONCLUSION: the LG can mimics systemic vasculits and is a diagnostic challenge.
Keyword: Lymphomatoid Granulomatosis, vasculitss, Epsteisn-Barr virus, vulvar lesion.
INTRODUÇÃO
A Granulomatose Linfomatóide (GL) é uma rara doença caracterizada por lesões proliferativas linforreticulares angiocêntricas e angiodestrutivas descrita inicialmente por Liebow et al. em 1972 1,2,3,4,5 . Pode acometer qualquer órgão havendo predomínio nos pulmões, seguidos da pele e do sistema nervoso central. Existem relatos menos freqüentes de acometimento em rins, fígado e medula óssea 1,2,3,4,6. Historicamente acreditava-se tratar de uma doença dos linfócitos T, porém hoje se sabe que corresponde a uma proliferação clonal de células B rica em células T 4 associada a infecção pelo vírus Epstein-Barr (EBV) em até 70% dos casos1,7. Acomete pacientes entre 30 e 50 anos de idade, com discreto predomínio no sexo masculino 2:1 sendo fatal mais de 50% dos casos. 8,9 O diagnostico diferencial com granulomatose de Wegner por vezes é muito difícil.3
]]> Histologicamente a GL é caracterizada por um infiltrado inflamatório linfóide misto constituído por células mononucleares atípicas, linfócitos pequenos, plasmócitos e histiócitos em arranjo angiocêntrico e angiodestrutivo com grandes focos de necrose. Granulomas podem estar presentes 1,2.
RELATO DE CASO.
Anamnese
Paciente com 65 anos de idade, branca, sexo feminino, com diagnóstico clínico de "câncer de vulva".
Há aproximadamente um mês notou lesão vulvar associada a ardor.
Foi realizada biópsia incisional da lesão em serviço particular, sendo o diagnóstico compatível com linfoma de alto grau (angiocêntrico de células B) (Figura 1).

Após o diagnóstico foi encaminhada ao Hospital Escola da Universidade Federal do Triângulo Mineiro (UFTM) para avaliação e tratamento.
No momento da internação, queixava-se também de tontura que persistia também há um mês, referindo cefaléia de forte intensidade, contínua, seguida por vômitos e astenia.
Antecedentes mórbidos pessoais
A paciente era chagásica há 20 anos, hipertensa, portadora de doença de Cröhn, e tinha história de excisão de carcinoma basocelular em membro superior direito. Negava tabagismo e etilismo.
Exame Físico
Ao exame físico, a paciente encontrava-se emagrecida, com edema periorbitário. Demonstrava ainda dificuldade para permanecer sentada e apresentava marcha atáxica, dismetria, disdiadococinesia, tremores nas estremidades, hipotonia muscular, mas sem nistagmo; caracterizando uma síndrome cerebelar. Notava-se ainda sensibilidade preservada com hipoestesia em plantas dos pés e força motora preservada, grau 4-5. Observou-se lesão ulcerada, friável em lábio direito da vulva.
Exames Complementares
À tomografia computadorizada pôde-se evidenciar extensa massa em cerebelo sugestivo de linfoma. (Figura 2)
]]>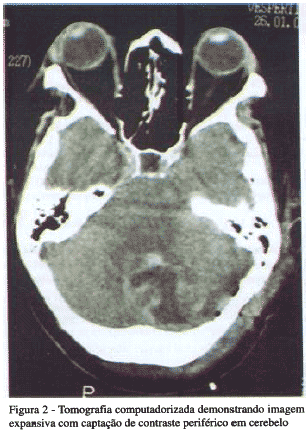
Na ressonância magnética observou-se lesão sólida, expansiva envolvendo o parênquima cerebelar esquerdo e o vêrmis, medindo 4 x 3,5 x 4,8 cm. A lesão se estendia ao parênquima encefálico adjacente com captação anelar periférica de contraste. Notou-se também que o quarto ventrículo estava comprimido e deslocado para a direita. A lesão atingiu a fossa posterior com possibilidade de crescimento e herniação iminente, bem como hidrocefalia.
A radiografia de tórax evidenciou opacidade em base esquerda sugestiva de derrame pleural. O eletrocardiograma revelou presença de taquicardia sinusal. O ecocardiograma mostrou um discreto refluxo mitral. Ausência de células neoplásicas no líquor, sendo que este apresentou coloração e composição normais. Sorologias negativas para HIV, HCV, HBV, e toxoplasmose. Ions normais.
Não foram evidenciadas outras alterações nos demais exames realizados.
Evolução e conduta
Diante da possibilidade de herniação cerebelar iminente a paciente foi encaminhada, em situação emergencial, à neurocirurgia e submetida à ressecção descompressiva da massa. A cirurgia procedeu sem intercorrências. A paciente permaneceu estável, sem déficits motores aparentes, apenas com certa dislalia.
Diagnóstico
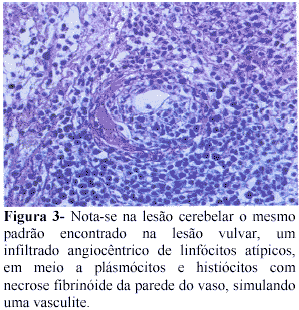
O exame anatomopatológico dos fragmentos excisionados demonstrou neoplasia linfóide com padrão angiocêntrico, associado à necrose fibrinóide da parede dos vasos. O infiltrado era constituído por plasmócitos, histiócitos e imunoblastos em meio a linfócitos atípicos, não havendo predomínio de neutrófilos e eosinófilos caracterizando linfoma angiocêntrico, compatível com granulomatose linfomatóide (Figura 3).
]]>
Feitos estudos imunoistoquímicos que demonstraram tratar-se de uma população de linfócitos B atípicos associada a um infiltrado rico em células T. O marcador para vírus Epstein-Barr também foi positivo, confirmando assim o diagnóstico.
Realizada biópsia de medula óssea, sem evidências de infiltração neoplásica.
Tratamento
A paciente realizou o primeiro ciclo de quimioterapia, no HEMOCENTRO da Universidade Federal do Triângulo Mineiro (UFTM). E estava em uso contínuo de dexametasona sem intercorrências.
Pouco depois veio a falecer de causa não relacionada à patologia de base.
]]> DISCUSSÃO
Existem apenas cerca de 600 casos de Granulomatose Linfomatoide (GL) referidos na literatura até o presente, sendo a pele o segundo local mais acometido. Além de ulcerações costumam ser vistas pápulas, placas, lesões crostosas, edema facial, erupções que lembram foliculites e lesões infiltrativas que podem inclusive mimetisar hanseníase 9,10.
Além da clínica que pode ser bastante inespecífica em fases precoces, o diagnóstico anatomopatógico também impõe grandes dificuldades, posto que, as vasculites encontradas podem ser facilmente confundidas com Granulomatose de Wegner3,8,9 ,principalmente, diante do informe clínico de lesões pulmonares e alterações renais, as quais não estavam presentes neste caso.
Ressalte-se, ainda, que as biópsias de pele nos casos precoces de GL raramente são diagnósticas apresentando muitas vezes apenas vasculites sem atípias celulares, ou células positivas para EBV. Locais acessíveis para biópsias como medula óssea e linfonodos costumam não estar envolvidos nesta fase da doença. Nestas situações não raro a GL é confundida com poliarterite nodosa 3.
Pela sua gravidade, inespecificidade e implicações prognosticas, a GL deve sempre entrar na lista de diagnósticos diferenciais de vasculites11. Alguns autores recomendam que sejam feitas biopsias repetidas ou biopsias múltiplas quando as manifestações forem multicêntricas principalmente em casos que sugerem vasculites, mas o paciente não responde a terapêutica específica 3.
REFERÊNCIAS
1. TANIERE, P.H.; THIVOLET-BÉJUI, F., VITREY, D.; ISAAC. S.; LOIRE, S.; CORDIER, J.F.; BERGER, F. –Lymphomatoid granulomatosis- a report on four cases: evidence for B phenotype of the tumoral cells, Eur. Respir. J.1998, (12): 102-106.
2. WILSON, W.H.; KINGMA, D.W.;RAFFELD, M.; WITTES, R.B.; JAFFE, E.- Association of Lymphomatoid Granulomatosis With Epstais-Bar Viral Infection of B Lymphocytes and Response to Interferon- α 2b, Blood.1996, 87 (4):4531-4537.
3. SHERRY, M.; YOON, M.; OSTRZEGA ,N.; CLEMENTS, J.; WONG – Lymphomatoid Granulomatosis: A Rare Mimicker of Vasculitis, J. Rheumatol. 2005, 32 (11):2242-2245.
4. BAE, W. K. ; LEE, K.S.; KIM, N. P.; KIM, I.Y.-Lymphomatoid Granulomatosis with Isolated Involvement of the Brain. J. Korea Med. Sc.1991, 6 (3): 255-259.
5. TATEISHI, U.; TERAE, S.; OGATA, A.; SAWAMURA, Y; SUZUKI, Y.-MR Imaging of the Brain in Lymphomatoid Granulomatosis. AJNR. 2001, 22: 1283-1290.
6. ROSAI, J.; Rosai and Ackermam's Surgical Pathology. 9 ed. China: Mosby, 2003. Cap.9; p. 418.
7. CULHACI, N.; LEVI, E.; SEM, S.;KACAR, F.; METEOGLU, I.; - Pulmonary Lymphomatoid Granulomatosis Envolving to Large Cell Lymphoma in the Skin. Pathology Oncology Reserch.2002, 8 (4): 280-282.
8. SHOEN, F. Os vasos sanguíneos. In: KUMAR, V.; ABBAS, A; FAUSTO; N. Robbins e Cotran-Patologia Bases Patológicas das Doenças. 7. Ed. Rio de Janeiro: Elsevier, 2005. Cap. 11; P. 569
9. PERCIK, R.; SERR, J.; SEGAL, G,; STIENLAUF, S.; TRAU, H.; SHALMON, B.; SHIMONI, A.; SIDI, Y. - Lymphomatoid granulomatosis: a Diagnostic Challenge. IMAJ.2005, (7): 198-199.
10. HU, H.; LIU, C,; CHIU, C; HSIAO, L;- Successful treatment of elderly advanced lymphomatoid granulomatosis with rituximab-CVP combination therapy, EJH. 2007, (78): 176-177.
11. MCCLOSKEY, M.; CATHERWOOD, M.; MCMANUS, D; TOOD,G.; CUTHBERT, R.-A case of lymphomatoid granulomatosis masquerading a lung abscess. Thorax.2004, 59 (8): 818-819.
]]>
 Endereço para correspondência:
Endereço para correspondência: Recebido em 12.03.2007 ]]> Aprovado em 27.06.2007
1Trabalho realizado no Hospital Escola da Universidade Federal do Triângulo Mineiro (UFTM), Uberaba, Minas Gerais.
]]>